US Pharm. 2013;38(8):34-37.
ABSTRACT: Urinary tract infections are relatively common in women. They may be classified as uncomplicated or complicated depending upon the anatomy and physiology of the urinary tract. Cystitis is an infection of the bladder that can be managed with prescription medications as well as nonprescription strategies. The current guidelines of the Infectious Diseases Society of America recommend several short- and long-term antibiotic regimens to treat uncomplicated cystitis. Preventive strategies to manage patients with recurring cystitis are also available.
Urinary tract infections (UTIs) can be divided into uncomplicated and complicated depending upon the anatomical and pathophysiological elements of the urinary tract.1 An infection in an intact, normally functional tract is classified as an uncomplicated infection.1 If there are any urinary tract abnormalities such as an obstruction, or the patient is predisposed to UTIs, then the infection is classed as complicated.1 Furthermore, the infection may involve only lower tract (bladder and urethra) or both the upper and lower tracts. In some cases, an infection of the upper urinary tract may be classified as a complicated infection.1
Cystitis is specifically an infection of the bladder that can be managed with prescription medications as well as nonprescription strategies.1 Since cystitis is so frequently encountered in the community pharmacy setting, it is useful for pharmacist to have in-depth knowledge of how it can be effectively managed.
Epidemiology
In 2007, 8.6 million physician visits for UTIs were reported, of which 84% were by women.2 Women are more susceptible than men as they have a shorter urethra. About one-fifth of all cases of UTIs end up in the emergency department.3
It has been shown that nearly one-third of all women have had an episode of UTI by the age of 24 years, and half of all women have had at least one uncomplicated UTI in their lifetime by the age of 32 years.2,4,5 Cystitis recurs in 25% of healthy women within 6 months of the first infection and in 20% of women within 1 year.6 The recurrence rate is directly proportional to the number of UTIs the patient has previously had.2
All these figures translate into high economic costs (exceeding over $1 billion annually), decreased workforce productivity, and morbidity.5,7 In older women, symptomatic and asymptomatic bacteriuria presents a risk factor for bacteremia and sepsis, as well as increased mortality.8
Pathophysiology
Cystitis occurs when urinary pathogens from the bowel or vagina colonize the periurethral mucosa and travel to the bladder.2 More than 80% of uncomplicated UTIs are caused by uropathogenic Escherichia coli (UPEC), 5% to 15% by Staphylococcus saprophyticus, and the remaining few cases by Enterococcus and Klebsiella species and Proteus mirabilis.5-7
Risk Factors
Diabetes, a history of recurring UTIs, urinary stones, and urinary catheters as well as any other obstructions are risk factors for developing cystitis. In females, pregnancy, a history of UTIs in a first-degree female relative, sexual intercourse, and the use of spermicides are additional risk factors.2 Males who are homosexual, uncircumcised, or have had sexual contact with an infected woman are at a higher risk of contracting a UTI.7
Signs and Symptoms
An acute uncomplicated UTI is characterized by dysuria and increased frequency and urgency to urinate.6,7,9 The urine may be dark, cloudy, or pink-tinged and foul smelling, and the onset of symptoms is abrupt. Fever, chills, and flank pain are signs of a complicated UTI.6,7,9
Diagnosis
Dipstick testing detects nitrites and leucocyte esterase as a means of screening for UTIs. Nitrites are found in urine as a result of breakdown of nitrates by bacteria and are therefore not present in normal urine. Leucocyte esterase is released from neutrophils that are attracted to the infected area.10 While a dipstick has a high negative predictive value allowing UTIs to be excluded with confidence, it has a relatively low predictive positive value.10 In patients who are at high risk of contracting a UTI, a negative urine dipstick test does not rule out the possibility of an infection.11 Furthermore, this method is unreliable in pregnant women and in children <3 years of age.10
The culture of a urine specimen is the most accurate way of diagnosing a UTI, although it takes longer than a dipstick test.10 Microscopic analysis may also be used to reveal pathogens present in the urine.11
