US Pharm. 2020;45(4):HS10-HS16.
ABSTRACT: Bacteria are remarkably adaptable organisms with an innate ability to circumvent damage if exposed to a toxic environment. Antimicrobial-resistant bacteria are present worldwide, and many common infections are becoming more difficult to treat. Continued resistance is rapidly eliminating treatment options for patients, and the cost burden to treat a multidrug-resistant infection is climbing. Owing to the substantial costs associated with drug development, the introduction of novel antibiotics has lagged behind the increase in bacterial resistance. To address this crisis, pharmacists can take an active role in antimicrobial stewardship and foster understanding of how bacteria evade even the strongest available antimicrobial agents.
Bacteria are remarkably adaptable organisms with an innate ability to circumvent damage if exposed to a toxic environment. Since the development of the first antibiotic less than a century ago, there has been an exponential growth in antimicrobial resistance that is disproportionate to the rate at which antibiotics are introduced.1 The emergence of resistance and the inversely stagnant development of novel antibiotics related to the substantial costs associated with drug development have worsened the impact of infectious diseases on mortality and healthcare costs. Continued resistance is rapidly eliminating treatment options for patients, and the cost burden to treat a multidrug-resistant infection is climbing, reaching more than $2.2 billion annually in the United States.2 Antibiotic resistance has been found in most bacteria, but several bacteria are particularly problematic and are becoming common among hospital-acquired infections: Enterococcus faecium, Staphylococcus aureus, Klebsiella pneumoniae, Acinetobacter baumannii, Pseudomonas aeruginosa, and Enterobacteriaceae (ESKAPE pathogens).3-5 The CDC recently published an updated list of the most threatening resistant organisms in the U.S. based on hospitalizations and mortality data from 2017 (TABLE 1).6

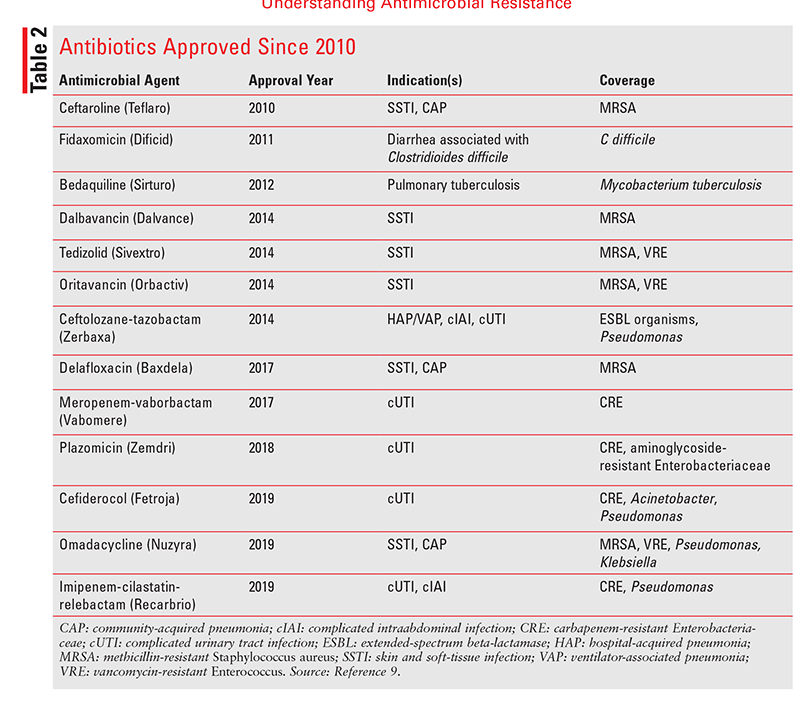
The CDC estimates that more than 47 million antibiotic courses are prescribed each year in the U.S. for infections that do not need antibiotic treatment.7 The misuse and overuse of antibiotics have put the world at risk, and the growing threat prompted the World Health Organization to issue a global action plan for antimicrobial resistance in 2015.8 In the same year, the U.S. formulated a national action plan for combating antibiotic-resistant bacteria.6 These initiatives launched the implementation of antimicrobial stewardship (AMS) programs and research to prevent further resistance. Unfortunately, bacteria adapt quickly, and the development of antimicrobial agents is truly a race against time. With each new agent designed to overcome a resistance mechanism, pathogens inevitably establish new strategies to withstand the next antibiotic. Few agents have been introduced since 2010 (TABLE 2), and even fewer have activity against ESKAPE pathogens.9 As of June 2019, only 42 antibiotics were in clinical development, and just three in five agents entering phase III trials are approved.9 Preventing further resistance requires not only persistent AMS to reserve existing agents, but also a fundamental understanding of antibiotic mechanisms of action and the strategies bacteria employ to resist these agents.
