US Pharm. 2022;47(1):HS1-HS7.
ABSTRACT: Postural orthostatic tachycardia syndrome (POTS) is a disorder of the autonomic nervous system that is often misunderstood and is typically seen in younger women. Emerging data suggest an association between coronavirus disease 2019 and POTS. Given the rise in POTS cases, it is imperative that clinicians and other healthcare professionals better understand this condition. Although several nonpharmacologic and pharmacologic treatments exist for patients with POTS, none are currently FDA-approved. As therapeutics experts and the most accessible members of the healthcare team, pharmacists play a pivotal role in optimizing treatment outcomes by directing patients to further evaluate symptoms and in proposing therapeutics to other healthcare professionals.
Postural orthostatic tachycardia syndrome (POTS) is a disorder of the autonomic nervous system (ANS) characterized by cardiac and neurologic symptoms that occur upon standing.1-3 Patients with POTS are routinely dismissed with inaccurate diagnoses by physicians who are unfamiliar with this syndrome. In fact, results from a survey conducted in more than 700 patients indicated challenges in obtaining the correct diagnosis, with more than 69% of patients being inappropriately diagnosed with an anxiety disorder rather than POTS.4 Although POTS affects both men and women, the literature suggests that the typical demographic diagnosed with POTS is premenopausal Caucasian women.5 It is imperative that clinicians familiarize themselves with POTS, as the number of cases has been growing since the onset of the coronavirus disease 2019 (COVID-19) pandemic.6 This has led to increased efforts by scientists and clinicians to better understand this syndrome and its connection to COVID-19.
Epidemiology
POTS affects anywhere from 1 million to 3 million people in the United States. Reports suggest that women aged 15 to 50 years are more commonly diagnosed with POTS.7 This condition is characterized by poor blood circulation to the heart when the patient stands up from a supine position. POTS is often misdiagnosed, owing to limited research and training of clinicians about this underappreciated condition. As an illustration, a case report described a 19-year-old female who presented with common POTS symptoms but was repeatedly misdiagnosed with anxiety beginning at age 13 years. The patient reported dizziness upon standing, frequent episodes of blurry vision, muffling sounds in her ears, and episodes of near collapse. The anxiety medications she was prescribed provided no discernible benefit.8 After completing extensive diagnostic tests, the patient was confirmed to have POTS. Although this patient ultimately received the correct diagnosis, many people with POTS are misdiagnosed and continue to receive inappropriate treatment.
