US Pharm. 2009;43(7):44-48.
Diabetes mellitus is a significant health concern for older persons in the United States. Approximately 23% of patients over the age of 60 have diabetes, with the majority suffering from type 2 diabetes.1 Elderly patients may experience critical health consequences of diabetes, including accelerated aging and increased rates of premature death and disability.2,3 Older patients are also more likely to have comorbidities such as hypertension, dyslipidemia, and cardiovascular disease, as well as geriatric syndromes like cognitive impairment, depression, and urinary incontinence.2,4 Optimal care of older patients with diabetes necessitates individualized treatment plans that consider life expectancy, severity of diabetes complications, and coexisting illnesses.2,3
Glycemic Goals
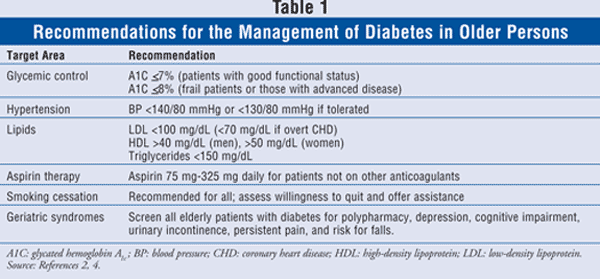
For diabetic patients with good cognitive and functional status, a target glycated hemoglobin A1c (A1C) of 7% or less is appropriate.2,4 However, the spectrum of diabetes is diverse in the elderly, and not all patients benefit from stringent glycemic control. Evidence from clinical trials demonstrates that approximately 8 years of glycemic control is required before reductions in microvascular events can be appreciated.5,6 Furthermore, there is limited evidence to substantiate that tight glycemic control appreciably reduces the incidence of macrovascular complications, particularly in long-standing diabetes.2 Thus, for frail elders, patients with limited life expectancy, or those with significant complications or comorbidities, a less aggressive glycemic goal is reasonable (TABLE 1). At a minimum, glycemic control should be adequate to prevent symptoms such as polyuria and to avoid hyperglycemic crises.3
Pharmacotherapy
Sulfonylureas
Sulfonylureas lower glucose primarily by stimulating insulin release from pancreatic beta cells.3,7,8 When used as monotherapy, sulfonylureas lower the A1C by 1% to 2%.9 All sulfonylureas are available in generic form, which makes them an inexpensive choice for the management of type 2 diabetes. The first-generation sulfonylureas (e.g., chlorpropamide, tolbutamide) are used infrequently, and chlorpropamide should be avoided in elderly patients due to its long half-life and its risk for prolonged hypoglycemia.4,7
Hypoglycemia and weight gain are the major adverse effects of the sulfonylureas.10 Hypoglycemia is of particular concern in older patients, as this population is prone to hypoglycemic unawareness, as are falls and cognitive dysfunction accompanying hypoglycemic episodes.7,11,12 Of the second-generation sulfonylureas, glyburide is most likely to accumulate during renal dysfunction and cause hypoglycemia. Therefore, glyburide is not recommended for patients with a creatinine clearance less than 50 mL/min. Glipizide and glimepiride are preferred agents in this setting.3,10 Regardless of the sulfonylurea chosen, the initial dose should be conservative with careful titration as needed.12
Meglitinides
Like the sulfonylureas, the meglitinides are also insulin secretagogues; however, they have a quicker onset and a shorter duration of action. As a single agent, repaglinide is more effective than nateglinide and lowers the A1C by 0.5% to 1.5%.9,13 Similarly to sulfonylureas, hypoglycemia and weight gain are the most commonly seen adverse effects. Meglitinides should not be used with sulfonylureas due to duplication of action and increased risk of hypoglycemia.
Because of their short-acting nature, meglitinides should be taken prior to meals. If a patient omits a meal, the dose should be withheld. Elderly patients may experience undue adverse effects from meglitinides if they are included in a prefilled medication box and the patient or caregiver administers the dose in the absence of a meal. Mealtime dosing requires multiple daily dosing for meglitinides, and adherence or pill burden can be a problem in elderly patients with polypharmacy or cognitive issues. In addition, the higher cost of meglitinides restricts their use in elderly patients with diabetes who have limited incomes. Meglitinides may have a niche in older patients with erratic eating habits or those unable to tolerate other agents.10
Metformin
The biguanide metformin lowers glucose by reducing hepatic gluconeogenesis. Metformin also decreases intestinal glucose absorption and enhances sensitivity to insulin.7,10 Similarly to sulfonylureas, metformin monotherapy reduces the A1C by 1% to 2%.9 In overweight patients with type 2 diabetes, metformin therapy has been associated with a decrease in diabetes-related end points (e.g., death from hyperglycemia, fatal or nonfatal myocardial infarction, renal failure) and all-cause mortality as compared to therapy with insulin or sulfonylureas.14 Metformin, along with lifestyle intervention, is currently recommended as initial therapy for the management of type 2 diabetes.9 Although controlled trials have not studied sufficient numbers of older patients with diabetes, clinical use suggests that metformin is an effective agent in this population.
