US Pharm. 2023;48(3):HS2-HS6.
ABSTRACT: Breakthrough pain is an abrupt, brief flare-up of pain that occurs despite well-controlled background pain. Unrecognized or inadequately managed breakthrough pain poses physical, psychological, and social challenges, including loss of productivity and diminished quality of life. Short-acting opioids are often used for breakthrough pain, and rapid-onset transmucosal fentanyl formulations are indicated for managing breakthrough pain in adults with cancer who are routinely using other opioid analgesics around the clock for pain. Pharmacists can give prescribers and patients key information about current pain-management approaches to breakthrough pain; they can also screen patients for potential drug-drug interactions and contraindications and make clinical recommendations, when warranted, to improve clinical outcomes or to reduce or prevent adverse events, among other duties.
In clinical practice, pain is one of the most common symptoms for which people seek medical care. Pain can affect both physical and psychological aspects of an individual’s ability to function in day-to-day activities. The intensity and frequency of pain vary from individual to individual and can be classified as chronic (persistent) pain or acute (abrupt-onset) pain. Additionally, some patients may experience breakthrough pain. Although no standard definition exists, in 1990, Portenoy and Hagen first described breakthrough pain as “a transient exacerbation of pain that occurs despite relatively stable and adequately controlled background pain.”1,2 Subsequently, breakthrough pain has been characterized as severe, acute pain that is transitory and either occurs spontaneously or is caused by a specific predictable or unpredicable trigger despite background pain being relatively stable and adequately controlled by a sustained-release, long-acting, oral, transdermal, or parenteral opioid regimen.2-6 Additionally, guidelines for managing breakthrough pain in cancer patients define breakthrough cancer pain as a temporary exacerbation of pain that evolves despite the use of around-the-clock opioids for pain management.7
Although anyone who lives with pain can experience breakthrough pain, it is commonly known to occur in patients with cancer, especially advanced cancer.7-9 Breakthrough pain also occurs with chronic conditions such as arthritis, multiple sclerosis, fibromyalgia, and back problems.7-9 It has been described as disabling and can have a profoundly negative impact on patients’ health-related quality of life (QoL).8,9 Unrecognized and unmanaged breakthrough pain is associated with significant physical and psychological health burdens for the patient and economic burdens for both the patient and the healthcare system owing to daily functional impairment and greater healthcare-resource utilization (i.e., office visits and hospitalizations). It has been found that breakthrough pain is often underestimated, especially in cancer patients, and that many patients are undertreated and continue to experience breakthrough pain.8,9 Moreover, an international survey concluded that the incidence of breakthrough pain may also indicate the likelihood of more severe pain, pain-related distress, and impaired productivity and QoL.3 Breakthrough pain is associated with sleep problems, anxiety, and depression.10
Estimated Incidence
The precise incidence of breakthrough pain remains unknown; however, statistics from the American Pain Foundation suggest that breakthrough pain occurs in 50% to 90% of all hospitalized cancer patients, 89% of all patients admitted to skilled-nursing geriatric facilities and end-of-life care centers, and 35% of all ambulatory-care cancer patients.11 The initial research on breakthrough pain concentrated on patients with cancer; however, breakthrough pain is now generally recognized to occur in patients with chronic conditions that are not cancer-related, as noted above; for example, breakthrough pain is common in persons with lower back pain.12 It has been calculated that 70% of patients with breakthrough pain have non–cancer-related chronic conditions.13 Moreover, it is estimated that more than 75% of patients with well-controlled baseline pain experience breakthrough pain.8
