US Pharm. 2017;42(8)HS-17–HS-28.
ABSTRACT: Despite a rise in opioid misuse, abuse, and diversion, as well as overdose deaths, many patients still suffer from inadequate acute and chronic pain control. Patients may see multiple providers and be prescribed various analgesics including opioids and nonopioids, which may complicate their medication regimen and increase the risk of medication errors during transitions of care. Pharmacists play an important role in pain management as patients transition from one care setting to another by providing such services as medication reconciliation, inpatient services, drug monitoring and assessment, patient and healthcare provider education, discharge counseling, and postdischarge follow-up and planning.
Pain, both acute and chronic, is a significant public-health problem that affects more than 100 million adults in the United States and costs the healthcare system roughly $560 to $635 billion annually.1 Inadequate pain control can result in longer hospital stays, increased rates of readmission, increased outpatient visits, and decreased ability to fully return to normal function, leading to lost income and insurance coverage.2 Pain also places an emotional and financial burden on patients and their families.
Every patient has a unique subjective pain experience that is highly individualized and requires patient-centered care. Pain management has been a core measure in the Hospital Consumer Assessment of Healthcare Providers and Systems survey scores; it has therefore become a priority for inpatient healthcare providers to safely and adequately manage patients’ pain. It is important for providers to effectively relieve acute pain in order to prevent the progression toward chronic pain without overprescribing or dispensing more analgesics than are necessary to control the pain.
In recent years, many organizations, such as the Society of Hospital Medicine, The Joint Commission (JC), and the CDC, have been involved in various initiatives to improve pain management.3-5 Furthermore, pain-management training continues to play a pivotal role in the professional development of healthcare providers. Patients may require complex pain regimens, which makes them vulnerable to medication errors as they transition from one care setting to another. Institutions should have coordinated care plans to optimize pain control as well as patient outcomes, and for seamless care, healthcare providers should empower patients and/or their caregivers to be knowledgeable about and involved in decision-making.
The Continuum of Care
The American Geriatrics Society defines transitional care as a “set of actions designed to ensure the coordination and continuity of healthcare as patients transfer between different locations or different levels of care within the same location.”6 The National Transitions of Care Coalition defines transitions of care as the movement of patients from one care setting (e.g., hospital, nursing home, assisted living facility, primary care physician, home health) to another that frequently involves multiple persons (e.g., patient, caregiver, nurses, social workers, case managers, pharmacists, physicians).7 The interaction of providers across various healthcare settings is often fragmented, resulting in a lack of connectivity between providers in the health system, which compromises patient safety and quality of care.
Pharmacist’s Role
A comprehensive approach to care coordination that emphasizes medication reconciliation at multiple points of care (e.g., admission, unit transfer, discharge) is essential for optimizing patient outcomes. Pharmacists, who are trained as the medication experts on the healthcare team, can lead and champion this process.
Patients who have complex conditions and/or medication regimens that require services from multiple practitioners in different settings are at an increased risk for medication errors, drug-related adverse events, and poor clinical outcomes.5 Tam and colleagues conducted a systematic review of studies and found that up to 67% of patients had errors in prescription-medication history at hospital admission.8 One Canadian study conducted by Forster and colleagues found that 23% of patients discharged from an internal-medicine service experienced at least one adverse event; 72% of those were adverse drug events.9 The detection, management, and reporting of adverse drug events are among the many responsibilities of the pharmacist and play an important role in decreasing readmissions.
