US Pharm. 2015;40(11):HS34-HS40.
ABSTRACT: QT prolongation is a rare adverse event associated with many drugs, including antipsychotics and antidepressants. The majority of cases have occurred in patients taking an offending agent with multiple identifiable risk factors for corrected QT (QTc) prolongation. Typical antipsychotics have been implicated in many cases of torsades de pointes and QTc prolongation. Most atypical antipsychotics are considered to have a better cardiac profile. Tricyclic and tetracyclic antidepressants and selective serotonin reuptake inhibitors have also been linked to QTc prolongation. Serotonin norepinephrine reuptake inhibitors have a better adverse-event profile. Clinicians should strive to use antipsychotics or antidepressants with a lower risk of QTc prolongation in patients with multiple risk factors for this adverse event.
Prolongation of the QT interval is a concern for clinicians managing psychiatric drug regimens. QT-interval prolongation is estimated to occur in up to 10% of patients taking antiarrhythmic drugs with QT-prolonging potential.1 This adverse event is estimated to occur less frequently with other drugs, such as psychiatric medications.1 Although QT prolongation occurs rarely, it can lead to serious conditions such as torsades de pointes (TdP), a serious ventricular arrhythmia that can lead to sudden cardiac death.2 This review will summarize the risk factors for developing QT prolongation and the QT-prolonging potential of antipsychotics and antidepressants.
QT prolongation is an extended corrected QT (QTc) interval seen on an ECG at rest.2 Because the QT interval is dependent on heart rate, the QTc interval is calculated to control for this factor.2 QTc can be calculated by a variety of methods.3 Definitions of QTc prolongation vary, but often this condition is described as a QTc interval of >440 ms.2 Other definitions allow for a higher cutoff, such as 460 ms, in females.3
Mechanism
The QT interval represents the summation of cardiac action potentials.2 Drug-induced QT prolongation is thought to be caused by the inhibition of the delayed potassium rectifier current IKr (rapid) by specific drugs.2 IKr is an outward current controlled by potassium channels that is responsible, in part, for the repolarization of ventricular myocytes.2 When a drug interferes with this current, thereby disrupting repolarization, the QT interval is prolonged.2
Clinical Significance of QTc Prolongation
Nonpsychiatric drugs that are well known for causing QTc prolongation, such as sotalol and dofetilide, extend the QTc interval by 30 to 40 ms.4 It is agreed that this extension of the interval is clinically significant.4 Clinicians continue to debate whether a lower threshold would be clinically significant. Drugs causing only a 5- to 10-ms increase have been withdrawn from the market because of cardiac concerns, making this lower interval a common definition of drug-induced QTc prolongation.5 An increase of <5 ms is not associated with an increased risk of TdP and therefore is not considered clinically significant, whereas an increase of >5 ms carries a potential increased risk of TdP.4 An increase of >20 ms has a significant increased risk of TdP.6 For the purposes of this article, the conservative increase of >5 ms is considered clinically significant.
Risk Factors
The majority of patients who develop drug-induced QT prolongation also have multiple risk factors (TABLE 1).1 A study evaluating the frequency of risk factors for drug-induced TdP found that two or more identifiable risk factors were present in 85% of cases.7 Risk factors included heart disease (90%), age >65 years (72%), female sex (70%), multiple offending drugs (15%), and hypokalemia (13%).7 Females are at higher risk than males since testosterone shortens the QT interval.2 Hypokalemia is a risk factor owing to the role of the potassium channels in QT prolongation.2 Despite these identifiable risk factors, there is intrapersonal variability in developing QT prolongation. It has been suggested that this is due to differences in genetic polymorphisms in IKr channels.2

Psychiatric Medications of Concern
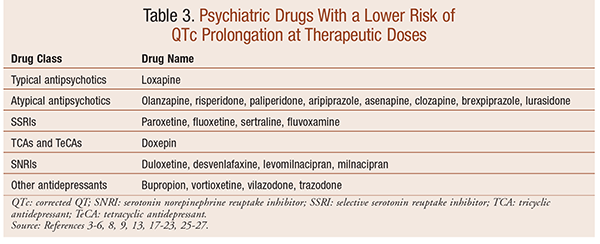
The antidepressants and antipsychotics that are correlated with a higher risk of QT prolongation are listed in TABLE 2. TABLE 3 includes medications that have been determined to have a lower risk. This determination was based on a review of literature and data from the comprehensive QT prolongation database, CredibleMeds, previously known as the University of Arizona Center for Education and Research on Therapeutics.8

Typical (First-Generation) Antipsychotics: The typical antipsychotics associated with the greatest risk of QTc prolongation are thioridazine, haloperidol, chlorpromazine, and pimozide. Harrigan and colleagues conducted an open-label, randomized, parallel-group trial of 183 patients with stable psychotic disorders who were randomized to six different antipsychotics, including thioridazine 300 mg/day and haloperidol 15 mg/day.9 Thioridazine increased the QTc interval from baseline by 30.1 ms, and haloperidol increased it by 7.1 ms.9 This is consistent with results of other published reports.2,3,10 Chlorpromazine is considered a high-risk drug for QTc prolongation, with one study finding an increased relative risk of 1.37 (95% CI 1.14-1.64).11 Pimozide, a typical antipsychotic usually reserved for patients unresponsive to standard treatment for Tourette syndrome, has also been linked to TdP, although well-designed clinical trials are lacking.8,12
Loxapine is not associated with QTc prolongation, according to a double-blind, placebo-controlled, crossover study in healthy volunteers.13 Fluphenazine, perphenazine, thiothixene, and trifluoperazine have not been evaluated, so conclusions about their QTc-prolongation potential cannot be drawn.