It is especially important that clinicians understand the diagnosis and treatment of this syndrome, as it has been triggered by bacterial and viral infections.9 In fact, researchers have identified a potential association between COVID-19 and POTS. Several case reports have been published in which patients who recovered from COVID-19 continued to experience POTS-like symptoms, including fatigue and lightheadedness. For instance, the first case report of COVID-associated POTS involved a patient who presented with palpitations and shortness of breath 7 days after her COVID-19 diagnosis.10 After completing several comprehensive tests, the patient was confirmed to have POTS. More than 246 million COVID-19 cases have been reported globally, and although few case reports on COVID-associated POTS have been published, the number of people affected by post–COVID-19 POTS is expected to grow as more patients worldwide become infected with severe acute respiratory syndrome coronavirus 2.11
Pathophysiologic Mechanisms
The cause of POTS is poorly understood, but episodes often occur after a trauma, surgery, or viral illness, and women may experience symptoms just prior to menses. Additionally, genetic abnormalities may play a role in some patients.7 Usually, patients experience a triggering event—such as COVID-19—weeks to months before the onset of POTS symptoms.12
POTS is characterized by an interruption of normal physiologic response when the patient transitions from a supine to a standing position. A normal physiologic response entails an instantaneous downward shift in blood volume to the magnitude of 500 mL to 800 mL upon standing.13 This causes blood to pool in the legs and abdomen, which reduces blood pressure (BP) secondary to a decreased return of blood to the heart. Baroreceptors (specialized cells sensitive to BP changes) sense this decline and send signals to the brain to initiate a compensatory response involving the sympathetic and parasympathetic nervous systems.13,14 As part of this response, increased sympathetic activity results in vasoconstriction and an increased heart rate (HR), with a consequent increase in stroke volume. Additionally, there is a reduction in parasympathetic outflow that results in a further increase in HR. These combined responses maintain cardiac output (CO) for perfusion of the brain and other organs.13 POTS occurs when an exaggerated compensatory response to the initial decline in BP and CO causes the patient to experience pronounced tachycardia when standing up from a supine position.2,14,15