Identifying Breakthrough Pain
To effectively manage breakthrough pain, it is imperative for clinicians to recognize the key features of breakthrough pain. Breakthrough pain is characterized by abrupt onset, brief duration, and moderate-to-severe intensity.4,15 The duration typically varies from a few seconds or minutes to an average of 45 to 60 minutes, and patients may experience multiple episodes throughout the day.10 The pain may be spontaneous in nature (idiopathic pain) or related to a specific trigger (incident pain).14,15 Incident pain may be further classified as volitional (triggered by a voluntary act, such as walking) or nonvolitional (triggered by an involuntary act, such as coughing).15 As previously noted, breakthrough pain has a significant negative impact on the patient’s QoL.4,15
Etiology and Pathophysiology
Breakthrough pain is classified as nociceptive, neuropathic, or a combination of these (mixed pain). See TABLE 1.14,15
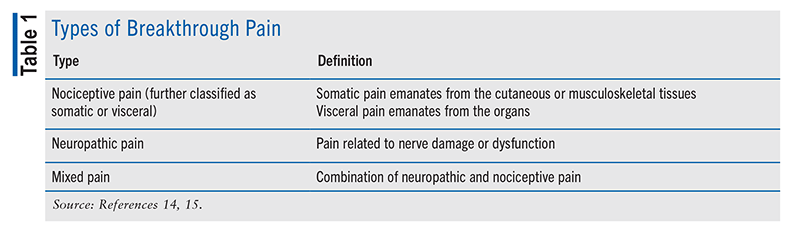
Breakthrough pain is a heterogeneous condition because it differs from patient to patient and has numerous causes.15 Although some cases are insignificant, breakthrough pain may be associated with serious physical, psychological, and social complications and contribute to greater morbidity.15 The National Cancer Institute (NCI) notes that the degree of pain may be severe, and the pathophysiology is often the same as that for the patient’s background pain.16 Breakthrough pain may be triggered by extreme levels of stress, certain illnesses, or activities (e.g., exercising, coughing), or it can happen when the analgesic effect of the patient’s pain medication is insufficient or wanes.16
Management
Effective management of breakthrough pain often entails an interdisciplinary and multimodal approach. Early clinical intervention with pharmacologic therapy is the foundation of breakthrough-pain treatment and can be instrumental in enhancing patients’ QoL and productivity.15
Optimal management of breakthrough pain calls for a thorough evaluation of the patient, including the pain etiology, factors that may trigger or exacerbate pain, and ongoing reassessment of the patient’s response to the selected pain-management strategy.15 Clinicians should also assess how breakthrough pain affects a patient’s productivity and QoL and tailor management to individual need. Factors that are often considered include the patient’s medical and medication history; prior analgesic use and response; severity, duration, and frequency of breakthrough pain; and treatment preferences.15,17 Prescribers should also consider patients’ risk factors for possible addiction, abuse, and misuse.15,17
In May 2019, the U.S. Department of Health and Human Services’ Pain Management Best Practices Inter-Agency Task Force published a report on pain management that stressed the significance of implementing a patient-centered approach to diagnosis and treatment of acute and chronic pain and the value of tailoring therapy to patient need.18 The report emphasizes the importance of developing an effective pain-treatment plan following proper evaluation to establish a diagnosis, with detectable outcomes that focus on improvements such as QoL, enhanced functionality, and activities of daily living.18
