US Pharm. 2021:46(5):HS-7-HS-12.
ABSTRACT: Mental health concerns have risen amid the coronavirus disease 2019 (COVID-19) pandemic. Depression and anxiety symptoms are exacerbated due to fear, uncertainty, and social isolation. Full mental health assessments of patients affected by COVID-19 should be completed to help guide treatment of depression and anxiety. Pharmacists can ensure that appropriate treatment is initiated and continued with appropriate monitoring. Treatment is individualized based on comorbidities, interactions, and patient needs. Telehealth solutions are utilized in the inpatient and outpatient settings to provide mental health services. Ultimately, additional research is needed regarding the long-term impact of the COVID-19 pandemic on mental health.
The coronavirus disease 2019 (COVID-19) is a profound global pandemic declared on March 11, 2020, by the World Health Organization. Statistics as of March 12, 2021, indicate over 118 million infections and 2.6 million deaths worldwide.1 Mental health concerns have risen amid the global pandemic due to a variety of factors, including stay-at-home orders, social distancing, fear of sickness and death, loss of employment, and loss of family and friends due to illness.2 A systematic review of the impact of the COVID-19 pandemic showed a 14.6% to 48.3% prevalence of depression symptoms in the general population.3
With concern for depression and other mental health conditions in the general population, there is also a significant worry for those who are hospitalized with COVID-19. Hospitalized patients face the previously mentioned risk factors for depression in COVID-19. They are also isolated from visitors while battling the illness in the inpatient setting. A hospital in Wuhan, China, the city and country where the virus is thought to originate, reported depressive symptoms in 13.4% of hospitalized patients with COVID-19.4 This article will focus on considerations in depression and anxiety treatment for inpatient and outpatient COVID-19 patients and resources available for patients and healthcare workers.
Treatment of Depression
Infectious epidemics are linked to anxiety, panic, and stress. It is believed that patients who have COVID-19 may suffer from anxiety, mood dysregulation, and worsening of preexisting mental illnesses.5 There are multiple guidelines addressing treatment of major depressive disorder (MDD), including the Department of Veterans Affairs/Department of Defense (VA/DoD) guidelines and the American Psychiatric Association guidelines, yet there are currently no specific guidelines for depression treatment in patients diagnosed with COVID-19. It is important to note that symptoms of depression do not equate to a MDD diagnosis, although symptomatic patients may require similar treatment. In patients with depressive symptoms, it is important to evaluate the patient’s psychiatric history, including current treatments, responses to previous treatments, past hospitalizations or suicide attempts, and the presence of co-occurring psychiatric disorders.6
Considerations for the treatment of depression in patients with COVID-19 are important. First, a complete assessment is required to determine the diagnosis and depression severity. Once a patient is diagnosed with depression or is found to have a history of depression, appropriate therapy should be initiated or continued, if possible. Currently, inpatient and outpatient depression treatment is guided by MDD guideline recommendations. The VA/DoD Clinical Practice Guideline for the Management of Major Depressive Disorder recommends evidence-based psychotherapy and/or evidence-based pharmacotherapy as first-line treatment for mild-to-moderate MDD.7
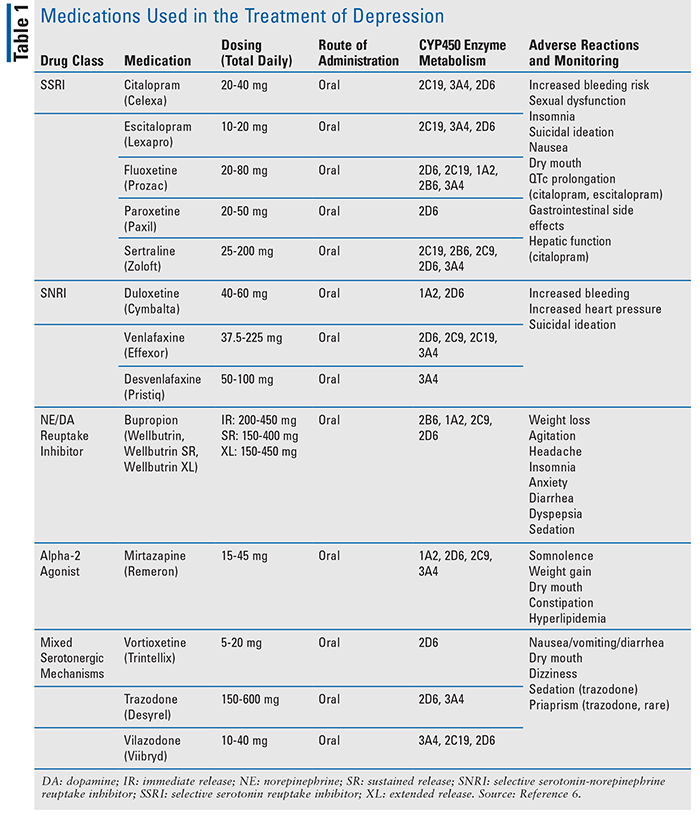
First-line pharmacotherapy includes selective serotonin reuptake inhibitors (SSRIs), selective serotonin-norepinephrine reuptake inhibitors (SNRIs), mirtazapine, and bupropion. Other agents, such as trazodone and vortioxetine, may also be used as adjuncts to depression treatment, among others.7 TABLE 1 provides drug dosing, metabolism, side effect, and monitoring information for first-line agents and a focused list of adjunct treatments. Antidepressant medications generally require at least 4 to 6 weeks to achieve maximum therapeutic effects.6 If moderate improvement is not observed with maximally tolerated doses following 4 to 8 weeks of treatment, reassessment and adjustment of the pharmacotherapy should be considered. This includes a dose increase, switching to a different antidepressant, or augmenting with a different agent.
