US Pharm. 2010;35(5):HS16-HS20.
Despite the availability of various therapeutic approaches to pain management and an improved understanding of pain pathophysiology, acute pain continues to be undertreated or treated ineffectively.1 In particular, postoperative pain that is not adequately relieved increases patient burden and the risk of subsequent complications, including the development of chronic pain syndromes.2 Opioid analgesics are often used to manage postoperative pain but are associated with a high incidence of adverse effects (AEs) such as nausea, vomiting, constipation, oversedation, and respiratory depression.2,3 Alternate means of analgesia are needed to decrease the incidence of opioid-related AEs, including the utilization of agents that exert analgesic effects through differing mechanisms of action.
Several studies have found that the use of non-steroidal anti-inflammatory drugs (NSAIDs), such as ketorolac, decrease opioid requirements and may decrease the incidence of AEs when compared to opioids.4-6 Additionally, IV ketorolac may be more cost-effective than IV morphine.7 Parenteral ketorolac tromethamine (Toradol) has been effectively used to treat postoperative pain for several decades. However, its use is limited to a 5-day treatment duration due to an increased risk of gastrointestinal (GI) bleeding.8 In June 2009, a parenteral formulation of ibuprofen (Caldolor) was approved for acute pain and can be used as monotherapy or in combination with opioids.9 Parenteral ketorolac tromethamine and IV ibuprofen (IVib) are reviewed to determine their role in acute pain management, specifically within the postoperative setting.
Pharmacokinetics
Ketorolac Tromethamine: Ketorolac tromethamine is a racemic mixture of (-)S and (+)R enantiomers, with the S-form having analgesic activity. It has been shown to be highly protein bound (99%) and will occupy approximately 5% of albumin binding sites even when administered in high concentrations.8 Ketorolac tromethamine is excreted in human milk, and its use is contraindicated in nursing mothers. Metabolism of ketorolac tromethamine occurs in the liver via hydroxylation and conjugation, and its metabolites and unchanged drug are excreted in the urine. Following a single dose, about 92% of drug is found in the urine, approximately 40% as metabolites, and 60% as unchanged ketorolac.8
IVib: Similar to ketorolac, IVib is formulated as an aqueous, racemic mixture with the (+)S-isomer producing its clinical activity. The (-)R form is partially converted to the active (+)S form in adults and serves as a reservoir to maintain levels of active drug.9 It is highly plasma protein bound (>99%), and its volume of distribution can be altered based on age and the presence of fever. The mean elimination half-life for IVib is similar after the administration of either a 400 mg or an 800 mg dose as an infusion over 60 minutes (2.22 and 2.44 hours, respectively).9 It is hepatically metabolized and renally eliminated.
Formulation and Dosing
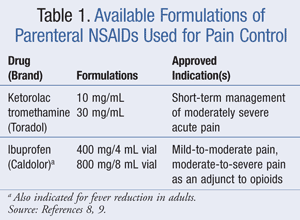
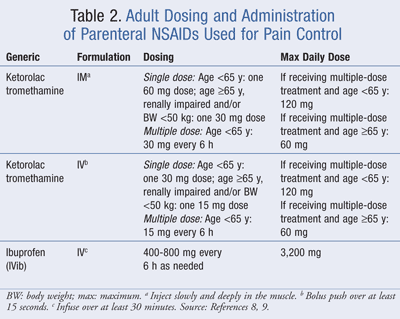
In 1998, Tramèr et al performed a systematic literature review examining the effects of various routes of NSAID administration on efficacy and AEs.10 In postoperative pain, the authors noted that ketorolac administered via IV and intramuscular (IM) routes did not show any difference in efficacy. Ultimately, direct conclusions could not be drawn when comparing drug formulation and efficacy. Adverse effects appeared to be independent of route of administration; however, IM injections were more commonly associated with injection site pain. To date, with the exception of a bioequivalence study by Chassard et al comparing IV ibuprofen to IM ibuprofen,11 studies have not been performed that compare IVib to other ibuprofen formulations to determine efficacy. Current formulations of parenteral ketorolac and ibuprofen that are indicated for pain control are listed in TABLE 1, and dosing for these agents is given in TABLE 2.