The most common adverse effects of metformin are gastrointestinal discomfort and diarrhea, which can be minimized by slow titration of the dose and administration with food.15 When used alone, metformin typically does not cause hypoglycemia and is usually weight neutral or causes modest weight loss.9,10 Given the low risk of hypoglycemia, metformin has an important role in elderly patients with diabetes, as long as patients are selected appropriately to avoid the risk of lactic acidosis.
Lactic acidosis is a rare but serious adverse effect of metformin, and it is more likely in patients with renal dysfunction. This is of particular concern since older adults with diabetes have a high prevalence of renal insufficiency. To reduce the risk of lactic acidosis, metformin is contraindicated in females with a serum creatinine of 1.4 mg/dL or greater and in males with a creatinine of 1.5 mg/dL or greater. Metformin should be used with caution in patients older than 80 years, unless laboratory studies indicate that creatinine clearance is not compromised, and titration to maximum dosage should be avoided if possible.4,15 The drug is also contraindicated in instances where renal perfusion may be reduced, such as acute myocardial infarction, congestive heart failure, shock, and sepsis. In addition, metformin should be discontinued prior to iodinated contrast studies and should not be reinstituted for at least 48 hours after the procedure, when renal function can be verified. Pharmacists need to be vigilant and recommend prompt discontinuation of metformin in the above instances. Although metformin has a number of contraindications and precautions, it provides an effective and inexpensive alternative for elderly patients with type 2 diabetes who have adequate renal function.3,10
Thiazolidinediones
The thiazolidinediones (TZDs) pioglitazone and rosiglitazone act as agonists of the peroxisome-proliferator-
Rosiglitazone has been a subject of controversy due to concerns about increased cardiovascular risk with this agent. Two recent meta-analyses have suggested that rosiglitazone is associated with an increased risk of myocardial infarction, and an interim analysis of a prospective trial was inconclusive regarding the risk of myocardial infarction and cardiovascular death with rosiglitazone.17-19 As a result, rosiglitazone is not recommended for the treatment of type 2 diabetes in the most recent treatment algorithm.9 In contrast, in a prospective trial, cardiovascular outcomes with pioglitazone did not differ significantly from placebo.20 The more beneficial effect of pioglitazone on the lipid profile may be one explanation for the disparity in cardiovascular outcomes between the two agents. In summary, many questions still remain regarding cardiovascular risk with TZDs. Results of large-scale ongoing trials are needed to better characterize cardiovascular outcomes with these agents.
TZDs can cause fluid retention and exacerbate heart failure. As such, the use of these agents is contraindicated in patients with New York Heart Association Class III and IV heart failure.16 In general, TZDs should be avoided in patients with symptomatic heart failure. Additionally, recent evidence shows that TZDs are associated with an increased risk of fractures in female patients.21 Since osteoporosis and heart failure are common comorbidities in older patients with diabetes, this may limit the use of TZDs somewhat. Given these issues, the expense of TZDs, and the questions regarding cardiovascular risk, TZDs should be reserved for second- or third-line therapy in elderly patients with diabetes.
Alpha-glucosidase Inhibitors
Acarbose and miglitol are alpha-glucosidase inhibitors that lower postprandial glucose by inhibiting the breakdown of complex starches in the intestine, thereby delaying carbohydrate absorption.10 They are taken at the beginning of each meal and may reduce A1C by 0.5% to 0.8%.9 Because they have a high incidence of flatulence, bloating, and diarrhea, alpha-glucosidase inhibitors have remained unpopular for the management of diabetes in the elderly.3,7,10
DPP-4 Inhibitors
Dipeptidyl-peptidase-4 (DPP-4) inhibitors inhibit the enzyme that inactivates the incretin hormones glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic polypeptide (GIP).3 Prolonging the activity of GLP-1 and GIP enhances glucose-mediated insulin secretion and suppresses glucagon release, resulting in reduced hepatic gluconeogenesis. Sitagliptin, currently the only FDA-approved medication in this class, lowers A1C by 0.5% to 0.8%.9 Overall, sitagliptin is relatively more expensive and lowers A1C less than most other oral agents. In general, sitagliptin is well tolerated; however, it has been associated with an increased incidence of upper respiratory infections, and effects on immune function may be a concern in older patients.9 It may be useful in elderly patients with diabetes with contraindications or intolerance to other medications. Of note, dosage adjustments of sitagliptin are required in renal dysfunction.3 DPP-4 inhibitors in the pipeline include saxagliptin and vildagliptin.
