US Pharm. 2009;34(7):HS-11-HS-15.
Exacerbations are an important outcome measure in chronic obstructive pulmonary disease (COPD) due to their profound effect on the patient's quality of life and prognosis. It has been estimated that patients with COPD suffer one to four exacerbations per year, and up to 70% of the direct health care costs associated with the disease are due to severe exacerbations, particularly those requiring hospitalization.1,2 Less than one-third of exacerbations are reported, and although some may not be serious enough to warrant an emergency visit or hospitalization, they have been shown to have an important impact on the patient's health status.3 Exacerbations are not random events but cluster together in time such that there is a high-risk period for recurrence in the 8-week period after an initial exacerbation.4 They also become more frequent and severe as the severity of the underlying COPD increases and contribute to further impairment in lung function.5
Definition and Etiology
An exacerbation of COPD is defined as an event in the natural course of the disease characterized by a change in the patient's baseline dyspnea, cough, and/or sputum that is beyond normal day-to-day variations; is acute in onset; and may warrant a change in regular medication.6 The most common causes of exacerbations are infection of the tracheobronchial tree and air pollution, which increase airway inflammation or directly affect expiratory flow limitation, but the cause of approximately one-third of severe exacerbations cannot be identified.5,7 Systemic inflammation, manifested by elevated fibrinogen levels, is significantly predictive for the occurrence of moderate-to-severe exacerbations.8 C-reactive protein concentration, in the presence of a major exacerbation symptom, has been the most effective biomarker for differentiating exacerbations from day-to-day symptom variations, but it is not helpful in predicting severity.9 Individual susceptibility to exacerbations may also be attributed to a genetic variance in the CCL1 gene, which encodes a chemotactic factor for a series of leukocytes, including monocytes and macrophages.10
Bacterial etiology in approximately 50% of exacerbations is substantiated by bronchoscopic isolation of bacteria in the distal airways; the relationship of new strain isolation and exacerbations; the development of a specific immune response to the infecting pathogen; and association of neutrophilic airway inflammation with bacterial isolation during exacerbations. Pathogens with the most clearly established role in exacerbations of COPD, Haemophilus influenzae, Streptococcus pneumoniae, and Moraxella catarrhalis, are present in higher concentrations compared with pathogens that are more likely to be colonizers, such as Haemophilus parainfluenzae.11 Pseudomonas aeruginosa is more likely to be isolated from patients with severe disease, particularly among those who require mechanical ventilation, have extremely low forced expiratory volume in one second (FEV1), and have used systemic steroids and/or antibiotics within the preceding months.12 New bacterial strain exacerbations are associated with more intense neutrophilic airway and systemic inflammation than those with preexisting strains and nonbacterial episodes.13 Both viral and bacterial infections are directly related to exacerbation severity and are associated with the vast majority of severe COPD exacerbations requiring hospitalization.14
Assessment of Severity
Assessment of the severity of an exacerbation is based on the patient's medical history before the exacerbation, preexisting comorbidities, symptoms, physical examination, arterial blood gas measurements, and other pertinent laboratory tests. Increased breathlessness is the main symptom, but is often accompanied by wheezing, chest tightness, increased cough and sputum, change of the color and/or tenacity of sputum, and fever. In patients with very severe COPD, the most important sign of a severe exacerbation is a change in the mental status of the patient.6
Exacerbations are categorized in terms of either clinical presentation and/or health care resource utilization, but there is no consensus regarding classification of severity.7 The American Thoracic Society/European Respiratory Society guidelines include a ranking based on the patient's clinical presentation and predicted outcome to facilitate appropriate therapy.15 Level I patients with mild-to-moderate COPD and no comorbidities can be treated on an outpatient basis. Level II patients with moderate-to-severe COPD and comorbidities require hospitalization. Level III patients who are hemodynamically unstable with severe COPD and comorbidities require treatment in an intensive care unit to prevent and/or treat respiratory failure.15 Indications for hospitalization are shown in TABLE 1.

