US Pharm. 2009;34(6):HS12-HS18.
Hypertension has been a well-recognized condition in the elderly for a very long time and is prevalent in over 70% of the elderly population.1 It is estimated that the number of persons aged 65 years and older will increase to 72 million by the year 2030, which will in turn result in an increased rate of hypertension among the elderly.2 While studies have shown that the rates of hypertension in the elderly have not changed since 1999, the number of elderly affected continues to grow due to this aging population.3 Hypertension puts the elderly at greater risk for developing several cardiovascular diseases (CVDs), ranging from myocardial infarction, angina, and cerebrovascular disease to peripheral artery disease and cardiac failure. Not only is hypertension considered the most important risk factor for strokes, it is now being linked as a risk factor for dementia as well.4,5
As a person becomes older, the body’s physiology changes. These changes ultimately cause the increasing rates of hypertension and influence the choice of which medications should be utilized for treatment. The physiologic changes affect the pharmacokinetic parameters of commonly used hypertension medications, sometimes leading to different recommendations when it comes to treatment. The elderly population tends to experience more pronounced side effects and consequences from drug interactions as well.6
Physiologic Changes in the Elderly
Heart disease is very prevalent among the elderly, representing the leading cause of death in people over the age of 75 years. There are several mechanisms of the heart that decrease with age that could ultimately lead to heart failure, pulmonary edema, arrhythmias, or exercise intolerance. The pathophysiology behind hypertension in the elderly is a complex process that is not entirely understood, but it is attributed to an increase in peripheral vascular resistance caused by decreased elasticity and increased stiffness due to smooth muscle hypertrophy in arterial walls.7 Both systolic blood pressure (SBP) and diastolic blood pressure (DBP) rise until about 55 years of age, after which the systolic pressure continues to rise almost linearly and the diastolic shows little to no change or declines by the sixth decade of life.8 Changes in collagen or elastin can contribute to an increase in SBP by as much as 6 to 7 mmHg per decade and result in the isolated SBP that affects about two-thirds of patients over the age of 60 years.
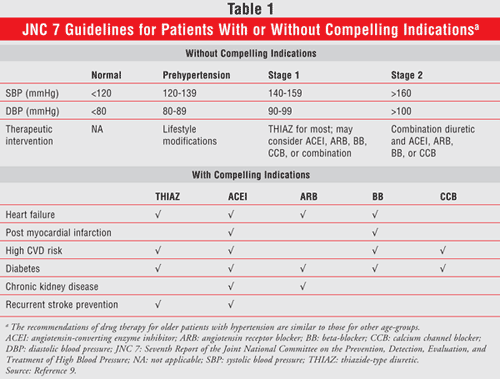
According to the Seventh Report of the Joint National Committee on the Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7), the SBP should be the primary target for diagnosis and treatment of hypertension in the elderly (TABLE 1).9 Between the ages of 20 and 80 years, the left ventricular filling rate during early diastole decreases distinctly by approximately 50%. This phenomenon is compensated for by decreased passive diastolic filling and is commonly seen in elderly patients with congestive heart failure.7 Other physiologic changes that can occur aside from those in the heart ultimately affect all aspects of a drug’s pharmacokinetic properties including absorption, distribution, metabolism, and excretion. A decline in blood flow to the gastrointestinal tract, microvilli atrophy, and a reduction in the acidity of the stomach all contribute to a decline in absorption.10 This may lead to an increase in the bioavailability of medications that undergo a high first-pass effect.11
Nonpharmacologic Treatments
Regardless of the patient’s age or the stage of hypertension, lifestyle modifications are a necessity. Nonpharmacologic treatment may improve hypertension therapy with medications or prevent the need for medications entirely. Losing weight and changing the amount of sodium intake can be very beneficial to the elderly.12 Changing from a high-sodium diet (4,000 mg/day) to a low-sodium diet (2,000 mg/day) over several years can lower blood pressure by as much as 10 mmHg. Reducing body weight by as little as 10% through a sensible exercise program (i.e., moderate physical activity 30 minutes per day at least five times a week) may decrease blood pressure by 5 to 15 mmHg.13
Pharmacologic Treatments
Beta-Blockers: Beta-blockers bind to beta-adrenoceptors, which inhibit normal sympathetic effects that act through the receptors norepinephrine and epinephrine. Nonselective beta-blockers block both beta receptors, whereas cardioselective beta-blockers bind to the beta-adrenoceptor and partially activate the receptor while preventing other receptor agonists from binding. Beta-blockers decrease arterial blood pressure by reducing cardiac output, which has proven to be an effective treatment for hypertension. Beta-blockers also inhibit the release of renin by the kidneys, which leads to a decrease in angiotensin II and aldosterone.14 This enhances renal loss of sodium and water and further diminishes arterial pressure.
