US Pharm. 2012;37(12):50-53.
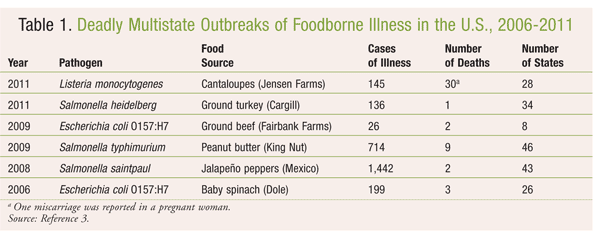
Foodborne illness poses a significant public health threat to the United States. The CDC estimates that consumption of contaminated food causes 48 million cases of illness each year, affecting approximately 15% of the population. Although the symptoms of foodborne illness are often mild and self-limiting, severe cases account for about 128,000 hospitalizations and 3,000 deaths annually in the U.S.1 The U.S. Department of Agriculture (USDA) estimates that the economic burden of foodborne illness ranges from $10 billion to $83 billion annually, a substantial impact.2 Media attention to outbreaks of foodborne illness has increased in recent years, raising awareness—as well as fear—in the American public. Television, Internet, and newspaper coverage of outbreaks, such as the contaminated bagged spinach in 2006 and contaminated cantaloupe in 2011, has contributed to awareness of the public health risk. Six deadly outbreaks were reported to the CDC from 2006 to 2011 (TABLE 1).3 In 2011, listeriosis associated with cantaloupes from a farm in Colorado was linked to 30 deaths, one of the deadliest known outbreaks of foodborne illness in the U.S.3
Foodborne illness, defined as any ailment associated with the ingestion of contaminated food, is most often associated with gastrointestinal symptoms, including diarrhea, nausea, and/or vomiting.4 Foodborne illness may be bacterial, viral, or parasitic in nature. Although most ailments have acute symptoms that resolve within a week, complications—including severe dehydration, bacteremia, renal and hepatic impairment, neurologic symptoms, miscarriage, and surgical complications—can occur.1,5
Risk Factors
Individuals who are aged less than 5 years or more than 60 years or who are immunocompromised are at greatest risk for acquiring a foodborne illness.5 Other risk factors for foodborne illness include the consumption of high-risk foods such as unpasteurized milk and milk products, unwashed fresh produce, and undercooked poultry, meat, and eggs. Outbreak information from the CDC suggests that eating out also increases the risk of contracting a foodborne illness. In 2008, 52% of single-source outbreaks were linked to restaurants or delicatessens, whereas only 15% were associated with eating at home.6 The use of proton pump inhibitors and histamine-2 antagonists also have been linked to foodborne illness.7
Trends
To track foodborne illness, the CDC, the USDA Food Safety and Inspection Service, the FDA, and 10 state health departments collaboratively collect information via the Foodborne Disease Active Surveillance Network (FoodNet). FoodNet conducts active, population-based surveillance for laboratory-confirmed cases of foodborne illness isolated from the 10 participating states (California, Colorado, Connecticut, Georgia, Maryland, Minnesota, New Mexico, New York, Oregon, and Tennessee). Currently, the seven bacterial pathogens tracked through FoodNet are Salmonella, Escherichia coli (E coli), Listeria, Campylobacter, Shigella, Yersinia, and Vibrio. Live, healthy animals are the source of most of these pathogens, with the exception of Shigella (intestines of an ill host) and Vibrio (marine waters and shellfish).1
According to the CDC, the incidence of five of the seven reportable foodborne bacterial pathogens (Campylobacter, Listeria, Shiga toxin–producing E coli (STEC) O157, Shigella, and Yersinia) decreased from 1996 to 2010 (TABLE 2).1 Salmonella incidence has not changed significantly over this time period. Vibrio infections are on the rise, although the overall incidence is quite low—0.4 illnesses per 100,000 people.1
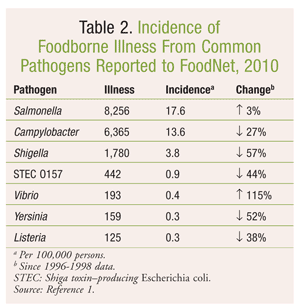
Although the incidence of foodborne illness in general does not appear to be significantly increasing, foodborne illness associated with fresh produce is on the rise.8,9 The bacterial pathogens of greatest concern are Salmonella, E coli (mainly O157:H7), and Listeria monocytogenes (L monocytogenes).8 Of these pathogens, Salmonella is the most prevalent, causing illness in 17.6 of 100,000 persons. Salmonella accounted for 2,290 hospitalizations and 29 deaths in 2010, the highest of any foodborne pathogen.1 Listeria infections increased greatly in 2011 as a result of the contaminated cantaloupe outbreak, with 30 deaths linked to that outbreak alone.10 Although the incidence of listeriosis is low (0.3 cases per 100,000 persons), the hospitalization and case-fatality rates (90% and 12.8%, respectively) are the highest of any bacterial pathogens associated with foodborne illness.1,11 The incidence of another common pathogen, E coli O157, has declined significantly in recent years, likely a result of increased prevention efforts as well as improved detection and investigation of outbreaks following the bagged spinach outbreak in 2006.1,12 The incidence of E coli O157 is now less than 1 per 100,000 persons, which meets the Healthy People 2010 goal for this organism.1 Despite this, E coli O157 is still commonly linked to outbreaks of foodborne illness involving both meat and produce and remains a significant public health threat. E coli O157 is responsible for approximately 75% of enterohemorrhagic E coli infections worldwide and has an estimated hospitalization rate of 46.2% in the U.S.11,13
