US Pharm. 2020;45(7/8):26-31.
ABSTRACT: Cigarette smoking harms almost every organ of the body and results in many negative health consequences, such as reproductive issues, cardiovascular diseases, chronic obstructive pulmonary disease, and several cancers. It is the leading cause of preventable disease and death in the United States and results in approximately $300 billion in direct and indirect expenses annually. Therefore, smoking cessation remains key to minimizing health and economic consequences to individuals and society. In January 2020, the Office of the Surgeon General released its first report on smoking cessation in 30 years. Smoking Cessation: A Report of the Surgeon General provides a focused update on scientific evidence regarding health benefits, effective clinical and behavioral interventions, and economic benefits of smoking cessation. In addition, the report found that more than two-thirds of U.S. adults who smoke cigarettes were interested in quitting smoking, and the majority of these individuals had attempted to quit in the past year. Pharmacists in various practice settings can assist these individuals by providing smoking-cessation screenings, education, encouragement, treatment recommendations, and support.
Cigarette smoking accounts for more than 480,000 deaths every year and remains the leading cause of preventable disease and death in the United States. In 2018, 13.7% of all adults aged 18 years or older (34.2 million people) in the U.S. were reported currently smoking combustible cigarettes, with more than 16 million Americans living with a smoking-related disease.1 Although current smoking of cigarettes has declined by an estimated 7.2% since 2005 and the number of persons who have quit smoking cigarettes has increased, this health issue continues to lead to significant disease, disability, and death.1,2
In 1964, the Office of the Surgeon General released its landmark report, Smoking and Health: Report of the Advisory Committee of the Surgeon General of the Public Health Service, on the warnings and health hazards of smoking and prioritizing the prevention of tobacco use in the U.S. Since that report, a number of other reports have also been published by the Surgeon General highlighting health risks and dangers of exposure to tobacco smoke, in addition to emerging evidence regarding the benefits of smoking cessation and electronic nicotine-delivery systems (e.g., electronic cigarettes, vaping devices) (TABLE 1).
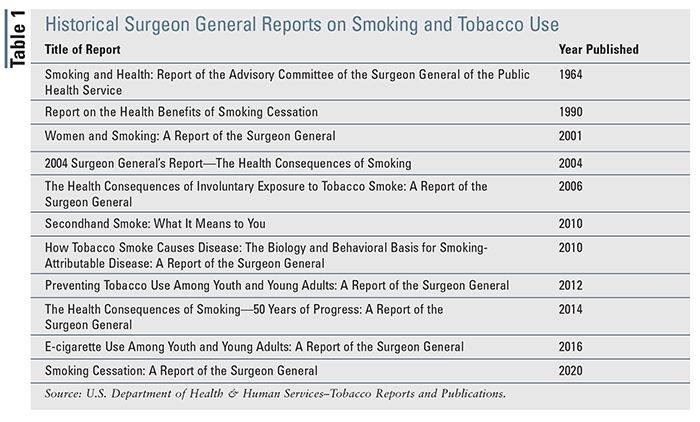
Earlier this year, the Surgeon General published its first report focused on smoking cessation in 30 years, Smoking Cessation: A Report of the Surgeon General. This publication presents updates on the health benefits of quitting smoking, as well as treatment approaches and strategies proven to assist people in successful smoking cessation.3,4 This article provides an overview of the key findings and latest evidence on the importance of smoking cessations of the 2020 report.
