ABSTRACT: The prevalence of dermatophytes and topical candidal infections is high worldwide. While unlikely to be the cause of a patient’s hospital visit, the infection should address be addressed by healthcare providers either by initiating treatment or continuing it as outpatient therapy. Improper treatment can lead to disease progression. As the severity of the condition increases, the patient can become more susceptible to other infections. A variety of topical treatments are available, including allylamines, azoles, and polyenes.
US Pharm. 2018;43(6):HS-9-HS-12.
Fungal infections of the epidermis are common worldwide and are estimated to affect 10% to 20% of the world’s population.1 They represent a persistent problem across healthcare settings owing to various fungal pathogens and sites of infection. While generally thought of as an outpatient condition, many patients who present to the hospital have concomitant fungal infections that if left untreated or treated inappropriately, can become severe and complicate the overall management of hospitalized patients.2
Epidemiology
Identification of dermatophyte infections is categorized based upon the anatomical site of infection through Latin terminology such as capitis (head); corporis (body); and pedis (foot). The majority of infectious dermatophytes belong to the genera Epidermophyton, Mirosporum, and Trichophyton.1,3,4 These fungi seed keratinized tissues, infecting the skin, hair, and nails.5 Most infections are confined to the stratum corneum, nails, and follicles of the hair; however, deeper infection is possible, especially when prudent treatment is not sought.1,3 Of the dermatophytes, Trichophyton rubrum has become the prevailing cause of infection in the United States and Europe, although various species predominate from one country to another.4,5 However, there are multiple species of Trichophyton as well as Microsporum that are responsible for tinea infections.4
In addition to dermatophytes, Candida species can also cause superficial infections that can be treated with topical medications. Vulvovaginal candidiasis (VVC) is an infectious condition, predominately of Candida albicans (85%), with Candida glabrata or Candida tropicalis causing the remaining infections.2 Superficial candidal infections can also manifest following tissue damage to superficial layers of the skin; in skin folds near the groin; in intergluteal folds; and between the fingers.2,6 Diabetes, genetics, and circulatory disorders, among others, impact the immune system and place the patient at higher risk for fungal infections.3,5
Clinical Presentation and Pathophysiology
Immune function of the host, site of infection, and the specific fungal species influence the pathogenicity of the infection. Patients with impaired immune systems are susceptible to more severe, systemic fungal infections, as well as secondary bacterial infections.5 Transmission is possible via direct and indirect contact.3 Direct contact is the skin-to-skin transmission of the fungi from one individual or animal to another, whereas indirect contact is common through towels, clothing, and bathroom accessories and in communal bathing areas. Indirect transmission is common because dermatophytes can live for extended periods of time without a host.3
Symptoms are dependent on the specific site of infection and range from scaling of the skin and patchy hair loss to scarring from inflammatory dermatologic conditions.1,3,4,7 Cutaneous infections may develop into papules or become larger and more inflamed, resulting in vesicopustules. Lesions that are larger will display irregular margins and can be surrounded by smaller lesions. Inappropriate treatment of the infection, such as with steroids, can cause an alteration in the presentation of the infection and potentially lead to misdiagnosis.3,8 Deeper dermatophyte infections are uncommon because they do not typically survive at the body’s normal core temperature of 98.6°F, although spread to the internal organs, central nervous system, and bones has been reported.5
Candida infections of the skin typically occur in warm, moist areas of the body but can be difficult to distinguish from a dermatophyte infection, owing to a similar clinical appearance.3 Infections caused by Candida are more likely than dermatophytes to be severe, and are more capable of causing invasive and systemic disease, especially in immunocompromised patients.3 Of the infections caused by the Candida species, VVC can be treated with topical medications. Women presenting with VVC will complain of sudden onset, intense vulval pruritus, external dysuria, and pain. Signs include swelling, fissures, and a thick, white, curdy vaginal discharge.3