The exact mechanism of the autonomic dysregulation seen in POTS is unclear, but some mechanisms have been postulated, such as hypovolemia and deconditioning. Deconditioning is a decrease in heart-muscle responsiveness that sometimes takes place after long periods of weightlessness and may be characterized by reduced blood volume and pooling of blood in the legs once normal conditions are restored.16 This can further contribute to hypovolemic symptoms because a higher HR will be necessary to sustain CO.13
Another proposed mechanism is neuroendocrine dysfunction, whereby patients may display increased cardiovascular adrenergic activity separate from tachycardia, suggesting a hyperadrenergic state. These patients tend to have higher levels of catecholamines compared with patients without POTS, and this may be due to functional or acquired deficiency in the norepinephrine transporter (NET).5 Genetic variations have also been identified in some patients with POTS who have a single point mutation, causing loss of function in the NET as well as diminished norepinephrine clearance and sympathetic nerve activation.4 Additionally, women are more likely to be diagnosed with POTS, and the severity of their symptoms can fluctuate throughout the menstrual cycle, leading to changes in BP and vasoconstriction.5 Nonetheless, researchers suspect that POTS may have various causes, some of which may be abnormal regulation of BP; impaired function of nerves, especially in the lower extremities; and changes in heart and blood-vessel function.
Subtypes and Clinical Presentation
Several subtypes of POTS account for the varying mechanisms leading to differences of symptoms seen in affected patients. However, POTS cannot always be explained by a subtype. Many patients experience chronic symptoms that cannot be mechanistically explained by postural intolerance or excessive tachycardia.5 More importantly, characteristics of POTS are not mutually exclusive, and multiple symptoms may be experienced simultaneously.
Neuropathic POTS: This is the most common subtype, affecting more than 50% of patients with the condition.5 In neuropathic POTS, patients experience a loss of sweat function in their distal lower extremities, which suggests that peripheral sympathetic denervation might lead to impaired vasoconstriction and increased pooling of blood in the lower extremities.5,17 To compensate for this, an exaggerated increase in HR and CO would be required to maintain systemic mean arterial pressure.5
