US Pharm. 2016;41(2)(Specialty&Oncology suppl):3-7.
ABSTRACT: Rheumatoid arthritis (RA) is a chronic, inflammatory, systemic autoimmune disorder. In the United States, the decreased quality of life and increased medical costs and healthcare utilization associated with RA have resulted in a high disease burden. The development of more effective and sustainable drug-treatment strategies for RA is necessary to combat disease progression and growing expenses. Treatment guidelines for RA have changed with the development of new biologic disease-modifying antirheumatic drugs (bDMARDs) in recent years. Their unique molecular specificity and proven efficacy make the newer bDMARDs attractive options for patients with moderate-to-severe RA. In choosing the most effective pharmacotherapeutic regimen, pharmacists should carefully consider disease severity, the patient’s response to therapy, and the drugs’ contraindications and adverse events.
Rheumatoid arthritis (RA) is a chronic, inflammatory, systemic autoimmune disorder characterized by symmetrical, erosive synovitis frequently leading to joint destruction, deformity, and disability.1,2 The prevalence of RA in the United States is estimated to be between 0.5% and 1% of the adult population. The incidence rate is roughly twice as high in women as in men (7.7/1,000 vs. 4.4/1,000). In general, the incidence of RA increases with age. In 2007, the rate in persons aged 18 to 34 years was 8.7 per 100,000 compared with 54 per 100,000 in those aged 85 years and older; the peak incidence occurred between ages 65 and 74 years regardless of gender.3
The premature mortality, decreased quality of life, and direct and indirect patient, employer, and government costs associated with RA place a large disease burden on the U.S. Of RA-related expenditures in 2005, nearly $39.2 billion was due to mortality and deteriorating quality of life, $8.4 billion was due to out-of-pocket medical expenses for numerous office visits and hospitalizations, and $10.9 billion was due to decreased work productivity, job loss, and disability payments by employers and the government.4 The development of more effective and sustainable RA drug-treatment strategies is necessary to counter disease progression and the increasing disease burden in the U.S.
The American College of Rheumatology (ACR) has issued guidelines for the management of RA, and the expert panel strongly recommends a treat-to-target strategy for both early and established RA.2 This strategy, which is based on disease activity, the patient’s risk tolerance, and comorbidity, aims to optimize RA outcomes by adjusting therapy. For early RA (disease duration <6 months), the panel strongly recommends the use of monotherapy with conventional disease-modifying antirheumatic drugs (cvDMARDs), specifically methotrexate (MTX), for DMARD-naïve patients with low, moderate, or high disease activity, in conjunction with short-term glucocorticoids if a patient experiences an arthritic flare. Patients who fail DMARD monotherapy and still have moderate-to-high disease activity should receive a combination of cvDMARDs or a tumor necrosis factor (TNF) inhibitor ± MTX, a non-TNF inhibitor biologic ± MTX, or tofacitinib + MTX.5 New evidence indicates that to slow down joint damage, preserve functioning, and improve long-term outcomes in patients with moderate-to-severe RA, the use of MTX plus biologics early in the treatment protocol often produces better results than the stepwise approach or monotherapy. However, management options are often limited to cvDMARDs owing to the increased potential for severe adverse events (AEs) and the higher cost of biologics. This paper will review the profiles of three recently approved biologic DMARDs (bDMARDs; certolizumab pegol [CZP], golimumab [GOL], and tocilizumab (TCZ]) and a Janus kinase (JAK) inhibitor (tofacitinib) for the treatment of RA (TABLE 1).