Spirometry measurements are not accurate during an acute exacerbation; therefore, their routine use is not recommended. Pulse oximetry can be used to evaluate a patient's oxygen saturation and need for supplemental oxygen therapy, and arterial blood gas measurements are crucial for assessing exacerbation severity.6 Chest radiographs are useful in identifying alternative diagnoses, and an echocardiogram aids in the diagnosis of right-heart hypertrophy, arrhythmias, and ischemic episodes.7
Management
Pharmacologic treatment of the patient with an exacerbation is based on adjusting and/or adding the same medications utilized in the management of stable COPD.6,15 The goals of therapy are prevention of hospitalization or reduction in hospital stay, prevention of acute respiratory failure and death, resolution of exacerbation symptoms, and a return to baseline clinical status and quality of life.16
Bronchodilators: For both outpatient and inpatient management of exacerbations, inhaled short-acting beta2-agonists are the preferred bronchodilators.6 Albuterol is the agent most commonly used due to its lower cost and equivalent efficacy when compared with levalbuterol.16,17 Dosing can be increased to two inhalations every 3 to 4 hours as needed to provide symptomatic relief and increase mucociliary clearance.16,17 Administration via metered-dose and dry-powder inhalers is at least as effective as nebulization therapy and is favored due to reasons of cost and convenience, even in the hospital setting.16 If a prompt response does not occur, the addition of the short-acting anticholinergic ipratropium is recommended, every 6 hours as needed, even though evidence concerning the effectiveness of this combination is controversial.7 Common side effects that occur include tachycardia and tremor for albuterol and dry mouth and nausea for ipratropium.16 The use of scheduled inhaled long-acting bronchodilators, either beta2-agonists (salmeterol and formoterol) twice daily or anticholinergic (tiotropium) daily, has been shown to reduce the rate of COPD exacerbations by approximately 20%.17,18 Methylxanthines (theophylline and aminophylline) are currently considered second-line intravenous therapy for insufficient response to inhaled short-acting bronchodilators.6
Corticosteroids: Systemic corticosteroids reduce recovery time, improve lung function (FEV1) and hypoxemia, and may reduce the risk of early relapse, treatment failure, and length of hospital stay.7 They are considered in addition to bronchodilators if the patient's baseline FEV1 is less than 50% of predicted, and therapy with oral prednisolone (or equivalent) is preferred at a dose of 30 to 40 mg daily for 7 to 10 days.6 Oral prednisolone has been shown to be as effective as the intravenous route in treating exacerbations.19 Extending the duration of therapy beyond 2 weeks and using higher doses does not confer additional benefits, but can increase the risk of short-term side effects such as hyperglycemia and insomnia.7,20 If steroid therapy is continued for longer than 2 weeks, a tapering schedule should be employed to avoid hypothalamic-pituitary-adrenal axis suppression.16
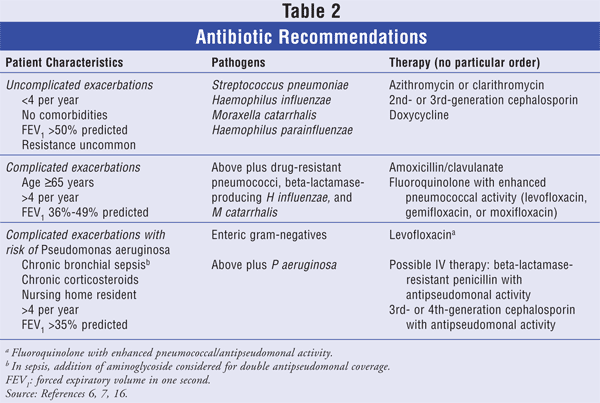
Antibiotics: Antibiotics should be given to patients with exacerbations who exhibit increased dyspnea, sputum volume, and purulence or who require mechanical ventilation.6 Increased emergence of drug-resistant organisms has mandated that antibiotic regimens be based on the most likely organisms responsible for the infection. Trimethoprim-sulfamethoxazole should not be used due to increasing pneumococcal resistance; amoxicillin and first-generation cephalosporins are not recommended due to beta-lactamase susceptibility; and erythromycin is not recommended due to insufficient activity against H influenzae.16 The route of administration depends on the ability of the patient to eat and on the pharmacokinetics of the antibiotic, but the oral route is preferred for a duration of 3 to 7 days.6 TABLE 2 summarizes recommended antimicrobial therapy for exacerbations based on the patient's clinical manifestations.
Oxygen: Oxygen therapy is of central importance in the hospital treatment of exacerbations, since administration for greater than 15 hours per day increases survival and improves hemodynamics, exercise capacity, and general alertness.18 The role of oxygen in patients with mild hypoxemia is controversial, since oxygen is usually recommended for patients with very severe COPD (partial arterial oxygen pressure [PaO2] <55 mmHg or oxygen saturation <88%) and the goal of therapy is to preserve the function of vital organs by increasing the PaO2 to ≥60 mmHg and oxygen saturation to ≥90%.18
Ventilatory Support: Ventilatory support includes both noninvasive intermittent ventilation (NIV) and invasive mechanical ventilation by orotracheal tube or tracheostomy. NIV improves respiratory acidosis and decreases respiratory rate, severity of breathlessness, and length of hospital stay.6,7 Invasive mechanical ventilation has inherent hazards, such as pneumonia, barotrauma, and failure to wean to spontaneous ventilation, but is indicated when NIV fails or is contraindicated (respiratory arrest, cardiovascular instability, high aspiration risk, extreme obesity, impaired mental status).6
Discharge and Mortality
Insufficient clinical data exist to establish the optimal duration of hospitalization for an exacerbation, but TABLE 3 summarizes the recommended discharge criteria. Due in part to other medical conditions that can aggravate or mimic COPD exacerbations, including pneumonia, congestive heart failure, pneumothorax, pleural effusion, pulmonary embolism, and cardiac arrhythmias, 10% to 30% of patients do not respond to treatment.6 In-hospital mortality of patients for acute exacerbations is relatively high, and clinical features seem to be the most reliable factors to predict this outcome.21 Mortality rates 1 year after hospital discharge for patients requiring mechanical ventilation for respiratory failure have been reported to be as high as 59%, and risk factors include hypercapnia, hypoxemia, low body mass index, older age, cardiac factors, comorbidities, severity of illness, low serum albumin level, long-term use of oral corticosteroids, and functional status.22

Conclusion
The frequency and severity of exacerbations seem to be the most important factors determining overall prognosis in COPD. Opportunities for prevention of future exacerbations can be reviewed with the patient prior to hospital discharge, including developing a written action plan. Patient education topics should include smoking cessation, influenza and pneumococcal vaccinations, current pharmacologic therapy including inhaler technique, and how to recognize symptoms of exacerbations.6 Early recognition of exacerbation symptoms and prompt treatment may reduce both the time to recovery and the need for hospitalization. Immediate follow-up of patients after an exacerbation may also help to identify those at risk of recurrence who are most likely to benefit from preventive therapies. Reducing the frequency and severity of acute exacerbations could potentially reduce the mortality inherent to COPD.