Epidemiology
Antimicrobial-resistant bacteria are present in every country in the world, and many common infections are becoming more difficult to treat.10 For example, urinary tract infections (UTIs) caused by resistant Escherichia coli have reduced the efficacy of fluoroquinolones globally. Gonorrhea treatment failure with third-generation cephalosporins has been reported in at least 10 countries. More than 2.8 million antibiotic-resistant infections occur each year in the U.S., leading to more than 35,000 deaths.6 There is also a direct relationship between the prevalence of resistant pathogens and rates of sepsis-related outcomes. In a recent study that examined this correlation in hospitalized patients in the U.S. from 2011 to 2014, the highest rates of sepsis were associated with fluoroquinolone-resistant E coli, third-generation cephalosporins and carbapenem-resistant Klebsiella species, and vancomycin-resistant Enterococcus (VRE).11
Resistance Mechanisms
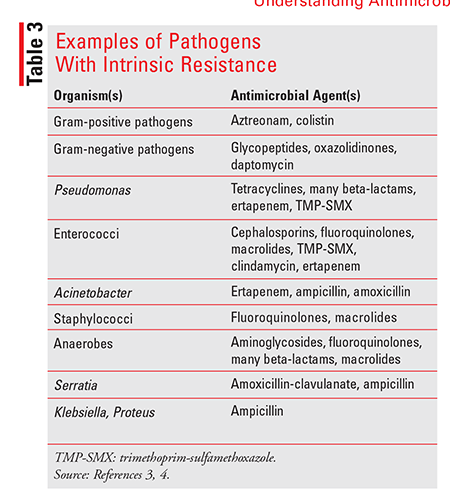
There are two types of bacterial resistance: intrinsic and acquired. In intrinsic resistance, the antibiotic never possessed activity against the pathogen (TABLE 3).3-5 Acquired resistance is achieved through the transfer of genetic material that confers resistance. Some bacterial genes are carried on plasmids—small, circular, double-stranded DNA molecules that are distinct from chromosomal DNA.12 Plasmids are transferred from one bacterium to another through conjugation, and this exchange can occur between bacteria of different species. The strategies that bacteria use to develop acquired resistance are encoded on plasmids and may be classified into four mechanisms: 1) decreased permeability of the cell wall to antibiotics; 2) modification of enzymes to inactivate antibiotics; 3) drug target site changes; and 4) efflux pumps that remove antibiotics from the cell.4 Drug inactivation through enzymes is the predominant mechanism used by bacteria, and the expression of genes that encode these enzymes may be induced by particular medications (facultative) or constantly expressed (constitutive).
Multidrug-Resistant Enterococcus: Enterococci, which are predominantly benign gut bacteria, may be the best-known family of microbes equipped with intrinsic and acquired antibiotic resistance. Of particular concern are E faecium and Enterococcus faecalis. These organisms can have multiple acquired resistance mechanisms, thereby resulting in multidrug resistance.13 High levels of resistance may exist to beta-lactams (through beta-lactamase enzymes and altered binding proteins), vancomycin (via changes in peptidoglycan synthesis; known as VRE), and aminoglycosides (through enzymatic degradation).14,15 Ampicillin remains the drug of choice for susceptible Enterococcus infections, but few options remain to treat systemic multidrug-resistant Enterococcus infections; these include linezolid, daptomycin, and tigecycline.3,14
Methicillin-Resistant Staphylococcus aureus (MRSA) and mecA: MRSA first appeared in the early 1960s, shortly after the introduction of methicillin.16 As with most gram-positive organisms, the cell wall serves as the main target for antimicrobial agents and consequently fosters acquired antimicrobial resistance. For S aureus to be considered MRSA, the bacterium must possess the mecA gene, which encodes for a structural change in penicillin-binding protein 2a (PBP2a).17 This change prevents beta-lactam antibiotics from binding to the cell wall. Laboratory testing for S aureus susceptibility to methicillin is not commonly performed, owing to the instability of methicillin plates; rather, MRSA is determined by a similar beta-lactam: oxacillin. The Clinical Laboratory Standards Institute defines methicillin resistance as an oxacillin mean inhibitory concentration of at least 4 mcg/mL, and isolates resistant to oxacillin are resistant to all beta-lactams, with few exceptions (e.g., ceftaroline).18
Extended-Spectrum Beta-Lactamase (ESBL)–Producing Organisms: Many gram-negative species of bacteria have been found to possess acquired resistance to beta-lactam antibiotics through the production of beta-lactamase. This enzyme deactivates the agent’s antimicrobial properties by hydrolyzing its beta-lactam ring.19 The first beta-lactamase to be isolated was a penicillinase identified in E coli in 1940, before penicillin entered medical use. New agents were developed over the years to resist the effects of this enzyme, including broad-spectrum cephalosporins. Predictably, the introduction of these antibiotics led to resistance against broader-spectrum agents, giving rise to the ESBL enzyme. Currently, more than 150 ESBLs are found in many different Enterobacteriaceae species and in P aeruginosa.20