Etiology and Pathophysiology
The exact etiology of RA is unknown; however, it is hypothesized that genetics and the environment are contributing factors.6 The proposed mechanism of RA development appears to be immune-system alteration caused by changes in B- and T-cell levels of proinflammatory and anti-inflammatory cytokines.7 The T-lymphocyte immune response to autoantigens mediated by activation of the cell-surface receptor HLA-DR4 (major histocompatibility complex gene product), as well as malfunctions of the humoral cell, leads to progressive inflammation and joint destruction.8 Joint damage begins with the proliferation of synovial fibroblasts and macrophages, infiltration of lymphocytes, and proliferation of endothelial cells. The blood vessels in the affected joint become occluded with inflammatory cells, and eventually inflamed synovial tissue begins to grow irregularly, forming invasive pannus tissue that destroys cartilage and bone.6 In addition, the release of cytokines, interleukins (ILs), proteinases, and growth factors results in further joint destruction and the development of systemic complications including—but not limited to—pulmonary fibrosis, digital vasculitis, skin ulceration, splenomegaly, and pericarditis.9
Although a wide variety of proinflammatory substances contribute to joint and systemic complications, IL-1, IL-6, and TNF-alpha are key players in the manifestation of RA.10 IL-1 regulates the immune response and causes an inflammatory reaction; IL-6 has various biological functions, including B-cell, neutrophil, and osteoclast maturation and stimulation of a growth factor that promotes synovitis and joint destruction. TNF-alpha is a cell-signaling protein that is involved in acute-phase reactions and systemic inflammation; its inhibitory effect results in a lessened inflammatory response. Systemic manifestations result from IL-6 and production of hepcidin.11 JAKs, which were recently discovered, are intracellular enzymes that influence the signaling cascade, resulting in cytokine or growth-factor receptor interactions on the cellular membrane that modulate gene expression and intracellular activity in RA.12 bDMARDs play a significant role by targeting sensitive inflammatory markers. Five of the 10 available bDMARDs inhibit TNF-alpha by neutralizing its activity or reducing its effect.13
Pharmacologic Management
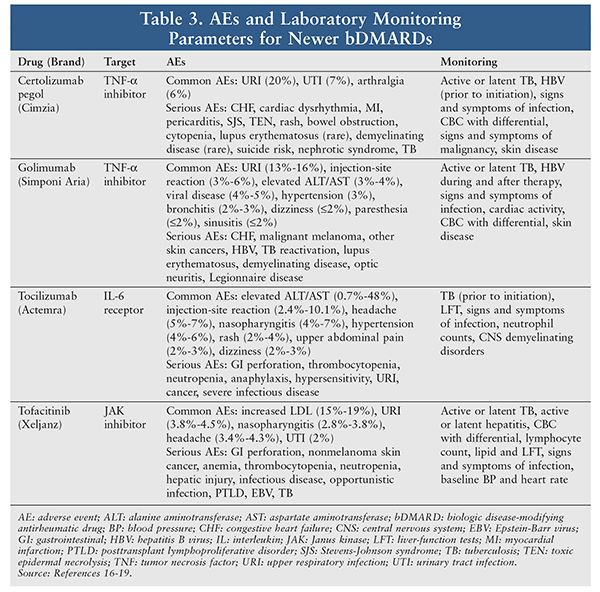
bDMARDs are categorized as TNF antagonists (anti-TNFs; i.e., CZP and GOL) or non-TNF inhibitors (i.e., tofacitinib). These agents are generally used in patients with moderate-to-severe RA in whom cvDMARDs have failed,5 based on safety concerns regarding prolonged use (TABLES 2 and 3).

The ACR 2012 guidelines recommend that bDMARDs be started when there is high disease activity with a poor prognosis factor in a patient in whom cvDMARDs have failed. However, in the ACR 2015 guidelines, the order in which to use bDMARDs was not established owing to the limited number of comparative studies that combined cvDMARDs or added biologics or tofacitinib during clinical trials. This means that bDMARDs may be used as first-line treatment in patients with high disease activity with poor prognostic factors.14 Data comparing the efficacy of the four newer bDMARDs are insufficient; however, various combinations of bDMARDs plus MTX were associated with more positive outcomes in clinical trials, compared with monotherapy with either bDMARDs or MTX (TABLE 4).15
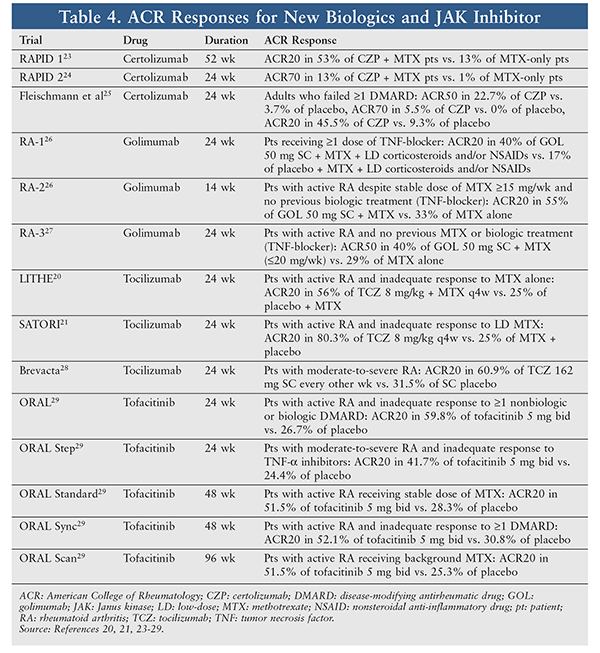
