Postherpetic neuralgia (PHN) is a common form of persistent neuropathic pain in the United States.1,2 Considered the most common complication of shingles, or herpes zoster (HZ), PHN occurs in approximately 10% to 15% of patients with HZ, and in 50% of those who develop shingles after age 60 years.3 Incidence of PHN increases dramatically with age and is uncommon in patients younger than 60 years.4 Prior to age 50 years, there exists virtually no risk of developing PHN; however, the risk increases to 50% to 75% after ages 60 and 75 years, respectively. Risk factors for PHN, including older age, can be found in Table 1.

Herpes zoster is a viral infection resulting from the reactivation of varicella-zoster virus (chickenpox virus) from its latent state in a posterior dorsal root ganglion.5 It affects an estimated 1 million individuals annually in the U.S. and millions of seniors across the globe.6,7 Usually, symptoms begin with pain along the affected dermatome (the area of skin supplied with afferent nerve fibers by a posterior spinal root), which is followed by a vesicular eruption (i.e., rash) in approximately 2 to 3 days.5 The shingles rash is usually diagnostic (an online source for a photo appears in Resources). Risk for HZ begins to rise sharply around age 50 years, and usually occurs in those aged 50 to 70.4,8,9 It can occur at any age, but the incidence increases dramatically with increasing age. Patients with HIV or cancer or who are immunocompromised are at increased risk for HZ.10

Additional complications associated with HZ include involvement of the ophthalmic division of the trigeminal nerve, which can lead to ocular complications and visual loss; referral to an ophthalmologist is recommended.4 Secondary infection of HZ lesions (e.g., with staphylococci, streptococci) may lead to cellulitis.4 Other less common complications include motor paresis and encephalitis.4,11 HZ is treated with antiviral agents (e.g., acyclovir, famciclovir, valacyclovir) initiated within 72 hours after skin lesions appear, to increase the rate of healing and decrease pain due to the acute rash; corticosteroids, although controversial, may be used to treat facial paralysis and cranial polyneuritis and to ease moderate-to-severe pain unrelieved by antivirals and analgesics.4,12 While antiviral agents have improved the management of HZ, many patients still develop pain complications, including PHN.13
Definition of PHN
Clinicians agree that the most common persistent, debilitating complication of shingles is PHN; however, its definition has variations. While PHN can be defined as pain along cutaneous nerves persisting for more than 30 days or continuing even after the shingles rash has healed, according to Gelb et al a more common benchmark used in practice is pain continuing after 90 days.14 Since onset is a more clearly defined point than healing, other researchers define PHN as pain persisting, or appearing, more than 90 days after the onset of the shingles rash.6 Pain may persist for months, years, or be lifelong.5 When HZ affects the trigeminal nerve, it is particularly likely to lead to severe, persistent pain.5 Pain ranges from mild to excruciating, intermittent to constant; it may be triggered by trivial stimuli (e.g., wind, clothes, bed sheets) and may be classified as debilitating.5 Patients report pain quality as burning, throbbing, stabbing, shooting, gnawing, or tender. While it has been stipulated that PHN pain is due to persistent C-fiber nociceptor activity in the nerve cells, data indicate that chronic neural loss and scarring occurs in nerves associated with HZ injury.15
Functional Disability and Depression
Persistent pain can disrupt mood, cause insomnia, interfere with activities of daily living and work, and adversely affect quality of life; patients are at risk for depression and social withdrawal.15
The impact of persistent pain on physical functioning should be assessed. Data have indicated that seniors with persistent pain may experience an increase in pain intensity with movement and, as a result, may limit the activities or movements that exacerbate the pain, such as walking or climbing stairs.16,17 Evidence has shown that by reducing the intensity of the pain by just 25%, a 50% improvement in functional status can be achieved.18 Pharmaceutical care planning should consider the premise that by successfully treating or reducing pain intensity, there may be improvement not only in physical functioning but also in psychosocial functioning.
Management
Pain management of PHN can be particularly difficult. Treatments include lidocaine patch, topical capsaicin, gabapentin, pregabalin, and tricyclic antidepressants (TCAs); opioid analgesics may also be required (for a summary of medication therapy options, including dosing, refer to Table 2 in this article online at www.uspharmacist.com). In some cases, intrathecal methylprednisolone may be of benefit.5 In patients experiencing a prodrome—symptoms preceding the rash by approximately 1 to 4 days—(Table 1), pain symptoms may be mistaken for glaucoma, trigeminal neuralgia, myocardial infarction, pleurisy, appendicitis, cholecystitis, renal colic, collapsed intervertebral disk, or unappreciated trauma.19 Treatment should be individualized based on patient characteristics and the agent’s adverse effect and drug interaction profile. Consultation with a pain management specialist should be considered for some patients.
