US Pharm. 2008;33(10):20-26.
In addition to lowering blood pressure, beta-blockers (TABLE 1) have been shown to reduce the risk of cardiovascular mortality and the incidence of cardiovascular events in high-risk patients with hypertension, such as those with coronary artery disease, previous myocardial infarction (MI), heart failure, or diabetes.1 In general, when using a beta-blocker to treat hypertension, a cardioselective beta-blocker has been preferred.2
While MI has been shown to be a leading cause of death in adults, those surviving MI have an increased risk of developing heart failure.3 The acute sympathetic nervous system activation accompanying MI becomes persistent in heart failure patients.3 Beta-blockers decrease adrenergic activation after acute MI.3 Although there is compelling evidence that angiotensin-converting enzyme (ACE) inhibitors, beta-blockers, and aldosterone antagonists decrease hospitalizations and mortality in patients with heart failure, these life-sustaining therapies are continually underutilized.4 The side-effect profile of the currently available beta-blockers, particularly the noncardioselective beta-blockers, is often considered a drawback, including sexual dysfunction, fatigue, depression, and metabolic abnormalities such as impaired glucose tolerance and lipid abnormalities.5 Concerns about potential worsening insulin resistance and dyslipidemia associated with some beta-blockers have hindered their use as monotherapy in hypertensive patients without other compelling indications for their use.
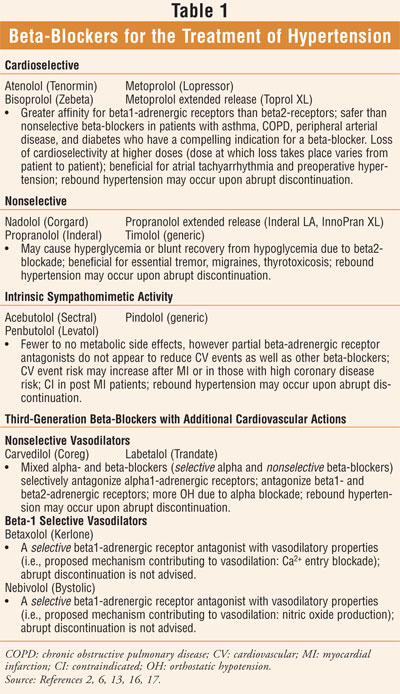
Third-generation beta-blockers have additional cardiovascular actions; multiple mechanisms are credited for the vasodilation seen in these agents (TABLE 1).6 Labetalol and carvedilol block the beta1-adrenergic receptors, in addition to blocking beta2- and alpha1-adrenergic receptors (i.e., as a selective alpha- [i.e., vasodilating] and nonselective beta-blocker); also, carvedilol has antioxidant properties.1 Compared with the traditional nonvasodilating beta-blockers, use of vasodilatory beta-blockers may result in improved cardiovascular outcomes.1,7
Newest Vasodilatory Beta-Blocker: Nebivolol
The most recent beta-blocker to enter the U.S. marketplace is nebivolol (Bystolic, Forest) (TABLE 2), approved by the FDA for the treatment of hypertension; in Europe, it is registered for use in mild-to-moderate, uncomplicated hypertension and mild-to-moderate heart failure and has been approved for hypertension outside Europe as well.1,8 Unlike carvedilol, nebivolol is selective for the beta1-adrenergic receptor in extensive metabolizers (most of the population) and at doses less than or equal to 10 mg (in poor metabolizers and at higher doses nebivolol inhibits both beta1- and beta2-adrenergic receptors).9 At therapeutically relevant doses, nebivolol lacks intrinsic sympathomimetic- and membrane-stabilizing activity.9 Like carvedilol, nebivolol also exhibits vasodilatory effects, although these are proposed to be through nitric oxide (NO)-potentiating actions.1,8

NO is an intrinsic vasodilator produced in the vascular endothelium; endothelium-derived NO is important in the regulation of large arterial stiffness, which in turn is a major risk factor for cardiovascular disease.5,10 Nebivolol enhances nitric oxide bioavailability and improves endothelial function, leading to a reduction in arterial stiffness.5,10 Beneficial hemodynamic effects are observed, such as reductions in central aortic blood pressure when arterial stiffness is decreased.10 Further, data demonstrate nebivolol's antioxidant property, enabling it to decrease markers of oxidative stress.5 Researchers believe it is these effects that conceivably modulate the endothelial dysfunction usually seen in hypertension.5 It remains to be investigated whether nebivolol may have a specific role in hypertensive populations with reduced endothelial function, such as African Americans, patients with diabetes, and individuals with vascular disease.1 Nebivolol has not been directly compared with any of the other recommended beta-blockers in a clinical outcomes trial.1
