US Pharm.2016;41(3):31-35.
ABSTRACT: The National Pain Strategy (NPS) is a comprehensive population health-level plan that addresses the issue of inadequate pain management in the United States, as well as the national opioid-abuse epidemic. Currently, the draft version is undergoing revisions. The National Pain Strategy focuses on six important areas of need in pain management: population research, prevention and care, disparities, service delivery and reimbursement, professional education and training, and public awareness and communication. Each of these key areas has direct implications for the pharmacy profession, and pharmacists will have the opportunity to play an active role in the optimal management of patients’ pain.
In 2011, the Institute of Medicine (IOM) published a report entitled Relieving Pain in America in response to a congressional mandate to increase the recognition of pain as a significant public-health problem in the United States.1 In its report, the IOM called for a cultural transformation in pain prevention, care, education, and research, and recommended the development of a comprehensive population health-level strategy.1 In response to this call, the U.S. Department of Health and Human Services (HHS) charged the Interagency Pain Research Coordinating Committee with overseeing the development of what would eventually become known as the National Pain Strategy (NPS).2 The NPS, the draft version of which is currently undergoing revision, offers guidance on enhancing the recognition and management of pain by focusing on six key areas. Each of these key areas has direct implications for the pharmacy profession.
Population Research
The IOM’s report made it clear that more information is needed on the prevalence, onset, course, impact, and outcomes of most common chronic pain conditions.1 Healthcare organizations and insurers would be able to use this information to help guide policies and initiatives. To achieve this goal, the NPS has proposed the use of pain-screening questions and brief self-assessment questions about high-impact chronic pain.2 These questions may be incorporated into a healthcare organization’s electronic health record system. In addition, validated pain-assessment tools that target specific patient populations (e.g., dementia patients, the elderly) are available.3
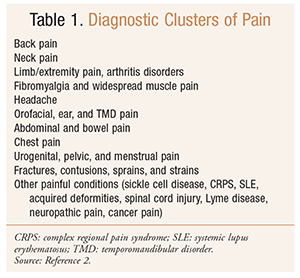
The NPS calls for the use of standardized electronic healthcare data from large healthcare databases to identify patterns of pain treatment among patients in specified diagnostic clusters (TABLE 1). As increasingly more healthcare facilities merge or develop affiliations, this goal could become a reality through effective communication. There is also a push to make adequate pain measures a component of the Centers for Medicare & Medicaid Services’ incentive programs on “meaningful use” of electronic health records. The NPS encourages the establishment of pain-research networks to study risk factors for the initiation and maintenance of chronic pain and high-impact chronic pain and to examine patterns of pain treatment using diagnostic clusters and pain-treatment indicators. Large healthcare networks may be ideally positioned to achieve these goals.2
The NPS advocates the longitudinal assessment of pain. The electronic health record may be an excellent tool to track changes in pain prevalence, the impact of treatment, and the costs of pain management over time. As identified in Healthy People 2020, national pain goals include reducing the prevalence of high-impact chronic pain and increasing the use of preventive services for chronic pain.4
Data gathered from the proposed NPS interventions should be used to guide enhancements to healthcare and preventive services. Demonstration projects examining these issues within healthcare organizations are also encouraged.2
Prevention and Care
The NPS calls for the identification of preventable causes of both acute and chronic pain and ways to avoid their occurrence throughout the healthcare delivery system. However, when pain is present, the proper use of clinical practice guidelines in pain management should be employed. The NPS recommends the use of an interdisciplinary team approach to pain management. Further, the NPS stresses the need for continuity of care during transitions of care.2
Healthcare facilities can undertake a cost-benefit analysis to identify high-yield pain-management interventions for both prevention and treatment. Based on work from the field, the most effective and cost-efficient treatments should be incorporated into practice guidelines and other best-practice initiatives. Treatment outcomes should take into account outcomes on pain, level of disability, and the psychosocial impact of pain.2