Carbapenems have remained the drug of choice for ESBL-producing pathogens. This beta-lactam antibiotic subgroup includes meropenem, ertapenem, doripenem, and imipenem-cilastatin. All of these agents—with the exception of ertapenem, which does not have activity against Acinetobacter or Pseudomonas—have demonstrated efficacy against ESBLs.3 Similar to the selective development of ESBL enzymes following the introduction of broad-spectrum cephalosporins, there has been an emergence of carbapenem-resistant pathogens capable of hydrolyzing carbapenems through the activity of a carbapenemase enzyme.
Carbapenemase Enzyme: Carbapenems are the broadest-spectrum antibiotics available and are favorable choices for many resistant gram-negative nosocomial infections.21 As effective as these agents are, there has been an increase in carbapenem-resistant organisms as a result of carbapenem overuse, leaving patients with limited to no treatment options. Carbapenem-resistant Enterobacteriaceae (CRE) and Acinetobacter are associated with a combined hospitalization of 21,600 patients and 1,800 deaths each year in the U.S.6 Other possible carbapenemase-producing organisms include K pneumoniae, P aeruginosa, and E coli.21
In order to preserve these antibiotics, carbapenem-sparing agents with activity against ESBL-producing pathogens should be used whenever possible. Such agents include piperacillin-tazobactam, cefepime, and ceftolozane-tazobactam.22 However, carbapenems are preferred for certain infection sites, including the bloodstream and lungs. In the MERINO trial, 30-day mortality was higher in patients with ESBL E coli or K pneumoniae–associated bacteremia that was treated with piperacillin-tazobactam versus a carbapenem.23
Much effort has gone into developing new antibiotics to combat these bacteria. A new cephalosporin, cefiderocol, which was approved in 2019 to treat UTIs, has activity against CRE. Recent beta-lactam combinations (meropenem-vaborbactam and ceftazidime-avibactam) have shown good in vitro activity against CRE and are becoming available on many hospital formularies to treat UTIs, intraabdominal infections, and respiratory tract infections.24 The polymyxins (colistin and polymyxin B), an older antibiotic class, have fallen out of favor because of their renal and neurologic toxicities; however, they are effective against carbapenem-resistant pathogens and may be useful for salvage therapy.25 Both polymyxin agents are highly similar and have a narrow therapeutic window, requiring careful dosing and close monitoring of renal function, although polymyxin B is associated with less nephrotoxicity than colistin.
P aeruginosa: Pseudomonas is an opportunistic gram-negative pathogen responsible for a large number of nosocomial infections. Antimicrobial agents used to treat Pseudomonas include beta-lactams, fluoroquinolones, and aminoglycosides, but this genus can display multiple mechanisms of resistance. Intrinsically, Pseudomonas has a relatively low membrane permeability (up to 100 times lower than that of E coli).26 The acquired-resistance mechanisms potentially expressed by Pseudomonas include any of the four previously described strategies. Fluoroquinolones exhibit antimicrobial activity by targeting bacterial enzymes involved in DNA replication.9,10 Fluoroquinolone-resistant strains of Pseudomonas avoid this effect by mutating the genes encoding for those enzymes. Aminoglycoside-resistant Pseudomonas is capable of producing aminoglycoside-modifying enzymes. Beta-lactam resistance in Pseudomonas is due to modifications in penicillin-binding proteins, overexpression of efflux pumps, and enzymatic drug inactivation.26
Increased exposure of Pseudomonas to an antipseudomonal beta-lactam antibiotic has been shown to increase the risk of developing resistance.27 In a retrospective cohort study of 7,118 patients, each additional day of antipseudomonal beta-lactam therapy was associated with a 4% increased risk of new resistance at 60-day follow-up. To avoid continuing resistance, diligent efforts should be made to limit beta-lactam exposure to the shortest effective duration.