Overview of Key Findings
Smoking Cessation: A Report of the Surgeon General expands on the findings from the 1990 report, as well as other publications, on tobacco use from the Surgeon General. It provides major conclusions on smoking cessation that include (1) benefits seen at any age; (2) reduction of the risk in premature death and increase in life expectancy; and (3) reduction in the substantial financial burden on smokers, healthcare systems, and society. The report also found that more than two-thirds of U.S. adults who smoke cigarettes were interested in quitting, and the majority of those who smoke cigarettes have tried to quit during the past year; however, less than one-third of individuals used FDA-approved cessation medications or behavioral counseling despite the greater chance for success with these interventions, especially when used in combination.3,5
Prevalence and Patterns
There has been substantial progress among U.S. adults who smoke cigarettes in the areas of past-year quit attempts, as well as recent and long-term smoking cessation observed over the past two decades.3,5 According to the 2020 Surgeon General Report, 61.7% of U.S. adults reported as ever having smoked cigarettes have quit.3 However, survey data reveal disparities in cessation behaviors in racial/ethnic minorities, older adults, and persons with less education. Level of education is also closely related to income, health insurance status, and geographic location. Examples of these disparities include (1) individuals living in rural areas tend to have lower socioeconomic status and have been found to have lower prevalence of recent successful smoking cessation despite similar past-year quit attempts as those who live in more urban areas; (2) black adult smokers have a higher prevalence of past-year quit attempts compared with white adult smokers and use of menthol-flavored cigarettes (which may increase dependence to nicotine); and (3) number of past-year quit attempts and recent successful smoking cessation decreases as age increases.3,5
The 2020 Surgeon General report also found that advice from health professionals regarding smoking cessation has greatly increased over the past 20 years, but approximately 44% of the individuals who saw a health professional within the past year did not receive any advice regarding cessation. The use of evidence-based counseling with or without medications has also increased among adult cigarette smokers since 2000, although more than two-thirds of these individuals who tried to quit in the past year did not use any evidence-based treatment, with a large number reporting the use of non–evidence-based approaches (e.g., switching to other tobacco products). It is important to note that non–evidence-based methods, such as the use of electronic cigarettes, do not currently have adequate data to conclude that these products assist with smoking cessation to increase success rates.3
Biological Insights
Numerous novel and promising targets for smoking cessation interventions have been identified as a result of increased understanding of the neurobiologic mechanism of nicotine addiction. Preclinical studies have shown promise for targeting the multiple stages of addiction as an effective way to decrease cigarette smoking. Below are some potential therapies discussed in the 2020 Surgeon General report.3
Immunotherapies for nicotine dependence, which target the drug instead of the brain, can stimulate the production of antibodies that bind nicotine within the blood, preventing or reducing the amount delivered to the brain. Phase III clinical trials have not been as successful in demonstrating effectiveness in humans. It is believed that this may be due to differences in antibody production and the antibody concentrations needed.
Neuroimaging and genetic analyses are also being investigated as methods to identify novel therapeutic targets. Although much is known about circuit and network connections of the brain related to nicotine dependence, additional studies are needed to determine their potential roles in serving as predictive biomarkers for individualized therapy and success of cessation strategies. Transcranial magnetic stimulation is one approach being studied and needs further investigation to determine its effectiveness for smoking cessation. This is an FDA-approved treatment for depression that has also been proposed for the treatment of addiction.
