US Pharm. 2017;42(9):34-38.
ABSTRACT: Vocal cord dysfunction (VCD) is the abnormal adduction of the vocal cords during inspiration or expiration that results in varying degrees of airway obstruction. VCD is more common in females and usually presents during childhood or adolescence and continues up to age 40 years. Studies have found an increased prevalence of VCD in female athletes and academic high-achievers compared with the general population. VCD is often misdiagnosed as asthma or exercise-induced bronchospasms (EIB) because of similarities in clinical presentation. Since misdiagnosis results in inappropriate pharmacotherapy, it is important for the pharmacist to have a thorough understanding of VCD in order to differentiate it from asthma and EIB.
Vocal cord dysfunction (VCD) is the abnormal adduction of the vocal cords during inspiration or expiration that results in varying degrees of airway obstruction.1-3 First described in 1842 as a disorder of the laryngeal muscles brought on by “hysteria” and subsequently observed by laryngoscopy in 1869, VCD was called hysteric croup, Munchausen’s stridor, and psychogenic stridor because the etiology was assumed to be psychological.4,5 It is now recognized that VCD is not solely psychological; therefore, the terminology has evolved to include factitious asthma, irritable larynx syndrome, paradoxical vocal-fold motion, paradoxical vocal cord dysfunction, and refractory asthma.4,6,7 The clinical presentation of VCD involves wheezing, stridor, change in vocal quality, dyspnea (including upon exertion), chest tightness, cough, respiratory distress, and choking sensations.1,3,4,8 VCD, which occurs more often in females, especially athletes, usually presents in childhood or adolescence and lasts to age 40 years.3,4
VCD is often misdiagnosed as asthma or exercise-induced bronchospasms (EIB) because of similarities in clinical presentation.3 The misdiagnosis is often discovered after asthma pharmacotherapy fails to control symptoms.1 To avoid inappropriate pharmacotherapy, pharmacists must be able to differentiate between asthma, EIB, and VCD. The diagnostic gold standard for VCD is laryngoscopy during an attack.9
It is possible for a person to have concomitant asthma or EIB with VCD, which makes diagnosis more difficult.3 Studies have found an increased prevalence of asthma and EIB in athletes (recreational or elite) and academic high-achievers compared with the general population.1,10 The female-to-male ratio for VCD prevalence ranges from 2:1 to 3:1.9,11,12
Epidemiology
VCD is a spectrum of uncommon, complex breathing disorders related to laryngeal dysfunction, and the most common presenting symptom is dyspnea upon exertion.10,13 The true prevalence and incidence of VCD are not known because of inconsistencies in the disorder’s definition and diagnostic criteria and because patients can have concomitant VCD and EIB or asthma.9,10 In 148 recreational athletes and middle-school to collegiate-level athletes evaluated for respiratory complaints upon exercise, 70% had confirmed VCD.10 Of those with confirmed VCD, 31% had concomitant EIB and 6% had concomitant asthma.10 The female-to-male ratio, which exceeded 2:1, was consistent with that in other studies that concluded that VCD is more prevalent in females, especially female athletes; therefore, pharmacists should be aware of female athletes who present to the pharmacy poorly controlled on their current asthma medication regimens.
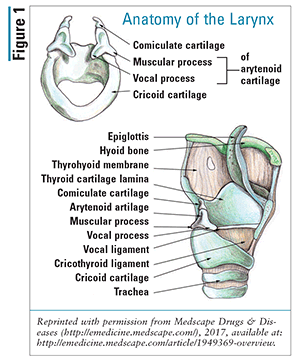
Airway Anatomy and Physiology
Knowledge of normal laryngeal anatomy and physiology will help the pharmacist understand the etiology of VCD (FIGURE 1).6 Important anatomical structures include the larynx (intrinsic and extrinsic muscles), arytenoids, epiglottis, glottis (vocal-fold complex), vocal cords, vocal ligament (true vocal cord), mucosal fold (vocal fold), aryepiglottic folds (false vocal folds), vestibular ligament (false vocal cord), and arytenoid cartilages.14 The larynx is located in the anterior neck above the trachea.14 The vocal cords, or vocal folds, are in the midsection of the larynx and stretch horizontally from the thyroid cartilage anteriorly, attaching to the vocal process of the arytenoid cartilage posteriorly.6,14 Contraction of the thyroarytenoid, interarytenoid, and lateral cricoarytenoid muscles causes adduction of the vocal cords.14 The respiratory movements of the vocal cords are coordinated with those of the diaphragm and other muscles of the ventilator pump.15 A complex innervation of muscles and nerves causes the larynx to adduct and abduct the vocal cords.14-16 The lateral cricoarytenoid and posterior cricoarytenoid muscles and the vagus, recurrent laryngeal, and superior laryngeal nerves are involved in this process.14-16 The vocal cords begin to separate just before the diaphragmatic contraction, which is mechanically advantageous.14 Sensory fibers in the intercostal nerves can affect laryngeal movements, but the responses are complex.14 These coordinated movements result in the vocal cords moving away from the midline during inspiration and slightly toward the midline during expiration.16