Incretin Mimetics
Exenatide, an incretin mimetic indicated for type 2 diabetes, targets blood glucose by increasing glucose-dependent insulin synthesis and release and diminishing inappropriate secretion of glucagon.22 Exenatide also slows gastric emptying and increases satiety, thereby reducing food intake. The drug is injected twice daily within the 60 minutes preceding a main meal. When used as monotherapy, exenatide lowers the A1C by 0.5% to 1%.22 Because of its peptide nature, patients may develop antibodies to exenatide. In most cases, the titers lessen over time. Patients who develop high titers of antiexenatide antibodies (3%-9%) may experience attenuated response to exenatide and require alternative pharmacotherapy.9,22
Due to delayed gastric emptying, exenatide has a high rate of nausea, especially upon initiation of treatment. Furthermore, delayed gastric emptying may negatively affect the absorption of oral medications, which can be particularly concerning in older patients on multiple medications.3 During postmarketing surveillance, exenatide has been associated with acute pancreatitis. Exenatide has the potential benefit of modest weight loss; however, weight loss is undesirable in the frail elderly.23 Due to the above concerns, the expense of the drug, and limited safety and efficacy data in the elderly, exenatide should be reserved for those who have failed other therapies.3,12,23
Pramlintide
Pramlintide is a synthetic analogue of amylin, a hormone that is co-secreted with insulin by pancreatic beta cells following food intake.24 Like exenatide, pramlintide decreases postprandial glucagon secretion, delays gastric emptying, and enhances satiety; however, it does not promote insulin secretion. Pramlintide is indicated for type 1 or 2 diabetes as an adjunct to mealtime insulin, and it reduces the A1C by an additional 0.5% to 0.6%.24
Pramlintide should be injected three times daily prior to major meals ( >30 g carbohydrate) and should not be mixed with insulin. Pramlintide increases the risk of severe hypoglycemia, and it should not be administered in patients with hypoglycemic unawareness, a condition more likely in the elderly. To reduce the risk of hypoglycemia, the dose of preprandial insulin should be decreased by 50% when initiating pramlintide.24 Due to delayed gastric emptying, pramlintide frequently causes nausea and can impact the absorption of oral medications, another important consideration in the elderly who take multiple medications.8 Because it necessitates multiple daily injections, increases the risk of severe hypoglycemia, and provides only modest efficacy, pramlintide has limited utility in older patients.
Insulin
As beta-cell function declines over time, a large percentage of patients with type 2 diabetes will require insulin therapy for adequate glycemic control.25 A variety of insulin formulations are available (TABLE 2). Rapid- or short-acting insulin covers mealtime or bolus insulin requirements, while intermediate- or long-acting insulin provides basal insulin coverage. Addition of bedtime basal insulin (NPH, glargine, or detemir) is a reasonable first step in patients not controlled with oral agents.8,26 Patients not achieving adequate response with basal insulin may be switched to twice-daily or multiple daily injections of basal and bolus insulin. Regimen complexity should be individualized based on functional and cognitive status of the patient and the desired level of glycemic control. Although short-term, sliding-scale insulin is frequently used during hospitalization or acute illness, routine usage should be avoided as it provides suboptimal glycemic control and places the patient at risk for prolonged hyperglycemia.8,26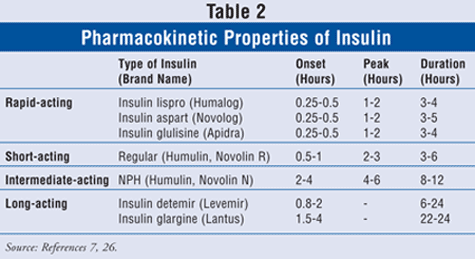
The main risk with insulin therapy in the elderly is hypoglycemia. As with sulfonylureas, patients should be educated on warning signs and symptoms and management of hypoglycemia. Another concern is the ability of the patient to accurately draw up and administer insulin. Many older patients have limited dexterity or poor visual acuity, which impedes their ability to mix or inject insulin. In this instance, patients may benefit from specialized delivery devices such as insulin pens or syringe magnifiers.7,26 Use of premixed insulin to simplify the regimen (e.g., insulin 70/30) and prefilling of syringes are alternatives.