The NPS addresses the lack of pain self-management programs nationwide, identifying this as an unmet opportunity to provide patients with appropriate skills, education, and resources to actively manage their pain. It proposes that pain self-management programs be integrated into healthcare systems, with goal setting, problem solving, decision making, and psychosocial aspects of care as targets.2
The gold standard for pain assessment involves patient self-assessment. Healthcare facilities can improve patient care by integrating appropriate pain-assessment tools into the electronic health record. They can also pilot new pain-assessment tools and determine the cost-benefit ratio of these instruments.2
Health Disparities
Healthy People 2020 defines a health disparity as “a particular type of health difference that is closely linked with social, economic, and/or environmental disadvantage.”4 The NPS goes a step further, including all higher-risk groups that comprise vulnerable populations and addressing negative healthcare provider (HCP) attitudes and behaviors toward pain that may lead to discrimination, bias, or stigma. Negative HCP attitudes may lead to patient unwillingness to report pain and decreased patient participation in decision making and treatment plan follow-up. Populations at risk for experiencing healthcare disparities include women exhibiting pain associated with chronic fatigue syndrome, fibromyalgia, and other conditions; elderly nursing home patients; minority patients with sickle cell disease; and patients with HIV-associated pain. Healthcare organizations can eliminate disparities in pain assessment and management by increasing access to high-quality pain treatment; developing strategies and expectations for equitable assessment and treatment of pain; creating appropriate supporting programs and services for patients with pain; and improving communication between HCPs and patients and their families or caregivers.2
The first step in addressing a problem is identifying its existence. The NPS encourages healthcare organizations to conduct baseline surveys of HCPs’ biases, attitudes, beliefs, knowledge, and behaviors regarding pain, especially as they pertain to vulnerable populations. If a problem is identified, strategies should be developed to overcome bias and identify gaps in knowledge. To combat disparities in their organization, healthcare facilities are urged to conduct demonstration projects based on the results of pilot pain projects.2
Healthcare organizations should promote awareness of patient and provider resources that can connect people with chronic pain to appropriate care. Healthcare facilities can create interactive Web-based gateway programs to link information and pain-management resources to patients and their families. A potential resource is Healthfinder.gov.5 Telemedicine consultations and training programs for hard-to-reach populations and for clinicians who do not practice in a multidisciplinary setting are other methods that healthcare networks can implement to help eliminate disparities. Facilities should be offered financial incentives to adopt effective models that minimize health disparities. Useful metrics would be the changes in prevalence of untreated or inadequately treated pain in vulnerable groups.
Healthcare institutions should facilitate communication regarding pain assessment and management between patients and HCPs in order to heighten awareness, eliminate disparities, and reduce the stigma associated with pain management. Efforts should be made to address the pain needs of patients with low English proficiency, low literacy, poor health literacy, or communication disabilities. There is a paucity of information on this subject. Pharmacists can play a significant role in enhancing appropriate medication use and promoting pain-medication literacy.6 Facilities should provide culturally and linguistically appropriate services to adequately address the pain needs of health-illiterate patients.7
Electronic health records can be used to track pain prevalence and treatment in vulnerable populations. For example, a Department of Veterans Affairs analysis of electronic health records identified disparity in pain assessment between black and white veterans.8 Costs (e.g., healthcare use, lost productivity or educational opportunities) associated with this disparity can be calculated.