When starting pharmacotherapy or psychotherapy in patients with COVID-19 and depression, it is important that the patient has scheduled follow-up with their primary care provider or behavioral health professional to manage depression treatment. Additionally, it is crucial to ensure that if the patient was already taking antidepressant therapy, they are continued on their regimen. This should be considered barring any contraindications or changes in health status that warrant holding those medications.
Treatment of Anxiety
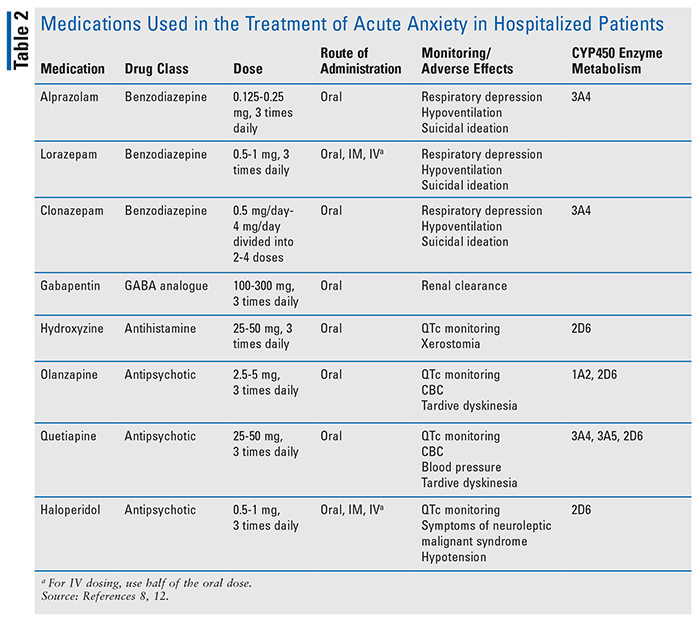
Currently, there are no specific guidelines regarding the treatment of COVID-19 anxiety. The current treatment approach is guided by individualizing therapy for each patient based on patient’s medical comorbidities, drug interactions, and preexisting mental illness. A combination of psychopharmacology and psychotherapy is recommended.8 TABLE 2 shows some medications, including common dosages and monitoring parameters, that can be used to treat acute anxiety in hospitalized patients. Managing acute anxiety pharmacologically differs significantly from managing chronic anxiety disorders.
Benzodiazepines may be considered for short-term use in certain patients given the immediate anxiolytic effect. Prior to initiation of a benzodiazepine, the cause of the anxiety should be evaluated since anxiety can be characteristic of acute respiratory decompensation where administration of benzodiazepines could worsen respiratory function. If benzodiazepine use is warranted, short-acting benzodiazepines such as alprazolam and lorazepam are preferred, and using the lowest effective dose is called for. Patients on a home regimen would want to continue to minimize risk of withdrawal. The route of administration of a benzodiazepine may guide the use of a certain benzodiazepine. For instance, alprazolam is only available orally while lorazepam can be administered orally, IV, and IM. In certain circumstances, a continuous infusion of benzodiazepine may be administered to attain light sedation with daily sedation interruption in critically ill, mechanically ventilated patients with COVID-19.9 Benzodiazepines have the potential to increase the risk of delirium in critically ill patients and should be closely monitored.
Alternative treatment options include gabapentin, which has shown benefit in treatment of anxiety disorders and alcohol withdrawal even though it has not been approved by the FDA for the treatment of anxiety.10 Hydroxyzine is sometimes used in children and young adults.8 Sedation is minimal with these medications, and delirium is less likely to occur in hospitalized patients compared with benzodiazepines.