Nebivolol is rapidly absorbed after oral administration, and the dose most commonly used in clinical trials was 5 mg daily for hypertension; once-daily dosing of nebivolol significantly reduces systolic blood pressure (SBP) and diastolic blood pressure (DBP) according to research.11 The most frequent treatment-emergent adverse events reported in nebivolol clinical trials worldwide were headache, fatigue, and dizziness; the most common adverse events that led to discontinuation were headache, nausea, and bradycardia.9,11
In placebo-controlled clinical hypertension studies in the U.S. (i.e., 2,800 total patients) those 65 or older were also represented (i.e., 478 total); between older and younger patients, no overall differences in efficacy or in incidence of adverse effects were found.9 While some clinicians have recommended dosage adjustments for elderly patients, the manufacturer's prescribing information does not deem it necessary.9
Hypertension and Cardiovascular Risk
As an individual ages, his or her average BP increases continuously.12 It is not surprising, therefore, that hypertension occurs in greater than two-thirds of those over 65.12 What is surprising to many patients, however, is that while most hypertensive individuals remain asymptomatic for many years, this condition is not without consequence; hypertension is a major cardiovascular risk factor.5,12 Reducing BP to goal levels, while avoiding the deterioration of quality of life, is a significant means of reducing cardiovascular risk.14 Pharmacists should be aware that the goal of treatment for hypertension is a reduction in hypertension-related morbidity and mortality (i.e., target-organ damage such as cardiovascular events, cerebrovascular events, heart failure, and kidney disease).12,15 Furthermore, independent of cardiovascular complications, hypertension might predispose to dementia and disability in advanced age, and data seem to support the hypothesis that disability and dementia might be reduced with improved BP control.12
JNC7-Recommended BP Goals and Therapy
A decrease in cardiovascular disease complications has been associated with SBP and DBP targets less than 140/90 mmHg, and thus the goal BP that is recommended by the Seventh Report of the Joint National Committee on the Detection, Evaluation, and Treatment of High Blood Pressure (JNC7); in patients with hypertension and diabetes or renal disease, the BP goal is less than 130/80 mmHg.13 Lifestyle modifications (e.g., weight reduction, dietary approaches, sodium restriction, physical activity, and moderation of alcohol consumption) should be prescribed in all patients with prehypertension (i.e., SBP 120-139 mmHg and DBP 80-89 mmHg) and hypertension since they have been shown to reduce SBP.13 Lifestyle modifications are considered an adjuvant, and not a replacement, to antihypertensive therapy in patients with hypertension.2
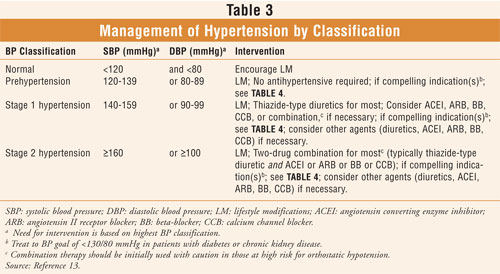
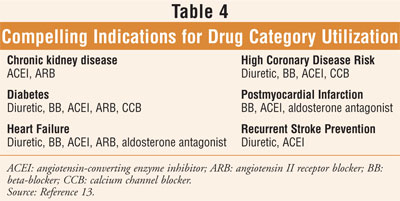
Medication selection for the treatment of hypertension, including tailoring of the regimen to the individual, is influenced by the available evidence that demonstrates risk reduction (TABLE 3).12 It is important to choose agents that do not worsen concomitant conditions or cause unacceptable side effects.1 When BP is greater than 20/10 mmHg above goal BP, the clinician should consider initiating therapy with two agents, one of which usually should be a thiazide diuretic; certain high-risk conditions are compelling indications for the initial use of other antihypertensive drug classes (TABLE 4).13 Most hypertensive patients require combination therapy to achieve goal BP values.2
Isolated Systolic Hypertension in the Elderly
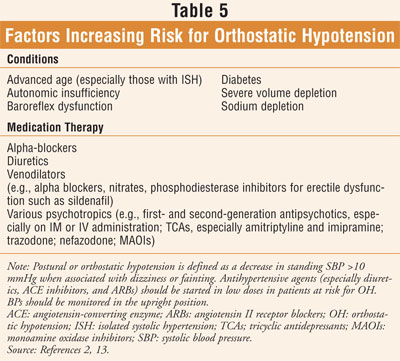