CZP: This TNF-alpha inhibitor, which is recommended for adults with moderate-to-severe active RA, may be used concomitantly with MTX or as monotherapy in patients unresponsive to cvDMARDs. Three randomized, placebo-controlled trials showed significant clinical improvement in patients taking CZP, as demonstrated by ACR response rates (TABLE 4).16 Dosages exceeding 400 mg SC every 2 weeks did not significantly improve ACR responses. The most common AEs were upper respiratory infection, arthralgia, and urinary tract infection (TABLE 3).16 Before initiation, patients should be evaluated for active or inactive tuberculosis (TB) and hepatitis B virus (HBV). If the patient is positive for latent TB, TB treatment should be initiated prior to CZP therapy. HBV carriers receiving CZP should be monitored closely before and during the course of therapy. If HBV reactivation occurs, CZP should be discontinued, based on case reports of death from HBV reactivation. Cases of worsening and new-onset congestive heart failure have been reported; therefore, CZP is contraindicated in patients with moderate-to-severe heart failure (New York Heart Association [NYHA] Class III/IV). Patients should be monitored for clinical signs of infection and for liver enzymes and renal function if symptomatic, and ECG and CBC with differential should be performed (TABLE 3). Because of drug-induced immunosuppression, live vaccination should be avoided. CZP must be refrigerated prior to use and kept at room temperature for 30 minutes before injection.16
GOL: This agent is an anti-TNF monoclonal antibody (Mab) that binds to TNF-alpha with high affinity. It is indicated in combination with MTX in adults with moderate-to-severe active RA. GOL was shown to be significantly more efficacious than placebo, improving ACR responses at weeks 14 and 24 in the treatment of active RA when combined with MTX (TABLE 4). As with CZP, patients should be screened for latent or active TB before therapy initiation and monitored periodically during therapy for latent infection. If the patient has latent TB, this must be treated before initiating GOL in order to minimize or prevent serious infection. GOL should be withheld in patients with a serious bacterial, viral, or fungal infection or moderate-to-severe heart failure (NYHA Class III/IV).17
TCZ: TCZ is an anti–IL-6 Mab used in combination with DMARDs as an SC or IV injection for moderate-to-severe RA in patients with an inadequate response to anti-TNF agents. During two phase III trials, TCZ with or without MTX demonstrated superior efficacy, improving ACR response rates at 24 weeks in the treatment of active RA (TABLE 4). IV dosing, which is initiated at 4 mg/kg every 4 weeks, may be increased to 8 mg/kg every 4 weeks. In SC dosing, patients weighing <100 kg receive 162 mg every other week and those >100 kg receive 162 mg every week. Importantly, TCZ should not be initiated in patients with an absolute neutrophil count (ANC) <2,000 per mm3, platelet count <100,000 per mm3, or alanine aminotransferase (ALT) or aspartate aminotransferase (AST) >1.5 times the upper limit of normal. The most common AEs with TCZ include hypertension, injection-site reaction, diarrhea, elevation of liver enzymes and lipid levels, decreased blood cell counts, and increased risk of nasopharyngitis. When TCZ therapy is initiated, it is important to monitor neutrophil and platelet counts and lipid and ALT/AST levels at baseline, after 4 to 8 weeks, and every 3 to 6 months thereafter (TABLE 3).18
Tofacitinib: This agent is indicated for monotherapy or in combination with MTX or other cvDMARDs (except azathioprine or cyclosporine) in adults with moderately to severely active RA with an inadequate response or intolerance to MTX. Tofacitinib should not be combined with bDMARDs. During phase III placebo-controlled trials, tofacitinib with or without MTX demonstrated a 20% improvement in ACR response. The recommended dosage is 5 mg orally twice daily; however, if tofacitinib is combined with a potent CYP3A4 inhibitor, the recommended dosage is 5 mg daily. Tofacitinib should not be initiated in patients with an ANC <1,000 cells/mm3, lymphocyte count <500 cells/mm3, or hemoglobin (Hb) level <9 g/dL. As with the previously mentioned TNF inhibitors, it is imperative to screen for HBV and latent or active TB before starting treatment because of the greater chance of disseminated TB (TABLE 3). The most common AEs include elevated LDL, elevated liver enzymes, hypertension, and lower RBC counts. Therefore, it is recommended to monitor for neutrophil counts, Hb, and lipid parameters at baseline, after 4 to 8 weeks of treatment, and every 3 months thereafter. When tofacitinib is being considered in patients of Asian ancestry aged 65 years and older, caution should be exercised owing to the increased risk of infection, including herpes zoster.19