Pharmacists should also be cognizant of postsurgical patients who are discharged with poorly controlled pain, as they utilize more healthcare resources and are at greater risk for hospital readmission.10 Psychological stress stemming from poorly controlled pain results in changes to cytokine levels that lead to elevated cortisol levels and depressed immune function, which can negatively impact the healing process.11 Furthermore, when pain is ineffectively managed, patients are at greater risk for developing chronic pain and/or pain-related functional decline.12
It is important to differentiate between acute and chronic pain because management recommendations may vary. Acute pain typically lasts hours to weeks, depending on the precipitating pathology (e.g., surgery, injury, labor, etc.); it has a predictable prognosis and is treated primarily with analgesics. Acute pain decreases quickly as the pain-producing stimulus is removed and/or the healing process occurs. Conversely, chronic pain may not have an identifiable etiology, lasts months to years, has an unpredictable prognosis, and is best treated with a multimodal approach (e.g., analgesics [opioid and nonopioid], therapeutic exercise, cognitive behavioral therapy, etc.).5
The Alliance for Home Health Quality and Innovation has identified five core values that serve as a foundation for best practices in transitional care across all settings.13 These elements include a patient-centered focus, medication management, communication and care coordination, timely follow-up by healthcare providers, and patient-activated education and coaching.13 Pharmacists, as the medication experts, can play an integral role in the implementation of these core values by providing a bundle of services such as medication reconciliation, inpatient services, drug monitoring and assessment, patient and healthcare provider education, discharge counseling, and postdischarge follow-up and planning.14,15
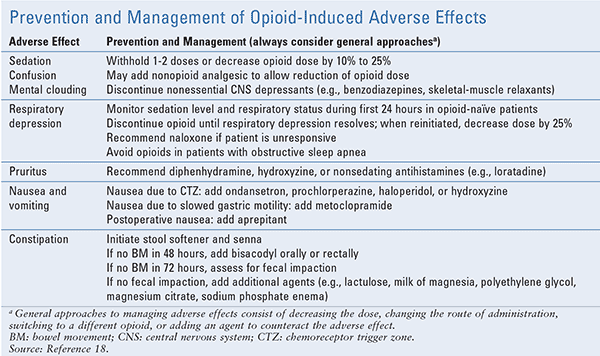
Inpatient Services: Clinical pharmacists should collaborate with the interdisciplinary team on daily rounds and provide comprehensive, evidence-based, patient-centered care by identifying medication-related problems, making medication-therapy recommendations, answering drug-information questions, and identifying patients who require medication reconciliation or patient education.16 A multimodal approach that includes pharmacologic (i.e., opioid and nonopioid) and nonpharmacologic (i.e., physical, psychological, psychosocial) therapies should be implemented to help patients manage their pain. Utilizing a rational polypharmacy strategy of combining opioids and nonopioid adjuvant analgesics such as acetaminophen and nonsteroidal anti-inflammatory drugs allows pain to be targeted at different points along the pain pathway, thereby providing greater pain relief, reducing dosages of opioids, and decreasing opioid-related adverse effects. The binding of opioids to mu receptors can result in adverse effects including confusion, mental clouding, sedation, respiratory depression, nausea and vomiting, pruritus, and constipation.17 TABLE 1 illustrates strategies that clinical pharmacists may recommend to prevent or minimize opioid-induced adverse effects.18
Pharmacists may also elect to refer patients to physical therapy. Physical therapies, which serve to decrease pain and restore physical functioning, may include cryotherapy, thermotherapy, ultrasound, therapeutic exercise, and transcutaneous electrical nerve stimulation.
Psychological treatments are used in both acute and chronic pain to help alleviate anxiety and depression and to improve coping skills. Some examples of psychological interventions include cognitive-behavioral therapy, relaxation, biofeedback, mindfulness, imagery, and distraction.19 Persistent pain can impact the social functioning of patients and negatively affect family, community, or work relationships. Psychosocial interventions aimed at restoring social functioning include coping skills training, support groups, and spiritual/religious support.19
Medication Reconciliation: Upon admission, patients or caregivers should be interviewed by a pharmacist (or an appropriately trained pharmacy technician, resident, or intern) to capture an accurate medication history, which should be documented in the patient’s electronic medical record.20 Medications ordered by the acute-care provider should be compared to the patient’s outpatient medications; and those that have been continued, changed, held, discontinued, or newly initiated should be noted, and any discrepancies should be resolved.14,21 The process of medication reconciliation should be repeated when patients are transferred between different settings and at discharge to assess clinical appropriateness, dosing, and accessibility of medications.
Monitoring and Assessment: Pharmacists should review pertinent laboratory results (e.g., comprehensive metabolic panel, CBC), medication regimens, and imaging and provide clinical recommendations to the appropriate providers when needed. The JC requires hospital healthcare providers to conduct comprehensive pain assessments at admission and reassessments during hospitalization and following discharge to guide treatment decisions. Based on these evaluations, institutions should have protocols in place to manage the patient’s pain or refer to a specialist when appropriate.