A systematic review utilizing data from multiple trials including the Swedish Trial in Old Patients with Hypertension (STOP) and the Systolic Hypertension in the Elderly Program (SHEP) evaluated the response rate of beta-blockers as first-line hypertension therapy in the elderly. Messerli et al found that 39% of the hypertensive patients sustained well-controlled blood pressure during first line beta-blocker monotherapy; however, diuretic therapy was found to be superior to beta-blockade with regard to all end points and was more effective in preventing cerebrovascular events.15 In a meta-analysis that explored randomized controlled clinical trials which utilized beta-blockers as first-line therapy for hypertension, the results were unfavorable to the use of beta-blocker monotherapy first. In contrast to diuretics, which remain the standard first-line therapy, beta-blockers should not be considered appropriate first-line therapy of uncomplicated hypertension in the elderly. Beta-blockers may be considered as adjunctive hypertensive therapy in patients with other indications such as heart failure, prior myocardial infarction, or symptomatic coronary disease in an effort to better prevent cardiovascular disease.16
Alpha-Blockers: Alpha-blockers block the effect of sympathetic nerves on blood vessels by binding to alpha-adrenoceptors located on the vascular smooth muscle. Alpha-blockers dilate both arteries and veins because both vessel types are innervated by sympathetic adrenergic nerves, and lead to a decrease in peripheral vascular resistance.14 The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT) was a randomized, double-blind, multicenter clinical trial sponsored by the National Heart, Lung, and Blood Institute. It was designed to determine whether the occurrence of fatal coronary heart disease (CHD) or nonfatal myocardial infarction is lower for high-risk patients with hypertension who were randomly assigned to receive chlorthalidone, amlodipine, lisinopril, or doxazosin.17 The average age of participants in the trial was 67 years. Total mortality did not differ between the doxazosin and chlorthalidone treatment arms. However, the doxazosin arm versus the chlorthalidone arm had a higher risk of stroke (P = .04) and combined CVD (P <.001).17 Therefore, alpha-blockers should not be used as first-line agents in complicated hypertension in the elderly and should only be considered as alternative and supplementary treatment.
Calcium Channel Blockers: Calcium channel blockers (CCBs) bind to L-type calcium channels on the vascular smooth muscle, cardiac myocytes, and cardiac nodal tissue. These channels are responsible for regulating the calcium entry into muscle cells, which controls smooth muscle contraction and cardiac myocyte contraction. By causing vascular smooth muscle relaxation, CCBs decrease the systemic vascular resistance, which in turn lowers arterial blood pressure. Dihydropyridines, because of their smooth muscle selectivity, are the CCBs mainly used to treat hypertension.18
In a paper published by the ALLHAT Collaborative Research Group, CCB use versus diuretics for the treatment of high-risk individuals was analyzed.19 Over half of the participants in the study were at least 65 years of age or older. There was no difference in combined fatal CHD or nonfatal myocardial infarction between amlodipine and chlorthalidone. Secondary outcomes showed similar results except for a statistically significant higher six-year risk rate of heart failure with amlodipine versus chlorthalidone (P <.001). The study concluded that for patients who cannot take a diuretic, first-step therapy with CCBs should be considered.
ACE Inhibitors: ACE inhibitors work by inhibiting the production of angiotensin II from angiotensin I, which leads to a reduction in aldosterone output and causes a reflex increase in renin secretion.20 ACE inhibitors cause venodilation and also induce natriuresis, which reduces cardiac preload.21 It has been said that agents that inhibit the renin-angiotensin system do more than just reduce blood pressure.22
In the Second Australian National Blood Pressure (ANBP2) trial, 6,083 hypertensive patients above the age of 65 were randomized to receive enalapril or hydrochlorothiazide. The study’s purpose was to achieve a goal blood pressure based on the SHEP goal of <140 mmHg. Overall, the results of the study showed a decrease of 26 mmHg systolic and 12 mmHg diastolic with no difference between the two treatment groups. Further analysis revealed a reduction in cardiovascular events or deaths favoring the ACE inhibitor group compared to the diuretic group. These finding suggest an advantage of the use of ACE inhibitors over diuretic therapy in cardiovascular complications with no effect on blood pressure reduction.23
Angiotensin Receptor Blockers: Angiotensin receptor blockers (ARBs), also known as sartans, act by blocking the activation of angiotensin II type 1 receptors.20 In a open-label, double-blind study completed by Belcher et al, the safety and tolerability of candesartan was tested in 5,464 patients.24 The study concluded that candesartan was equally tolerated by patients both above and below the age of 65. Even though the study did not incorporate a direct comparison between candesartan and other antihypertensive medications, it was noted that candesartan was not associated with as many adverse events as are seen to be common with other antihypertensive drug classes.
