US Pharm. 2012;37(4)(Compliance suppl):3-6.
Poor adherence to appropriate medication therapy has been shown to result in complications, death, and increased health care costs.1-4 Medication adherence in patients with chronic conditions such as diabetes, hypertension, hyperlipidemia, asthma, and depression is a significant problem requiring intervention.5-12 According to the World Health Organization’s (WHO) World Health Report 2003, the degree of medication nonadherence is so great and the consequences are of such concern that more people worldwide would benefit from efforts to improve medication adherence than from the development of new medical treatments.13 In fact, a number of studies have shown that, in developed countries, patients with chronic conditions have adherence rates of 50% to 60%, despite evidence that medication improves quality of life and prevents death.5-10 In developing countries, when poor access to health care, possible lack of diagnosis, and limited availability of medications are taken into account, poor adherence threatens all efforts to treat chronic conditions such as diabetes, depression, and HIV/AIDS.11
The rate of patients who persistently take their medication for a chronic condition drops most significantly after the first 6 months of therapy.14-17 Acceptable rates of adherence in some trials are 80% or greater, while those for HIV are considerably higher (95%).17 Of all medication-related hospital admissions in the United States, 33% to 69% are related to poor medication adherence. The resulting costs are approximately $100 billion annually.17 It has been estimated that 125,000 deaths per year in the U.S. can be attributed to medication nonadherence.18 A retrospective analysis of patients aged under 65 years that was conducted between 1997 and 1999 concluded that diabetic patients with poor medication adherence had a 30% yearly risk of hospitalization, while those with high adherence (defined as following the medication regimen 80%-100% of the time) had a 13% risk.19 In the same analysis, total health care spending for patients with low medication adherence was almost twice that of patients with high adherence.
It was estimated in 2001 that more than 89,000 deaths from cardiovascular disease would have occurred in hypertensive patients aged 40 years and older who were not receiving antihypertensive medication therapy.20 Patients who are diabetic or who have heart disease are 48% less likely to die prematurely when they are adherent to their medication regimen.21 In addition, asthma patients who are adherent to their medications are 11% less likely to have an emergency room (ER) visit or to be hospitalized.21
When counseling about medication adherence for the three major disease states—diabetes, hypertension, and hyperlipidemia—it is important to educate the patient about the consequences of not appropriately treating these conditions, which can result in heart attack, heart failure, stroke, paralysis, and potentially permanent and devastating alterations to their quality of life. Pharmacists must paint a picture of the situation and remind patients why they are taking the medication in the first place.
Defining Adherence
It has been said that a primary determinant of treatment success is adherence to therapy.22 As defined by the WHO, adherence is the degree to which the patient’s behavior is in agreement with the health care provider’s recommendations. This is a collaborative approach between the patient and the provider in which the patient’s values, lifestyle, and beliefs coincide with the provider’s medical advice and opinion. Compliance, which is often confused with adherence, refers to a patient’s obedience to therapy under the authority of the provider, rather than to a collaborative approach. Another term that relates to adherence is persistence, which is the patient’s ability to continue taking the medication for the duration of treatment. When a medication is initiated, discussing the intended course of therapy with the patient has been shown to help keep the patient persistently following his or her medication regimen.12
Factors That Impact Adherence
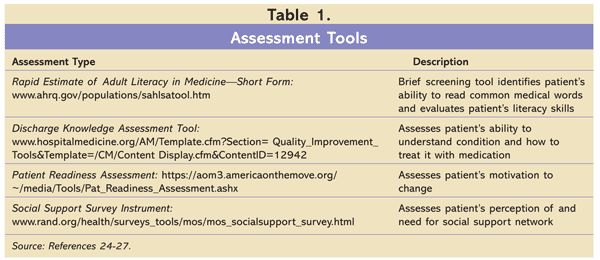
The most consistently reported factors impacting adherence are low literacy, lack of health insurance coverage, poor social support, family instability, and homelessness.12 Forty-five percent of U.S. adults have a literacy level at or below eighth grade.12 It has been reported that one-half of adults lack the skills to complete tasks related to following medication-label directions, comprehending nutrition labels, describing symptoms, or using a map to locate health facilities.23 This can be a particular problem in ethnic groups that already have a low English-literacy level. Decreased health literacy has been reported with increasing age, such that adults aged 60 years may not understand basic materials such as medication labels. See TABLE 1 for tools used both to assess health literacy, medication literacy, and willingness to change behaviors and to evaluate the degree of social support available to the patient.24-27 Patient beliefs about the diagnosis and medication benefits also have been shown to affect the adherence rate regardless of whether the patient can afford the medication. This means that patients may have a low perceived need for the medication and more concerns about side effects, thus possibly choosing to forgo the cost of the medication based on their beliefs.28
As providers, pharmacists can use the patient education program Ask Me 3, which is designed to promote communication between health care providers and patients, to improve adherence and outcomes. The Ask Me 3 questions are: What is my main problem? What do I need to do? and Why is it important for me to do this?29 Pharmacists should instruct their patients to ask these three questions, and they should state them to the patient and answer them in the event that the patient does not ask. It is equally important that the patient rephrase what the pharmacist has communicated in order to verify the patient’s comprehension and to clarify whether the information fits the patient’s beliefs. When answering these questions, particularly with asymptomatic patients, it is helpful for pharmacists to remind patients of the consequences of failing to take their medication, such as a devastating or life-ending event (heart attack or stroke) in patients with cardiovascular disease.