At-home tests such as Azo Test Strips also detect nitrites and leukocytes. They are useful for early detection of UTIs in patients who experience recurrent UTIs.12 Patients should be informed that false negatives may occur in those taking tetracycline or in strict vegetarians who do not consume sufficient nitrates. Additionally, patients who test within 24 hours of consuming >500 mg of vitamin C may get a false negative, as the ascorbic acid interferes with the test. Using the test strips during the menstrual cycle will result in a false-positive result.12
Treatment
Cystitis very rarely develops into a more severe form even when untreated. The main goal of treatment is to ameliorate the symptoms that the patient is experiencing.2
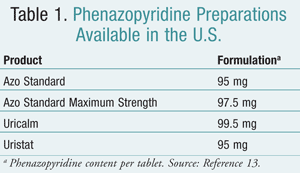
Phenazopyridine hydrochloride is a urinary analgesic that is widely available in many OTC preparations (TABLE 1).13 It is an azo dye that exerts a local anesthetic effect on the mucosa of the urinary tract, providing relief from dysuria and bladder spasms. The recommended dosage is 100 to 200 mg twice daily for 2 days. Patients should be informed that the medication turns urine and tears dark orange, stains contact lenses, and interferes with urinalysis.13
A number of antibiotic regimens, both conventional (7-14 days) and short term (1-3 days) are presently available to treat the bacterial infection.14 Updated guidelines released by the Infectious Diseases Society of America (IDSA) in 2010 can assist health care professionals in the management of women with uncomplicated UTIs.15 The recommended dosages are listed in TABLE 2.2,15

Nitrofurantoin: Nitrofurantoin is listed as an appropriate choice of therapy since it has similar efficacy to trimethoprim-sulfamethoxazole (TMP-SMX), minimal resistance, and minimal collateral damage.15 It has been used for over 50 years and is still one of the most active drugs against E coli.16
The most common adverse effects of nitrofurantoin involve the gastrointestinal (GI) tract and are normally dose related.17 These effects, including nausea, vomiting, anorexia, abdominal pain, flatulence, and diarrhea, tend to be less common when the nitrofurantoin is administered in its macrocrystalline form. Other side effects include headache, drowsiness, vertigo, dizziness, nystagmus, and intracranial hypertension. In rare cases, severe peripheral polyneuropathy may develop, and patients may experience hypersensitivity reactions extending up to an asthma attack. Patients should be advised that nitrofurantoin may cause a false-positive reaction in urine tests for glucose using copper reduction methods, and may discolor urine brown.17
Nitrofurantoin should be avoided in patients with renal failure or pyelonephritis; in patients who are sensitive to nitrofurans; and in those with glucose-6-phosphate dehydrogenase (G6PD) deficiency.2,17 While nitrofurantoin is safe in pregnancy, it can cause hemolytic anemia due to glutathione instability in the immature erythrocytes of the fetus or newborn. For this is reason, it is best avoided near term or during labor.18
Concomitantly administered quinolones antagonize the action of nitrofurantoin, while probenecid and sulfinpyrazone reduce its excretion.17
TMP-SMX: TMP-SMX is considered first-line therapy, as it is effective despite increasing resistance and has fewer ecologic adverse effects than seen with fluoroquinolones.2,15 This means that TMP-SMX has a lower likelihood of inducing resistance to antimicrobials than fluoroquinolones. A randomized, comparative trial showed that a 3-day course of TMP-SMX was more effective and less expensive than a course of nitrofurantoin, cefadroxil, or amoxicillin of the same duration at treating uncomplicated cystitis in women.19
TMP-SMX is inexpensive and relatively well tolerated, with the most common adverse effects being those of the GI tract such as nausea, vomiting, and anorexia, as well as skin reactions including rash, urticaria, and photosensitivity. Rarely, hematologic complications have led to death, particularly in elderly patients.2,17 If a rash appears, treatment should be discontinued immediately due to the risk of severe allergic reactions such as Stevens-Johnson syndrome with SMX.17
Patients should be advised to drink adequate fluids to prevent the risk of crystalluria with SMX.17 For the same reasons, the concomitant administration of any compound that renders the urine acidic should be avoided.17