Multiple publications recommend as-needed (PRN) use of a short-acting opioid as the ideal approach to managing breakthrough pain when no contraindications are present.19-21 For example, Portenoy and colleagues note that because of the increased occurrence of breakthrough pain in patients with cancer and the numerous negative clinical consequences, a therapeutic approach known as rescue dosing is extensively employed.19 An Oxford University Press textbook on cancer-related breakthrough pain considers short-acting opioids the rescue medication of choice for managing breakthrough pain.15 Other recommended nonopioid strategies include the use of nonsteroidal anti-inflammatory drugs and the avoidance of triggers when feasible.15 The rescue dose is separate from the fixed-schedule opioid-analgesic regimen, and it typically entails the use of one of the single-entity oral opioid formulations, such as immediate-release morphine, oxycodone, hydromorphone, or oxymorphone.19 In general, the dose of short-acting opioids for breakthrough pain ranges from approximately 5% to 15% of the total 24-hour scheduled opioid dose.19,21-23 The clinician should regularly reassess patients and make dosing adjustments as warranted, based on response.19-21
If feasible, clinicians should prescribe the same pharmacologic class for both long-acting (24-hour scheduled doses) and short-acting (PRN doses for relief of breakthrough pain) opioid analgesics.21 The NCI states that rapid-acting oral, buccal, sublingual, transmucosal, rectal, and intranasal products are appropriate for treating breakthrough pain when no contraindications exist.24
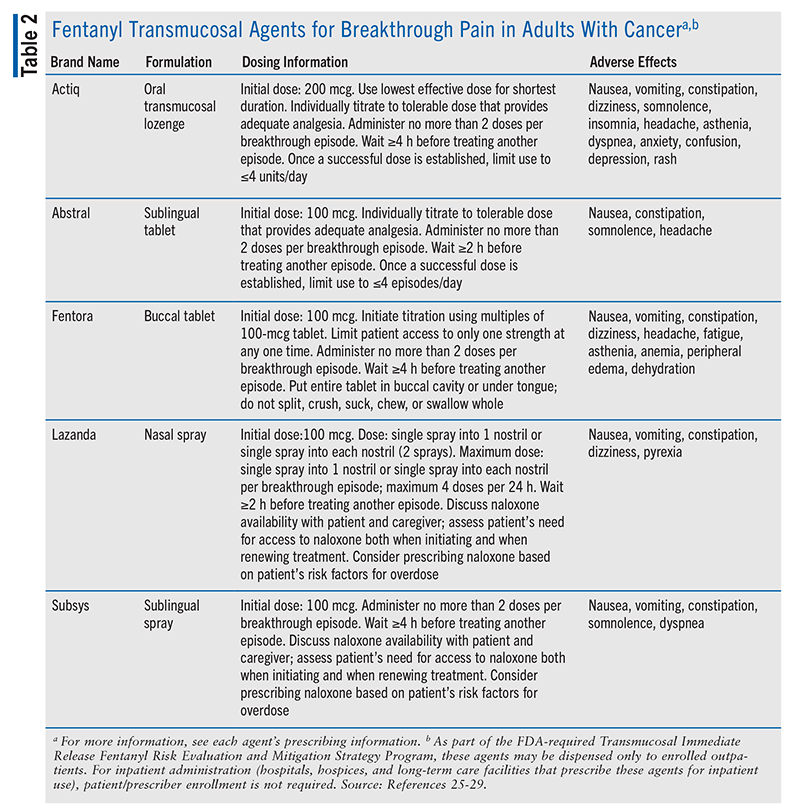
Breakthrough pain may also be managed with rapid-onset transmucosal fentanyl formulations, which are specifically indicated for managing breakthrough pain in adults with cancer who are already receiving and tolerate around-the-clock opioid therapy for underlying cancer pain (TABLE 2).19 The agent should be initiated at the lowest dose and titrated to effect according to its prescribing information.19,25-29 Prescribers should be aware that all transdermal fentanyl products, including generics, require adherence to the agent’s shared Risk Evaluation and Mitigation Strategy (REMS) program; enrollment in the REMS program is mandatory and is intended to lessen the risk of misuse/abuse and unintentional overdose.19,25-29 Clinicians should also consider the patient’s risk factors for addiction, abuse, and misuse.25-29 When opioid therapy is no longer necessary, clinicians should consider discontinuing these agents, along with a gradual decrease in other opioids, to lessen possible withdrawal effects.25-29
Nonpharmacologic Therapies
In conjunction with pharmacologic therapy, patients often use nonpharmacologic interventions when reasonable for management of breakthrough pain. Examples include application of heat or cold therapy, the use of braces, physical therapy, relaxation techniques, massage therapy, transcutaneous electrical nerve stimulation, and acupuncture.15 Before implementing any of these interventions, patients should discuss the appropriateness with their primary healthcare provider.
Recent Clinical Information
A recent review reported that breakthrough pain may occur in the following cases: 1) the basal opioid dose may be inadequate to control the total daily pain level; 2) the PRN analgesic dose is insufficient; 3) the patient may not be using the PRN analgesic strategically before activities that trigger the pain.17
In November 2022, the CDC issued an updated clinical-practice guideline for prescribing opioids for pain.30 This guideline provides clinicians with valuable guidance on the selection of pain-management strategies for short-term and long-term pain.
A recently published American Society of Clinical Oncology guideline on the use of opioids to manage pain in adults with pain from cancer or cancer treatment presented guidance based on a review of clinical evidence, including the following recommendations for breakthrough pain31:
• In patients receiving opioids around the clock, immediate-release opioids at a dose of 5% to 20% of the regular daily morphine equivalent dose should be prescribed for breakthrough pain.
• The evidence remains insufficient for recommending a specific short-acting opioid for breakthrough pain.