Service Delivery and Reimbursement
The management of pain has shifted from a single-modality treatment to integrated, collaborative, multimodal, interdisciplinary, patient-centered care that is effective and safe. Pharmacists can play an integral role in this area. Pharmacist-physician collaboration in pain management can help optimize outcomes and minimize risks associated with potent analgesics.9 Healthcare facilities must do a better job of improving communication between clinicians and should take patient preferences regarding pain management into account. Evidence-based pain management should be incorporated into clinical practices. Facilities can seek out funding for pilot projects that evaluate innovative models of high-value, integrated care for chronic pain, including the stepped-care model, the biopsychosocial model, team-based care, pain self-management approaches, and/or comprehensive pain-assessment care planning. The impact of reimbursement innovations on quality measures and cost savings of pain care should also be evaluated.2
The NPS calls for the implementation of population-based studies using real-world settings to determine the efficacy, safety, and cost-effectiveness of pain-management strategies. This can be accomplished through the use of electronic health records and pain registries. Meeting clinical quality measures for pain can become part of institutions’ incentive programs for HCPs.2
Professional Education and Training
The NPS states that education is central to the necessary cultural transformation of the approach to pain, warning that “education and training of health professionals in the complex etiology, prevention, assessment, safe and effective treatment of pain, and risks associated with poor pain management is insufficient, in part because educators lack access to valid information about pain and pain care.”2 The NPS calls for “an attitudinal transformation toward pain and a reorganization of pain management by the health care system, in the education and training of health professionals,” including pharmacists.2
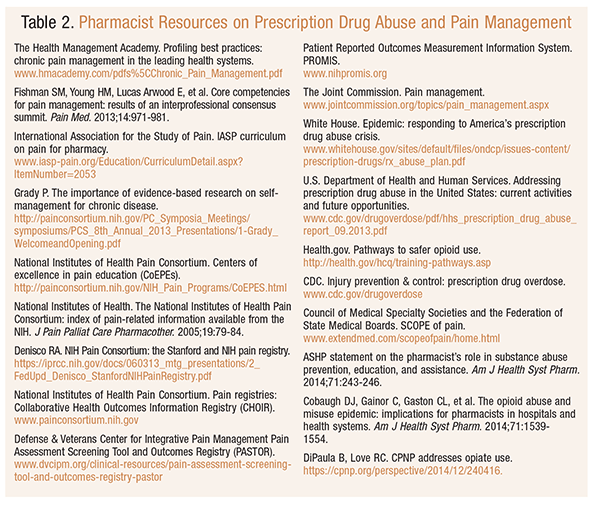
Opportunities exist for pharmacists to enhance their skills in this area (TABLE 2). A listing of certification programs for pharmacists identified two credentialing organizations (the American Society of Pain Educators and the American Academy of Pain Management) in which pharmacists can become credentialed pain educators or practitioners.10 A review of the American Society of Health-System Pharmacists (ASHP) website found 13 postgraduate year 2 (PGY-2) residencies in palliative care/pain management available in the U.S. in 2016.11 The ASHP Foundation offers a traineeship in pain management and palliative care.12 The NPS advises that the demonstration of competency in the areas of pain assessment, safe and effective pain care, and prescription analgesic–associated risks should be a requirement for licensure and certification of HCPs and should be considered in curriculum review for accreditation of HCP training programs. The NPS also advocates for subspecialty training and certification in effective team management for patients with the most complex pain conditions.2
Healthcare systems can play a major role in this area during the preceptorship of undergraduates and by sponsoring pharmacy residencies and fellowships in pain management, developing position-specific core competencies, being active members of interdisciplinary pain or palliative-care teams, and fostering ongoing education programs in pain management for pharmacy staff.2
Public Education and Communication
The NPS advocates a national pain-awareness campaign involving both public and private partner organizations. The focus of this national pain awareness campaign should be twofold: to increase public awareness about pain, and to promote safe medication use by patients. The NPS calls for an increased awareness of the prevalence, significance, nature, impact, features, and management of pain. This campaign should take health literacy and cross-cultural awareness into account and should be tailored to specific patient populations’ needs. Pharmacy departments in healthcare facilities may be ideally positioned to address these population-specific pain-management needs.2
Goals of the NPS are to foster public and private coalitions to promote the core message of the campaign that pain is, in fact, a disease; to debunk stereotypes and biases with respect to pain sufferers; and to promote safe medication use.2