Management
The azoles, allylamines, and polyenes represent the most widely used treatments for infection caused by dermatophytes and Candida. The azoles are separated into two distinct classes: the imidazoles (clotrimazole, ketoconazole, miconazole, and others) and triazoles (fluconazole, itraconazole, and others). The triazoles are used as systemic first-line agents for most severe fungal diseases, including candidal infections. The imidazoles exert their antifungal effects through various mechanisms. These include altering the permeability of the cell wall resulting in loss of intracellular elements, or interfering with phospholipid synthesis, resulting in cell wall destruction.9
The allylamines (terbinafine, naftifine) have fungicidal activity against dermatophytes and fungistatic activity against C albicans.10,11 Allylamines exert their effects through inhibiting squalene epoxidase, a key enzyme of sterol biosynthesis, resulting in fungal cell membrane disruption. Butenafine and tolnaftate are structurally similar to the allylamines and exert a similar mechanism of action.12
Nystatin, a polyene antifungal, is used in superficial and VVC treatment. Polyenes exert their effect through targeting the fungal cell membrane via ergosterol binding, causing an increase in cell wall permeability. Nystatin does not have utility in dermatophyte infections.6
Overall, there is a lack of strong data to support one class or specific antifungal agent over another when comparing mycological cure and clinical cure rates.1 Some sources may suggest allylamines as first-line agents because they are thought to have a more rapid onset of action and generally have a shorter duration of therapy.7,13 Shortened treatment durations should improve patient compliance and likelihood of mycological cure; however, drug cost must be considered. Topical agents within the azole and allylamine classes are generally well tolerated. Reported adverse effects from these products occur at a rate of 1% to 2%.1,12 Most adverse effects are considered mild and related to localized irritation around the application site.1,12
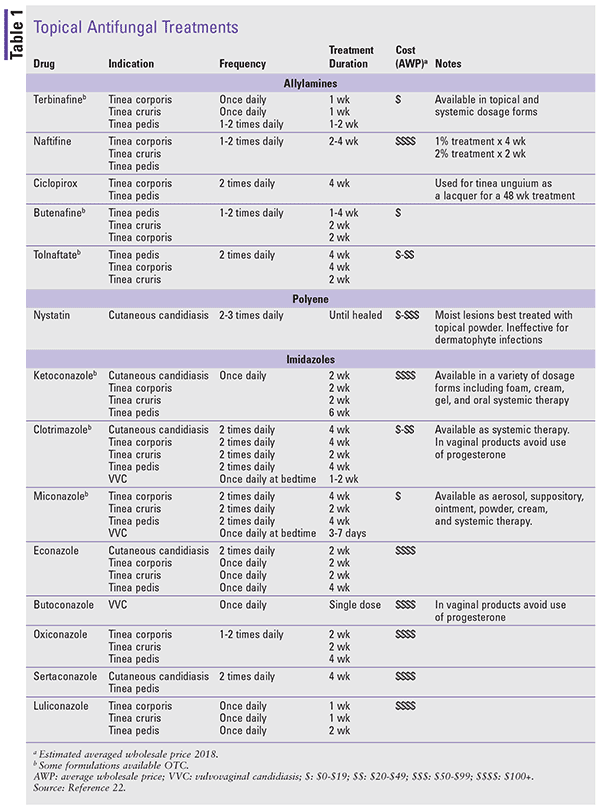
Treatment duration varies between 2 and 6 weeks; however, treatment of each infection should be individualized (Table 1). Owing to lengthy tinea treatment courses, it is imperative that providers and pharmacists be aware that treatment should continue while a patient is hospitalized. Because treatment courses will rarely be completed while a person is an inpatient, recommendations and counseling should be provided to promote compliance and proper continuation of therapy upon discharge and ensure clearing and prevention of recurrent infection.12
Topical corticosteroids are widely used in various forms of skin conditions, with the clinical presentation of dermatophyte infections overlapping with other skin manifestations—including atopic dermatitis, rosacea, seborrheic dermatitis, and lupus erythematosus, among others.8,14,15 While numerous products exist combining potent corticosteroids with antifungals, corticosteroids have been linked to persistent or recurrent infections and their use is discouraged.8,16,17 Using corticosteroids in the setting of a dermatophyte infection may improve resolution of symptoms initially, but these agents are associated with treatment failure, severe or refractory treatment, deep folliculitis, and tinea incognito.8,16,17 The term tinea incognito originated in 1968 when a small collection of patients had unusual symptoms that were attributed to initial treatment with steroids.8 Assessing the location, symptoms, and history of the rash is important prior to beginning treatment with corticosteroids, to prevent complications. When tinea incognito is officially diagnosed, systemic antifungal therapy becomes necessary.8
Topical therapy is not indicated in all tinea infections. Tinea capitis and tinea unguium (onychomycosis) will require initial treatment with oral agents, as topical agents will not penetrate the hair shaft or the nail beds.3,7,13 Systemic therapy with oral agents is also indicated after failed topical treatment or if extensive surfaces are affected.7
New prescription azole topical therapies have been approved in recent years. Most notably, luliconazole (Luzu) has indications for tinea corporis, cruris, and pedis with a 1-week, daily treatment course for tinea corporis and cruris.18 This is a noted advantage over other agents that may require more than three daily applications with 4 weeks of treatment.18,19 The drawback, however, is that these newer options are unlikely to be available for inpatient use as formulary items, owing to high costs.