• The dose should be increased if the patient reports persistent pain after being on a certain dose of a regular opioid for a few days, or when the pain level is low but the patient requires multiple breakthrough-opioid doses per day. A straightforward approach to determining the new dose of an opioid that is administered around the clock is to add the total daily dose of the regular plus breakthrough opioids and increase this number by 20% to 30%. It is also beneficial to adjust the breakthrough-opioid dosing to maintain each dose at approximately 10% (5%-20%) of the regular daily opioid dose.31
A 2021 study examined the use of opiate analgesics, including dose, frequency, and actual adverse effects (AEs), in cancer patients with breakthrough pain.32 Patients received opioids around the clock for background pain, as well as rescue medication for breakthrough pain. Immediate-release morphine, the analgesic most often prescribed for breakthrough pain, was used at 6.67% to 60% of the daily dose, with a frequency of use of two to six times per day.32 There were 189 patient visits (56.42% of visits) for AEs experienced with the opioid, with the most common AEs being constipation, nausea, and vomiting.32
The Pharmacist’s Role
Owing to their drug expertise, pharmacists are well poised to make clinical recommendations regarding appropriate pain management and customization of pain-management therapies to patient need. As integral members of the healthcare team, pharmacists can provide prescribers and patients with key information about current pain-management approaches to acute and chronic pain as well as breakthrough pain, and they can screen for potential drug-drug interactions and contraindications and make clinical recommendations, when warranted, to improve clinical outcomes or to reduce or prevent AEs. Pharmacists can also be instrumental in ensuring that patients and caregivers understand the proper administration, dose, and dosing intervals of the prescribed pain medications. It is imperative that pharmacists be knowledgeable about the challenges associated with pain management, current recommendations for managing breakthrough pain, and efficacy and safety data for available analgesics. This awareness may in turn help address pain-related problems, reduce the incidence of breakthrough pain, improve overall clinical outcomes, and enhance patients’ health-related QoL.
Findings from a recently published pooled analysis revealed that clinical interventions by pharmacists helped lessen pain intensity among study participants with chronic pain.33 The analysis also found that pharmacists were integral in ensuring the proper use of analgesics, which resulted in reductions in pain intensity.33 Pharmacists’ valuable clinical duties may also extend to the identification and management of breakthrough pain.
Conclusion
Patient education is essential to effective management of breakthrough pain. Pharmacists are well poised to identify patients experiencing episodes of breakthrough pain, and they can be instrumental in educating patients about treatment options. Through patient education, pharmacists can ensure that patients and caregivers are familiar with the treatment goals and expectations, the monitoring and management of potential AEs, and when to contact the primary healthcare provider. Pharmacists can also make clinical recommendations tailored to patient need, monitor therapeutic response, and suggest dose adjustments (including decreases or increases, when warranted), which in turn may lessen patients’ pain and improve their productivity and overall health-related QoL.
REFERENCES
1. Portenoy RK, Hagen NA. Breakthrough pain: definition, prevalence, and characteristics. Pain. 1990;41(3):273-281.
2. Portenoy RK, Payne D, Jacobsen P. Breakthrough pain: characteristics and impact in patients with cancer pain. Pain. 1999;81(1-2):129-134.
3. Caraceni A, Martini C, Zecca E, et al. Breakthrough pain characteristics and syndromes in patients with cancer pain. An international survey. Palliat Med. 2004;18(3):177-183.
4. López Alarcón MD, Estevez FV, Triado VD, et al. Consensus statement on the management of breakthrough cancer pain: assessment, treatment, and monitoring recommendations. Open J Pain Med. 2019;3(1):008-014.
5. Davies AN, Dickman A, Reid C, et al. The management of cancer-related breakthrough pain: recommendations of a task group of the Science Committee of the Association for Palliative Medicine of Great Britain and Ireland. Eur J Pain. 2009;13(4):331-338.
6. Pérez-Hernández C, Blasco A, Gándara Á, et al. Prevalence and characterization of breakthrough pain in patients with cancer in Spain: the CARPE-DIO study. Sci Rep. 2019;9(1):17701.?
7. Caraceni A, Davies A, Poulain P, et al. Guidelines for the management of breakthrough pain in patients with cancer. J Natl Compr Canc Netw. 2013;11(suppl 1):S29-S36.
8. Mercadante S. Breakthrough pain in cancer patients: prevalence, mechanisms, and treatment options. Curr Opin Anaesthesiol. 2015;28(5):559-564.
9. Canal-Sotelo J, Trujillano-Cabello J, Larkin P, et al. Prevalence and characteristics of breakthrough cancer pain in an outpatient clinic in a Catalan teaching hospital: incorporation of the Edmonton Classification System for Cancer Pain into the diagnostic algorithm. BMC Palliat Care. 2018;17(1):81.