Strategies have been identified that not only may reduce drug misuse, abuse, and diversion, but also may result in cost savings from avoidance of misadventures. Among the interventions that healthcare facilities can implement are extensive physician and patient education regarding opiates and their associated abuse; use of electronic health records to detect inappropriate prescribing and medical errors; use of physician-patient contracts during opioid treatment; requiring photo identification to pick up an opioid prescription at an outpatient/ambulatory pharmacy; implementing urine toxicology screening; providing patients with options for safe disposal of unused opioids; referring difficult-to-manage patients or patients with a substance-abuse disorder to pain and addiction specialists; and encouraging the use of deterrent-containing opioid formulations in outpatient formularies.13 The NPS has identified objectives and potential outcome measures for the safe use of pain medications (TABLE 3).2

The HHS Behavioral Health Coordinating Committee’s Subcommittee on Prescription Drug Abuse has published a report on current activities and future opportunities for addressing prescription drug abuse.14 The purpose of this report is to improve the understanding of current prescription drug abuse activities, provide a review of current initiatives, and identify opportunities to ensure the safe use of prescription drugs with abuse potential and the treatment of prescription drug dependence.14 To further these goals, in October 2015 the Obama Administration announced public and private efforts to address prescription drug abuse and heroin use.15
Conclusion
The NPS, although still in draft form, offers pharmacists and healthcare systems the opportunity to play an active role in the optimal management of patients experiencing pain. It also promotes the safe and appropriate use of medication in this patient population.
REFERENCES
1. Institute of Medicine. Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research. Washington, DC: The National Academies Press; 2011.
2. Interagency Pain Research Coordinating Committee. National Pain Strategy: a comprehensive population health-level strategy for pain. http://iprcc.nih.gov/docs/DraftHHSNationalPainStrategy.pdf. Accessed September 8, 2015.
3. Lisi DM. Pain assessment for pharmacists: a primer. US Pharm. 2015;40(3):53-63.
4. HealthyPeople.gov. Healthy People 2020. www.healthypeople.gov. Accessed September 8, 2015.
5. U.S. Department of Health and Human Services (HHS). Healthfinder.gov. http://healthfinder.gov. Accessed September 8, 2015.
6. Chang FC, Chi HY, Huang LJ, et al. Developing school-pharmacist partnerships to enhance correct medication use and pain medication literacy in Taiwan. J Am Pharm Assoc (2003). 2015;55:595-602.
7. HHS. National standards for culturally and linguistically appropriate services (CLAS) in health and health care. www.thinkculturalhealth.hhs.gov/pdfs/enhancednationalclasstandards.pdf. Accessed October 19, 2015.
8. Burgess DJ, Gravely AA, Nelson DB, et al. A national study of racial disparity in pain screening rates in the VA health care system. Clin J Pain. 2013;29:118-123.
9. Strickland JM, Huskey A, Brushwood DB. Pharmacist-physician collaboration in pain management practice. J Opioid Manag. 2007;3:295-301.
10. Council on Credentialing in Pharmacy. Certification programs for pharmacists. www.pharmacycredentialing.org/files/certificationprograms.pdf. Accessed November 10, 2015.
11. American Society of Health-System Pharmacists (ASHP). Online residency directory. https://accred.ashp.org/aps/pages/directory/residencyprogramsearch.aspx. Accessed November 10, 2015.
12. ASHP Foundation. Pain management and palliative care traineeship. www.ashpfoundation.org/MainMenuCategories/Traineeships/PainMgmtTraineeship. Accessed November 10, 2015.
13. Hahn KL. Strategies to prevent opioid misuse, abuse, and diversion that may also reduce the associated costs. Am Health Drug Benefits. 2011;4:107-114.
14. HHS. Addressing prescription drug abuse in the United States. www.cdc.gov/drugoverdose/pdf/hhs_prescription_drug_abuse_report_09.2013.pdf. Accessed November 10, 2015.
15. White House. Fact Sheet: Obama Administration announces public and private sector efforts to address prescription drug abuse and heroin use. www.whitehouse.gov/the-press-office/2015/10/21/fact-sheet-obama-administration-announces-public-and-private-sector. Accessed November 10, 2015.
To comment on this article, contact rdavidson@uspharmacist.com.