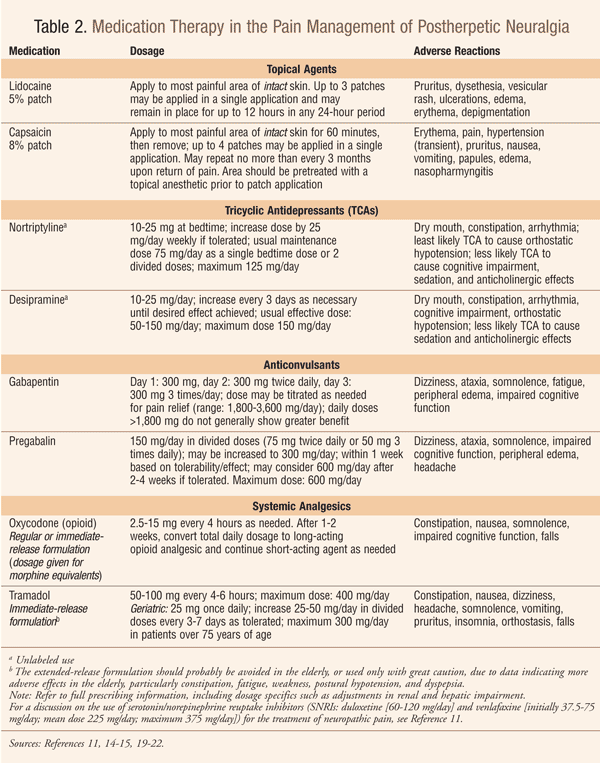
Topical treatments should not be used during the acute phase of HZ with open lesions.19 Use of the capsaicin 8% patch requires the treatment area to be anesthetized by a physician prior to patch application.20,21 Inhalation of airborne capsaicin, secondary to rapid removal of patches, may result in coughing or sneezing; if shortness of breath occurs, medical care is required.21 The capsaicin 8% patch should be used with caution in patients with uncontrolled hypertension or a history of cardiovascular or cerebrovascular events.21 Transient increases in blood pressure have occurred secondary to treatment-related pain during and after patch application.21
Amitriptyline and imipramine should be avoided in the elderly since these agents may produce ataxia, impaired psychomotor function, syncope, and additional falls.22 Nortriptyline is the least likely TCA to cause orthostatic hypotension.21 Side effects of anticonvulsants can be minimized by initiating therapy with low doses and slowly titrating doses upward over several weeks.15 A discussion of the use of chronic opioid therapy for noncancer pain may be found in Reference 23. For a discussion on the use of serotonin/norepinephrine reuptake inhibitors (duloxetine and venlafaxine; for dosing information see Table 2 online) for the treatment of neuropathic pain, see Reference 11.
Prevention of HZ: Zoster Vaccine
Prevention of HZ involves preventing the primary infection (chickenpox) via the varicella vaccine in children and susceptible adults.5 Further, adults 60 years and older should receive a single dose of zoster vaccine live whether or not they have had HZ, since it has been shown to decrease the incidence of HZ. Data have shown that older patients who receive a zoster vaccine might also minimize their chances of developing PHN.13 According to the study, vaccinated patients had a 51% reduction in the incidence of HZ and a 61% reduction in the onset of shingles versus the placebo group.13 Additionally, the rate of PHN was 66% lower in the group receiving the vaccine.13
The zoster vaccine live (Zostavax) was approved by the FDA in 2006; currently, it carries an indication for the prevention of shingles in individuals aged 50 and older.24 Severe adverse reactions, including anaphylaxis, have been reported; therefore, appropriate treatment provisions should be available (e.g., epinephrine 1:1,000) during administration. Of note, this vaccine should not be given at the same time as the pneumococcal vaccine polyvalent (Pneumovax 23).22 Information regarding Web addresses for vaccine highlights and full prescribing information are available in Resources.
Patient Counseling
The CDC recommends a zoster vaccine for use in people aged 60 and older to prevent shingles.8 There is no maximum age for receiving this one-time vaccination; those aged 60 years and older should receive it regardless of whether or not they recall having had chickenpox.8 Patients should be assured that even if they have had shingles, they can still be vaccinated to assist in preventing future occurrences of HZ. While there is no specific waiting period after having shingles before receiving the zoster shingles vaccine, generally a patient should wait until the shingles rash has resolved before getting vaccinated. The vaccine should not be used in people who report an allergy to any component of the vaccine (including gelatin and neomycin); pregnant women; patients with untreated active tuberculosis; individuals who are receiving immunosuppressant therapy (e.g., high-dose corticosteroids); or patients with immunodeficiencies (e.g., HIV/AIDS, leukemia).24 Patients and health care providers should report negative side effects of the vaccine to the FDA via www.fda.gov/medwatch, or by calling 1-800-FDA-1088. A vaccine information statement for zoster vaccine live in English and other languages including Spanish, as well as an audio version, may be found at the CDC Web site (see Resources).
Zoster Vaccine Storage
The FDA approved a change to the prescribing information for zoster vaccine live in July 2009. Specific conditions under which the vaccine can be stored at refrigerator temperature in connection with a change to expiration dating for the product have been defined in this change. The section entitled “How Supplied/Storage and Handling” of the prescribing information was revised and can be accessed at the Web site listed in Resources.
