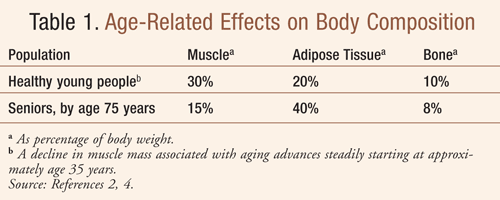
Aging causes muscle mass and muscle strength to decrease.1 By age 75 years, approximately 50% of an individual's total muscle mass has vanished.2 This age-related reduction in skeletal muscle mass is referred to as sarcopenia.3 But the process by which skeletal muscle mass progressively decreases, and thus lean body mass as well, begins occurring many years earlier--at about age 35 (TABLE 1).2,4
The cumulative loss of muscle mass results in decreased strength and exercise tolerance, weakness and fatigue, and a reduced ability to perform activities of daily living.4 Furthermore, a decrease in strength is a risk factor for poor balance, slowed gait, and falls.4 While most seniors retain adequate muscle mass and strength to perform all necessary tasks, individuals with the greatest loss in lean body mass are considered among the most vulnerable to falls and injuries.1,4 Ultimately, sarcopenia can have a profound impact on functional abilities of seniors in the oldest age brackets.4
Beyond the loss of strength, sarcopenia may alter the resting metabolic rate; irregularities in thermoregulation and the heat and cold intolerance seen in aging appear related to this occurrence.4 Additionally, the increasing insulin resistance and glucose intolerance seen in middle-aged and older-age populations is partially blamed on the gradual replacement of lean body tissue by adipose (and fibrous) tissue.4
Avoiding Prolonged Bed Rest
All patients are prone to muscle loss from prolonged bed rest.5 However, prolonged bed rest in the elderly can result in rapid acceleration of muscle loss and decrease in strength (deconditioning); additionally, stiffness of muscles, ligaments, and tendons, even to the extent of a resultant contracture, may occur.1,2,5 So significant can the muscle loss be in bedridden seniors that while complete bed rest causes young adults to lose about 1% of muscle mass per day, the elderly may lose up to 5% per day secondary to age-related decreases in growth hormone.5 In these individuals, muscle mass loss is greatest in the antigravity muscles (those used to sit up, stand up, and pull up) and can require up to 2 weeks of reconditioning to return to baseline function for each day of absolute bed rest.2 Patients should sit up in bed, transfer to a chair, stand, and exercise when safe to do so depending on their medical condition or surgical procedure.5 Patients need to be educated about the fact that avoiding sarcopenia is essential to recovery.5 Patients should be advised to avoid extended bed rest and immobilization when possible to prevent muscle weakness and joint stiffness.1
Growth Hormone Levels in Sarcopenia
Growth hormone (GH) levels decrease with aging; this decrease is probably one of many factors that contribute to sarcopenia.2 The age-related decrease in estrogen and testosterone may also reduce GH secretion.2 A number of the signs and symptoms of GH deficiency (e.g., decreased muscle mass, weakness, fatigue) are comparable to those that occur with normal aging.2 While increased muscle mass and decreased fat mass appear to occur with GH replacement therapy, muscle strength increases only to a small degree, if at all, unless GH is accompanied by weight training or is given with testosterone replacement therapy in hypogonadal men.2 GH supplementation should be used only as replacement therapy for those patients with a documented deficiency or for patients with muscle atrophy due to AIDS.2
Adverse effects associated with the supplementation of GH include arthralgias, carpal tunnel syndrome, fluid retention, glucose intolerance, gynecomastia, headaches, and lethargy.2 While long-term effects are unclear, elevated levels of GH and insulin-like growth factor I (IGF-I) in middle-aged individuals are associated with higher mortality rates than in those with lower levels of GH and IGF-I.2 While beyond the scope of this article, a broader discussion of the use and administration of GH supplementation, contraindications, IGF-I, and alternatives to GH may be found in Section 8, chapter 66 in Reference 2.