Atypical (Second-Generation) Antipsychotics: The atypical antipsychotics ziprasidone and iloperidone are considered to have the potential to cause clinically significant increases in QTc. Two well-designed QTc trials demonstrated that ziprasidone caused a QTc increase of 15.9 ms and 9.6 ms, respectively.9,14 Despite these findings, a post hoc analysis of phase II–IV trials involving 4,306 subjects taking ziprasidone revealed a mean change in QTc of only 3.6 ms.15 In a thorough QTc trial, iloperidone was studied at therapeutic and supratherapeutic doses in stable patients who were diagnosed with schizophrenia or schizoaffective disorder.14 Iloperidone 8 mg twice daily increased QTc by an average of 8.5 ms, 12 mg twice daily increased it by 9.0 ms, and 24 mg daily increased it by 15.4 ms.14 These results are similar to those from other trials of iloperidone.14,16 Overall, caution should be exercised with use of iloperidone and ziprasidone.
Quetiapine has had several mixed reports regarding its ability to prolong the QTc interval. Studies indicate changes in QTc intervals from –12.2 ms to 8 ms.9,10,14,17,18 A review of 12 published case reports of quetiapine-related QTc prolongation concluded that all 12 patients had at least one identifiable risk factor for QTc prolongation.10 Large-scale, thorough QTc trials are needed to clarify the prolongation risk of quetiapine.
Other atypical antipsychotics are considered to have a lower potential to increase QTc. In the trial by Harrigan and colleagues, both risperidone and olanzapine had clinically insignificant increases in QTc (3.6 ms and 1.7 ms, respectively).9 These findings are consistent with those of other trials.9,19,20 Active-control studies investigating paliperidone and asenapine also found clinically insignificant increases.17,18 Several studies, including a meta-analysis comparing atypical antipsychotics, concluded that aripiprazole is not associated with increases in QTc interval.21,22 Clozapine has been linked to TdP in case reports, but it is typically not considered to extend the QTc interval.3 The two newer atypical antipsychotics, brexpiprazole and lurasidone, have limited data but have not been shown to have significant effects on QTc interval.23 Except for ziprasidone, iloperidone, and possibly quetiapine, atypical antipsychotics are considered to have a relatively benign effect on QTc interval.
Selective Serotonin Reuptake Inhibitors (SSRIs): There are published case reports linking all six currently available SSRIs (fluvoxamine, fluoxetine, paroxetine, sertraline, citalopram, and escitalopram) to QTc prolongation.5 According to a recent meta-analysis of 16 articles representing all six currently available SSRIs, the SSRIs as a drug class may increase QTc by 6.10 ms compared with placebo (95% CI 3.47-8.73).5 Citalopram (10.58 ms), escitalopram (7.27 ms), and sertraline (3.00 ms) caused significant increases in QTc intervals, whereas fluoxetine, paroxetine, and fluvoxamine were not associated with a significant increase compared with placebo. The 3-ms increase by sertraline was not considered a clinically significant finding. The results of this meta-analysis are consistent with other findings.4 In addition to causing the largest change in QTc interval of all the SSRIs, citalopram has been linked to numerous episodes of TdP, and dosing limits have been imposed by the FDA.5,7 Clinicians should routinely monitor for QTc prolongation when citalopram and escitalopram are used at high doses or in patients with identifiable risk factors.