Hyperadrenergic POTS: Hyperadrenergic POTS affects 30% to 60% of patients with POTS.5 In hyperadrenergic POTS, patients experience palpitations, abdominal pain, nausea, and hyperhidrosis, and these symptoms are likely to be exaggerated upon physical exertion and emotional stress.15 This is likely due to the elevated standing plasma norepinephrine levels in the hyperadrenergic state, which elicits an exaggerated sympathetic response such as excessive orthostatic tachycardia.5
Secondary POTS: This subtype refers to POTS occurring in the presence of another medical condition known to cause or contribute to dysautonomia, which is a disorder of the ANS.2 Common conditions that are known to cause dysautonomia are diabetes, Lyme disease, lupus, and Sjögren’s syndrome.2
Diagnosis
A diagnosis of POTS involves ruling out health conditions that share similar symptomatology, such as orthostatic hypotension (OH), which is defined as a decline of at least 20 mmHg in systolic BP and/or 10 mmHg in diastolic BP within the first 3 minutes of standing up from a supine position.2,3 In the absence of a clear underlying cause for a patient’s POTS symptoms, several tests may be ordered to aid diagnosis, the most common one being the tilt table test, where a patient is secured on a table while lying flat.2 The table is then raised to a nearly upright position, and the patient’s HR and BP are measured to detect alterations in vitals upon the change in position. A POTS diagnosis is established if the following criteria are met: 1) the patient demonstrates an abnormal HR response to being upright (i.e., HR increase of 30 BPM in adults and adolescents and at least 40 BPM in children); 2) the patient’s symptoms worsen while upright; and 3) OH does not occur within the first 3 minutes of testing.2,3
Nonpharmacologic Treatment
The goals of treatment are to improve blood flow and to address the circulatory problems seen in POTS.2,3 The initial treatment approach should employ nonpharmacologic modalities (TABLE 1).3,18,19
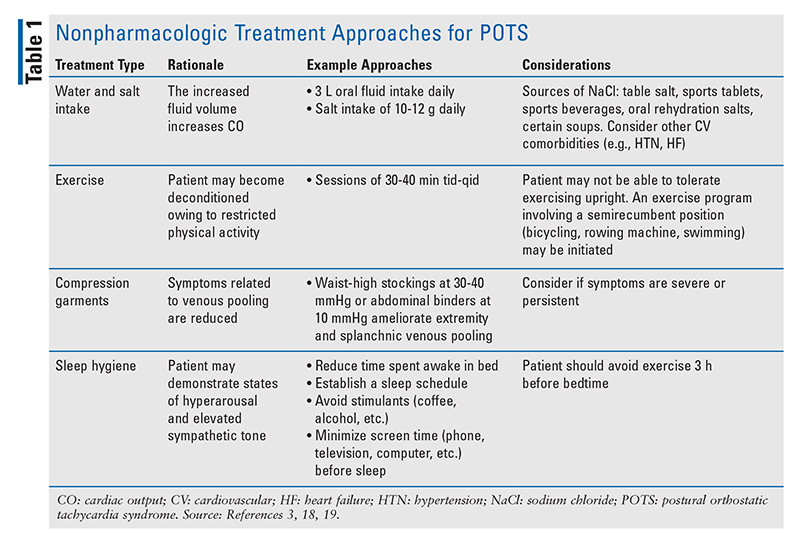
Pharmacologic Treatment
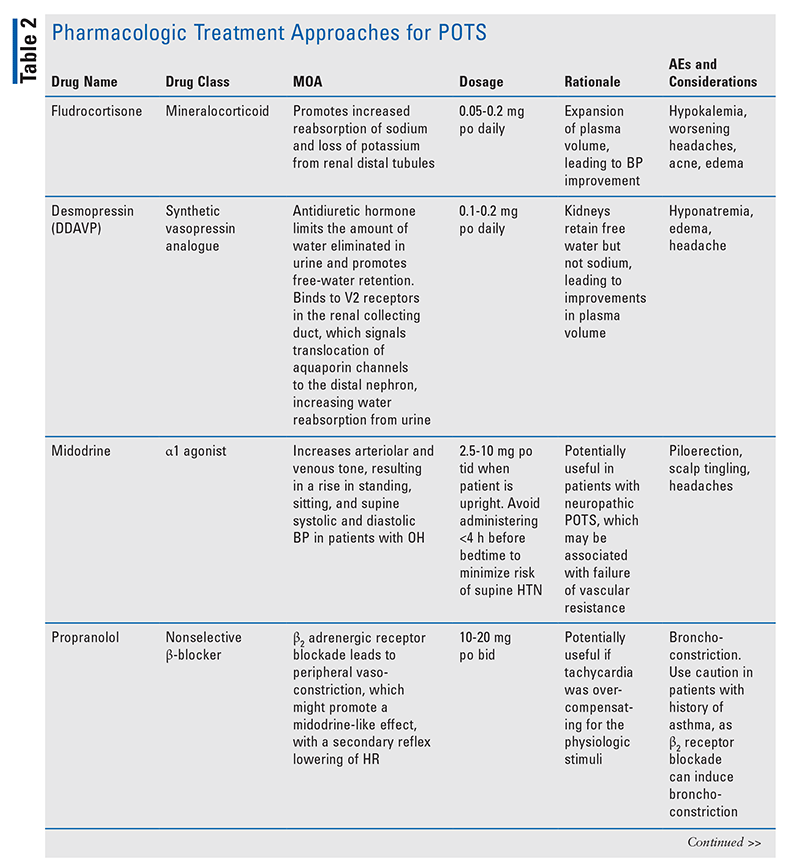
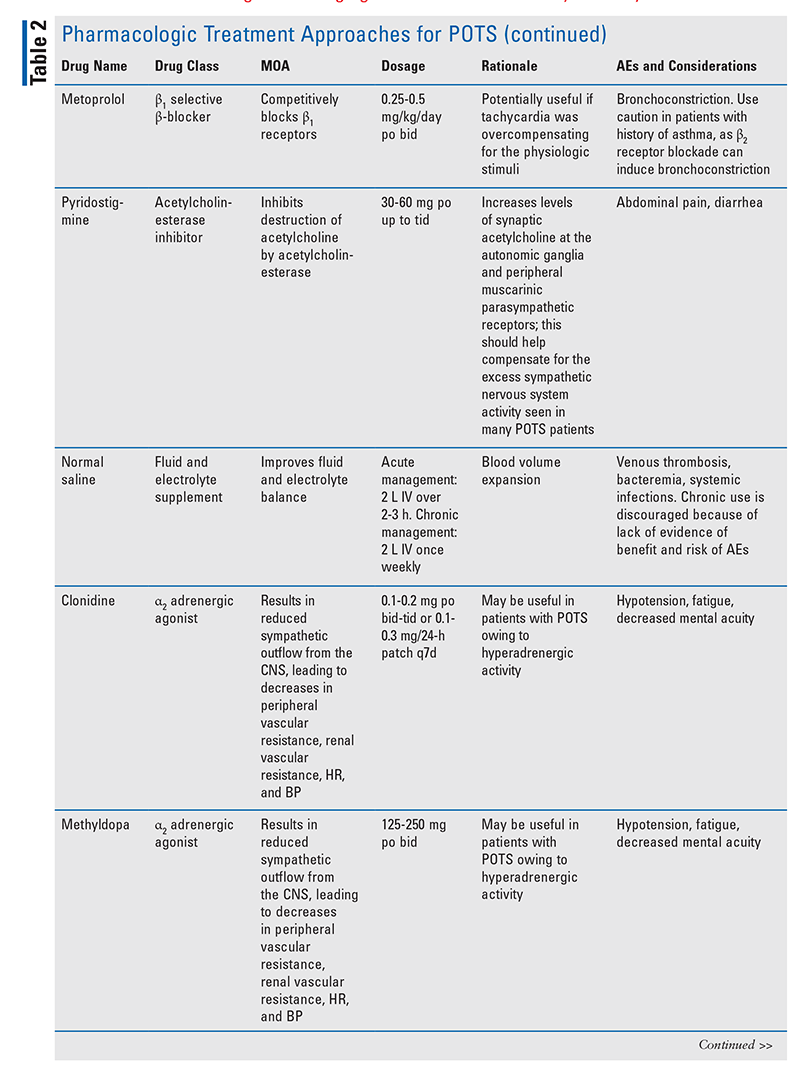
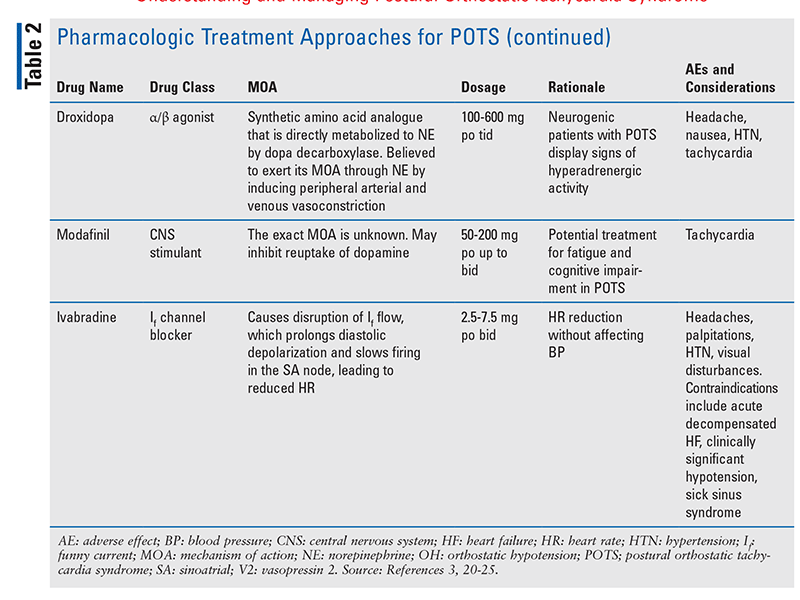
If a suboptimal response is observed following nonpharmacologic management, pharmacologic treatment may be considered (TABLE 2).3,20-25 Although currently no medications are FDA-approved for managing POTS, some therapies exist that are based on clinical observation and results from small studies.3 Before treatment is initiated, pharmacists and other healthcare professionals should take into consideration past medical history, comorbidities, and potential drug-drug and drug-disease interactions that may influence the selected approach. To optimize therapy, patients should be monitored for their symptomatic response to therapeutics and for signs of adverse effects warranting a dose reduction or discontinuation of therapy.
