US Pharm. 2016;41(5):23-26.
ABSTRACT: Pediatric patients commonly present with various types of headaches, acutely or chronically. Each patient has individual risk factors and qualifying components that contribute to diagnosis, warranting strategic nonpharmacologic and pharmacologic treatment. Nonpharmacologic techniques can be attempted, with ibuprofen as the most common pharmacologic treatment. Other options may be preferred depending on the individual patient, risk factors, and diagnoses. Pharmacologic options for treatment of chronic headaches are even more vast; complementary and alternative medications have been utilized with relatively unsupported evidence. The management of acute or chronic pediatric headache opens up considerable treatment options for practicing pharmacists.
In the realm of pediatrics, headaches are surprisingly prevalent. Various types of headaches are experienced within the very early years of childhood, with approximately 3% to 8% of children experiencing headaches by the age of 3 years. The incidence ranges from 57% to 82% by the ages of 8 to 15 years
RISK FACTORS
Pediatric patients are at risk for headaches if they have certain risk factors, such as being female. Male and female patients exhibit opposing frequency of headaches as they age. However, males tend to have more headaches as younger children, while females show higher incidence past puberty. Ultimately, females have more headaches than males at a 1.5 to 1 ratio.2
Genetics plays a crucial role and is important to ask about when gathering a patient’s history. According to the American Headache Society (AHS), patients who have immediate family members (i.e., parents or siblings) with migraines are said to have a 1.4- to 1.9-fold increase in risk.1 Additionally, if a pediatric patient struggles with stress, has vision problems, or has issues at school, he or she is at an increased risk of developing headaches.
Regardless of the age or gender of the child, headache has a significant impact on the patient’s quality of life. This article will delve into the variety of treatment options for these patients.
CLASSIFICATION AND DIAGNOSIS OF PEDIATRIC HEADACHE
Classifying and diagnosing headaches have revolved around distinguishing between acute and chronic headaches. Acute headaches can be recurrent or nonrecurrent. Recurrent, acute head-aches are the most common headache classification and contain the indications of migraine, with or without aura, and tension-type headache (TTH). Cluster headaches may occur in pediatrics, but are less common. TABLE 1 shows the 2004 International Headache Society’s classification criteria for pediatric migraine without aura.3,4

Symptomatology of these classically diagnosed headache categories may present differently in pediatric patients compared to adults and tend to be diagnosed retrospectively.1 In some circumstances, a person may come to the emergency department of a hospital seeking immediate care; for example, an alarmed parent whose child is presenting with a first-time migraine or a patient experiencing a migraine refractory to treatment.1 However, management in this setting is not within the scope of this article.
Chronic headaches are diagnosed when the patient experiences 15 or more headaches each month.1 This classification contains chronically occurring headaches that start as acute, like migraine and TTH, as well as the indications of new daily persistent headaches (NDPHs), trigeminal autonomic cephalgias (TACs), and headaches associated with comorbid conditions. Some of these chronic headaches have a duration of less than an hour but can still greatly impact a child’s quality of life.5 The majority of chronic-type headaches diagnosed in pediatric patients directly echo the majority of acute-type headaches—migraine and TTH.
In order to determine what type of headache etiology a child is experiencing, practitioners use the International Classification of Headache Disorders, 3rd Edition (ICHD-3).6 The ICHD-3 is dependent on patterns, including those that correlate with symptomatology. For diagnosis, a complete, very detailed patient history, including family, social, and even school histories, is required in addition to a physical examination.3 Imaging is not routinely done unless etiology cannot otherwise be established or if there are abnormal neurologic examination results.4 If a patient is experiencing chronic headaches, comorbidities such as depression, anxiety, and sleep disturbances need to be evaluated. Symptom presentation may be different in pediatric patients, especially in younger children as compared with adults, so other components of diagnosis—i.e., presentation of cyclical vomiting syndrome or, conversely, no presentation of autonomic symptoms or other typical migraine symptoms—should not be overlooked.2
TREATMENT
As with most other conditions, selecting the appropriate therapy is crucial in designing an individual treatment plan. Treatment for pediatric headache has two main components: nonpharmacologic and pharmacologic. Therapy should always start with the nonpharmacologic component, especially since many children do not require pharmacologic treatment at all.3 If pharmacologic treatment is necessary, the goal is to treat early, appropriately, and effectively. Educating the patient and parents about the potential longevity of treatment for a chronic diagnosis is also crucial to successful treatment. Ultimately, the goal of treatment is to improve quality of life.
Nonpharmacologic Treatment
Nonpharmacologic treatment options may seem simple on the outset, but the implications can vastly improve quality of life. Ensuring healthy lifestyle habits, such as eating breakfast, staying hydrated with water, getting enough sleep, exercise, and full school participation, can decrease frequency and intensity of headaches.2 As with adults, avoiding common triggers including, but not limited to, certain foods, beverages, and tobacco smoke are also good practices.