The Losartan Intervention For Endpoint Reduction in Hypertension (LIFE) study showed an advantage that ARBs had over other antihypertensive agents.25 This prospective, randomized, double-blind, parallel group study compared a regimen based on losartan to that of a regimen based on atenolol. The results of the study showed that despite similar reductions in blood pressure, new-onset atrial fibrillation occurred in 150 patients randomized to losartan as opposed to the 221 patients randomized to atenolol (P <.001). Because of their more tolerable side-effect profile, the role of ARBs in the treatment of hypertension is beginning to expand.
Diuretics: Diuretics promote diuresis by altering how the kidneys handle sodium.26 Each class of diuretics works at different sites in the kidneys. Diuretics can be divided into five different classes, of which thiazide, loop, and potassium-sparing diuretics are the most commonly used in treating hypertension.21
The overall efficiency of antihypertensive treatments was tested in ALLHAT. The study set out to determine whether treatment with an ACE inhibitor or a CCB as opposed to a diuretic would lower the incidence of CHD or other CVD in hypertensive patients. It was concluded from the study that treatment with a thiazide diuretic was superior in preventing one or more major forms of CVD.17 Of the subjects 65 years old and older who were treated in the trial, those who were randomized to the diuretic group showed a lower incidence of heart failure. The group randomized to the calcium channel blocker had a 38% higher risk of heart failure (P <.001) with a 6-year absolute risk difference of 2.5% and a 35% higher risk of hospitalized fatal heart failure (P <.001). In comparison to those who were treated with an ACE inhibitor, the study showed that those who were treated with a thiazide diuretic had lower incidences of combined CVD outcomes, combined CHD, and heart failure. The group treated with the ACE inhibitor had a 15% higher risk for stroke (P = .02) and a 10% higher risk of combined CVD (P <.001).19
Psaty et al completed a meta-analysis that incorporated ALLHAT along with many other trials to assess major CVD end points.27 The analysis concluded that low-dose diuretics are the most effective first-line treatment for preventing the occurrence of CVD morbidity and mortality. The results of ALLHAT, and the other trials that followed, have been the basis for treatment guidelines incorporating low-dose diuretics as the first-line treatment in elderly patients with hypertension. Combination therapy is recommended with two or more agents to achieve the most favorable results, with diuretics remaining the first-line drug of choice.9
Adverse Effects of Antihypertensive Agents
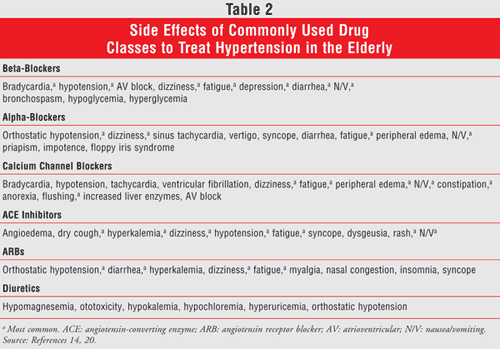
The safety profiles of antihypertensive agents warrant critical evaluation due to the increased risk of falls related to common side effects such as hypotension, dizziness, and syncope. Falls remain a significant threat to the elderly and a major cause of morbidity and mortality.28All classes of medications are likely to contribute to these effects (TABLE 2) but vary depending on the specific medication and the dose administered. Combination medications have the ability to potentiate these effects and should be conservatively prescribed only where the benefit outweighs the risk.
Recommendations for Clinical Practice
As we await the results of the eighth report of the JNC, which is scheduled to become available for review and comment by December 2009, we need to remain focused on the physiologic changes that occur in the elderly population and how medications and disease states can be affected by these changes. With little information available regarding the specific guidelines to treat the aging, pharmacists need to stay current on evidence-based medicine and its role in treating hypertension in an effort to prevent future serious cardiovascular complications. There are several classes of medications available for the treatment of hypertension in the elderly, of which alpha-blockers, beta-blockers, CCBs, diuretics, ACE inhibitors, and ARBs are the most commonly prescribed, as well as combination agents. Caution must be used when individualizing an appropriate course of therapy, and medications should be titrated carefully in the elderly in order to attain desired clinical goals. Thus remember, when beginning drug therapy in the elderly, it is always best to “start low and go slow.”
REFERENCES
1. National Center for Health Statistics. National Health and Nutrition Examination Survey: Hypertension and elevated blood pressure among persons 20 years of age and over by selected characteristics. In: Health, United States, 2008. Hyattsville, MD: Public Health Service; 2008.
2. McDonald M, Hertz RP, Unger AN, Lustik MB. Prevalence, awareness, and management of hypertension, dyslipidemia, and diabetes among United States adults aged 65 and older. J Gerontol A Biol Sci Med Sci. 2009;64:256-263.
3. Cutler JA, Sorlie PD, Wolz M, et al. Trends in hypertension prevalence, awareness, treatment, and control rates in United States adults between 1988-1994 and 1999-2004. Hypertension. 2008;52:818-827.