Enterobacteriaceae and ampC: More than 100 species of Enterobacteriaceae exist, but a few pathogens in this family (Serratia marcescens, Morganella morganii, Proteus vulgaris, Citrobacter species, and Enterobacter species) possess an inducible beta-lactamase enzyme known as ampC.28 The ampC enzyme, which is normally not expressed, does not appear to confer resistance against many antibiotics upon first glance at a culture and sensitivity report, but this may be deceiving. Many penicillins and first- to third-generation cephalosporins do not show resistance, but these agents activate ampC and will induce resistance. The presence of ampC is not detectable by most laboratories, but if resistance to cefoxitin is displayed on culture and sensitivity reports, this can serve as a surrogate marker for ampC, in which case penicillins and narrow-spectrum cephalosporins should be avoided.29
The Pharmacist’s Role
Pharmacists serve as medication experts on healthcare teams, and given the rapid expansion of the pharmacist’s professional role, they are optimally positioned to assess treatment necessity and appropriate antibiotic selection. Their knowledge of antibiotic mechanisms of action and strategies used by resistant bacteria enables pharmacists to make evidence-based decisions about drug therapy even without formal training in infectious diseases. The Society of Infectious Diseases Pharmacists recognizes that every pharmacist can contribute to AMS.30
Objective data have been published that illustrate the impact pharmacists have on the use of antimicrobials. A literature review that investigated the clinical and economic impact of pharmacist-led interventions related to antimicrobial use showed a decrease in antibiotic costs up to 95%, as well as reductions in readmission, mortality, and infection rates.31 Selection of the most appropriate agent positively affects patient outcomes and ensures the preservation of available antimicrobial resources.
Conclusion
The pathogens and mechanisms described in this article are limited to those that are involved in the global crisis of antimicrobial resistance. Bacteria are ancient organisms equipped with the abilities necessary for survival in their environment, including the host who is taking antibiotics. The gap between increasing resistance and drug development is growing wider, which necessitates heightened AMS and a comprehensive understanding of how bacteria evade even the strongest available antibiotics. The time expended in attempts to develop new antibiotics capable of withstanding the latest resistance mechanism has proven futile. Pharmacist involvement in drug selection and AMS can improve patient outcomes and prevent further progression of bacterial resistance. Developing new medications is not the solution to this crisis, but preserving the available agents is critical.
REFERENCES
1. Chen LF, Chopra T, Kaye KS. Pathogens resistant to antibacterial agents. Med Clin North Am. 2011;95(4):647-676.
2. Thorpe KE, Joski P, Johnston KJ. Antibiotic-resistant infection treatment costs have doubled since 2002, now exceeding $2 billion annually. Health Aff (Millwood). 2018;37(4):662-669.
3. Gallagher JC, MacDougall C. Antibiotics Simplified. 4th ed. Burlington, MA: Jones and Bartlett Learning; 2018.
4. Lee GC, Burgess DS. Antimicrobial regimen selection. In: Di Piro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 9th ed. New York, NY: McGraw Hill Education; 2014.
5. Reygaert WC. An overview of the antimicrobial resistance mechanisms of bacteria. AIMS Microbiol. 2018;4(3):482-501.
6. CDC. Antibiotic resistance threats in the United States, 2019. Atlanta, GA: U.S. Department of Health and Human Services, CDC; 2019.
7. CDC. Antibiotic use in the United States, 2018 update: progress and opportunities. Atlanta, GA: U.S. Department of Health and Human Services, CDC; 2019.
8. World Health Organization. Global action plan on antimicrobial resistance. Geneva, Switzerland: World Health Organization; 2015.
9. Pew Charitable Trusts. Tracking the global pipeline of antibiotics in development. www.pewtrusts.org/en/research-and-analysis/issue-briefs/2019/09/tracking-the-global-pipeline-of-antibiotics-in-development. Accessed March 9, 2020.
10. World Health Organization. Antimicrobial resistance and primary health care. Geneva, Switzerland: World Health Organization; 2018.