In addition, genetic variances related to nAChRs (CHRNA5-A3-B4 gene cluster) and nicotine metabolism (CYP2A6 gene) have yielded the strongest evidence on potential therapeutic targets to date due to their effects on nicotine dependence and smoking intensity. Emerging evidence suggests that understanding these variations can lead to the optimization and personalization of therapeutic selections for smoking cessation.3
Health Benefits of Smoking Cessation
The 1990, 2004, and 2014 Surgeon General reports collectively identified 12 different types of cancers as causally linked to combustible cigarette smoking: lung, larynx, oral cavity and pharynx, esophagus, pancreas, bladder, stomach, liver, colon and rectum, kidney, cervix, and acute myeloid leukemia (AML).6-8 The 2020 report also highlighted these detrimental health consequences with additional evidence sufficient to suggest that smoking cessation reduces the risk of all 12 cancers linked to combustible cigarette smoking. It reported that the risk for most of these cancers drops progressively as the time since successful quitting increases. For example, the relative risk (RR) for lung cancer decreases to half for those who previously smoked compared with those who continue to smoke cigarettes for up to 15 years after cessation. Similar RR reductions have also been observed for cancers of the stomach, kidney, and cervix and AML. The studies for liver cancer were consistent with the 2014 report of the Surgeon General supporting smoking cessation for lowered risk. There is also evidence to suggest that those who previously smoked have a slightly lowered risk of developing colorectal cancers compared with those who continue to actively smoke, with the risk decreasing as the number of years since cessation increased (up to 40 years).3,7
The 2020 Surgeon General report expands on previous reports regarding the effects of cessation and the risk for cardiovascular disease (CVD), as well.5 Smoking cessation showed a reduction in the risk of CVD morbidity and mortality, which continued to decline as cessation duration increased. Smoking cessation was also found to reduce the risk of developing coronary heart disease (CHD), with risk decreasing rapidly in the period immediately following cessation, along with a slower long-term decline. In certain studies, the risk for CHD in persons who previously smoked eventually decreased to match that of individuals who never smoked. After the diagnosis of CHD, smoking cessation demonstrated a reduction in all-cause mortality, cardiac-related mortality and sudden death, and new and recurrent cardiac events. Further evidence suggests, but does not conclude, that smoking cessation was beneficial in reducing the risk of atrial fibrillation, sudden cardiac death without coronary artery disease, heart failure among former smokers, hospitalizations, peripheral arterial disease, and abdominal aortic aneurysm.5
According to the 2010 Surgeon General report, smoking cessation was the only proven strategy for reducing the pathogenetic processes leading to chronic obstructive pulmonary disease (COPD).9 The 2020 report addresses updates in this evidence and the benefits of smoking cessation. It presents a particular emphasis on the persistence of airway inflammation for years after smoking cessation and that cessation is the only intervention proven to reduce the risk for developing COPD and minimize loss of lung function over time for those already diagnosed. For patients with asthma, the 2014 report found that active smoking increased inflammation of the airways, thereby increasing asthma exacerbations and accelerating lung-function decline.8 Evidence from the current report suggests that improved lung function, reduction of symptoms, and favorable treatment outcomes were likely in asthma patients who quit smoking.3
Reproductive health benefits of smoking cessation were also emphasized in the 2020 Surgeon General report. Numerous studies were reviewed and reaffirmed findings from previous reports that smoking cessation before and during pregnancy reduces the adverse effects on fetal growth, including risk for being small for gestational age and low birth weight.3,6-8 Since fetal growth accelerates in the third trimester of pregnancy, it is beneficial to quit smoking as early as possible in the pregnancy. Additional research on the timing of cessation with respect to pregnancy onset is needed to determine how to maximize improvements in pregnancy outcomes for women and infants. Other health benefits addressed in the report include the risk reduction of (1) placental abruptions, (2) preterm delivery, (3) stillbirths, and (4) early-age menopause. Evidence regarding smoking cessation and male and female fertility remains inadequate and inconclusive.