Conclusion
Given the number of patients in the U.S. with RA, the ACR guidelines strongly recommend the treat-to-target strategy over the nontargeted approach in early and established RA cases. To achieve positive outcomes in RA, patients with moderate-to-severe disease activity and lack of disease remission on DMARD monotherapy should receive a combination of cvDMARDs or TNF inhibitor ± MTX, a non-TNF inhibitor ± MTX, or tofacitinib plus MTX.5
The focus of this article was to assess the contributions of the three newest bDMARDs (CZP, GOL, and TCZ) and the JAK inhibitor tofacitinib to RA management. The unique advantage of these newer agents is their affinity to target specific cytokines and other proinflammatory mediators that trigger the autonomic response and cause pain and deformity in the joints of patients with RA. Multiple clinical trials using the ACR criteria have demonstrated benefits of early treatment with these specialty medications ± MTX in patients who have had RA for at least 6 months. These medications are important additions to the arsenal of treatments for RA because they reduce inflammation and increase remission rates.20,21 Although these agents have great advantages for RA management, they also present some potential AEs. Therefore, it is important for physicians and pharmacists to counsel their patients so as to achieve the best clinical outcomes. Optimizing patient compliance with medication adherence, timely laboratory monitoring, and physician follow-up can significantly reduce the symptoms and slow down the disease progression of RA. Pharmacists can play a key role in the success of a patient’s medication adherence by providing counseling regarding the proper dosage, route of administration, onset of action, and AEs, as well as the importance of follow-up via laboratory monitoring and medication refills.
REFERENCES
1. Majithia V, Geraci SA. Rheumatoid arthritis: diagnosis and management. Am J Med. 2007;120:936-939.
2. American College of Rheumatology Subcommittee on Rheumatoid Arthritis Guidelines. Guidelines for the management of rheumatoid arthritis: 2002 update. Arthritis Rheum. 2002;46:328-346.
3. Myasoedova E, Crowson CS, Kremers HM, et al. Is the incidence of rheumatoid arthritis rising?: results from Olmsted County, Minnesota, 1955-2007. Arthritis Rheum. 2010;62:1576-1582.
4. Birnbaum H, Pike C, Kaufman R, et al. Societal cost of rheumatoid arthritis patients in the US. Curr Med Res Opin. 2010;26:77-90.
5. Singh JA, Furst DE, Bharat A, et al. 2012 update of the 2008 American College of Rheumatology recommendations for the use of disease-modifying antirheumatic drugs and biologic agents in the treatment of rheumatoid arthritis. Arthritis Care Res (Hoboken). 2012;64:625-639.
6. Rindfleisch JA, Muller D. Diagnosis and management of rheumatoid arthritis. Am Fam Physician. 2005;72:1037-1047.
7. Edwards CJ, Cooper C. Early environmental factors and rheumatoid arthritis. Clin Exp Immunol. 2006;143:1-5.
8. Doherty M, Lanyon P, Ralston SH. Musculoskeletal disorders. In: Boon NA, Colledge NR, Walker BR, eds. Davidson’s Principles and Practice of Medicine. 20th ed. Edinburgh, Scotland: Churchill Livingstone Elsevier; 2006:1100-1106.
9. Turesson C, Matteson EL. Clinical features of rheumatoid arthritis: extra-articular manifestations. In: Hochberg MC, Silman AJ, Smolen JS, et al, eds. Rheumatoid Arthritis. Philadelphia, PA: Mosby Elsevier; 2009:62-67.