4. Nilsson P. Reducing the risk of stroke in elderly patients with hypertension: a critical review of the efficacy of antihypertensive drugs. Drugs Aging. 2005;22:517-524.
5. Skoog I. The relationship between blood pressure and dementia: a review. Biomed Pharmacother. 1997;51:367-375.
6. Beyth R, Shorr R. Epidemiology of adverse drug reactions in the elderly by drug class. Drugs Aging.
7. Gaballa MA, Jacob CT, Raya TE, et al. Large artery remodeling during aging: biaxial passive and active stiffness. Hypertension. 1998;32:437-443.
8. Fagard RH. Epidemiology of hypertension in the elderly. Am J Geriatr Cardiol. 2002;11:23-28.
9. Chobanian AV, Bakris GL, Black HR, et al. Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA.
10. Dhanani S, Norman DC. Care of the elderly patient. In: Current Critical Care Diagnosis & Treatment. 2nd ed. New York, NY: Lange Medical Books/McGraw Hill Companies, Inc; 2002:478-487.
11. Knight-Klimas T, Boullata. Nutrient-drug interactions in the elderly. In: Boullata T, Armenti V, eds. Handbook of Drug-Nutrient Interactions. Totowa, NJ: Humana; 2004:371-374.
12. Appel LJ, Espeland MA, Easter L, et al. Effects of reduced sodium intake on hypertension control in older individuals: results from the trial of nonpharmacologic interventions in the elderly (TONE). Arch Intern Med. 2001;161:685-693.
13. Kaplan N. Patient information: high blood pressure, diet, and weight. UpToDate Online. www.utdol.com/online/content/ 1999;14:231-239. 2003;289:2560-2572.
14. Hoffman B. Catecholamines, sympathomimetic drugs, and adrenergic receptor antagonists. In: Hardman J, Limbird L, eds. Goodman & Gilman’s The Pharmacological Basis of Therapeutics. 10th ed. New York, NY: McGraw-Hill; 2001:242-260.
15. Messerli FH, Grossman E, Goldbourt U. Are beta-blockers efficacious as first-line therapy for hypertension in the elderly? A systematic review. JAMA. 1998;279:1903-1907.
16. Khan N, McAlister FA. Re-examining the efficacy of beta-blockers for the treatment of hypertension: a meta-analysis. CMAJ. 2006;174:1737-1742.
17. ALLHAT Collaborative Research Group. Major cardiovascular events in hypertensive patients randomized to doxazosin vs chlorthalidone. JAMA. 2000;283:1967-1975.
18. Kerins D, Robertson R, Robertson D. Drugs used for the treatment of myocardial ischemia. In: Hardman J, Limbird L, eds. Goodman & Gilman’s The Pharmacological Basis of Therapeutics. 10th ed. New York, NY: McGraw-Hill; 2001:853-860.
19. ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group. Major outcomes in high-risk hypertensive patients randomized to angiotensin converting enzyme inhibitor or calcium channel blocker vs diuretic: the Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). JAMA. 2002;288:2981-2997.
20. Clinical Pharmacology [database online]. Tampa, FL: Gold Standard, Inc; 2009. www.clinicalpharmacology.com. Accessed January 15, 2009.
21. Rosenfeld G, Loose D. Pharmacology. 4th ed. Baltimore, MD: Lippincott Williams & Wilkins; 2007:73-76.
22. Baruch L. Hypertension and the elderly: more than just blood pressure control. J Clin Hypertens. 2004:6:249-255.
23. Wing LM, Reid CM, Bellin LJ, et al. Second Australian National Blood Pressure Study (ANBP2). Program of Hypertension Prague 2002–Joint 19th Scientific Meeting of the International Society of Hypertension; June 23-27, 2002; Prague, Czech Republic.
24. Belcher G, Hubner R, George M, et al. Candesartan cilexetil: safety and tolerability in healthy volunteers and patients with hypertension. J Hum Hypertens. 1997;11(suppl 2):S85-S89.
25. Wachtell K, Lehto M, Gerdts E, et al. Angiotensin II receptor blockade reduces new-onset atrial fibrillation and subsequent stroke compared to atenolol: the Losartan Intervention For End Point
Reduction in Hypertension (LIFE) study. J Am Coll Cardiol. 2005;45:712-719.
26. Klabunde RE. Diuretics. Cardiovascular Pharmacology Concepts. www.cvpharmacology.com/
27. Psaty BM, Lumley T, Furberg CD, et al. Health outcomes associated with various antihypertensive therapies used as first-line agents: a network meta-analysis. JAMA. 2003;289:2534-2544.
28. Pedelty L, Gorelick P. Management of hypertension and cerebrovascular disease in the elderly. Am J Med. 2008;121(suppl 8):S23-S31.