10. Guitart J, Vargas MI, De Sanctis V, et al. Breakthrough pain management with sublingual fentanyl tablets in patients with cancer: age subgroup analysis of a multicenter prospective study. Drugs R D. 2017;17(3):419-425.
11. Margarit C, Juliá J, López R, et al. Breakthrough cancer pain—still a challenge. J Pain Res. 2012;5:559-566.
12. Torres LM, Jiménez AJ, Cabezón A, Rodríguez MJ. Prevalence and characterization of breakthrough pain associated with chronic low back pain in the south of Spain: a cross-sectional, multicenter, observational study. Pain Res Treat. 2018;2018:4325271.
13. Smith H. A comprehensive review of rapid-onset opioids for breakthrough pain. CNS Drugs. 2012;26(6):509-535.
14. Lara-Solares A, Ahumada Olea M, Basantes Pinos ALÁ, et al. Latin-American guidelines for cancer pain management. Pain Manag. 2017;7(4):287-298.
15. Davies A. Cancer-Related Breakthrough Pain. 3rd ed [online]. Oxford, UK: Oxford University Press; 2019.
16. National Cancer Institute. Breakthrough pain. www.cancer.gov/publications/dictionaries/cancer-terms/def/breakthrough-pain. Accessed January 3, 2023.
17. Scarborough BM, Smith CB. Optimal pain management for patients with cancer in the modern era. CA Cancer J Clin. 2018;68(3):182-196.
18. U.S. Department of Health and Human Services. Pain Management Best Practices Inter-agency Task Force report: updates, gaps, inconsistencies, and recommendations. www.hhs.gov/sites/default/files/pmtf-final-report-2019-05-23.pdf. Accessed January 3, 2023.?
19. Portenoy RK, Mehta Z, Ahmed E. Cancer pain management with opioids: optimizing analgesia. Post TW, ed. UptoDate. Waltham, MA: UptoDate Inc. www.uptodate.com. Accessed January 3, 2023.
20. Nadeau SE, Lawhern RA. Management of chronic non-cancer pain: a framework. Pain Manag. 2022;12(6):751-777.
21. Kishner S. Opioid equivalents and conversions. Medscape. https://emedicine.medscape.com/article/2138678-overview. Accessed January 3, 2023.
22. Azhar A, Kim YJ, Haider A, et al. Response to oral immediate-release opioids for breakthrough pain in patients with advanced cancer with adequately controlled background pain. Oncologist. 2019;24(1):125-131.
?23. National Comprehensive Cancer Network (NCCN). NCCN clinical practice guidelines in oncology. Adult cancer pain. Version 2.2017. www.nccn.org/professionals/physician_gls/pdf/pain.pdf. Accessed January 3, 2023.
24. National Cancer Institute. Cancer pain (PDQ®)–health professional version. www.cancer.gov/about-cancer/treatment/side-effects/pain/pain-hp-pdq#_39_toc. Accessed January 3, 2023.
25. Abstral (fentanyl) product information. Solana Beach, CA: Sentynl Therapeutics, Inc; December 2016.
26. Lazanda (fentanyl) product information. Northbrook, IL: West Therapeutic Development, LLC; March 2021.
27. Subsys (fentanyl) product information. Northbrook, IL: West Therapeutic Development, LLC; April 2021.
28. Fentora (fentanyl) product information. Parsippany, NJ: Teva Pharmaceuticals USA, Inc; November 2022.
29. Actiq (fentanyl) product information. Parsippany, NJ: Teva Pharmaceuticals USA, Inc; November 2022.
30. Dowell D, Ragan KR, Jones CM, et al. CDC Clinical Practice Guideline for Prescribing Opioids for Pain—United States, 2022. MMWR Recomm Rep. 2022;71(RR-3):1-95.
31. Paice JA, Bohlke K, Barton D, et al. Use of opioids for adults with pain from cancer or cancer treatment: ASCO guideline. J Clin Oncol. 2023;41(4):914-930.
32. Rahmadi M, Madina U, Sulianto I, et al. Study on dosage range evaluation opioid analgesic for breakthrough pain in cancer patients: a retrospective study. Ann Palliat Med. 2021;10(2):1237-1243.
33. Thapa P, Lee SWH, Kc B, et al. Pharmacist-led intervention on chronic pain management: a systematic review and meta-analysis. Br J Clin Pharmacol. 2021;87(8):3028-3042.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.