Colesevelam
Colesevelam is a bile acid sequestrant that is indicated as adjunctive therapy for glycemic control in type 2 diabetes.27 The mechanism of action of colesevelam in diabetes is unknown. When added to metformin, sulfonylurea, insulin, or other combination therapies, colesevelam reduces the A1C by less than 0.5%. Monotherapy with colesevelam has not been investigated.
The recommended dosage of colesevelam is six 625-mg tablets daily, which imposes a heavy pill burden in the elderly who are on multiple medications. Colesevelam is also known to bind medications such as glyburide and phenytoin, and administration must be separated from them by at least 4 hours.27 Adverse effects include constipation and dyspepsia. Since it has only minor effects on A1C and is associated with a significant pill burden, colesevelam should be reserved for patients intolerant of other therapies.
Management of Cardiovascular Risk
Macrovascular disease such as heart disease and stroke is the main cause of morbidity and mortality in patients with diabetes.2 Although landmark trials such as the Diabetes Control and Complications Trial and the United Kingdom Prospective Diabetes Study established benefits of tight glycemic control in reducing microvascular complications of diabetes, they did not show similar benefits for macrovascular disease.7,28 Recent large-scale trials have also failed to demonstrate a reduction in macrovascular outcomes with tight glycemic control.19,29,30 Furthermore, the Action to Control Cardiovascular Risk in Diabetes study was halted early due to concerns of increased cardiovascular risk in the tight glycemic control arm.19 Thus, while glycemic control is important in older patients with diabetes, this population may obtain greater reduction in macrovascular events by controlling their modifiable cardiovascular risk factors such as hypertension and hyperlipidemia.4,7,28
Strong evidence exists that blood pressure management in older patients with diabetes reduces cardiovascular morbidity and mortality.2,4,31,32 The recommended blood pressure goal in diabetes is <130/80 mmHg; however, in elderly diabetic patients the target should be <140/80 mmHg with a goal of <130/80 mmHg if tolerated.4 Angiotensin-converting enzyme inhibitors and angiotensin receptor blockers have cardiovascular and renal benefits in diabetes and are recommended as initial therapy for hypertension.2 With these agents, routine monitoring of renal function and serum potassium is essential in the elderly patient with diabetes.
Dyslipidemias are another contributing risk factor for cardiovascular disease in patients with diabetes. Desired lipid goals for older patients with diabetes are provided in TABLE 1. If tolerated, statins should be utilized in all elderly patients with diabetes along with lifestyle therapy to achieve desired LDL goals.2 For other dyslipidemias, therapy should be individualized based on primary lipid abnormalities. For example, for low HDL and high triglycerides, fibrates have been shown to be beneficial in lowering triglycerides, increasing HDL, and reducing cardiovascular events.2,4 In addition, aspirin therapy is recommended in older patients with diabetes who are not taking other anticoagulants to reduce the risk of myocardial infarction and cardiovascular mortality. Finally, since smoking also increases the risk of cardiovascular disease, all patients with diabetes should be counseled to quit smoking and offered pharmacologic assistance if needed.2,4,7
Geriatric Syndromes
Common geriatric syndromes in elderly patients with diabetes as identified by the American Geriatrics Society include polypharmacy, cognitive impairment, urinary incontinence, injurious falls, pain, and depression.2,4 Polypharmacy is very common in older patients with diabetes due to multiple medications needed for diabetes as well as for comorbid conditions such as hypertension, hyperlipidemia, and others. Pharmacists, in particular, have a responsibility to review medication profiles of these patients, ensure there is an indication for each medication, and screen for drug-drug interactions. Furthermore, pharmacists should keep patients and caregivers updated about the risks and benefits of medications and encourage them to report adverse events. Use of multiple medications may be an exacerbating factor for other geriatric syndromes such as cognitive impairment, urinary incontinence, falls, and depression.4
Elderly patients with diabetes also have a greater likelihood of cognitive impairment.3,4 Decreased cognitive function may prevent patients from successfully managing diabetes pharmacotherapy or associated lifestyle modifications. It should be noted that hyperglycemia may be a reversible cause of impaired cognition in elderly patients with diabetes. In addition, older adults with diabetes, particularly women, are also at higher risk of urinary incontinence. Common conditions associated with urinary incontinence in diabetic patients include polyuria and neurogenic bladder.4 Many elderly patients with diabetes have diabetic neuropathy that is often undertreated. Undertreated pain may further contribute to depression and the inability to implement lifestyle changes. Due to comorbidities such as loss of vision, neuropathic pain, hypoglycemia, and polypharmacy, elderly patients with diabetes are in jeopardy of injurious falls. Aggressive glycemic control in this population increases the risk of hypoglycemia and related falls. Lastly, having multiple coexisting conditions along with diabetes, the diabetic elderly are twice as likely to experience depression as those without diabetes. Given the prevalence of these conditions and the detrimental effect they can have on quality of life, all elderly patients with diabetes should be screened for these syndromes upon initial evaluation and periodically thereafter.4 Pharmacists should be aware of geriatric syndromes and seek to optimize medication use to lessen their impact in elderly patients.