Caution should be used in patients with renal or hepatic failure, and in severe cases TMP-SMX should be avoided altogether due to the SMX content. Likewise, TMP should be avoided in patients with hematologic disorders and in those with a folate deficiency. While TMP-SMX is widely used in pregnancy, recent studies suggest it might not be safe, particularly in the first trimester.20 Fluoroquinolones or beta-lactams may be indicated as suitable alternatives in patients who cannot tolerate TMP-SMX.2
Fluoroquinolones: The fluoroquinolones ofloxacin, ciprofloxacin, and levofloxacin should only be used as first-line therapy in communities with high rates of TMP-SMX resistance (≥10%) to E coli since these agents have other important indications.2 Fluoroquinolones have been shown to have similar effects to TMP-SMX when given for 3 days to treat uncomplicated UTIs in women.14
This group of drugs has a propensity for adverse effects including nausea, vomiting, diarrhea, headache, drowsiness, insomnia, rash, and pruritus. In rare cases, patients may experience pseudomembranous colitis.17 Other side effects reported include hematologic disorders, renal effects, crystalluria, and cardiovascular effects such as tachycardia. Patients should be advised to maintain an adequate fluid intake to reduce the risk of crystalluria and to avoid strong sunlight or sunlamps.17
Fluoroquinolones should be used with caution in patients with epilepsy or other central nervous system (CNS) disorders, renal or hepatic impairment, or G6PD deficiency.17 They should not be given to children, teenagers, and pregnant or lactating mothers because of the risk of tendon damage.17,21 The absorption of fluoroquinolones is reduced with the concomitant administration of aluminum, magnesium, or iron-containing products.17
Beta-Lactams: Beta-lactams are generally not recommended because of limited efficacy in treating UTIs, as many strains of E coli have become resistant to ampicillin.2,3 However, these agents generally have fewer ecologic adverse effects than are seen with parenteral broad-spectrum cephalosporins.2 The most common adverse effects associated with beta-lactams are hypersensitivity reactions, particularly rashes and urticaria, as well as GI disturbances.
Beta-lactams should not be prescribed to patients with a known allergy to penicillins or cephalosporins. Unlike some other antimicrobials available to treat UTIs, beta-lactams are considered safe to use in pregnancy.8,22,23
Fosfomycin: While fosfomycin has lower resistance and a lower propensity for ecologic damage, it also has inferior efficacy when compared to TMP-SMX or fluoroquinolones.15 Its range of possible adverse effects includes nausea, headache, diarrhea, vaginitis, skin rashes, and visual disturbances. It should be avoided if pyelonephritis is suspected due to the risk of hepatic side effects. Fosfomycin is considered safe in pregnancy, but its use in pregnant women is limited.22 The fosfomycin powder contained in the sachet must not be taken dry. It must be mixed with water before ingesting, and may be taken with or without food.
Other Treatment Considerations: In addition to the efficacy of the regimen, it is important to take into consideration patient allergies, compliance history, local practice patterns, local resistance trends, availability, and cost to the patient.2 As many uropathogenic strains develop resistance to antimicrobials, including TMP-SMX, the effective management of UTIs including cystitis is becoming complicated.3
Short-course therapies have been shown to offer improved compliance, a lower risk of adverse reactions, and lower cost compared to conventional therapies.14 A randomized trial found that short-course ciprofloxacin therapy of 3 to 5 days had an outcome similar to that of conventional ciprofloxacin or norfloxacin therapy of 7 days.14 Within the short-course therapies, the single-dose regimens have shown lower cure rates and a higher rate of recurrence than the 3-day regimens.14 In older women, however, there is some evidence for a 7-day antibiotic regimen, although a Cochrane review showed no additional benefit of increased duration of therapy.24 Men generally require a longer duration of therapy than women because of poor tissue penetration as well as the presence of a larger number of complicating factors.2,25
Recurrent Cystitis
In cases of recurrent cystitis, the long-term goal is to minimize antimicrobial use and improve the patient’s quality of life.2 The following points should be noted when selecting the appropriate antimicrobial therapy for patients with recurrent cystitis.