Tricyclic Antidepressants (TCAs) and Tetracyclic Antidepressants (TeCAs): TCAs are associated with prolongations in QTc intervals. A prospective cohort study in the Netherlands demonstrated statistically significant increases for amitriptyline (5.1 ms), imipramine (12.8 ms), maprotiline (13.9 ms), and nortriptyline (23.3 ms).24 These findings are consistent with those of other prospective studies.5,11 Desipramine, clomipramine, and trimipramine are all considered to confer a possible risk of TdP.8 Doxepin is not associated with a clinically significant increase in QTc interval, with one study demonstrating a small increase (2.38 ms).25
Serotonin Norepinephrine Reuptake Inhibitors (SNRIs): With the exception of venlafaxine, SNRIs are not associated with increased QTc intervals. The majority of studies have not shown a statistically significant increase in QTc interval with therapeutic doses of venlafaxine; however, there is some concern based on published case reports.6 Venlafaxine should be used with caution in patients with risk factors for QTc prolongation. In clinical trials, levomilnacipran, milnacipran, desvenlafaxine, and duloxetine have not demonstrated increases in QTc.6,26
Other Antidepressants: Bupropion, trazodone, vilazodone, and vortioxetine are not associated with clinically significant increases in QTc intervals at therapeutic doses.6,8,27 In some resources, mirtazapine is listed as a QT-prolonging drug; however, the evidence behind these claims has been debated.6,8 Case reports from the manufacturer and a pharmacoepidemiologic study show the potential for mirtazapine to extend the QTc interval.6 However, results of an ECG safety analysis and two toxicology studies did not find QTc prolongation with mirtazapine, even in overdose.6 Higher-quality studies are needed to further explore the relationship between mirtazapine and QTc prolongation; however, bupropion, vilazodone, and vortioxetine are considered to have minimal potential to increase QTc.
Recommendations
Pharmacists and other clinicians should consider the following recommendations when managing antidepressants and antipsychotics8:
1. Identify risk factors for QT prolongation (TABLE 1).
2. When multiple risk factors are present, strive to use drugs with less potential to cause QT prolongation (TABLE 2).
3. If a drug with higher potential (TABLE 3) is necessary and an alternative cannot be used, monitoring is recommended. Consider obtaining an ECG and serum potassium levels following initiation of the drug.1 Clinicians should consult individual package inserts for drug-specific manufacturer recommendations.
4. Additional ECG monitoring should be considered with any dose increase or the addition of a risk factor (drug interaction, concomitant use of a QT-prolonging drug, etc.).
5. Clinicians should use reliable databases, such as CredibleMeds, for quick access to up-to-date information.
Conclusion
Almost all antidepressants and antipsychotics have been linked to QT prolongation. This effect is thought to occur when specific drugs interfere with cardiac potassium channels and repolarization. It has been shown that the majority of patients who experience QT prolongation have multiple identifiable risk factors.1 The typical antipsychotics thioridazine and haloperidol have the strongest evidence linking their use to QT prolongation and TdP. Common medications that are considered to have a high risk are the SSRIs citalopram and escitalopram. New studies on this topic are expected to emerge owing to the FDA’s requirement to investigate the cardiac profiles of medications.
REFERENCES
1. Zipes DP, Camm AJ, Borggrefe M, et al. ACC/AHA/ESC 2006 Guidelines for Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death: a report of the American College of Cardiology/American Heart Association Task Force and the European Society of Cardiology Committee for Practice Guidelines (writing committee to develop Guidelines for Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death): developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society. Circulation. 2006;114:e385-e484.
2. Kallergis EM, Goudis CA, Simantirakis EN, et al. Mechanisms, risk factors, and management of acquired long QT syndrome: a comprehensive review. ScientificWorldJournal. 2012;2012:212178.
3. Wenzel-Seifert K, Wittmann M, Haen E. QTc prolongation by psychotropic drugs and the risk of Torsade de Pointes. Dtsch Arztebl Int. 2011;108:687-693.
4. Funk KA, Bostwick JR. A comparison of the risk of QT prolongation among SSRIs. Ann Pharmacother. 2013;47:1330-1341.
5. Beach SR, Kostis WJ, Celano CM, et al. Meta-analysis of selective serotonin reuptake inhibitor-associated QTc prolongation. J Clin Psychiatry. 2014;75:e441-e449.
6. Jasiak NM, Bostwick JR. Risk of QT/QTc prolongation among newer non-SSRI antidepressants. Ann Pharmacother. 2014;48:1620-1628.
7. Aström-Lilja C, Odeberg JM, Ekman E, Hägg S. Drug-induced torsades de pointes: a review of the Swedish pharmacovigilance database. Pharmacoepidemiol Drug Saf. 2008;17:587-592.