Prerequisites for medication adherence may include being interested in one’s health and understanding the diagnosis; comprehending the impact or potential impact of the diagnosis; believing that what has been prescribed will help; and knowing precisely how to take the medication and for how long. Other prerequisites may be determining how to fit the medication into one’s daily routine; valuing the results of treatment more than the cost of therapy; believing that one can fulfill the treatment plan; and feeling that the provider has true concern for the patient as a person, as opposed to just treating the disease.12
The following steps have been shown to increase adherence: verifying the patient’s understanding of the disease and its treatment and providing education where gaps in understanding exist; correlating medication-taking with other daily routines; using medication organizers or charts; reducing the pill burden, if possible; providing care support (i.e., health care team); and recognizing any struggles or other sociobehavioral issues that may affect adherence.12
How to Overcome Adherence Challenges
Many different factors can affect adherence. The first step, and the one that is most often missed, is to identify which factors are preventing adherence. One way to identify adherence gaps is to perform a medication reconciliation—best done using pharmacy adjudication records—allowing for discovery of pharmacy-dispensing gaps. This might reveal the need for a simplification of the dosing regimen.30 See TABLE 2 for a list of factors that affect adherence and strategies for overcoming them.29,31,32

Strategies to overcome low health literacy include creating a shame-free environment that promotes open dialogue; using plain language versus medical terminology; providing written communication on a fifth-grade level; using picture or video instruction; involving family members in the instruction; having the patient repeat the instruction; and following up by telephone to confirm the patient’s understanding.12
The inability to pay for health care can be a deterrent to adequate adherence; however, the degree to which patients value their medication or perceive it to help their condition, along with their beliefs about side effects, can influence their decision to forgo treatment, regardless of cost.28 Patients with depression show a greater tendency to be deterred by their beliefs and medication costs, thereby putting those with diabetes and depression at even greater risk for medication nonadherence. This is true for patients who have depression with other comorbid conditions. Providers should initiate more in-depth discussions about medication cost concerns in patients with depression.28
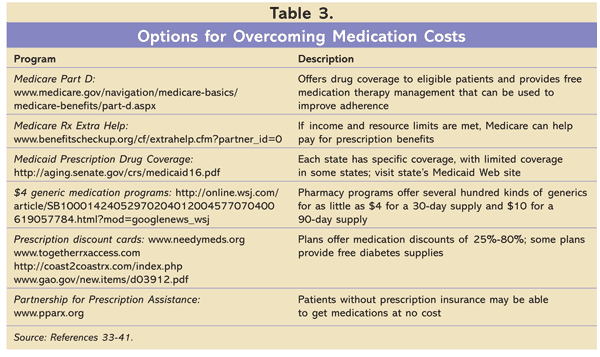
Lack of prescription coverage can be a major roadblock to medication adherence. There are several options for patients who do not have prescription coverage, including Medicare Part D (for patients eligible for Medicare), Medicare Extra Help (for those who have Medicare but have limited income and resources), Medicaid programs, the Together Rx Access Card (25%-40% off brand-name prescription products), Partnership for Prescription Assistance (free medications to qualified patients), NeedyMeds Drug Discount Card (80% off the price of prescriptions), Coast2Coast Rx Card (free diabetes supplies and up to 55% off medication costs), and discount cards offered by some pharmacy benefit management companies and individual pharmaceutical companies.33-40 This list of discount cards is not all-inclusive. The $4 generic program is another option offered by some large chain pharmacies and supermarket pharmacies; in some cases, independent pharmacies offering this program may match pricing.41 All of these discount programs have restrictions, so check their respective Web sites (TABLE 3).33-41 Lastly, some employers offer reduced copayments or medication deductibles to patients who participate in a health program for chronic diseases.42