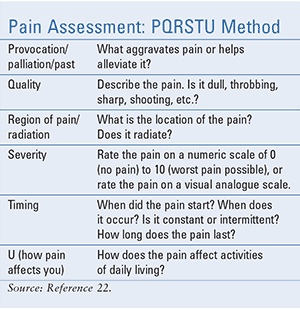
Table 2 illustrates the PQRSTU (provocation/ palliation/past, quality, region of pain/radiation, severity, timing, U [how pain affects you]) acronym, which is a systematic method used to assess and record a patient’s pain history.22 The PQRSTU mnemonic is a useful tool for pharmacists to employ to help guide clinical recommendations to healthcare providers. Treatment strategies may include pharmacologic (opioid and nonopioid analgesics) and nonpharmacologic approaches and should reflect a patient-centered approach that considers the patient’s current presentation, the healthcare provider’s clinical judgment, and the risks and benefits associated with these strategies to mitigate the potential risk of dependency, addiction, and abuse.
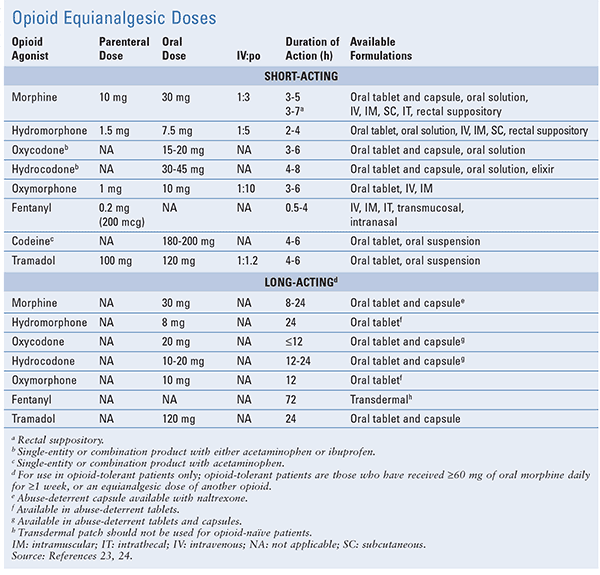
Treatment plans involving opioids should be individualized and based on patient-specific factors, which may include pain intensity, adverse effects (e.g., respiratory depression), prior therapies and responses to therapies, and comorbidities (e.g., renal insufficiency, diabetes). Caution should be exercised when administering opioids to patients with impaired ventilation, bronchial asthma, increased intracranial pressure, sleep apnea, or liver failure. Prior to discharge, it is also important to consider the IV-to-oral conversions for opioids. Table 3 lists common opioids currently available in the U.S. and their equianalgesic dosing and important considerations.23,24
The CDC recommends short-acting opioids for breakthrough pain and, when possible, using the same class of opioid analgesics for long-acting pain relief.5 The CDC also recommends that the majority of patients receive no more than 3 days of opioid therapy for acute pain (rarely exceed 7 days) and be educated on the known risks as well as the realistic benefits of nonpharmacologic and pharmacologic therapies.5 Healthcare providers should emphasize and communicate practical pain-management goals to the patient. Desired outcomes for pain management include facilitating recovery from the underlying illness, injury, or disease, decreasing pain perception, achieving a level of pain relief that improves functionality, improving quality of life, and reducing the use of analgesics. In addition, patients should be informed that usually all pain cannot be eliminated.5
Patient Education: The definition of health literacy, developed for the National Library of Medicine, is an individual’s “ability to obtain, process, and understand basic health information and services needed to make appropriate health decisions.”25 Because approximately one-third of Americans have low literacy skills, educational documents provided to patients should be written in plain language at the 4th to 6th-grade level that avoids the use of medical jargon.26 Visual and graphic aids relating to text are useful tools that can help patients understand the intended message.27 Patients who receive an explanation of administered medications often report greater levels of patient satisfaction.28
For patients initiated on high-risk medications (e.g., opioids), the goal should be to provide inpatient education within 24 hours of initiation.10 As-needed pain medications should be assessed and a plan of care for pain management following discharge should be implemented to minimize the risk of hospital readmission.27 In addition, patients discharged on opioid medications should be educated on possible adverse effects, particularly constipation. Preemptive action should be taken to initiate an appropriate bowel regimen designed to produce a bowel movement at least every 3 days to prevent the risk of bowel obstruction.