The Pharmacist’s Role
Despite the growing number of POTS cases since the start of the COVID-19 pandemic, the epidemiology and pathophysiology of POTS are not fully elucidated. This may result in misdiagnosis of this syndrome related to a paucity of research and the lack of formal education clinicians receive on the diagnosis and management of POTS. Consequently, these patients may also be misinformed. As the most accessible healthcare professionals, pharmacists are uniquely positioned to educate clinicians and care for patients with POTS.
Given their medication expertise, pharmacists can collaborate interprofessionally with other healthcare providers to ensure that patient factors such as comorbidities and drug interactions are considered in order to optimize medication therapy. When it is safe to do so, treatment should be initiated using an individualized approach. It should be kept in mind that there is no FDA-approved medication for POTS and no medication will work universally for all patients. Pharmacists should be aware of the various treatment approaches and monitor patients to determine optimal therapeutics.
In an outpatient setting, pharmacists can recognize patients presenting with classic symptoms of POTS, such as lightheadedness, fatigue, and elevated HR upon standing up from a supine position. In the absence of a clear underlying cause, pharmacists can recommend that patients schedule an appointment with their physician to further evaluate symptoms. If a patient is diagnosed with POTS, the pharmacist can provide education on the disorder, including typical presentation and nonpharmacologic and pharmacologic treatment approaches. It is important to understand that pharmacist collaboration in the care of patients with POTS will ultimately help improve quality of life and health outcomes.
REFERENCES
1. Fedorowski A. Postural orthostatic tachycardia syndrome: clinical presentation, aetiology and management. J Intern Med. 2019;285(4):352-366.
2. Johns Hopkins Medicine. Postural orthostatic tachycardia syndrome (POTS). www.hopkinsmedicine.org/health/conditions-and-diseases/postural-orthostatic-tachycardia-syndrome-pots. Accessed October 22, 2021.
3. Miller AJ, Raj SR. Pharmacotherapy for postural tachycardia syndrome. Auton Neurosci Basic Clin. 2018;215:28-36.
4. Dysautonomia International. Diagnostic delay in POTS. www.dysautonomiainternational.org/page.php?ID=184. Accessed October 10, 2021.
5. Bryarly M, Phillips LT, Fu Q, et al. Postural orthostatic tachycardia syndrome: JACC focus seminar. J Am Coll Cardiol. 2019;73(10):1207-1228.
6. CDC. COVID-19: data & surveillance. www.cdc.gov/coronavirus/2019-ncov/cases-updates/index.html. Accessed December 15, 2021.