Conclusion
Poor adherence to medication regimens is multifactorial, involving the patient’s beliefs about and understanding of the diagnosis and how the medication will help his or her prognosis.22 Three important questions to answer for the patient are: What is the patient’s main problem? What does the patient need to do? and Why is it important for the patient to do this? After these questions have been answered, ascertain that the patient believes that this treatment will help. Afterward, probe for any issues that may result in low adherence, such as low literacy, inability to pay for the medication, and poor social support, among many others.29 The first step is to check medication adherence and persistence by way of a pharmacy medication reconciliation that utilizes pharmacy adjudication claims.12
REFERENCES
1. McDonnell PJ, Jacobs MR. Hospital admissions resulting from preventable adverse drug reactions. Ann Pharmacother. 2002;36:1331-1336.
2. Schiff GD, Fung S, Speroff T, McNutt RA. Decompensated heart failure: symptoms, patterns of onset, and contributing factors. Am J Med. 2003;114:625-630.
3. Senst BL, Achusim LE, Genest RP, et al. Practical approach to
determining costs and frequency of adverse drug events in a health care
network. Am J Health Syst Pharm. 2001;58:1126-1132.
4. Rodgers PT, Ruffin DM. Medication nonadherence: part II—a pilot study in patients with congestive heart failure. Manag Care Interface. 1998;11:67-69,75.
5. Benner JS, Glynn RJ, Mogun H, et al. Long-term persistence in use of statin therapy in elderly patients. JAMA. 2002;288:455-461.
6. Avorn J, Monette J, Lacour A, et al. Persistence of use of lipid-lowering medications: a cross-national study. JAMA. 1998;279:1458-1462.
7. Feldman R, Bacher M, Campbell N, et al. Adherence to pharmacologic management of hypertension. Can J Public Health. 1998;89:116-118.
8. Flack J, Novikov SV, Ferrario CM. Benefits of adherence to anti-hypertensive drug therapy. Eur Heart J. 1996;17(suppl A):16-20.
9. Mallion JM, Baguet JP, Siche JP, et al. Compliance, electronic monitoring and antihypertensive drugs. J Hypertens Suppl. 1998;16:S75-S79.
10. Haynes RB, McKibbon KA, Kanani R. Systematic review of randomised
trials of interventions to assist patients to follow prescriptions for
medications. Lancet. 1996;348:383-386.
11. World Health Organization. Adherence to long-term therapies:
evidence for action.
www.who.int/hiv/pub/prev_care/lttherapies/en/index.html. Accessed
January 1, 2012.
12. Adult Meducation. Social and economic factors, health care system
related-factors, condition-related factors, therapy-related factors,
patient-related factors. (Note: As of February 28, 2012, this Web site is no longer accessible; for a copy of this reference, contact the author.)
13. Bosworth HB, Granger BB, Mendys P, et al. Medication adherence: a call for action. Am Heart J. 2011;162:412-424.
14. Jackevicius CA, Mamdani M, Tu JV. Adherence with statin therapy
in elderly patients with and without acute coronary syndromes. JAMA. 2002;288:462-467.
15. Cramer J, Rosenheck R, Kirk G, et al. Medication compliance
feedback and monitoring in a clinical trial: predictors and outcomes. Value Health. 2003;6:566-573.
16. Haynes RB, McDonald HP, Garg AX. Helping patients follow prescribed treatment: clinical applications. JAMA. 2002;288:2880-2883.
17. Osterberg L, Blaschke T. Adherence to medication. N Engl J Med. 2005;353:487-497.
18. McCarthy R. The price you pay for the drug not taken. Bus Health. 1998;16:27-28,30,32-33.
19. Sokol MC, McGuigan KA, Verbrugge RR, Epstein RS. Impact of
medication adherence on hospitalization risk and healthcare cost. Med Care. 2005;43:521-530.