Even though antipsychotics are not approved by the FDA for treatment of anxiety, there is supporting literature showing olanzapine or quetiapine have been effective for treatment-refractory anxiety and insomnia.8 Low-dose IM haloperidol may be considered with telemetry monitoring for ventricular arrhythmias and QTc prolongation in addition to monitoring for potential dystonic reactions.8 There is an increased risk of QTc prolongation when antipsychotics are administered with other medications, including antibiotics and antivirals for the treatment of COVID-19, which would require additional monitoring.11
Telehealth Services
Given the CDC recommendations for social distancing to reduce transmission of COVID-19, telehealth services have greatly expanded since the start of the pandemic.13 Previously, telehealth was used primarily in areas with decreased access to certain services (e.g., rural areas). A subset of telehealth is providing behavioral and/or mental health care services using technological modalities instead of, or in addition to, in-person methods. Remote behavioral therapy or psychotherapy requires HIPAA-compliant phone calls, video conferencing, or text-based messaging.14 Now that high-quality technology is more accessible, telehealth services for mental health are often implemented in hospital systems, allowing the patient to connect with a remote provider and receive care while practicing social distancing. This approach has also been successful in the outpatient setting by increasing access to services, especially if patients have transportation issues. Additionally, Centers for Medicare & Medicaid Services has expanded billing codes for telepsychiatry appointments both in the inpatient and outpatient setting. Yet, the continuation of these expansions is uncertain past the pandemic.13
Mental Health Resources
The stigma associated with mental health conditions may cause patients to be reluctant to seek support for COVID-19–related mental health issues. It is important that healthcare professionals are empathetic with their patients and can provide them with reassurance and resources to cope with anxiety and depression. Psychotherapy including relaxation techniques, breathing exercises, and mindfulness exercises can be beneficial. Healthcare professionals should encourage patients to avoid using negative coping strategies like tobacco, alcohol, or other substances not prescribed. Some organizations have created apps and educational materials to help support self-care and mental health for patients.15-17 Patients, family, and caregivers should be provided with education regarding mental health resources in their community. TABLE 3 lists phone numbers that are available to patients or family in need of immediate assistance once patients are discharged. Pharmacists can seek resources for patients within communities for mental health treatment.

Pharmacist’s Role
Pharmacists have an important role in caring for patients with depression and COVID-19 to help prevent complications of withdrawal, monitor side effects, and ensure continuity of depression treatment. After studies have shown benefit in mortality and time to clinical improvement with remdesivir in hospitalized patients with severe COVID-19, this agent is now recommended in the Infectious Diseases Society of America COVID-19 treatment guidelines.18,19 Severe COVID-19 is defined as patients with SpO2 £94% on room air or patients who require supplemental oxygen, mechanical ventilation, or extracorporeal mechanical oxygenation.20 Dexamethasone is also commonly used in the inpatient setting for COVID-19 patients who require respiratory support, after findings from the RECOVERY trial.21 When treating depression in hospitalized COVID-19 patients, it is important to consider how the recommended COVID-19 treatment agents interact with depression treatments. Pharmacists can assess drug interactions based on the patient’s individualized treatment regimens and assist with additional monitoring when indicated. There are no significant drug interactions with SSRIs and SNRIs and the two aforementioned inpatient COVID-19 treatments, yet a complete medication reconciliation should be completed to determine interactions with other medications. Another consideration is to hold all medications for depression during acute illness.
Other pharmacokinetic and pharmacodynamic considerations include seizure threshold lowering with concomitant dexamethasone and bupropion use in addition to CYP enzyme induction by dexamethasone, lowering the concentration of vortioxetine. Steroid use can lead to neuropsychiatric effects based on dose and duration of therapy. Possible psychiatric side effects include depression, mania, delirium, psychosis, confusion, and cognitive changes.22 It is important for pharmacists to monitor for these changes during dexamethasone treatment.
Pharmacists have the opportunity to help find resources in their communities for mental health treatment and provide additional resources.
Conclusion
COVID-19 has impacted everyone’s mental health in some way. Ongoing research will be needed to understand the impact the pandemic has and will have on mental health. As healthcare workers, we should be empathetic to those patients with COVID-19 and provide patients with appropriate resources. Healthcare workers have been impacted by caring for patients with COVID-19, including long working hours and concern about potential transmission to their family members. Maintaining a routine, physical exercise, a balanced diet, and relaxation techniques are some ways to promote self-care during this time. This pandemic has already changed how healthcare services are provided and will hopefully bring light to the expanded resources needed for the population’s mental health.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
REFERENCES
1. Dong E, Du H, Gardner L. An interactive web-based dashboard to track COVID-19 in real time. Lancet Infect Dis. 2020;20(5):533-534.