Tolerability
Ketorolac Tromethamine: In studies evaluating ketorolac tromethamine, AEs that occurred in more than 1% of patients included headache, nausea, flatulence, constipation/diarrhea, dizziness, anemia, and stomatitis. Nausea and headache were reported by more than 10% of included patients.8 In a large, observational postmarketing study of 10,000 patients receiving ketorolac tromethamine, the risk for the development of clinically serious GI bleeding was considered to be dose dependent, with a higher incidence occurring in patients who were older than 65 years of age, particularly if they were receiving daily doses greater than 60 mg/day for up to 5 days.8 For patients with a history of GI perforation, ulcer, or bleeding, the risk for serious GI bleeding increased significantly, especially with increasing age. Because of its ability to decrease prostaglandin production, ketorolac tromethamine can cause GI and renal toxicity and should be used judiciously in patients with underlying disorders of these organ systems.
IVib: The most commonly reported AE from the pain studies involving IVib was nausea; however, it is important to consider that all of these patients also received anesthesia and postoperative morphine.12-14 Other common AEs occurring in more than 5% of patients included flatulence, headache, and hemorrhage. In studies evaluating IVib for fever reduction in hospitalized adults, the most commonly reported AEs were related to blood dyscrasias.15-18 There were no significant renal events occurring in any of the IVib clinical studies.12-18 Due to the assumed risk of renal toxicity associated with the use of any parenteral NSAID, renal adverse events can be avoided with adequate hydration prior to drug administration.9 Additionally, the incidence of hematologic events did not differ significantly from the control group in any study; in patients with major bleeds, the rate of need for transfusion did not differ from the placebo group.
Drug Interactions
Ketorolac Tromethamine: The use of ketorolac tromethamine is contraindicated in patients who are currently taking other NSAIDs (due to cumulative toxicity), pentoxifylline (increased bleeding), and probenecid (increased ketorolac concentration).8 It should be used cautiously in patients taking lithium, diuretics, anticoagulants/antiplatelet drugs, methotrexate, angiotensin-converting enzyme (ACE) inhibitors, and selective serotonin reuptake inhibitors (SSRIs).
IVib: With the exception of a study on fever reduction in patients with malaria, IVib has been studied only in combination with morphine.12 Additional studies are needed to determine the extent of drug interactions with regard to the use of IVib in hospitalized patients for pain or fever. However, based on class pharmacologic activity, IVib may diminish the antihypertensive effects of ACEIs. Additionally, use should be avoided in combination with aspirin or any other NSAIDs due to the increased risk for bleeding and other adverse effects. It is also important to note that pharmacokinetic variables were altered when IVib was evaluated in critically ill, febrile adults, which may indicate the need for higher doses to achieve effective fever reduction in this population.16,17
Efficacy
Ketorolac Tromethamine: The efficacy of ketorolac is well established. Ketorolac is often used to decrease the demand for postoperative opioid analgesics.6 One study found that ketorolac used in combination with patient-controlled epidural analgesia (PCEA) after a cesarean delivery resulted in a 30% reduction in meperidine dose requirements.6 Another study found that when ketorolac was used in combination with fentanyl, patients required lower fentanyl doses to provide the same level of pain relief as compared to higher doses of fentanyl alone in the setting of thyroid surgery.5 Studies similar to these are extensive and have resulted in ketorolac becoming a mainstay in postoperative pain management.
IVib: In a study of 406 patients undergoing elective orthopedic or abdominal surgery, the use of IVib 800 mg every 6 hours (in combination with morphine via patient-controlled analgesia [PCA] or nurse administration) was associated with a significant reduction in median morphine requirements compared to placebo (P = .030) within the first 24 hours after surgery.12 Additionally, during postoperative hours 1 through 24, the group receiving IVib 800 mg experienced improved pain relief at rest and with movement versus the placebo group (P <.001 and P = .002, respectively). Patients who received IVib 400 mg every 6 hours demonstrated significant reductions in pain at rest and with movement compared to those receiving placebo (P = .013 and P = .021, respectively). Nonetheless, it is important to note that although pain relief was improved in groups receiving IVib 400 mg or 800 mg, this was evaluated as a secondary end point, and additional studies utilizing clinically meaningful outcomes (e.g. pain relief, improved ambulation) are warranted.
