US Pharm. 2011;36(9):8.
According to the CDC, the number of live births reached an all-time high (4.3 million) in 2007, but has since declined to 4.1 million. Despite this decline, the number of births in 2008 was greater than the rate for any year from 1962 through 2005. Although the first-order birthrate varied over the last decade, in 2008 it was 1% lower than in 2007. The first-order birthrate for females aged 15 to 39 years fell by 2%, whereas it rose from 2 to 2.2 per 1,000 women aged 40 to 44 years (the only age group to have an increase). The number of first-order births fell by 8%, 5%, and 2% among Central/South American, Hispanic Mexican, and non-Hispanic white women, respectively. Notable contributors to the decline were fertility rate (4% decline) and low birthrates (9%, 6%, and 2% for women aged 20-24, 25-29, and ≥30 years, respectively), even though the birthrate in unmarried women increased to 40.6%.
Place of Delivery: In 2008, 99% of all births took place in hospitals; 91.3% were attended by physicians in hospitals. Of the 42,746 out-of-hospital births, 66% occurred in a residence and 28% were in a freestanding birthing center. Certified nurse-midwives (CNMs) have been reported to have attended 60% of home births and 8% of all births, and this number has changed little since 1989. CNM-attended hospital births were more frequent among American Indian women (17%) than among Hispanic (8%), non-Hispanic white (7%), non-Hispanic black (6.8%), and Asian–Pacific Island (5.9%) women.
Method of Delivery: According to the National Center for Health Statistics (NCHS), 32% of all deliveries were by cesarean section (1.4 million cesarean; 2.9 million vaginal), and the rate of increase of cesarean delivery has started to slow after a jump of 56% since 1996. First-order births were more likely to be delivered by cesarean section in women aged 40 to 54 years compared with women younger than 20 years (49% vs. 23%).
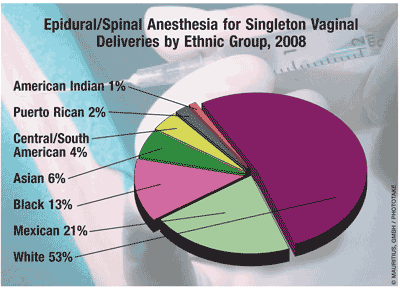
NCHS data show that 61% of women received epidural or spinal anesthesia (ESA) during first-order birth. ESA use has been found to increase with increasing maternal education. Early initiation of prenatal care heightened the likelihood of ESA receipt, as did attendance at the birth by a medical doctor. ESA use was more common in vaginal deliveries assisted by forceps (84%) or vacuum extraction (77%) than in spontaneous vaginal deliveries (60%). ESA use was less likely when infants were born prior to 34 weeks’ gestation or weighed less than 1,500 g. Labor of less than 3 hours was associated with decreased ESA use.
To comment on this article, contact rdavidson@uspharmacist.com.