REFERENCES
1. Soler-Cataluna JJ, Martinez-Garcia MA, Sanchez PR, et al. Severe acute exacerbations and mortality in patients with chronic obstructive pulmonary disease. Thorax. 2005;60:925-931.
2. McGhan R, Radcliff T, Fish R, et al. Predictors of rehospitalization and death after a severe exacerbation of COPD. Chest. 2007;132:1748-1755.
3. Langsetmo L, Platt RW, Ernst P, et al. Underreporting exacerbation of chronic obstructive pulmonary disease in a longitudinal cohort. Am J Respir Crit Care Med. 2008;177:396-401.
4. Hurst JR, Donaldson GC, Quint JK, et al. Temporal clustering of exacerbations in chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2009;179:369-374.
5. Hurst JR, Wedzicha JA. The biology of a chronic obstructive pulmonary disease exacerbation. Clin Chest Med. 2007;28:525-536.
6. Global Initiative for Chronic Obstructive Lung Disease (GOLD) 2008. Global strategy for diagnosis, management, and prevention of COPD. www.goldcopd.org. Accessed May 27, 2009.
7. Rabe KF, Hurd S, Anzueto A, et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: GOLD executive summary. Am J Respir Crit Care Med. 2007;176:532-555.
8. Groenewegen KH, Postma DS, Hop WC, et al. Increased systemic inflammation is a risk factor for COPD exacerbations. Chest. 2008;133:350-357.
9. Hurst JR, Donaldson GC, Perera WR, et al. Use of plasma biomarkers at exacerbation of chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2006;174:867-874.
10. Takabatake N, Shibata Y, Abe S, et al. A single nucleotide polymorphism in the CCL1 gene predicts acute exacerbations in chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2006;174:875-885.
11. Sethi S, Sethi R, Eschberger K, et al. Airway bacterial concentrations and exacerbations of chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2007;176:356-361.
12. Murphy TF, Brauer AL, Eschberger K, et al. Pseudomonas aeruginosa in chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2008;177:853-860.
13. Sethi S, Wrona C, Eschberger K, et al. Inflammatory profile of new bacterial strain exacerbations of chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2008;177:491-497.
14. Papi A, Bellattato CM, Braccioni F, et al. Infections and airway inflammation in chronic obstructive pulmonary disease severe exacerbations. Am J Respir Crit Care Med. 2006;173:1114-1121.
15. Celli BR, MacNee W; ATS/ERS Task Force. Standards for the diagnosis and treatment of patients with COPD: a summary of the ATS/ERS position paper. Eur Respir J. 2004;23:932-946.
16. Williams DM, Bourdet SV. Chronic obstructive pulmonary disease. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 7th ed. New York, NY: McGraw Hill Co Inc; 2008:chap 29.
17. Hanania NA, Sharafkhaneh A. Update on the pharmacologic therapy for chronic obstructive pulmonary disease. Clin Chest Med. 2007;28:589-607.
18. Wise RA, Tashkin DP. Optimizing treatment of chronic obstructive pulmonary disease: an assessment of current therapies. Am J Med. 2007;120:S4-S13.
19. De Jong YP, Uil SM, Grotjohan HP, et al. Oral or IV prednisolone in the treatment of COPD exacerbations. Chest. 2007;132:1741-1747.
20. Quon BS, Gan WQ, Sin DD. Contemporary management of acute exacerbations of COPD. Chest. 2008;133:756-766.
21. Bustamante-Fermosel A, De Miguel-Yanes JM, Duffort-Falco M, et al. Mortality-related factors after hospitalization for acute exacerbation of chronic obstructive pulmonary disease: the burden of clinical features. Am J Emergency Med. 2007;25:515-522.
22. Groenewegen KH, Schols AM, Wouters EF. Mortality and mortality-related factors after hospitalization for acute exacerbation of COPD. Chest. 2003;124:459-467.
To comment on this article, contact rdavidson@jobson.com.