Hyperglycemic Crises
Hyperglycemic crises consist of hyperglycemic hyperosmolar state (HHS) and diabetic ketoacidosis. In older adults where type 2 diabetes is more common, HHS is more prevalent. Infection is the most common precipitating factor, accounting for 20% to 55% of cases.33 Another common precipitating factor is inappropriate dosing of insulin or insulin omission.34 Cerebrovascular events, pancreatitis, myocardial infarction, alcohol intoxication, and polypharmacy may also lead to HHS.33,34 Medications that affect carbohydrate metabolism such as beta blockers, corticosteroids, pentamidine, sympathomimetics, second-generation antipsychotics, and high-dose diuretics are potential causative agents.34 The mortality rate of patients with HHS is approximately 11%, so prompt treatment is needed. Treatment of HHS consists of adequate hydration, insulin therapy, and repletion of electrolytes, particularly potassium.35 It is also important to identify precipitating events in order to prevent future recurrent crises. Appropriate sick-day management to avert possible hyperglycemic crisis is an essential component of diabetes education for the elderly.
Conclusion
Management of diabetes in the elderly is often challenging due to coexisting conditions, geriatric syndromes, and variable functional status. In frail older patients or those with limited life expectancy, more relaxed glycemic goals are acceptable. Most elderly patients obtain considerable benefit from management of cardiovascular risk factors, and control of hypertension and hyperlipidemia should be a focus in this population. Pharmacotherapy should be tailored based on desired glycemic goals, functional status, and current comorbidities. By optimizing medication use and reducing risks associated with polypharmacy, pharmacists play a key role in decreasing morbidity and mortality and improving quality of life in elderly patients with diabetes.
REFERENCES
1. American Diabetes Association. Diabetes statistics. www.diabetes.org/diabetes-
2. American Diabetes Association. Standards of medical care in diabetes-2009. Diabetes Care. 2009;32(suppl 1):S13-S61.
3. Cayea D, Boyd C, Durso SC. Individualising therapy for older adults with diabetes mellitus. Drugs Aging. 2007;24(10):851-863.
4. Guidelines for improving the care of the older person with diabetes mellitus. California Healthcare Foundation/American Geriatrics Society Panel on Improving Care for Elders with Diabetes. J Am Geriatr Soc. 2003;51(5):S265-S280.
5. United Kingdom Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet. 1998;352(9131):837-853.
6. Shorr RI, Franse LV, Resnick HE, et al. Glycemic control of older adults with type 2 diabetes: findings from the Third National Health and Nutrition Examination Survey, 1988-94. J Am Geriatr Soc. 2000;48(3):264-267.
7. Campbell S. Management of type 2 diabetes in the geriatric patient. J Pharm Prac. 2000;13(4):263-276.
8. American Medical Directors Association (AMDA). Diabetes Management in the Long-Term Care Setting. Columbia, MD: American Medical Directors Association (AMDA); 2008.
9. Nathan DM, Buse JB, Davidson MB, et al. American Diabetes Association; European Association for the Study of Diabetes. Medical management of hyperglycemia in type 2 diabetes: a consensus algorithm for the initiation and adjustment of therapy: a consensus statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2009;32(1):193-203.
10. Sakharova OV, Inzucchi SE. Treatment of diabetes in the elderly: addressing its complexities in this high-risk group. Postgrad Med. 2005;118(5):19-29.
11. Shorr RI, Ray WA, Daugherty JR, Griffin MR. Incidence and risk factors for serious hypoglycemia in older persons using insulin or sulfonylureas. Arch Intern Med. 1997;157(15):1681-1686.