Role in Children
While many studies of parenteral NSAIDs in children have been conducted in premature infants for closure of patent ductus arteriosus, other studies have focused on postoperative and acute pain control. Efficacy with parenteral NSAIDs has been reported for pain control following spinal and cardiothoracic surgery.19,20 The use of ketorolac in combination with morphine in infants aged 6 to 18 months for postoperative pain did not show a significant decrease in morphine usage, nor did it show an increase in AEs.21 Ketorolac has also been studied with mixed results in children when used with morphine for sickle cell crisis.22 Of note, when provided with the option to use a parenteral NSAID containing polyethylene glycol and benzyl alcohol in children or to use preservative-free formulations (e.g., ibuprofen lysine [NeoProfen]), the preservative-free formulation may be preferable.23,24 With appropriate dosing and monitoring, parenteral NSAIDs may provide an appropriate therapeutic option in children for short-term pain control when opioids are not wanted or are unnecessary.
Role of the Pharmacist
With the increasing number of drugs and drug formulations available within the United States, pharmacists continue to be uniquely positioned within the health care system to promote the safe and effective use of these agents. The increasing attention to the safety profile for NSAIDs has recently overshadowed the benefit that this class of drugs has for many inflammatory and pain disorders. Although there are differences with regard to clinical efficacy within the NSAID class, the adverse effects for these drugs remain consistent throughout the class and can occur regardless of formulation. Pharmacists should continue to encourage the use of NSAIDs while employing drug-specific monitoring parameters to ensure their safety, as well as consider opportunities for synergistic use, particularly in the setting of postoperative analgesia.
Conclusion
The use of NSAIDs for analgesia is well documented, and the use of parenteral NSAIDs for acute pain management either alone or in combination with opioids is also established. Parenteral NSAIDs are used as an analgesic option for postoperative pain, for renal colic, and now for fever in adults.5,6,9,10,12 Until recently, parenteral ketorolac tromethamine was the only parenteral NSAID available in the U.S. with an approved indication for analgesia. The availability of IVib makes it another option for analgesia, particularly in the postoperative setting, to potentially reduce opioid requirements and the risk of AEs associated with higher doses of such analgesics. To date, there have been no trials on comparative efficacy between IV ketorolac and IVib. It is known that ketorolac is an effective postoperative analgesic option for patients experiencing acute pain, and IVib is approved for this indication as well. In addition, IVib is not restricted by duration of treatment (although it has only been studied for up to 5 days) and carries a second indication for fever reduction in hospitalized adults. However, the advantages to the use of one agent over the other remain unknown, and patient- and health care system–specific factors should continue to guide choice in therapy.
REFERENCES
1. Brennan F, Carr DB, Cousins M. Pain management: a fundamental human right. Anesth Analg. 2007;105:205-221.
2. Carr DB, Jacox AK, Chapman CR, et al. Acute Pain Management: Operative or Medical Procedures and Trauma. Clinical Practice Guideline. Rockville, MD: Agency for Health Care Policy and Research, Public Health Service, U.S. Department of Health and Human Services; 1992. AHCPR Pub No. 92-0032.
3. Vila H, Smith RA, Augustyniak MJ, et al. The efficacy and safety of pain management before and after implementation of hospital-wide pain management standards: is patient safety compromised by treatment based solely on numerical pain ratings? Anesth Analg. 2005;101:474-480.
4. Oderda GM, Said Q, Evans RS, et al. Opioid-related adverse drug events in surgical hospitalizations: impact on costs and length of stay. Ann Pharmcother. 2007;41:400-406.
5. Kim SY, Kim EM, Nam KH, et al. Postoperative intravenous patient-controlled analgesia in thyroid surgery: comparison of fentanyl and ondansetron regimens with and without the nonsteroidal anti-inflammatory drug ketorolac. Thyroid. 2008;18:1285-1290.