A Quality Discharge
Discharge Counseling/Discharge Checklist: Patients are able to comprehend and recall about half of the information provided during counseling sessions.29 Therefore, education should focus on key points related to a patient’s medication regimen, such as changes or additions to a regimen, management of common or serious adverse effects, and follow-up monitoring.27 An effective way to confirm patient understanding is the “teach-back” method.30 In this approach, the healthcare provider clearly explains healthcare information in plain language and then asks the patient to repeat back his or her understanding of what he or she needs to know or do. This process should be repeated until the patient is able to correctly describe the information in his or her own words.
An interdisciplinary team approach should be utilized to help patients successfully transition from the acute to the ambulatory care setting. Table 4 is an example of a checklist that could be used as a framework for all patients discharged on opioid therapy.3 Using the discharge checklist can help ensure coordination of care across various settings to identify and resolve any logistical, psychological, or socioeconomic barriers to obtaining and adhering to prescribed pain-management therapies.

Postdischarge Follow-Up and Planning: Potential barriers that may prevent a patient from obtaining and adhering to medication regimens following discharge include high medication costs or copays, lack of insurance coverage, and inadequate transportation to a community pharmacy. In anticipation of discharge, pharmacists should be aware of the patient’s insurance policy regarding opioid drugs and access to specialists.14 Ideally, a pharmacist should conduct a follow-up telephone call within 48 to 72 hours after discharge to identify medication-related problems, help resolve medication discrepancies, and address patient concerns.14 Reported issues outside the pharmacist’s scope should be triaged to the appropriate provider (e.g., physician, case manager, social worker).14
Conclusion
The transition of care is a time when a patient is vulnerable to medication errors. As medication experts on the healthcare team, pharmacists play an integral role in ensuring the appropriate and safe use of medications. They also collaborate with other professionals between the inpatient and outpatient settings to help patients optimize their medication regimens and improve their care. Through their service as patient-care advocates, pharmacists play an important role in facilitating seamless care to promote better pain management and overall health outcomes.
REFERENCES
1. Institute of Medicine Report from the Committee on Advancing Pain Research, Care, and Education. Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research. Washington, DC: National Academies Press; 2011. www.nap.edu/read/13172/chapter/2. Accessed December 1, 2016.
2. American Academy of Pain Medicine. AAPM facts and figures on pain. www.painmed.org/patientcenter/facts_on_pain.aspx#refer. Accessed December 3, 2016.
3. Society of Hospital Medicine. Transitions of care. Improving pain management for hospitalized patients. Improving transitions of care for patients with pain. 2016. www.hospitalmedicine.org/Web/Quality___Innovation/Implementation_Toolkit/Pain_Management_/transition_care.aspx. Accessed December 3, 2016.
4. The Joint Commission. Joint Commission statement on pain management. April 18, 2016. www.jointcommission.org/joint_commission_statement_on_pain_management/. Accessed December 3, 2016.
5. Dowell D, Haegerich TM, Chou R. CDC guideline for prescribing opioids for chronic pain—United States, 2016. MMWR Recomm Rep. 2016;65(RR-1):1-49. www.cdc.gov/mmwr/volumes/65/rr/rr6501e1.htm. Accessed December 3, 2016.
6. Coleman EA, Boult C. American Geriatrics Society Health Care Systems Committee. Improving the quality of transitional care for persons with complex care needs. J Am Geriatr Soc. 2003;51(4):556-557.
7. National Transitions of Care Coalition. Transitions of care measures. www.ntocc.org/Home.aspx. Accessed December 15, 2016.
8. Tam VC, Knowles SR, Cornish PL, et al. Frequency, type and clinical importance of medication history errors at admission to hospital: a systematic review. CMAJ. 2005;173:510-515.
9. Forster AJ, Clark HD, Menard A. Adverse events among medical patients after discharge from hospital. CMAJ. 2004;170:345-349.