20. Cutler DM, Long G, Berndt ER, et al. The value of antihypertensive drugs: a perspective on medical innovation. Health Aff (Millwood). 2007;26:97-110.
21. National Priorities Partnership, in collaboration with NEHI. Improving Patient Medication Adherence: A $100+ Billion Opportunity. Washington, DC: National Priorities Partnership; April 2011.
22. Jimmy B, Jose J. Patient medication adherence: measures in daily practice. Oman Med J. 2011;26:155-159.
23. Office of the Surgeon General. Surgeon General’s workshop on
improving health literacy.
www.surgeongeneral.gov/topics/healthliteracy/panel1.htm. Accessed
January 2, 2012.
24. Agency for Healthcare Research and Quality. Health literacy
measurement tools. www.ahrq.gov/populations/sahlsatool.htm. Accessed
February 28, 2012.
25. Society of Hospital Medicine. Discharge knowledge assessment
tool.
www.hospitalmedicine.org/AM/Template.cfm?Section=Quality_Improvement_Tools&Template=/CM/ContentDisplay.cfm&ContentID=12942.
Accessed February 28, 2012.
26. America on the Move. Patient readiness assessment.
https://aom3.americaonthemove.org/~/media/Tools/Pat_Readiness_Assessment.ashx.
Accessed February 28, 2012.
27. Rand Health. Medical outcomes study: social support survey
instrument.
www.rand.org/health/surveys_tools/mos/mos_socialsupport_survey.html.
Accessed February 28, 2012.
28. Piette JD, Beard A, Rosland AM, McHorney CA. Beliefs that
influence cost-related medication non-adherence among the “haves” and
“have nots” with chronic diseases. Patient Prefer Adherence. 2011;5:389-396.
29. National Patient Safety Information. Ask Me 3: good questions for
your good health.
www.npsf.org/wp-content/uploads/2011/12/AskMe3_WordsToWatch_English.pdf.
Accessed January 3, 2012.
30. NEHI. Thinking outside the pillbox: a system-wide approach to
improving patient medication adherence for chronic disease.
www.nehi.net/publications/44/thinking_outside_the_pillbox_a_systemwide_approach_to_improving_patient_medication_adherence_for_chronic_disease.
Accessed January 9, 2012.
31. PDFCast.org. Dimension 1: social and economic factors.
http://pdfcast.org/pdf/social-and-economic-factors. Accessed February
28, 2012.
32. U.S. Pharmacopeial Convention. USP pictograms. www.usp.org/audiences/consumers/pictograms. Accessed February 28, 2012.
33. Medicare.gov. Medicare prescription drug coverage (Part D).
www.medicare.gov/navigation/medicare-basics/medicare-benefits/part-d.aspx.
Accessed January 10, 2012.
34. BenefitsCheckUp. Medicare Rx extra help application.
www.benefitscheckup.org/cf/extrahelp.cfm?partner_id=0. Accessed January
10, 2012.
35. Hearne J. CRS report for Congress. Prescription drug coverage
under Medicaid. http://aging.senate.gov/crs/medicaid16.pdf. Accessed
January 10, 2012.
36. Together Rx Access. www.togetherrxaccess.com. Accessed January 10, 2012.
37. Partnership for Prescription Assistance. www.pparx.org. Accessed January 10, 2012.
38. NeedyMeds. www.needymeds.org. Accessed January 10, 2012.
39. Coast2CoastRx.com. Coast2Coast Rx card. http://coast2coastrx.com/index.php. Accessed January 10, 2012.
40. GAO. Prescription Drug Discount Cards. Savings Depend on Pharmacy and Type of Card Used. Washington, DC: U.S. General Accounting Office; 2003.
41. Gerencher K. Save at the drug store.
http://online.wsj.com/article/SB10001424052970204012004577070400619057784.html?mod=googlenews_wsj.
Accessed December 10, 2011.
42. Bunting BA, Lee G, Knowles G, et al. The Hickory Project:
controlling healthcare costs and improving outcomes for diabetes using
the Asheville Project model. Am Health Drug Benefits. 2011;4:343-350.
To comment on this article, contact rdavidson@uspharmacist.com.