Overall Morbidity, Mortality, and Economic Costs
All Surgeon General reports on smoking cessation have found that combustible cigarette smoking diminishes overall health and increases the risk for a number of disease states.3,6-8 The 2020 Surgeon General report brings attention to the immediate and long-term health benefits, reduced risk for various diseases, and improvement of overall health associated with smoking cessation. Recent evidence is presented and is consistent for lower morbidity and higher quality of life (QoL) scores among persons who previously smoked when compared with those who currently smoke cigarettes. In addition, higher levels of improvement in QoL were seen among those who had been smoke-free for a longer period of time.3
All-cause mortality has been extensively reviewed in previous reports and reaffirmed in the current report, as well.3,6-8 Patients who quit smoking were found to live longer than those who continued to smoke. Furthermore, persons who quit smoking before age 50 years have half the risk of dying over the next 15 years compared with those who continue to smoke. Smoking cessation at any age reduces the risk of premature death, and risk of death declines shortly after cessation and continues for at least 10 to 15 years thereafter (mirroring all-cause mortality to that of persons who never smoked). Smoking cessation by age 40 years decreased mortality by 90% compared with those who continued smoking, and premature death would be decreased by 40% if persons who smoke quit by age 60 years, validating the benefits of smoking cessation regardless of age.3
Increased morbidity and mortality associated with cigarette smoking leads to increased costs for persons who smoke cigarettes and their families, healthcare systems, and society.3,6-8 Studies have consistently showed that incorporation of nicotine replacement therapy (NRT) and/or nonnicotine pharmacotherapies (e.g., varenicline, bupropion) with counseling or quitline therapy were incrementally cost-effective versus brief counseling alone per quality-adjusted life-years (QALY) gained. One study found that one-to-one pharmacist-led interventions showed incremental cost-effectiveness ratios per QALY gained of $11,671 and ratios per quit of $2,047 compared with self-assisted quit attempts. Additionally, the incorporation of antitobacco educational programs and increased tobacco product pricing through taxation positively affected cost-effectiveness ratios per QALY gained compared with status quo.10 Regardless of methodologies, the evidence is conclusive that smoking-cessation interventions are cost-effective from an economic, healthcare, and societal perspective and should be supported and implemented as widely as possible.3
Interventions and Treatment Options
Treatment modalities were found to be efficacious when used alone or in combination with screenings, motivational interviewing, individual and group counseling, quitline counseling, and/or pharmacotherapy.3,11 FDA-approved medications along with behavioral and/or quitline counseling were proven to increase quit attempt success rates (TABLE 2). These products can be used alone, in combination, and with various behavioral therapies.3
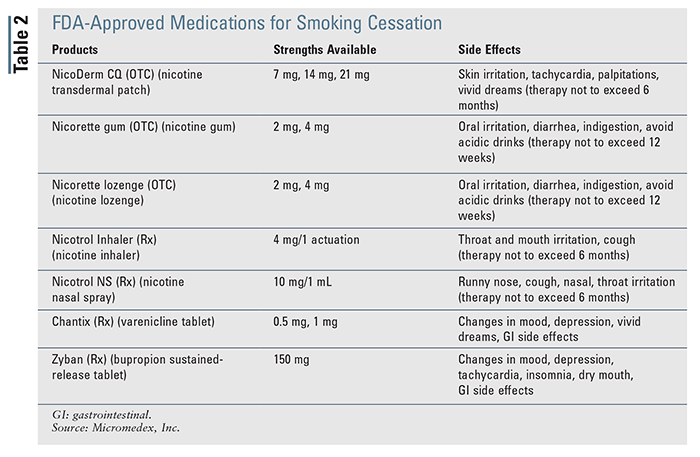
Major life events, such as hospitalization, surgery, lung-cancer screening results, and pregnancy, were noted to be catalysts in one’s readiness to quit smoking, desire to use evidence-based interventions, and ultimate success in quit attempts. The evidence overwhelmingly acknowledged that behavioral counseling strategies (e.g., behavioral therapy, cognitive behavioral therapy, motivational interviewing) and cessation medications increased the likelihood of cessation when compared with no treatment or self-help treatments alone. When used independently, they were effective in increasing smoking cessation, but the highest quit rates were achieved when used in combination, particularly in those who were considered heavy smokers. The combination of long-acting and short-acting NRT also increased cessation, and the incorporation of quitline counseling, individualized text message services, interactive Web-based interventions, and smartphone apps all positively increased smoking cessation efforts, as well.3
The literature is inconclusive on the use of electronic cigarettes as a smoking-cessation aid. Some evidence suggests that the use of nicotine-containing electronic cigarettes, in general, increases smoking cessation. Other studies suggest that more frequent use of electronic cigarettes increases smoking cessation. Further research is needed to assess how these products impact smoking cessation and to assess the potential negative consequences to their use.3
Strategies for Cessation