12. Silverberg AB, Ligaray KP. Oral diabetic medications and the geriatric patient. Clin Geriatr Med. 2008;24(3):541-549.
13. Rosenstock J, Hassman DR, Madder RD, et al. Repaglinide versus nateglinide monotherapy. Diabetes Care. 2004;27(6):1265-1270.
14. United Kingdom Prospective Diabetes Study (UKPDS) Group. Effect of intensive blood-glucose control with metformin on complications in overweight patients with type 2 diabetes (UKPDS 34). Lancet. 1998; 352(9131):854-865.
15. Glucophage XR [package insert]. Princeton, NJ: Bristol-Myers Squibb Company; 2008.
16. Avandia [package insert]. Research Triangle Park, NC: GlaxoSmithKline; 2008.
17. Nissen SE, Wolski K. Effect of rosiglitazone on the risk of myocardial infarction and death from cardiovascular causes. N Engl J Med. 2007;356(24):2457-2471.
18. Singh S, Loke YK, Furberg CD. Long-term risk of cardiovascular events with rosiglitazone: a meta-analysis. JAMA. 2007;298(10):1189-1195.
19. Gerstein HC, Miller ME, Byington RP, et al. The Action to Control Cardiovascular Risk in Diabetes Study Group. Effects of intensive glucose lowering in type 2 diabetes. N Engl J Med. 2008;358(24):2545-2559.
20. Dormandy JA, Charbonnel B, Eckland DJ, et al. Secondary prevention of macrovascular events in patients with type 2 diabetes in the PROactive (PROspective pioglitAzone Clinical Trial in macroVascular Events): a randomised controlled trial. Lancet. 2005;366(9493):1279-1289.
21. Schwartz AV, Sellmeyer DE, Vittinghoff E, et al. Thiazolidinedione use and bone loss in older diabetic adults. J Clin Endocrinol Metab. 2006;91(9):3349-3354.
22. Byetta [package insert]. San Diego, CA: Amylin Pharmaceuticals, Inc; 2008.
23. Abbatecola AM, Maggi S, Paolisso G. New approaches to treating type 2 diabetes mellitus in the elderly: role of incretin therapies. Drugs Aging. 2008;25(11):913-925.
24. Symlin [package insert]. San Diego, CA: Amylin Pharmaceuticals, Inc; 2008.
25. Zarowitz BJ, Tangalos EG, Hollenack K, O'Shea T. The application of evidence-based principles of care in older persons (issue 3): management of diabetes mellitus. J Am Med Dir Assoc. 2006;7(4):234-240.
26. Bray B. Transitioning and adjusting insulin analog therapy in elderly patients: clinical review. The Consultant Pharmacist. 2008;23(suppl B):17-23.
27. Welchol [package insert]. Parsippany, NJ: Daiichi Sankyo; 2008.
28. Sherman FT. Tight blood glucose control and cardiovascular disease in the elderly diabetic? Let the randomized controlled trials speak for themselves [editorial]. Geriatrics. 2008;63(8):8-10.
29. American Diabetes Association. Intense blood glucose control yields no significant effect on CVD reduction in VA diabetes trial, June 8, 2008 (immediate release). www.diabetes. org/for-media/pr-intense-
30. Patel A, MacMahon S, Chalmers J, et al. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Engl J Med. 2008;358(24):2560-2572.
31. United Kingdom Prospective Diabetes Study (UKPDS) Group. Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes (UKPDS 38). BMJ. 1998;317(7160):703-713.
32. Curb JD, Pressel SL, Cutler JA, et al. Effect of diuretic-based antihypertensive treatment on cardiovascular disease risk in older diabetic patients with isolated systolic hypertension: Systolic Hypertension in the Elderly Program Cooperative Research Group. JAMA. 1996;276(23):1886-1892.
33. Gaglia JL, Wyckoff J, Abrahamson MJ. Acute hyperglycemic crisis in the elderly. Med Clin N Am. 2004;88(4):1063-1084.
34. Kitabchi A, Umpierrez GE, Murphy MB, et al. Management of hyperglycemic crises in patients with diabetes. Diabetes Care. 2001;24(1):131-153.
35. Kitabchi A, Umpierrez GE, Murphy MB, Kreisberg RA. Hyperglycemic crises in adult patients with diabetes: a consensus statement from the American Diabetes Association. Diabetes Care. 2006;29(12):2739-2748.
To comment on this article, contact rdavidson@jobson.com.