• If a patient presents with a recurring case of cystitis within a week or two of treatment for uncomplicated cystitis, she should be advised to get a culture at a laboratory to rule out the possibility of a resistant strain.2
• If the condition recurs at least 1 month after the first episode, a longer course of first-line therapy can be prescribed.16 The first-line drug used should be different from the one used for the first episode, particularly if the infection has recurred within 6 months or the drug was TMP-SMX.16
Preventive Strategies
A number of preventive strategies are available to patients, although the use of some is not well established. Various behavioral strategies may also be useful in some cases of recurring cystitis (TABLE 3).2,13

Cranberry juice has been used for many years in the prevention of cystitis, although a Cochrane review found no evidence to support its use for this purpose.26 The recommended dosage is 16 oz of unsweetened juice daily or 500 mg of cranberry extract twice daily.13
Topical estrogen can be used to normalize the vaginal flora, particularly in postmenopausal women; oral estrogens are not effective in this regard.27 Application of 0.5 mg estriol vaginally every night for 2 weeks, followed by twice weekly administration, is recommended.13
Adhesion blockers such as D-mannose may prove useful in preventing the adhesion of bacteria to mannosylated receptors in the urothelium. While there are no clinical trials to evaluate these data, dosages of ¾ to 1 teaspoon 3 times daily are thought to be ideal.2,13
Methenamine hippurate 1 g taken twice daily has been shown to be effective for preventing cystitis, particularly when used for short-term prophylaxis.17,28
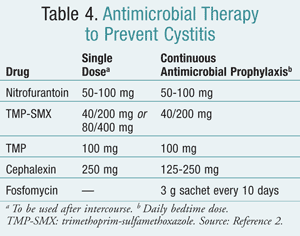
In patients who are able to recognize the initial onset of symptoms of cystitis, first-line antimicrobial regimens may be prescribed for the patient to keep at hand.2 In other cases, a single dose of antimicrobial therapy may be prescribed to use as soon as possible after intercourse. The choice of the agent should be based upon the patient’s susceptibility to and history of any drug allergies.2 Recommended dosages in such cases are listed in TABLE 4.2
Vaccine Development: A vaccine against UPEC is currently under development that may reduce the rates of incidence and recurrence of UTIs.5 Uromone, available in Spain, is a sublingual bacterial vaccine for the prevention of recurrent UTIs.29 No information regarding trials on its use in the United States was found.
Conclusion
Despite the range of antimicrobials available to manage UTIs, their incidence and recurrence rates still remain high. Effective management is further complicated by the fact that the causative uropathogenic organisms continue to develop resistance to antimicrobials. Pharmacists play an important role in counseling patients on the correct use of their prescribed medications and discussing various strategies to prevent recurrence of cystitis.
REFERENCES
1. Mandell GL, Bennett JE, Dolin R. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 7th ed. New York, NY: Churchill Livingstone; 2009.
2. Hooton TM. Clinical practice. Uncomplicated urinary tract infection. N Engl J Med. 2012;366:1028-1037.
3. Brusch JL. Cystitis in females. Medscape Reference. http://emedicine.medscape.com/article/233101-overview. Accessed March 28, 2013.
4. Blondeau JM. Current issues in the management of
urinary tract infections: extended-release ciprofloxacin as a novel
treatment option. Drugs. 2004;64:611-628.
5. Brumbaugh AR, Mobley HL. Preventing urinary tract infection: progress toward an effective Escherichia coli vaccine. Expert Rev Vaccines. 2012;11:663-676.
6. Fihn SD. Clinical practice. Acute uncomplicated urinary tract infection in women. N Engl J Med. 2003;349:259-266.
7. Mehnert-Kay SA. Diagnosis and management of uncomplicated urinary tract infections. Am Fam Physician. 2005;72:451-456.
8. Weissenbacher ER, Reisenberger K. Uncomplicated urinary tract infections in pregnant and non-pregnant women. Curr Opin Obstet Gynecol. 1993;5:513-516.