Journaling about the presentation and duration of the migraine as well as the moments leading up to it helps patients pinpoint potential triggers and also helps parents and patients be better prepared for the next occurrence. Additionally, stress management is a large component of nonpharmacologic treatment. Management through techniques such as biofeedback, acupuncture, hypnosis (especially self-hypnosis), and cognitive behavioral therapy (CBT) has been shown to decrease stress-induced headaches in 50% to 75% of patients.7
Pharmacologic Treatment
Once the requirement for pharmacologic treatment has been established, there are two components to consider: rescue therapy and prophylactic therapy. Rescue therapy is used when pharmacologic treatment is acutely indicated, whereas prophylactic therapy is utilized in patients with more chronic occurrences. Sometimes rescue therapy is determined to be insufficient, and consideration of comorbidities, along with their potential role as a headache source or trigger, comes into play. Comorbidities include conditions such as epilepsy, anxiety, and obesity.2 Prescribers can choose to treat comorbidities appropriately as a means of prophylactic therapy in addition to treating any specific headache type a patient is experiencing. Furthermore, when considering chronic headache types that do not have indicated treatments explicitly addressing the headache’s pathology, treatments for comorbidity could potentially alleviate components of the patient’s symptomatology. Ultimately, the interest of this article is the treatment of headaches specifically. The following two subsections explore the realm of acute and chronic therapy, respectively.
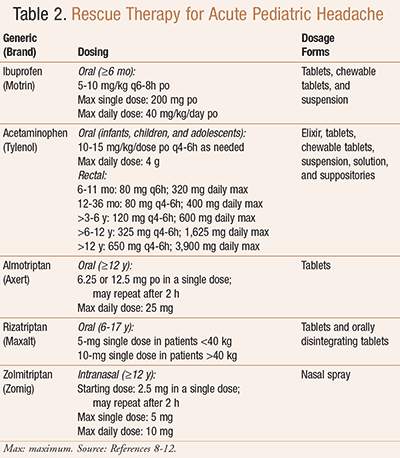
Acute Headaches: When treating acute headaches, rescue therapy is essential. First-line therapy includes the use of nonsteroidal anti-inflammatory drugs (NSAIDs) and acetaminophen.8,9 The NSAID recommended for pediatric patients is ibuprofen; in fact, it is the most studied medication in the treatment of pediatric headache.1,3 In terms of acute migraine treatment, the “triptan” medication class presents FDA-approved options. This class of migraine treatment has been consistently used in pediatric patients for some time. Currently, almotriptan, rizatriptan, and zolmitriptan have obtained approved pediatric indications in the treatment of migraine.10-12 The 2004 American Academy of Neurology guidelines discuss trials devoted to the use of sumatriptan, even referring to its efficacy in acutely treating pediatric patients, but the medication’s package insert does not suggest its use nor offer dosage guidelines.3,13 TABLE 2 lists the medications for acute/rescue treatment along with dosing considerations.8-12 Other therapies for acute treatment include agents to treat nausea/vomiting, gastroparesis, and anxiety. For example, promethazine can help alleviate nausea and vomiting, while amitriptyline or trazodone can cover anxiety and even sleep disturbances that may be present.3
Chronic Headaches: A variety of medication classes have been employed in attempts to treat chronic headaches, yet relying on evidence-based medicine is difficult due to scarce or conflicting data in pediatric use. Depending on the type of headache, the considerations for implementing long-term chronic therapy differ. For instance, chronic or prophylactic migraine treatment is specifically indicated when patients experience migraines that are debilitating to functioning and quality of life three to four times per month.1 The burden of migraine headaches is also assessed by considering the number of school days missed. Chronic treatment is additionally indicated when a Pediatric Migraine Disability Assessment Score (PedMIDAS) is determined and indicates the need for daily prophylaxis.2
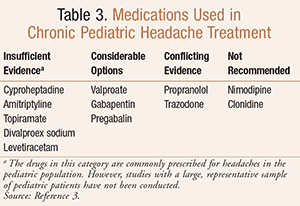
Research has demonstrated that the use of topiramate and valproate sodium in chronic migraine treatment has shown effectiveness in alleviating and shortening the various components of migraines.3 Other medications, including amitriptyline, cyproheptadine, levetiracetam, and zonisamide have some evidence indicating that their use may be effective in pediatric migraine; however, more studies are needed.1,3 Propranolol, a beta-blocker commonly used for migraine prophylaxis in adults, does not have established efficacy in pediatric use and may be worrisome with regard to potential adverse effects.1,3 Additionally, nimodipine, a calcium channel blocker, and clonidine, an alpha-adrenergic agonist, are not recommended in pediatric patients, although they may be used in adults.1,3 The 2004 guidelines set forth by the American Academy of Pediatrics (AAP) and the AHS do not make any official recommendations for the preventive therapy of migraines in children.3 TABLE 3 contains a listing of various medications that have been used to treat chronic pediatric headache.3
In terms of treatment for other types of chronic pediatric headache, treatment for cluster headache uses oxygen, verapamil, and aspirin, among other options.5 Indomethacin, an NSAID, is indicated in the treatment of TAC headaches, such as paroxysmal hemicrania and primary idiopathic stabbing (“ice-pick”) headache, which are very rare in the pediatric population.Complete response of paroxysmal hemicrania, which presents in only 1.3% of pediatric patients, has been observed only when taking indomethacin.5
Complementary and Alternative Medicine (CAM)
Neutraceuticals are another treatment category sought out when treating pediatric migraines. Common CAM products include magnesium, riboflavin (vitamin B2), coenzyme Q10, and fish oil supplements.7 These products may be used individually or in combination, athough there are limited data to support their use.7 However, riboflavin was shown to decrease migraine frequency and duration in 68% of adults.14 Additionally, herbals like feverfew, butterbur, and gingkolide B have been speculated to help with pediatric migraines, although there are conflicting efficacy and safety data.2
When considering the use of herbal supplements, it is vital to encourage patients to purchase products with ingredients that have been tested and subsequently verified by the U.S. Pharmacopeial Convention (i.e., are USP-verified products). Neutraceutical use should be discussed with practitioners before and after starting such therapy. CAM products and herbals can interact with other medications or have negative effects on comorbid disease states. Since these products are commonly sold in pharmacies, pharmacists are presented with a good opportunity for intervening and counseling these consumers.