Conclusion
HZ affects 1 million Americans every year. About half of those who develop it after age 60 develop the most common persistent, debilitating complication, PHN. Zoster vaccine live decreases the incidence of HZ and may also minimize the chance of developing PHN.
References
1. Schmader KE. Epidemiology and impact on quality of life of postherpetic neuralgia and painful diabetic neuropathy. Clin J Pain. 2002;18:350-354.
2. Bowsher D. The lifetime occurrence of Herpes zoster and prevalence of postherpetic neuralgia: a retrospective survey in an elderly population. Eur J Pain. 1999;3:335-342.
3. Roberts MJ, Barbee K. Dermatologic health. In: Meredith PV, Horan NM, eds. Adult Primary Care. Philadelphia, PA: WB Saunders Co; 2000.
4. Moinsey AL, Matthew LG, Slawson DC. Herpes zoster and postherpetic neuralgia: prevention and management. Am Fam Physician. 2005;72(6):1075-1080.
5. Herpes zoster. Herpes viruses. Infectious diseases. Merck Manual Online.
www.merckmanuals.com/
6. Oxman MN, Levin MJ, Johnson GR, et al. A vaccine to prevent herpes zoster and postherpetic neuralgia in older adults. N Engl J Med. 2005;352:2271-2284.
7. Terrell J, Cox H, Evans J. Immunizations in the older population. US Pharm. 2009;34(6):HS-1–HS-4.
http://www.uspharmacist.com/
8. Shingles vaccination: what you need to know. Last modified January 13, 2011. Department of Health and Human Services. Centers for Disease Control and Prevention.
www.cdc.gov/vaccines/vpd-vac/
9. Beers MH, Jones TV, Berkwits M, et al, eds. The Merck Manual of Health & Aging. Whitehouse Station, NJ: Merck Research Laboratories; 2004:286, 294, 344-345, 438-442.
10. Insinga RP, Itzler RF, Pellissier JM, et al. The incidence of herpes zoster in a United States Administrative Database. J Gen Intern Med. 2005;20:748-753.
11. Moultry AM, Poon IO. The use of antidepressants for chronic pain. US Pharm. 2009;34(5):26-34.
12. Dworkin RH, O’Connor AB, Backonja M, et al. Pharmacologic management of neuropathic pain: evidence-based recommendations. Pain. 2007;132:237-251.
13. Shingles vaccination reduces postherpetic neuralgia in seniors. Clinical news digest. US Pharm. 2008;33(2):11.
www.uspharmacist.com/content/
14. Gelb L, Hogue M, Levin MJ. Advances in the treatment and prevention of herpes zoster and postherpetic neuralgia. American Pharmacists Association 2006 Annual Meeting and Exhibition. San Francisco, CA; March 20, 2006.
15. Osemene N. Herpes zoster (shingles) and postherpetic neuralgia management. Released May 1, 2009.
www.uspharmacist.com/
16. Davis GC, Hiemenz ML, White TL. Barriers to managing chronic pain of older adults with arthritis.
J Nurs Scholarsh. 2002;34(2):121-126.
17. Duong BD, Kerns RD, Towle V, et al. Identifying the activities affected by chronic nonmalignant pain in older veterans receiving primary care. J Am Geriatr Soc. 2005;53(4):687-694.
18. Flor H, Fydrich T, Turk DC. Efficacy of multidisciplinary pain treatment centers: a meta-analytic review. Pain. 1992;49(2):221-230.
19. Twersky JI, Schmader K. Herpes zoster. In: Halter JB, Ouslander JG, Tinetti ME, et al, eds. Hazzard’s Geriatric Medicine and Gerontology. 6th ed. New York, NY: McGraw-Hill; 2009:1567-1575.
20. My Epocrates, Version 9.0. San Mateo, CA: Epocrates, Inc.
www.epocrates.com. Updated November 7, 2010.
21. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 14th ed. Hudson, OH: Lexi-Comp, Inc; 2009.
22. Fick DM, Cooper JW, Wade WE, et al. Updating the Beers criteria for potentially inappropriate medication use in older adults: results of a U.S. consensus panel of experts. Arch Intern Med. 2003;163(22):2716-2724.
23. Zagaria ME. Chronic opioid therapy for noncancer pain. US Pharm. 2010;35(5):20-24.
24. Zostavax (zoster vaccine live) prescribing information. Whitehouse Station, NJ: Merck & Co, Inc; March 2011.
25. Burns CM, Farr GE. Dermatologic disorders. In: Youngkin EQ, Sawin KJ, Kissinger JF, et al, eds. Pharmacotherapeutics: A Primary Care Guide. Upper Saddle River, NJ: Pearson Prentice Hall; 2005:538.
To comment on this article, contact robdavidson@uspharmacist.com.