In patients 50 years and older, data indicate cardiovascular morbidity and mortality are more closely related to SBP than DBP.2 In the elderly, isolated systolic hypertension (ISH) is especially prevalent and is recognized as a strong risk factor for cardiovascular disease.12 In most elderly patients, particularly those with ISH, the initial antihypertensive agent should be a thiazide diuretic at a low starting dose (e.g., hydrochlorothiazide 12.5 mg).2 Due to ISH, and a greater sensitivity to volume depletion and sympathetic inhibition compared with their younger counterparts, the elderly are at risk for orthostatic hypotension (OH) (i.e., a decrease in standing SBP > 10 mmHg) when antihypertensive medication therapy is initiated.2 Due to dizziness and the risk of fainting secondary to OH, the risk of falls may be increased. The occurrence of OH is particularly prevalent with the initiation of a diuretic, an ACE inhibitor, or an angiotensin II receptor blocker. Patients with factors predisposing them to OH (TABLE 5) should be started on very low doses that are gradually titrated.2 Standard doses of antihypertensive agents and multiple drug therapy are usually necessary in the majority of geriatric patients to achieve appropriate BP goals.13
REFERENCES
1. Weber MA, Brookes L. Vasodilatory beta-blockade in hypertension and heart failure. Highlights of the American Heart Association (AHA) 2007 Scientific Sessions. Medscape CME/CE. www.medscape.com/viewprogram/8457_pnt. Accessed August 28, 2008.
2. Saseen JJ, Carter BL. Hypertension. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 6th ed. New York, NY: McGraw-Hill Inc; 2005:185-217.
3. Ciarka A, van de Borne P, Pathak A. Myocardial infarction, heart failure and sympathetic nervous system activity: new pharmacological approaches that affect neurohumoral activation. Expert Opin Investig Drugs. 2008;17:1315-1330.
4. Fonarow GC. How well are chronic heart failure patients being managed? Rev Cardiovasc Med. 2006;7(suppl 1):S3-S11.
5. Wojciechowski D, Papademetriou V. Beta-blockers in the management of hypertension: focus on nebivolol. Expert Rev Cardiovasc Ther. 2008;6:471-479.
6. Westfall TC, Westfall DP. Adrenergic agonists and antagonists. In: Brunton LL, Lazo JS, Parker KL, eds. Goodman & Gilman's The Pharmacological Basis of Therapeutics. 11th ed. New York, NY: McGraw-Hill Inc; 2006:271-295.
7. Pedersen ME, Cockcroft JR. The vasodilatory beta-blockers. Curr Hypertens Rep. 2007;9:269-277.
8. de Boer RA, Voors AA, van Veldhuisen DJ. Nebivolol: third-generation beta-blockade. Expert Opin Pharmacother. 2007;81539-1550.
9. Bystolic (nebivolol) [package insert]. St. Louis, MO: Forest Pharmaceuticals, Inc; December 2007.
10. Cockcroft J. A review of the safety and efficacy of nebivolol in the mildly hypertensive patient. Vasc Health Risk Manag. 2007;3:909-917.
11. Gray CL, Ndefo UA. Nebivolol: a new antihypertensive agent. Am J Health Syst Pharm. 2008;65:1125-1133.
12. DiBari M, Furberg CD, Psaty BM, et al. Hypertension. In: Hazzard WR, Blass JP, Halter JB, et al. Principles of Geriatric Medicine and Gerontology. 5th ed. New York:, NY: McGraw-Hill, Inc; 2003:499-509.
13. Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7 Express). Department of Health and Human Services; National Institutes of Health; National Heart, Lung, and Blood Institute. December 2003. www.nhlbi.nih.gov/guidelines/hypertension/express.pdf. Accessed August 28, 2008.
14. Van Bortel LM, Fici F, Mascagni F. Efficacy and tolerability of nebivolol compared with other antihypertensive drugs: a meta-analysis. Am J Cardiovasc Drugs. 2008;8:35-44.
15. Chobanian AV, Bakris GL, Black HR, et al; Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. National Heart, Lung, and Blood Institute; National High Blood Pressure Education Program Coordinating Committee. Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension. 2003;42:1206-1252.
16. Epocrates Rx Pro. version 8.10. Updated September 6, 2008.
17. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 12th ed. Hudson, OH: Lexi-Comp, Inc; 2007.
To comment on this article, contact rdavidson@jobson.com.