Under normal conditions, the vocal cords form a V-shaped opening that is narrowest anteriorly when viewed from the upper airway.14-16 FIGURE 2a demonstrates vocal cord abduction during normal inhalation, and FIGURE 2b shows the vocal cords during normal phonation. In patients with VCD, however, only the anterior two-thirds of the vocal cords adducts during inspiration and there is a posterior diamond-shaped chink (lack of full closure).14-16 FIGURE 2c demonstrates vocal cord adduction (paradoxical movement) and the diamond-shaped chink. This can be detected only by direct observation with flexible laryngoscopy, which is the gold standard to confirm the presence of VCD.9

VCD Etiology
The cause of VCD may be multifactorial. VCD may be triggered by many factors that also trigger asthma or EIB. The major exacerbating factors include exercise, airborne irritants, postnasal drip (PND), gastroesophageal reflux disease (GERD), laryngopharyngeal reflux (LPR), and certain medications.
Exercise: Exercise can trigger both VCD and EIB, making diagnosis difficult. When a patient presents with dyspnea upon exertion and is not achieving symptom control with bronchodilators, VCD should be included in the differential.3,10 This is important because in 96% of subjects in one study who participated in sports, the most common primary respiratory complaint was dyspnea upon exertion and the most common diagnosis was VCD (in 70%).10 Respiratory symptoms associated with exercise occurred more frequently in younger athletes than in college athletes, and VCD was more common in females.10 Other activities, such as talking, laughing, deep breathing, and swallowing, also can trigger VCD.17
Airborne Irritants: Exposure to respiratory irritants has been implicated in both VCD and asthma. In patients with asthma, this is classified as irritant-induced asthma.18 Acute or recurrent irritant exposure could lead to laryngeal hypersensitivity and result in VCD.16 Patients should be questioned on the temporal relationship of their exposure to strong odors and substances such as perfumes, dust or particulate matter, smoke, smoldering fumes, and household cleaning chemicals and the onset of VCD symptoms.3,6 One irritant associated with VCD, especially in swimmers and divers, is chlorine.6 Athletes with known allergies or rhinitis should avoid training environments with high levels of airborne allergens.19
PND: PND can cause direct irritation of the vocal cords, resulting in VCD.15 Common disease states associated with PND include allergic and nonallergic rhinitis, maxillofacial sinus infections, and rhinosinusitis.3 Often these are chronic disease states, and patients therefore assume that PND is normal. PND causes airway hyperresponsiveness, especially in patients with rhinosinusitis.3 Upon diagnosis, treatment may require months before symptoms resolve.20
GERD and LPR: GERD has been estimated to be as high as 60% in the general population and has been associated with VCD and asthma.21 The precise mechanism of GERD in VCD has not been fully elucidated, but is thought to be secondary to laryngeal damage. Symptoms of GERD include throat-clearing, hoarseness, chronic cough, heartburn, burning sensation in the throat, acid regurgitation, chest pain, and wheezing.21,22 Treatment of GERD to improve VCD symptoms is helpful only in some patients.3
LPR is the retrograde flow of gastric secretions into the laryngopharynx, which is highly susceptible to these secretions.21 Upon repeated contact with the laryngeal mucosa, these gastric secretions can cause laryngeal inflammation, resulting in VCD.21 Chronic PND and LPR may lead to increased laryngeal sensitivity and subsequent laryngeal hyperresponsiveness.21 Symptoms of LPR include persistent throat irritation and tightness, excessive mucus production, dyspnea, and stridor.23 Dyspepsia and heartburn are less common in LPR.23
Patients with VCD may not report classic symptoms of acid reflux or heartburn even in the presence of laryngoscopic evidence of laryngeal inflammation.6
Medications: Extrapyramidal signs, such as torticollis, are associated with neuroleptic drugs and metoclopramide, which may result in a focal dystonic reaction and have been reported to lead to VCD.3,24 These events are rare; however, the pharmacist should conduct a thorough medication review in patients presenting with symptoms of VCD.12,25
Evaluation and Management
Before pharmacotherapy is initiated, objective testing for EIB or asthma should be done.11 Because of the common misdiagnosis of VCD as asthma or EIB, patients should not be treated for asthma based on symptoms alone; objective tests must be conducted.3,10 To differentiate the diseases, a thorough patient history with physical examination should be conducted to determine which factors precipitate an attack, and spirometry should be performed by a trained professional.6 Spirometry should be conducted to determine the presence of asthma or EIB.6 Once asthma has been ruled out, the diagnosis of VCD should be considered and confirmed by laryngoscopy. As explained previously, laryngoscopy is used to observe the abnormal adduction of vocal cords during inspiration and to rule out other laryngeal anomalies.16 Because VCD is multifaceted, a multidisciplinary approach to management is necessary.6 Pulmonologists, otolaryngologists, physiatrists, clinical psychologists, allergists, and speech therapists work together in the diagnosis and management of VCD. Therefore, it is important for the pharmacist to monitor the patient’s medications for drug interactions or duplication of pharmacologic classes prescribed by multiple healthcare providers.