8. Woosley RL, Romero KA. QTdrugs list. www.crediblemeds.org. Accessed August 30, 2015.
9. Harrigan EP, Miceli JJ, Anziano R, et al. A randomized evaluation of the effects of six antipsychotic agents on QTc, in the absence and presence of metabolic inhibition. J Clin Psychopharmacol. 2004;24:62-69.
10. Hasnain M, Vieweg WV, Howland RH, et al. Quetiapine and the need for a thorough QT/QTc study. J Clin Psychopharmacol. 2014;34:3-6.
11. Ozeki Y, Fujii K, Kurimoto N, et al. QTc prolongation and antipsychotic medications in a sample of 1017 patients with schizophrenia. Prog Neuropsychopharmacol Biol Psychiatry. 2010;34:401-405.
12. Pimozide. Clinical Pharmacology [database]. www.clinicalpharmacology.com. Accessed August 25, 2015.
13. Spyker DA, Voloshko P, Heyman ER, Cassella JV. Loxapine delivered as a thermally generated aerosol does not prolong QTc in a thorough QT/QTc study in healthy subjects. J Clin Pharmacol. 2014;54:665-674.
14. Potkin SG, Preskorn S, Hochfeld M, Meng X. A thorough QTc study of 3 doses of iloperidone including metabolic inhibition via CYP2D6 and/or CYP3A4 and a comparison to quetiapine and ziprasidone. J Clin Psychopharmacol. 2013;33:3-10.
15. Camm AJ, Karayal ON, Meltzer H, et al. Ziprasidone and the corrected QT interval: a comprehensive summary of clinical data. CNS Drugs. 2012;26:351-365.
16. Weiden PJ, Cutler AJ, Polymeropoulos MH, Wolfgang CD. Safety profile of iloperidone: a pooled analysis of 6-week acute-phase pivotal trials. J Clin Psychopharmacol. 2008;28(2 suppl 1):S12-S19.
17. Hough DW, Natarajan J, Vandebosch A, et al. Evaluation of the effect of paliperidone extended release and quetiapine on corrected QT intervals: a randomized, double-blind, placebo-controlled study. Int Clin Psychopharmacol. 2011;26:25-34.
18. Chapel S, Hutmacher MM, Bockbrader H, et al. Comparison of QTc data analysis methods recommended by the ICH E14 guidance and exposure-response analysis: case study of a thorough QT study of asenapine. Clin Pharmacol Ther. 2011;89:75-80.
19. Czekalla J, Beasley CM, Dellva MA, et al. Analysis of the QTc interval during olanzapine treatment of patients with schizophrenia and related psychosis. J Clin Psychiatry. 2001;62:191-198.
20. Vieweg WV, Hasnain M, Hancox JC, et al. Risperidone, QTc interval prolongation, and torsade de pointes: a systematic review of case reports. Psychopharmacology (Berl). 2013;228:515-524.
21. Chung AK, Chua SE. Effects on prolongation of Bazett’s corrected QT interval of seven second-generation antipsychotics in the treatment of schizophrenia: a meta-analysis. J Psychopharmacol. 2011;25:646-666.
22. Pigott TA, Carson WH, Saha AR, et al. Aripiprazole for the prevention of relapse in stabilized patients with chronic schizophrenia: a placebo-controlled 26-week study. J Clin Psychiatry. 2003;64:1048-1056.
23. Citrome L. A review of the pharmacology, efficacy and tolerability of recently approved and upcoming oral antipsychotics: an evidence-based medicine approach. CNS Drugs. 2013;27:879-911.
24. Van Noord C, Straus SM, Sturkenboom MC, et al. Psychotropic drugs associated with corrected QT interval prolongation. J Clin Psychopharmacol. 2009;29:9-15.
25. Mansbach RS, Ludington E, Rogowski R, et al. A placebo- and active-controlled assessment of 6- and 50-mg oral doxepin on cardiac repolarization in healthy volunteers: a thorough QT evaluation. Clin Ther. 2011;33:851-862.
26. Periclou A, Palmer RH, Zheng H, Lindamood C III. Effects of milnacipran on cardiac repolarization in healthy participants. J Clin Pharmacol. 2010;50:422-433.
27. Carta MG, Pala AN, Finco G, et al. Depression and cerebrovascular disease: could vortioxetine represent a valid treatment option? Clin Pract Epidemiol Ment Health. 2015;11:144-149.
To comment on this article, contact rdavidson@uspharmacist.com.