7. Genetic and Rare Diseases Information Center. Postural orthostatic tachycardia syndrome. https://rarediseases.info.nih.gov/diseases/9597/postural-orthostatic-tachycardia-syndrome. Accessed October 10, 2021.
8. Kesserwani H. Postural orthostatic tachycardia syndrome misdiagnosed as anxiety: a case report with a review of therapy and pathophysiology. Cureus. 2020;12(10):e10881.
9. Johns Hopkins Medicine. COVID-19 and POTS: is there a link? www.hopkinsmedicine.org/health/conditions-and-diseases/coronavirus/covid19-and-pots-is-there-a-link. Accessed October 9, 2021.
10. Goldstein DS. The possible association between COVID-19 and postural tachycardia syndrome. Heart Rhythm. 2021;18(4):508-509.
11. Johns Hopkins Coronavirus Resource Center. COVID-19 map. https://coronavirus.jhu.edu/map.html. Accessed November 1, 2021.
12. Kanjwal K, Jamal S, Kichloo A, Grubb BP. New-onset postural orthostatic tachycardia syndrome following coronavirus disease 2019 infection. J Innov Card Rhythm Manag. 2020;11(11):4302-4304.
13. Sprangers RL, Wesseling KH, Imholz AL, et al. Initial blood pressure fall on stand up and exercise explained by changes in total peripheral resistance. J Appl Physiol (1985). 1991;70(2):523-530.
14. Mayo Clinic. Orthostatic hypotension (postural hypotension): symptoms and causes. www.mayoclinic.org/diseases-conditions/orthostatic-hypotension/symptoms-causes/syc-20352548. Accessed October 24, 2021.
15. Benarroch EE. Postural tachycardia syndrome: a heterogeneous and multifactorial disorder. Mayo Clin Proc. 2012;87(12):1214-1225.
16. Merriam-Webster. Deconditioning. www.merriam-webster.com/medical/deconditioning. Accessed October 24, 2021.
17. van der Zalm T, Alsma J, van de Poll SWE, et al. Postural orthostatic tachycardia syndrome (POTS): a common but unfamiliar syndrome. Neth J Med. 2019;77(1):3-9.
18. George SA, Bivens TB, Howden EJ, et al. The international POTS registry: evaluating the efficacy of an exercise training intervention in a community setting. Heart Rhythm. 2016;13(4):943-950.
19. Miglis MG, Barwick F. Sleep disorders in patients with postural tachycardia syndrome: a review of the literature and guide for clinicians. Auton Neurosci. 2018;215:62-69.
20. Fortunato JE, Wagoner AL, Harbinson RL, et al. Effect of fludrocortisone acetate on chronic unexplained nausea and abdominal pain in children with orthostatic intolerance. J Pediatr Gastroenterol Nutr. 2014;59(1):39-43.
21. Coffin ST, Black BK, Biaggioni I, et al. Desmopressin acutely decreases tachycardia and improves symptoms in the postural tachycardia syndrome. Heart Rhythm. 2012;9(9):1484-1490.
22. Deng X, Zhang Y, Liao Y, Du J. Efficacy of B-blockers on postural tachycardia syndrome in children and adolescents: a systematic review and meta-analysis. Front Pediatr. 2019;7:460.
23. Gaffney FA, Lane LB, Pettinger W, Blomqvist CG. Effects of long-term clonidine administration on the hemodynamic and neuroendocrine postural responses of patients with dysautonomia. Chest. 1983;83(2 suppl):436-438.
24. Ruzieh M, Dasa O, Pacenta A, et al. Droxidopa in the treatment of postural orthostatic tachycardia syndrome. Am J Ther. 2017;24(2):e157-e161.
25. Kpaeyeh AG, Mar PL, Raj V, et al. Hemodynamic profiles and tolerability of modafinil in the treatment of POTS: a randomized placebo-controlled trial. J Clin Psychopharmacol. 2014;34(6):738-741.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.