The management of VCD is multifactorial, with speech therapy universally considered the cornerstone of treatment.11 The purpose of speech therapy is to teach the patient to maintain an open airway during respiration, and success rates are as high as 95% in female athletes.1 Other nonpharmacologic management techniques are to approach the patient in a calm, reassuring manner to help terminate an attack and to use chronic therapies such as biofeedback, psychotherapy, and/or hypnosis.11,16 Pharmacologic therapies that have shown limited benefit in acute attacks include benzodiazepines, inhaled heliox, and nebulized lidocaine.11 The benzodiazepine selection and dosage depend on the patient’s individual needs. It should be emphasized that benzodiazepines have the potential to be habit-forming and can result in abuse or misuse.26 Heliox is a gas mixture of 70% to 80% helium and 20% to 30% oxygen.27 Nebulized lidocaine has been administered at concentrations of 1%, 2%, and 4%, but levels exceeding 5 mcg/mL are associated with serious toxicity; therefore, the pharmacist should be careful not to exceed these investigational doses.28 Limited data have also demonstrated that inhaled ipratropium bromide (two inhalations prior to exercise) is advantageous in preventing exercise-induced symptoms.29 None of these agents are FDA-approved for this use.
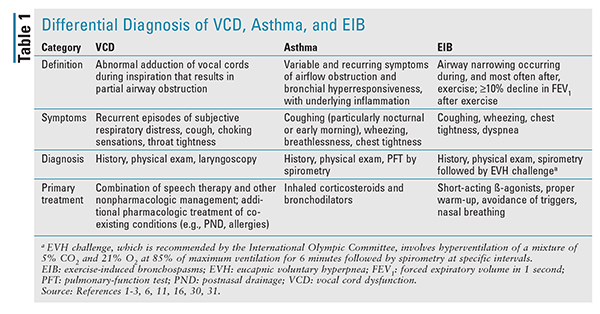
Pharmacists usually see patients more often than the prescribing physician does, and they can monitor whether a patient is refilling medications too frequently. When a problem is perceived, the pharmacist can further question the patient and recommend additional medical consultation. For a summary of the differences between VCD, asthma, and EIB, see TABLE 1.
Conclusion
VCD is a multifaceted disease characterized by abnormal adduction of the vocal cords during inspiration that results in varying degrees of obstruction.1-3,9 Frequently, VCD is diagnosed only after a patient has failed traditional pharmacotherapy for asthma or EIB; therefore, better awareness and understanding of the disease are needed. Knowledge that VCD is more prevalent in females—particularly female athletes—places the pharmacist in an ideal position to recognize these patients when they present for medications. A multidisciplinary approach is necessary to properly diagnose patients and avoid unnecessary pharmacotherapy.6 As a key member of the healthcare team, the pharmacist can refer patients who have not achieved symptom control with usual treatments for asthma or EIB to the appropriate specialist to be tested for VCD.
REFERENCES
1. Sullivan MD, Heywood BM, Beukelman DR. A treatment for vocal cord dysfunction in female athletes: an outcome study. Laryngoscope. 2001;111:1751-1755.
2. Amimoto Y, Nakano H, Masumoto N, et al. Lung sound analysis in a patient with vocal cord dysfunction and bronchial asthma. J Asthma. 2012;49:227-229.
3. Deckert J, Deckert L. Vocal cord dysfunction. Am Fam Physician. 2010;81:156-159.
4. Chiang WC, Goh A, Ho L, et al. Paradoxical vocal cord dysfunction: when a wheeze is not asthma. Singapore Med J. 2008;49:e110-e112.