VVC
Treatment of VVC remains broad. The Infectious Diseases Society of America candidiasis treatment guidelines recommend treatment with topical products for uncomplicated disease. Uncomplicated VVC occurs in 90% of women and is defined as sporadic or infrequent, mild-to moderate, presumed C albicans within a nonimmunocompromised host.2,20 No evidence exists demonstrating superiority of one topical product or duration of therapy over another; this is also true for oral products compared with topical products.2 An alternative to topical therapy is a one-time dose of oral fluconazole 150 mg, which provides patients with convenience compared with topical products. Both routes of administration have high success with similar cure rates of greater than 90%.2
Topical treatment of complicated infections requires 5 to 7 days of topical therapy; recurrent VVC with four or more symptomatic episodes in 1 year can be treated with topical agents with a 10 to 14-day treatment course.2 Topical nystatin achieved mycological cure rates of approximately 75% to 80%; however, the cure rate was lower than that of oral azole agents (>90%).2,21
REFERENCES
1. El-Gohary M, Van Zuuren EJ, Fedorowicz Z, et al. Topical antifungal treatments for tinea cruris and tinea corporis. Cochrane Database of Systematic Reviews. 2014;(8):CD009992.
2. Pappas PG, Kauffman CA, Andes D, et al. Clinical practice guidelines for the management of candidiasis: 2016 update by the Infectious Diseases Society of America. Clin Infect Dis. 2016; 62(4):e1-e50.
3. Richardson MD, Warnock DW. Fungal Infection Diagnosis and Management. 3rd ed. Malden, MA: Blackwell Publishing; 2011.
4. Hayette M, Sacheli R. Dermatophytosis, trends in epidemiology and diagnostic approach. Curr Fungal Infect Rep. 2015;9(3):164-179.
5. Brasch J. Current knowledge of host response in human tinea. Mycoses. 2008;52:304-312.
6. Kalra MG, Higgins KE, Kinney BS. Intertrigo and secondary skin infections. Am Fam Physician. 2014; 89(7):569-573.
7. Ely JW, Rosenfeld S, Stone MS. Diagnosis and management of tinea infections. Am Fam Physician. 2014; 90(10):704-710A.
8. Verma S. Steroid modified tinea. BMJ. 2017; 356:j973.
9. Bondaryk M, Kurztkowski W, Staniszewska M. Antifungal agents commonly used in superficial and mucosal candidiasis treatment: mode of action and resistance development. Postepy Dermatol Allergol. 2013;30(5):293-301.
10. Cannon RD, Lamping E, Holmes AR, et al. Efflux-mediated antifungal drug resistance. Clin Microbiol Rev. 2009;22:291-321.
11. Brennan B, Leyden JJ. Overview of topical therapy for common superficial fungal infections and the role of new topical agents. J Am Acad Dermatol. 1997;36:S3-S5.
12. Katzung BG, Trevor AJ. Basic and Clinical Pharmacology. 13th ed. New York, NY: McGraw-Hill; 2015.
13. Moriarty B, Hay R, Morris-Jones R. The diagnosis and management of tinea. BMJ. 2012; 345(7865):37-42.
14. Arenas R, Moreno-Coutino G, Vera L, Welsh O. Tinea incognito. Clin Dermatol. 2010; 28(10):137-139.
15. Erbagci Z. Topical therapy for dermatophytoses: should corticosteroids be included? Am J Clin Dermatol. 2004;5(6):375-384.
16. Bae BG, Kim HJ, Ryu DJ, et al. Majoochi granuloma caused by Microsporum canis as tinea incognito. Mycoses. 2010;54:361-362.
17. Alston SJ, Cohen BA, Braun M. Persistent and recurrent tinea corporis in children treated with combination antifungal/corticosteroid agents. Pediatrics. 2003;111(1):201-203.
18. Luzu (luliconazole) package insert. Bridgewater, NJ: Valeant Pharmaceuticals; 2013.
19. Gupta AK, Foley KA, Versteeg SG. New antifungal agents and new formulations against dermatophytes. Mycopathologia. 2017;182(1-2):127-141.
20. CDC. Vulvovaginal candidiasis. www.cdc.gov/std/tg2015/candidiasis.htm. Accessed March 20, 2018.
21. Sobel JD. Fungal infections of the genitourinary tract. In: Anaissie EJ, McGinnis MR, Pfaller MA, eds. Clinical Mycology. Philadelphia, PA: Churchill Livingstone Elsevier; 2003:496-508.
22. Lexicomp Online. Hudson OH: Lexicomp Inc. www.lexicomp.com. Accessed March 28, 2018.
To comment on this article, contact rdavidson@uspharmacist.com.