10. Wu CL, Raja SN. Treatment of acute postoperative pain. Lancet. 2011;377(9784):2215-2225.
11. Dent C, Willis M, Jacobson C, et al. Improving the heart of patient transitions. Nursing. 2016;46(3):16-20.
12. Simmons SF, Schnelle JF, Saraf AA, et al. Pain and satisfaction with pain management among older patients during the transition from acute to skilled nursing care. Gerontologist. 2016;56(6):1138-1145.
13. Alliance for Home Health Quality and Innovation. Improving Care Transitions Between Hospital and Home Health: A Home Health Model of Care Transitions. January 2014. http://ahhqi.org/images/uploads/AHHQI_Care_Transitions_Tools_Kit_r011314.pdf. Accessed December 16, 2016.
14. Gilmore V, Efird L, Fu D, et al. Implementation of transitions-of-care services through acute care and outpatient pharmacy collaboration. Am J Health Syst Pharm. 2015;72(9):737-744.
15. McNeely EB. Treatment considerations and the role of the clinical pharmacist throughout transitions of care for patients with heart failure. J Pharm Pract. 2017; 30(4):441-450.
16. Trang J, Martinez A, Aslam S, Duong MT. Pharmacist advancement of transitions of care to home (PATCH) service. Hosp Pharm. 2015;50(11):994-1002.
17. Kalso E, Edwards JE, Moore RA, McQuay HJ. Opioids in chronic non-cancer pain: systematic review of efficacy and safety. Pain. 2004;112(3):372-380.
18. Swegle JM, Logemann C. Management of common opioid-induced adverse effects. Am Fam Physician. 2006;74(8):1347-1354.
19. Keefe FJ, Porter L, Somers T, et al. Psychosocial interventions for managing pain in older adults: outcomes and clinical implications. Br J Anaesth. 2013;111(1):89-94.
20. Truong JT, Backes AC. The impact of a Continuum of Care Resident Pharmacist on heart failure readmissions and discharge instructions at a community hospital. SAGE Open Med. Mar 30, 2015;3:2050312115577986.
21. Mueller SK, Sponsler KC, Kripalani S, Schnipper JL. Hospital-based medication reconciliation practices: a systematic review. Arch Intern Med. 2012;172(14):1057-1069.
22. Buppractice. Pain history: a systemic approach using PQRSTU acronym. www.buppractice.com/node/5519. Accessed December 15, 2016.
23. Kishner S, Schraga E. Opioid equivalents and conversions. Medscape. April 10, 2016. http://emedicine.medscape.com/article/2138678-overview. Accessed December 1, 2016.
24. McPherson ML. Demystifying Opioid Conversion Calculations: A Guide for Effective Dosing. Bethesda, MD: American Society of Health-System Pharmacists; 2010.
25. Office of Disease Prevention and Health Promotion. National Action Plan to Improve Health Literacy. Washington, DC: U.S. Department of Health and Human Services; 2010. https://health.gov/communication/HLActionPlan/pdf/Health_Literacy_Action_Plan.pdf. Accessed December 16, 2016.
26. Kutner M, Greenberg E, Jin Y, Paulsen C. The Health Literacy of America’s Adults: Results From the 2003 National Assessment of Adult Literacy. Washington, DC: National Center for Education Statistics; September 2006. http://nces.ed.gov/pubs2006/2006483.pdf. Accessed December 16, 2016.
27. Sponsler KC, Neal EB, Kripalani S. Improving medication safety during hospital-based transition of care. Cleve Clin J Med. 2015;82(6):351-360.
28. Reichard JS, Savage S, Eckel SF. Pharmacy-initiated transitions of care services: an opportunity to impact patient satisfaction. Hosp Pharm. 2015;50(10):911-917.
29. Crane JA. Patient comprehension of doctor-patient communication on discharge from the emergency department. J Emerg Med. 1997;15(1):1-7.
30. Brega AG, Barnard J, Mabachi NM, et al. AHRQ Health Literacy Universal Precautions Toolkit. 2nd ed. AHRQ Publication No. 15-0023-EF. Rockville, MD: Agency for Healthcare Research and Quality; January 2015. www.ahrq.gov/sites/default/files/publications/files/healthlittoolkit2_4.pdf. Accessed December 16, 2016.
To comment on this article contact rdavidson@uspharmacist.com.