5. Hoyte FC. Vocal cord dysfunction. Immunol Allergy Clin North Am. 2013;33(1):1-22.
6. Wilson JJ, Theis SM, Wilson EM. Evaluation and management of vocal cord dysfunction in the athlete. Curr Sports Med Rep. 2009;8:65-70.
7. Newsham KR, Klaben BK, Miller VJ, Saunders JE. Paradoxical vocal-cord dysfunction: management in athletes. J Athl Train. 2002;37:325-328.
8. Wood RP II, Milgrom H. Vocal cord dysfunction. J Allergy Clin Immunol. 1996;98:481-485.
9. Kenn K, Balkissoon R. Vocal cord dysfunction: what do we know? Eur Respir J. 2011;37:194-200.
10. Hanks CD, Parsons J, Benninger C, et al. Etiology of dyspnea in elite and recreational athletes. Phys Sportsmed. 2012;40:28-33.
11. Ibrahim WH, Gheriani HA, Almohamed AA, Raza T. Paradoxical vocal cord motion disorder: past, present and future. Postgrad Med J. 2007;83:164-172.
12. Karaman E, Duman C, Alimoglu Y, et al. Paradoxical vocal cord motion—haloperidol usage in acute attack treatment. J Craniofac Surg. 2009;20:1602-1604.
13. Hayes JP, Nolan MT, Brennan N, FitzGerald MX. Three cases of paradoxical vocal cord adduction followed up over a 10-year period. Chest. 1993;104:678-680.
14. Bartlett D Jr. Respiratory functions of the larynx. Physiol Rev. 1989;69:33-57.
15. Shusterman D. Review of the upper airway, including olfaction, as mediator of symptoms. Environ Health Perspect. 2002;110(suppl 4):649-653.
16. Al-Alwan A, Kaminsky D. Vocal cord dysfunction in athletes: clinical presentation and review of the literature. Phys Sportsmed. 2012;40:22-27.
17. Murry T, Branski RC, Yu K, et al. Laryngeal sensory deficits in patients with chronic cough and paradoxical vocal fold movement disorder. Laryngoscope. 2010;120:1576-1581.
18. Labrecque M. Irritant-induced asthma. Curr Opin Allergy Clin Immunol. 2012;12:140-144.
19. Kippelen P, Fitch KD, Anderson SD, et al. Respiratory health of elite athletes—preventing airway injury: a critical review. Br J Sports Med. 2012;46:471-476.
20. Mikita JA, Mikita CP. Vocal cord dysfunction. Allergy Asthma Proc. 2006;27:411-414.
21. Balkissoon R, Kenn K. Asthma: vocal cord dysfunction (VCD) and other dysfunctional breathing disorders. Semin Respir Crit Care Med. 2012;33:595-605.
22. Fass R. Symptom assessment tools for gastroesophageal reflux disease (GERD) treatment. J Clin Gastroenterol. 2007;41:437-444.
23. Spyridoulias A, Lillie S, Vyas A, Fowler SJ. Detecting laryngopharyngeal reflux in patients with upper airways symptoms: symptoms, signs or salivary pepsin? Respir Med. 2015;109:963-969.
24. Tianyi FL, Agbor VN, Njim T. Metoclopramide induced acute dystonic reaction: a case report. BMC Res Notes. 2017;10:32.
25. Christodoulou C, Kalaitzi C. Antipsychotic drug-induced acute laryngeal dystonia: two case reports and a mini review. J Psychopharmacol. 2005;19:307-311.
26. Lader M. Benzodiazepine harm: how can it be reduced? Br J Clin Pharmacol. 2014;77:295-301.
27. Brugman SM, Simons SM. Vocal cord dysfunction: don’t mistake it for asthma. Phys Sportsmed. 1998;26:63-85.
28. Slaton RM, Thomas RH, Mbathi JW. Evidence for therapeutic uses of nebulized lidocaine in the treatment of intractable cough and asthma. Ann Pharmacother. 2013;47:578-585.
29. Doshi DR, Weinberger MM. Long-term outcome of vocal cord dysfunction. Ann Allergy Asthma Immunol. 2006;96:794-799.
30. National Asthma Education and Prevention Program Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma. Bethesda, MD: National Heart, Lung, and Blood Institute; 2007:1-74.
31. Parsons JP, Mastronarde JG. Exercise-induced bronchoconstriction in athletes. Chest. 2005;128:3966-3974.
To comment on this article, contact rdavidson@uspharmacist.com.