11. Goldstein E, MacFadden DR, Karaca Z, et al. Antimicrobial resistance prevalence, rates of hospitalization with septicemia and rates of mortality with sepsis in adults in different US states. Int J Antimicrob Agents. 2019;54(1):23-34.
12. Smalla K, Jechalke S, Top EM. Plasmid detection, characterization, and ecology. Microbiol Spectr. 2015;3(1):PLAS-0038-2014.
13. Murray BE. The life and times of the Enterococcus. Clin Microbiol Rev. 1990;3(1):46-65.
14. Gao W, Howden BP, Stinear TP. Evolution of virulence in Enterococcus faecium, a hospital-adapted opportunistic pathogen. Curr Opin Microbiol. 2018;41:76-82.
15. Miller WR, Murray BE, Rice LB, Arias CA. Vancomycin-resistant enterococci: therapeutic challenges in the 21st century. Infect Dis Clin North Am. 2016;30(2):415-439.
16. Enright MC, Robinson DA, Randle G, et al. The evolutionary history of methicillin-resistant Staphylococcus aureus (MRSA). Proc Natl Acad Sci U S A. 2002;99(11):7687-7692.
17. Peacock SJ, Paterson GK. Mechanism of methicillin resistance in Staphylococcus aureus. Annu Rev Biochem. 2015;84:577-601.
18. Patel JB, Weinstein MP, Eliopoulos GM, et al. M100: Performance Standards for Antimicrobial Susceptibility Testing. 27th ed. Wayne, PA: Clinical and Laboratory Standards Institute; 2017.
19. Brook I. Beta-lactamase-producing bacteria and their role in infection. Rev Med Microbiol. 2005;16(3):91-99.
20. Bradford PA. Extended-spectrum beta-lactamases in the 21st century: characterization, epidemiology, and detection of this important resistance threat. Clin Microbiol Rev. 2001;14(4):933-951.
21. Ye Y, Xu L, Han Y, et al. Mechanism for carbapenem resistance of clinical Enterobacteriaceae isolates. Exp Ther Med. 2018;15(1):1143-1149.
22. Wilson APR. Sparing carbapenem usage. J Antimicrob Chemother. 2017;72(9):2410-2417.
23. Harris PNA, Tambyah PA, Lye DC, et al. Effect of piperacillin-tazobactam vs meropenem on 30-day mortality for patients with E coli or Klebsiella pneumoniae bloodstream infection and ceftriaxone resistance: a randomized clinical trial. JAMA. 2018;320(10):984-994.
24. Pogue JM, Bonomo RA, Kaye KS. Ceftazidime/avibactam, meropenem/vaborbactam, or both? Clinical and formulary considerations. Clin Infect Dis. 2019;68(3):519-524.
25. Tsuji BT, Pogue JM, Zavascki AP, et al. International consensus guidelines for the optimal use of the polymyxins: endorsed by the American College of Clinical Pharmacy (ACCP), European Society of Clinical Microbiology and Infectious Diseases (ESCMID), Infectious Diseases Society of America (IDSA), International Society for Anti-infective Pharmacology (ISAP), Society of Critical Care Medicine (SCCM), and Society of Infectious Diseases Pharmacists (SIDP). Pharmacotherapy. 2019;39(1):10-39.
26. Pang Z, Raudonis R, Glick BR, et al. Antibiotic resistance in Pseudomonas aeruginosa: mechanisms and alternative therapeutic strategies. Biotechnol Adv. 2019;37(1):177-192.
27. Teshome BF, Vouri SM, Hampton N, et al. Duration of exposure to antipseudomonal B-lactam antibiotics in the critically Ill and development of new resistance. Pharmacotherapy. 2019;39(3):261-270.
28. Jacoby GA. AmpC beta-lactamases. Clin Microbiol Rev. 2009;22(1):161-182.
29. Meini S, Tascini C, Cei M, et al. AmpC B-lactamase-producing Enterobacterales: what a clinician should know. Infection. 2019;47(3):363-375.
30. Parente DM, Morton J. Role of the pharmacist in antimicrobial stewardship. Med Clin North Am. 2018;102(5):929-936.
31. Leache L, Aquerreta I, Aldaz A, et al. Evidence of clinical and economic impact of pharmacist interventions related to antimicrobials in the hospital setting. Eur J Clin Microbiol Infect Dis. 2018;37(5):799-822.
To comment on this article, contact rdavidson@uspharmacist.com.