Exercise Intervention
When older adults remain healthy, they usually can climb stairs, rise from a squatting position, walk along a straight line, hop on either foot, and perform typical activities of daily living with ease.2 However, while maximum isometric contraction force is reduced approximately 20% by age 50, by age 70 the reduction reaches about 50%.2 This occurs because slower-contracting type I fibers function to maintain posture and to perform rhythmic, endurance-type exercises, while the faster-contracting type II muscle fibers that contribute to sudden powerful muscle contractions decrease with aging to a greater extent than do type I fibers.2
Regular exercise can partially overcome or significantly delay loss of muscle mass and strength, and participation in regular strength-training exercises is considered essential to staying strong and vital in one's senior years.6 By stimulating the growth of muscle and bone, strength-training exercises help to prevent osteoporosis and frailty.6 When individuals feel physically strong, mental and emotional health is promoted as well.6 Programs to guide seniors with strength training (see Strength Training for Seniors, page 30) have the potential not only to help them become stronger, but to assist with maintenance of health and independence (TABLE 2). Extensive scientific study has shown that this type of exercise is safe and effective.7 Even seniors who have never exercised before can increase muscle mass and strength through strength-training exercises.1

Pharmacist Counseling: Safe Medication Use During Exercise
Pharmacists play an important role in counseling patients who receive medication therapy while engaging in strength-training exercises. The following are examples of medications requiring special instructions for the patient:
Beta-blockers prevent the use of the target heart rate method for monitoring of endurance intensity; these agents have the potential to mask hypoglycemic symptoms other than sweating.7-9
Insulin and oral hypoglycemic agents may require dosage adjustments to avoid hypoglycemia during exercise; patients with non-insulin-dependent diabetes benefit from an exercise-induced rise in insulin sensitivity that eases the uptake of glucose by muscle tissue.7-9
Medications with the potential to cause orthostatic hypotension (e.g., antihypertensives, diuretics, antidepressants, anxiolytics, sedative-hypnotics) may require downward dosage adjustments to prevent exacerbation of orthostasis caused by fluid loss during exercise (which may result in presyncope or syncope).7-9 Patients should be made aware that adequate fluid intake is essential during exercise.7-9
Medications with anabolic activity (e.g., GH, estrogen, testosterone, vitamins) have been suggested as a modality to build muscle mass in seniors with sarcopenia.7 However, studies using various hormones have shown the following: 1) mixed results with exogenous growth hormone; 2) the effect of estrogen replacement on muscle strength is limited and inconsistent; 3) testosterone replacement for men with hypogonadism, while appearing to increase muscle strength, lacks dose-response information, and adverse effects such as prostate cancer remain a concern.7
Sedative-hypnotics can potentially reduce physical performance (i.e., directly through inhibiting effects on muscles and nerves or indirectly by a reduction in activity levels) and are associated with the risk of falls.7-9 In order to improve the safety of exercise and to increase patient adherence to an exercise program, dosage reduction or discontinuation may be required.7-9
Strength Training for Seniors
Nelson and Wernick indicate that many sedentary individuals want to change; however, they do not have the accurate and practical information necessary to commence.10 In their book entitled Growing Stronger: Strength Training for Older Adults (see Resource), Seguin et al provide a highly effective program that is safe, simple, and based on the principles of strength training.7 According to the authors, worldwide laboratory research has shown that strength training not only benefits both men and women of all ages, but of all levels of fitness as well.7 Furthermore, such a program can play a role in helping to prevent and treat chronic conditions such as arthritis and osteoporosis, among others (TABLE 3).7 The program was developed at the Nutrition, Exercise Physiology and Sarcopenia Laboratory at Tufts University and includes motivational tips, safety precautions, and specific exercises. It is comprised of three phases: Part I uses an individual's own body weight to strengthen the body slowly and gently; Part II introduces dumbells and ankle weights to increase strength; and Part III adds variety so that new techniques boost strength further.7


Seguin et al note the goal of Growing Stronger: Strength Training for Older Adults is to help seniors make strength training a lifelong habit. To that end, the program is tailored to the needs of an older adult and provides step-by-step instructions on getting started, staying on track, and growing stronger and healthier as one ages.7
Conclusion
Strength-training exercises have the potential to make a profound difference in a senior's physical, mental, and emotional health. It can help both male and female older adults, at all fitness levels, reach toward greater strength and vitality and maintain independence. Pharmacists have the potential to make a difference in the lives of older adults by appropriately recommending the role of strength training in a plan of care and by counseling patients on safe medication use during exercise.
REFERENCES
1. Beers MH, Jones TV, Berkwits M, et al, eds. The Merck Manual of Health & Aging. Whitehouse Station, NJ: Merck Research Laboratories; 2004:13-14, 128.
2. Beers MH, Jones TV, Berkwits M, et al, eds. The Merck Manual of Geriatrics. Whitehouse Station, NJ: Merck Research Laboratories; 2009-2010: Section 3, chapter 31; Section 7, chapter 48; Section 8, chapter 66. www.merck.com/mkgr/mmg/contents.jsp. Accessed August 10, 2010.
3. Dorland's Pocket Medical Dictionary. 28th ed. Elsevier Saunders; 2009.
4. Fried LP, Walston J. Frailty and failure to thrive. In: Hazzard WR, Blass JP, Halter JB, et al, eds. Principles of Geriatric Medicine and Gerontology. 5th ed. New York, NY: McGraw-Hill, Inc; 2003:1487-1502.
5. Beers MH, Porter RS, Jones TV, et al. The Merck Manual of Diagnosis and Therapy. 18th ed. Whitehouse Station, NJ: Merck Research Laboratories; 2006:2748.
6. Satcher D. Introduction. In: Seguin RA, Epping JN, Buchner DM, et al. Growing Stronger: Strength Training for Older Adults. Boston, MA and Atlanta, GA: Tufts University Nutrition and the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention; 2002. www.cdc.gov/nccdphp/dnpa/physical/growing_stronger/growing_stronger.pdf. Accessed August 10, 2010.7. Seguin RA, Epping JN, Buchner DM, Growing Stronger: Strength Training for Older Adults. Boston, MA and Atlanta, GA: Tufts University Nutrition and the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention; 2002. www.cdc.gov/nccdphp/dnpa/physical/growing_stronger/growing_stronger.pdf. Accessed August 10, 2010.
8. My Epocrates, Version 9.0. San Mateo, CA: Epocrates, Inc. www.epocrates.com. Accessed August 12, 2010.
9. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 14th ed. Hudson, OH: Lexi-Comp, Inc; 2009.
10. Nelson ME, Wernick S. Strong Women Stay Young. New York, NY: Bantam Books; 1997.
To comment on this article, contact rdavidson@uspharmacist.com.