6. Pavy TJ, Paech MJ, Evans SF. The effect of intravenous ketorolac on opioid requirement and pain after cesarean delivery. Anesth Analg. 2001;92:1010-1014.
7. Rainer TH, Jacobs P, Ng YC, et al. Cost effectiveness analysis of intravenous ketorolac and morphine for treating pain after limb injury: double-blind randomised controlled trial. BMJ. 2000;321:1247-1251.
8. Toradol (ketorolac tromethamine) package insert. Nutley, NJ: Roche Pharmaceuticals; 2007.
9. Caldolor (ibuprofen injection) package insert. Nashville, TN: Cumberland Pharmaceuticals, Inc; 2009.
10. Tramèr MR, Williams JE, Carroll D, et al. Comparing analgesic efficacy of non-steroidal anti-inflammatory drugs given by different routes in acute and chronic pain: a qualitative systematic review. Acta Anaesthiol Scand. 1998;42:71-79.
11. Chassard D, Geneteau A, Gualano V, et al. Bioequivalence study of two ibuprofen formulations administered intravenously in healthy male volunteers. Clin Drug Invest. 2004;24:739-747.
12. Southworth S, Peters J, Rock A, Pavliv L. A multicenter, randomized, double-blind, placebo-controlled trial of intravenous ibuprofen 400 and 800 mg every 6 hours in the management of postoperative pain. Clin Ther. 2009;31:1922-1935.
13. Abdominal Hysterectomy Pain Study Group. A multi-center, randomized, double-blind, placebo-controlled trial of intravenous ibuprofen for treatment of pain in postoperative adult patients. Nashville, TN: Cumberland Pharmaceuticals, Inc; 2009 (data on file).
14. Orthopedic Pain Study Group. Efficacy and safety of intravenous ibuprofen in hospitalized adult orthopedic patients. Nashville, TN: Cumberland Pharmaceuticals, Inc; 2009 (data on file).
15. Single-Cause Fever Study Group. A single centre, randomized, double-blind, placebo-controlled trial to evaluate the efficacy and safety of ibuprofen in hospitalized febrile adult patients. Nashville, TN: Cumberland Pharmaceuticals, Inc; 2009 (data on file).
16. All-Cause Fever Study Group. A multi-center, randomized, double-blind, parallel, placebo-controlled trial to evaluate the efficacy, safety, and pharmacokinetics of ibuprofen injection in adult febrile subjects. Nashville, TN: Cumberland Pharmaceuticals, Inc; 2009 (data on file).
17. Morris P, Promes J, Guntapalli K, et al. A multi-center, randomized, double-blind, placebo-controlled trial of the efficacy and safety of intravenous ibuprofen in febrile adults. Crit Care Med. 2008;36(suppl):A65.
18. Fever and Pain Study Group. Efficacy and safety of intravenous ibuprofen in hospitalized burn patients. Nashville, TN: Cumberland Pharmaceuticals, Inc; 2009 (data on file).
19. Hayes J, Pehora C, Bissonnette B. The use of NSAIDs in pediatric scoliosis surgery—a survey of physicians’ prescribing practice. Paediatr Anaesth. 2009;19:756-763.
20. Dawkins TN, Barclay CA, Gardiner RL, Krawczeski CD. Safety of intravenous use of ketorolac in infants following cardiothoracic surgery. Cardiol Young. 2009;19:105-108.
21. Lynn AM, Bradford H, Kantor ED, et al. Postoperative ketorolac tromethamine use in infants aged 6-18 months: the effect on morphine usage, safety assessment, and stereo-specific pharmacokinetics. Anesth Analg. 2007;104:1040-1051.
22. Hardwick WE, Givens TG, Monroe KW, et al. Effect of ketorolac in pediatric sickle cell vaso-occlusive pain crisis. Pediatr Emerg Care. 1999;15:179-182.
23. Gandhi M, Prosser D. Our experience of Dyloject (intravenous diclofenac) in children. Paediatr Anaesth. 2009;19:908-929.
24. NeoProfen (ibuprofen lysine injection) package insert. Deerfield, IL: Lundbeck, Inc; 2010.
To comment on this article, contact rdavidson@uspharmacist.com.