Smoking-cessation strategies at the clinical, health systems, and population levels collectively influence the smoking behaviors in patients in ways that increase successful smoking-cessation attempts.3,10 Actions taken at the clinical and health systems levels focus on the use and effectiveness of smoking-cessation treatments, targeting quitting behavior directly. These actions include the development and dissemination of clinical guidelines for smoking cessation, implementing policies to increase patient screening, promoting evidence-based treatments for smoking cessation, and addressing gaps in health-insurance coverage. The evidence presented in the recent report found that accessible and comprehensive health insurance increased the use of treatment services and that incentivizing clinicians, clinics, and health systems increased the rate of delivery of clinical treatments for smoking cessation.3
Population-based strategies target smoking cessation on a much broader level through patient motivation and the provision of supportive environments to lower barriers impeding successful quit attempts. Successful population-based strategies presented in the 2020 Report included increasing taxes and prices of cigarettes to reduce cigarette consumption, establishing smoking-cessation quitlines to motivate quit attempts, implementing smoke-free and tobacco-free policies in the workplace and other establishments to reduce overall smoking prevalence, funding and sustaining state tobacco control programs to help increase quit attempts, carrying out mass media campaigns which in turn increased the number of calls to quitlines, large pictorial health warnings that depict the harms from smoking to pique the interest in quitting, and public education campaigns targeting subpopulations like pregnant women and LGBT young adults.3
Conclusion
One of the most significant public-health victories over the past few decades has been the steady decline of cigarette smoking among Americans.4 However, cigarette smoking remains the predominant cause of preventable disease and death in the U.S., leading to significant disease, disability, and mortality.1,2 The combination of clinical, health systems, and population-based strategies is likely to create the most supportive environment for quit attempts and successful smoking cessation.
REFERENCES
1. Centers for Disease Control and Prevention. Current cigarette smoking among adults in the United States. www.cdc.gov/tobacco/data_statistics/fact_sheets/adult_data/cig_smoking/index.htm. 2019.
2. Creamer MR, Wang TW, Babb S, et al. Tobacco product use and cessation indicators among adults – United States, 2018. Morbidity and Mortality Weekly Report. 2019;68(45):1013-1019.
3. U.S. Department of Health & Human Services. Smoking ce
ssation: a report of the Surgeon General. www.cdc.gov/tobacco/data_statistics/sgr/index.htm. 2020.4. U.S. Department of Health & Human Services. Surgeon General releases first report focused on smoking cessation in 30 years. www.hhs.gov/about/news/2020/01/23/surgeon-general-releases-first-report-focused-on-smoking-cessation-in-30-years.html. 2020.
5. U.S. Department of Health & Human Services. Smoking cessation: a report of the Surgeon General – key findings. www.hhs.gov/surgeongeneral/reports-and-publications/tobacco/2020-cessation-sgr-factsheet-key-findings/index.html. 2020.
6. Samet JM. The 1990 report of the Surgeon General: the health benefits of smoking cessation. Am Rev Respir Dis. 1990;142(5):993‐994.
7. The 2004 United States Surgeon General’s report: the health consequences of smoking. Public Health Bull. 2004;15(5-6):107.
8. National Center for Chronic Disease Prevention and Health Promotion (U.S.) Office on Smoking and Health. The health consequences of smoking—50 years of progress: a report of the Surgeon General. Atlanta, GA: U.S. Centers for Disease Control and Prevention; 2014.
9. Centers for Disease Control and Prevention (U.S.); National Center for Chronic Disease Prevention and Health Promotion (U.S.); Office on Smoking and Health (U.S.). How tobacco smoke causes disease: the biology and behavioral basis for smoking-attributable disease: a report of the Surgeon General. Atlanta, GA: U.S. Centers for Disease Control and Prevention; www.ncbi.nlm.nih.gov/books/NBK53017/. 2010.
10. Boyd KA, Briggs AH. Cost-effectiveness of pharmacy and group behavioral support smoking cessation services in Glasgow. Addiction. 2009;104(2):317‐325.
11. Clinical practice guideline for treating tobacco use and dependence 2008 update panel, liaisons, and staff. A U.S. Public Health Service report. Am J Prev Med. 2008;35(2):158‐176.
To comment on this article, contact rdavidson@uspharmacist.com.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.