FUTURE TREATMENT OPTIONS
It can be difficult to point to the future of pediatric headache treatment, especially when the 2004 AAP/AHS guidelines have not been updated to meet the standards of care that have become more established in the past 12 years. A 2012 review completed by the AHS pointed to three rising treatments.2 The first of these is the formulations of triptans that are used in treating the onset of a migraine in children. Specifically, sumatriptan has continually been in the forefront of effective dosage forms. The medication is now available in a needle-free injectable form, and a patch is reported to be in production. More clinical trials are needed in order to prove sumatriptan’s efficacy in children so that this medication, with its various dosage forms, can be utilized.2,13 Additionally, the 2012 review pointed out that diclofenac powder is becoming increasingly useful in the pediatric population. Finally, botulinum toxin type A (Botox) is another potential option for migraine treatment in pediatric patients. Even though there is ample evidence supporting its use in adults, indications in pediatric patients, including adolescents, still require more clinical studies.2
CONCLUSION
The diagnosis of pediatric headache—whether acute, nonrecurrent, or chronic, with or without comorbid conditions—opens up considerable treatment options for practitioners, including pharmacists. However, the importance of nonpharmacologic treatment should never be overlooked or underestimated. The varying headache types have specific treatment recommendations and considerations that should be observed when prescribing for the individual patient. If ibuprofen or acetaminophen is not enough, use of other medications should be evidence-based when possible. The use of neutraceuticals should also be strategically and cautiously considered. The treatment of pediatric headache has not drastically changed over the years, but the need for continued studies and research exists and is rather urgent considering the sizable number of patients impacted by headaches.
REFERENCES
1. Singhi S, Jacobs H, Gladstein J. Pediatric headache: where have we been and where do we need to be? Headache. 2014;54(5):817-829.
2. Jacobs H, Gladstein J. Pediatric headache: a clinical review. Headache. 2012;52(2):333-339.
3. Lewis D, Ashwal S, Hershey A, et al. Practice parameter: pharmacological treatment of migraine headache in children and adolescents: report of the American Academy of Neurology Quality Standards Subcommittee and the Practice Committee of the Child Neurology Society. Neurology. 2004;63(12):2215-2224.
4. Lewis DW. Headaches in children and adolescents. Am Fam Physician. 2002;65(4):625-632.
5. McAbee GN. A review of episodic and chronic pediatric headaches of brief duration. Pediatr Neurol. 2015;52(2):137-142.
6. The International Classification of Headache Disorders, 3rd Edition (beta version). Cephalalgia. 2013;33(9):629-808.
7. Sibinga EM, Kemper KJ. Complementary, holistic, and integrative medicine: meditation practices for pediatric health. Pediatr Rev. 2010;31(12):91-103.
8. Motrin (ibuprofen) package insert. New York, NY: Pfizer; 2007.
9. Tylenol (acetaminophen) package insert. New Brunswick, NJ: Johnson & Johnson Consumer Inc; 2015.
10. Axert (almotriptan) package insert. Titusville, NJ: Janssen; 2009.
11. Maxalt (rizatriptan) package insert. Whitehouse Station, NJ: Merck & Co; 2011.
12. Zomig (zolmitriptan) package insert. Hayward, CA: AstraZeneca; 2015.
13. Imitrex (sumatriptan) package insert. Triangle Park, NC: GlaxoSmithKline; 2013.
14. Schoenen J, Jacquy J, Lenaerts M. Effectiveness of high-dose riboflavin in migraine prophylaxis. A randomized controlled trial. Neurology. 1998;50:466-470.
To comment on this article, contact rdavidson@uspharmacist.com.





