US Pharm. 2010;35(11):10.
Psychotropic medications are a major resource in the treatment of mental disorders. National Ambulatory Medical Care Survey findings show that, from 2004 to 2005, elderly patients made 12 million physician visits in which psychotropic medications were prescribed. A greater number of these visits were made by patients who were 84 years of age or older, female, white, or from the western United States. The use of antipsychotics, sedative antihistamines, and sedative-hypnotics in nursing homes decreased significantly following the implementation of the Nursing Home Reform Act (OBRA '87), while prescribing of anxiolytics increased. The psychotropics most frequently prescribed by office-based physicians for patients aged 20 to 59 years were antidepressants and anxiolytics. Primary care physicians prescribed a majority of the psychotropic drugs.
Demographic Differences: From 2005 to 2006, non-Hispanic black patients had higher rates of depression (8.0%) than non-Hispanic white patients (4.8%). Among persons below the poverty level, non-Hispanic white patients had higher rates of depression (18.0%) than Mexican American patients (7.6%). Non-Hispanic black and non-Hispanic white patients below the poverty level had higher rates of depression than those with higher incomes, but depression rates in Mexican American patients did not vary by poverty status.
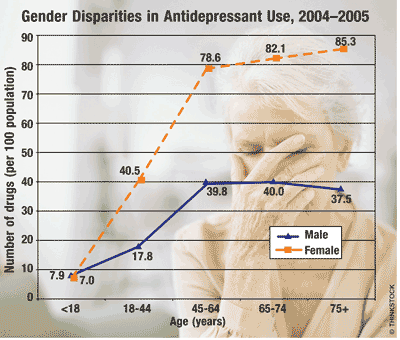
It was found that women used twice as many antidepressants as men. Women respond better than men to serotonin-modulating agents, but this effect is reversed after menopause. In addition, certain psychopharmacologic agents can cause weight gain, hyperglycemia, cardiac arrhythmias, and sexual dysfunction in women.
People with depression, anxiety, or other mental-health disorders are more likely to gain weight over time and become obese. Obesity did not significantly increase the risk of depression, anxiety, or other mental-health disorders, however.
Compliance: Half of the psychiatric morbidity in the primary care setting goes unrecognized. Noncompliance with the treatment regimen and inadequate counseling of patients about time to clinical effect, duration of treatment after response, and possible side effects were identified as major contributors to undertreatment of depression.
To optimize clinical outcomes in patients with depression, pharmacists should embrace their responsibilities as pharmaceutical care providers. In addition to recognizing the more obvious mood symptoms, pharmacists should be aware of somatic symptoms, which are more common in women. Since a diet high in processed foods and saturated fats may increase the risk of depression, pharmacists should encourage patients to consume a diet rich in vegetables, fruits, whole grains, and high-quality protein. Finally, pharmacists can educate patients about their illness and the appropriate use of antidepressant pharmacotherapy; they also can utilize call-back programs to assess compliance, adverse effects, and medication response.
To comment on this article, contact rdavidson@uspharmacist.com.