10. Feldmann M, Brennan FM, Maini RN. Role of cytokines in rheumatoid arthritis. Annu Rev Immunol. 1996;14:397-440.
11. Srirangan S, Choy EH. The role of interleukin 6 in the pathophysiology of rheumatoid arthritis. Ther Adv Musculoskelet Dis. 2010;2:247-256.
12. Zerbini CA, Lomonte AB. Tofacitinib for the treatment of rheumatoid arthritis. Expert Rev Clin Immunol. 2012;8:319-331.
13. Zalevsky J, Secher T, Ezhevsky SA, et al. Dominant-negative inhibitors of soluble TNF attenuate experimental arthritis without suppressing innate immunity to infection. J Immunol. 2007;179:1872-1883.
14. Singh JA, Saag KG, Bridges SL Jr, et al. 2015 American College of Rheumatology Guideline for the Treatment of Rheumatoid Arthritis. Arthritis Care Res (Hoboken). November 6, 2015 [Epub ahead of print].
15. Donahue KE, Gartlehner G, Jonas DE, et al. Systematic review: comparative effectiveness and harms of disease-modifying medications for rheumatoid arthritis. Ann Intern Med. 2008;148:124-134.
16. Cimzia (certolizumab pegol) product information. Smyrna, GA: UCB, Inc; October 2015.
17. Simponi Aria (golimumab) product information. Horsham, PA: Janssen Biotech, Inc; August 2015.
18. Actemra (tocilizumab) product information. South San Francisco, CA: Genentech, Inc; October 2013.
19. Xeljanz (tofacitinib) product information. New York, NY: Pfizer Inc; June 2015.
20. Kremer JM, Blanco R, Brzosko M, et al. Tocilizumab inhibits structural joint damage in rheumatoid arthritis patients with inadequate responses to methotrexate: results from the double-blind treatment phase of a randomized placebo-controlled trial of tocilizumab safety and prevention of structural joint damage at one year. Arthritis Rheum. 2011;63:609-621.
21. Nishimoto N, Miyasaka N, Yamamoto K, et al. Study of active controlled tocilizumab monotherapy for rheumatoid arthritis patients with an inadequate response to methotrexate (SATORI): significant reduction in disease activity and serum vascular endothelial growth factor by IL-6 receptor inhibition therapy. Mod Rheumatol. 2009;19:12-19.
22. RED BOOK Online [Micromedex 2.0; subscription database]. Greenwood Village, CO: Truven Health Analytics, Inc; 2015.
23. van der Heijde D, Strand VD, Keystone E, et al. Inhibition of radiographic progression by lyophilized certolizumab pegol added to methotrexate in comparison with methotrexate alone in patients with rheumatoid arthritis/the RAPID 1 trial. Poster presented at: 71st Annual Scientific Meeting of the American College of Rheumatology; November 6-11, 2007; Boston, MA. Abstract 940.
24. Smolen J, Landewé RB, Mease P, et al. Efficacy and safety of certolizumab pegol plus methotrexate in active rheumatoid arthritis: the RAPID 2 study. A randomised controlled trial. Ann Rheum Dis. 2009;68:797-804.
25. Fleischmann R, Vencovsky J, van Vollenhoven RF. Efficacy and safety of certolizumab pegol monotherapy every 4 weeks in patients with rheumatoid arthritis failing previous disease-modifying antirheumatic therapy: the FAST4WARD study. Ann Rheum Dis. 2009;68:805-811.
26. Inman RD, Davis JC Jr, Heijde Dv, et al. Efficacy and safety of golimumab in patients with ankylosing spondylitis: results of a randomized, double-blind, placebo-controlled, phase III trial. Arthritis Rheum. 2008;58:3402-3412.
27. Keystone EC, Genovese MC, Klareskog L, et al. Golimumab, a human antibody to tumour necrosis factor a given by monthly subcutaneous injections, in active rheumatoid arthritis despite methotrexate therapy: the GO-FORWARD Study. Ann Rheum Dis. 2009;68:789-796.
28. Kivitz A, Olech E, Borofsky M, et al. Subcutanous tocilizumab versus placebo in combination with disease-modifying antirheumatic drugs in patients with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2014;66:1653-1661.
29. Lundquist LM, Cole SW, Sikes ML. Efficacy and safety of tofacitinib for treatment of rheumatoid arthritis. World J Orthop. 2014;5:504-511.
To comment on this article, contact rdavidson@uspharmacist.com.