2. Marroquin B, Vine V, Morgan R. Mental health during the COVID-19 pandemic: effects of stay-at-home policies, social distancing behavior, and social resources. Psychiatry Res. 2020;293:113419.
3. Xiong J, Lipsitz O, Nasri F, et al. Impact of COVID-19 pandemic on mental health in the general population: a systematic review. J Affect Disord. 2020;277:55-64.
4. Dai LL, Wang X, Jiang TC, et al. Anxiety and depr
essive symptoms among COVID-19 patients in Jianghan Fangcang Shelter Hospital in Wuhan, China. PLoS One. 2020;15(8):e0238416.5. Wang C, Pan R, Wan X, et al. Immediate psychological responses and associated factors during the initial stage of the 2019 coronavirus disease (COVID-19) epidemic among the general population in China. Int J Environ Res Public Health. 2020;17(5):11729.
6. Gelenberg AJ, Freeman MP, Markowitz JC, et al. Practice Guideline for the Treatment of Patients With Major Depressive Disorder. 3rd ed. Washington, DC: American Psychiatric Association; 2010.
7. Management of Major Depressive Disorder Working Group. VA/DoD clinical practice guideline for the management of major depressive disorder. Published April 2016. www.healthquality.va.gov/guidelines/MH/mdd/VADoDMDDCPGFINAL82916.pdf. Accessed February 23, 2021.
8. Khawam E, Khouli H, Pozuelo L. Treating acute anxiety in patients with COVID-19. Clev Clin J Med. May 2020.
9. Devlin JW, Skrobik Y, Gelinas C, et al. Clinical practice guidelines for the prevention and management of pain, agitation/sedation, delirium, immobility, and sleep disruption in adult patients in the ICU. Crit Care Med. 2018;46(9):e825-e873.
10. Berlin RK, Butler PM, Perloff MD. Gabapentin therapy in psychiatric disorders: a systematic review. Prim Care Companion CNS Disord. 2015;17(5).
11. Ostuzzi G, Papola D, Gastaldon C, et al. Safety of psychotropic medications in people with COVID-19: evidence review and practical recommendations. BMC Med. 2020;18:215.
12. Mayo Clinic Laboratories. Pharmacogenomic Association Tables. www.mayocliniclabs.com/it-mmfiles/Pharmacogenomic_Associations_Tables.pdf. Accessed February 15, 2021.
13. Warren JC, Smalley KB. Using telehealth to meet mental health needs during the COVID-19 crisis. The Commonwealth Fund. June 18, 2020. https://doi.org/10.26099/qb81-6c84. Accessed April 19, 2021.
14. American Psychological Association. What are telehealth and telepsychology? Published 2014. www.apa.org/pi/disability/resources/publications/telepsychology. Accessed March 3, 2021.
15. Mental Health America. Mental health and COVID-19 information and resources. https://mhanational.org/covid19. Accessed March 5, 2021.
16. American Psychiatric Association. APA coronavirus resources. www.psychiatry.org/psychiatrists/covid-19-coronavirus. Accessed March 5, 2021.
17. CDC. Mental health and coping during COVID-19. Updated January 22, 2021. www.cdc.gov/coronavirus/2019-ncov/daily-life-coping/managing-stress-anxiety.html. Accessed March 5, 2021.
18. Beigel JH, Tomashek KM, Dodd LE, et al. Remdesivir for the treatment of Covid-19—final report. N Engl J Med. 2020;383(19):1813-1826.
19. Goldman JD, Lye D, David HS, et al. Remdesivir for 5 or 10 days in patients with severe Covid-19. N Engl J Med. 2020;383:1827-1837.
20. Bhimraj A, Morgan RL, Shumaker AH, et al. IDSA Guidelines on the treatment and management of patients with COVID-19. Infectious Diseases Society of America. 2021; Version 4.1.0. www.idsociety.org/practice-guideline/covid-19-guideline-treatment-and-management/. Accessed February 26, 2021.
21. Horby P, Lim W, Emberson J, et al. Dexamethasone in hospitalized patients with Covid-19—preliminary report. N Engl J Med. 2021;384:693-704./
22. Brown ES, Chandler P.A Mood and cognitive changes during systemic corticosteroid therapy. Prim Care Companion J Clin Psychiatry. 2001;3(1):17-21.
To comment on this article, contact rdavidson@uspharmacist.com.