9. Warren JW, Abrutyn E, Hebel JR, et al. Guidelines for
antimicrobial treatment of uncomplicated acute bacterial cystitis and
acute pyelonephritis in women. Infectious Diseases Society of America
(IDSA). Clin Infect Dis. 1999;29:745-758.
10. Balakrishnan I. Dealing with urinary tract infections. Pharm J. 2011;287:687-690.
11. Panesar K. Urinalysis: a guide for pharmacists. US Pharm. 2009;34(6):52-60. www.uspharmacist.com/continuing_education/ceviewtest/lessonid/106254. Accessed March 28, 2013.
12. Berardi RR. Handbook of Nonprescription Drugs. 17th ed. Washington, DC: American Pharmaceutical Association; 2011.
13. Rakel D. Integrative Medicine. 3rd ed. Philadelphia, PA: Elsevier Saunders; 2012.
14. McCarty JM, Richard G, Huck W, et al. A randomized
trial of short-course ciprofloxacin, ofloxacin, or
trimethoprim/sulfamethoxazole for the treatment of acute urinary tract
infection in women. Ciprofloxacin Urinary Tract Infection Group. Am J Med. 1999;106:292-299.
15. Gupta K, Hooton TM, Naber KG. International clinical
practice guidelines for the treatment of acute uncomplicated cystitis
and pyelonephritis in women: a 2010 update by the Infectious Diseases
Society of America and the European Society for Microbiology and
Infectious Diseases. Clin Infect Dis. 2011;52:e103-e120.
16. Hooton TM. The current management strategies for community-acquired urinary tract infection. Infect Dis Clin North Am. 2003;17:303-332.
17. Sweetman SC, ed. Martindale: The Complete Drug Reference. 34th ed. London, UK: Pharmaceutical Press; 2005.
18. Nicolle LE. Empirical treatment of acute cystitis in women. Int J Antimicrob Agents. 2003;22:1-6.
19. Hooton TM, Winter C, Tiu F, et al. Randomized
comparative trial and cost analysis of 3-day antimicrobial regimens for
treatment of acute cystitis in women. JAMA. 1995;273:41-45.
20. Stamm WE, Hooton TM. Management of urinary tract infections in adults. N Engl J Med. 1993;329:1328-1334.
21. Schaefer C, Amoura-Elefant E, Vial T, et al. Pregnancy
outcome after prenatal quinolone exposure. Evaluation of a case
registry of the European Network of Teratology Information Services
(ENTIS). Eur J Obstet Gynecol Reprod Biol. 1996;69:83-89.
22. Christensen B. Which antibiotics are appropriate for treating bacteriuria in pregnancy? J Antimicrob Chemother. 2000;46(suppl 1):29-34; discussion 63-65.
23. Krcmery S, Hromec J, Demesova D. Treatment of lower urinary tract infection in pregnancy. Int J Antimicrob Agents. 2001;17:279-282.
24. Lutters M, Vogt-Ferrier NB. Antibiotic duration for
treating uncomplicated, symptomatic lower urinary tract infections in
elderly women. Cochrane Database Syst Rev. 2008;(3):CD001535.
25. Naber KG. Treatment options for acute uncomplicated cystitis in adults. J Antimicrob Chemother. 2000;46(suppl 1):23-27; discussion 63-65.
26. Jepson RG, Williams G, Craig JC. Cranberries for preventing urinary tract infections. Cochrane Database Syst Rev. 2012;10:CD001321.
27. Raz R, Stamm WE. A controlled trial of intravaginal
estriol in post-menopausal women with recurrent urinary tract
infections. N Engl J Med. 1993;329:753-756.
28. Lee BS, Simpson JM, Craig JC, et al. Methenamine hippurate for preventing urinary tract infections. Cochrane Database Syst Rev. 2007;(4):CD003265.
29. Lorenzo-Gómez MF, Padilla-Fernández B, García-Criado
FJ, et al. Evaluation of a therapeutic vaccine for the prevention of
recurrent urinary tract infections versus prophylactic treatment with
antibiotics. Int Urogynecol J. 2013;24:127-134.
To comment on this article, contact rdavidson@uspharmacist.com.