Bacterial Pathogens
Salmonella: Salmonella has traditionally been linked to animal products, including poultry and eggs, although recently it has caused many foodborne illnesses involving fresh fruits and vegetables. Since 2006, Salmonella has been associated with foods such as alfalfa sprouts, tomatoes, jalapeño peppers, black pepper, papayas, cantaloupes, and various nuts.3 Salmonella is spread via the fecal-oral route, commonly through contact with contaminated water. There are two categories of salmonellosis: nontyphoidal and typhoidal (caused by Salmonella typhi or Salmonella paratyphi). Salmonella strains predominantly cause nontyphoidal salmonellosis in the U.S. Symptoms (commonly diarrhea, nausea, vomiting, abdominal cramps, headache, and fever) typically occur within 72 hours of exposure and last for 4 to 7 days. Most cases are self-limiting, and the mortality rate is less than 1%.14
Approximately 8% of patients with nontyphoidal salmonellosis will develop bacteremia and require treatment with antibiotics, including ceftriaxone or azithromycin in children and a fluoroquinolone (commonly levofloxacin) or azithromycin in adults. Patients with nontyphoidal salmonellosis and one or more risk factors for bacteremia should be given antibiotics immediately. These risk factors include age under 3 months or over 65 years, corticosteroid use, inflammatory bowel disease, immunosuppression, and hemodialysis. Antibiotics are recommended in patients with a prosthetic heart valve or abdominal aneurysm to reduce the risk of focal infection.15 Diarrheal ailments such as salmonellosis are generally treated with rehydration therapy with oral fluids (IV, if necessary), salt intake (commonly through soups and crackers), and an easily digestible diet such as “BRAT” (bananas, rice, applesauce, and toast) until symptoms resolve.15,16
E coli O157: E coli bacteria are an essential part of the intestinal flora of humans. E coli is usually harmless and, in fact, is protective to the host. However, strains of STEC, such as E coli O157, can cause serious, bloody diarrhea in the host.13 E coli O157 is predominantly associated with undercooked beef and beef products, although lately it has been more prevalent in fresh produce. In recent years, E coli O157 contamination has occurred in foods such as spinach, romaine lettuce, hazelnuts, and clover sprouts.3 Waterborne outbreaks have been linked to bodies of fresh water, swimming pools, and ice.17 After exposure, hemorrhagic colitis often results within 48 hours. Hemorrhagic colitis presents as severe abdominal cramping, nausea, vomiting, and diarrhea that changes from watery to bloody. Life-threatening complications of E coli O157 infections include hemolytic uremic syndrome (HUS) and thrombotic thrombocytopenia purpura.13 HUS, which occurs when Shiga toxin is absorbed, thereby injuring glomerular cells, results in death in 3% to 5% of cases.13,15 Antibiotic therapy is thought to increase the risk of HUS, as is the use of antimotility drugs (e.g., loperamide), which may slow the exit of the enteropathogen from the body; these therapies therefore are not recommended.15,16 Treatment should focus on rehydration and on reducing the risk of severe complications.
L monocytogenes: L monocytogenes is another pathogen that can contaminate foods and cause foodborne illness. Unlike many other pathogens, L monocytogenes can live and grow in refrigeration temperatures and salty environments.18 L monocytogenes contamination has been associated with unpasteurized milk and milk products (e.g., soft cheeses), meats (especially deli meats), hot dogs, raw produce, and seafood. The incidence of L monocytogenes contamination is low, but the fatality rate is high. Pregnant women are at greater risk for listeriosis. Although frequently the mother has mild symptoms, the risks to the fetus are severe. There is a 1-in-3 chance of spontaneous abortion or stillbirth, as well as an increased risk of bacteremia or meningitis in the neonate.19
Listeriosis usually occurs within 3 days after exposure and in less severe cases lasts from days to weeks; symptoms are consistent with a diarrheal ailment. More severe cases may last for several months and can cause complications such as septicemia and meningitis.19 The treatment of choice for complicated listeriosis is ampicillin (trimethoprim-sulfamethoxazole, in the case of penicillin allergy), with or without gentamicin, for 3 to 6 weeks.20 As with all foodborne illnesses in which diarrhea is present, rehydration therapy is vital.
Prevention
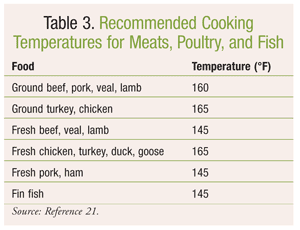
The key to reducing the incidence of foodborne illness is prevention. Proper food storage, refrigeration, handling, and cooking are vital. Patients should be educated to avoid high-risk items such as unpasteurized milk and milk products, as well as raw or undercooked items like oysters, meat, poultry, and eggs. The consumption of more meals in the home may also decrease the risk of foodborne illness.6 According to food-safety experts, two important steps should be implemented in the home to reduce the risk of foodborne illness: washing the hands thoroughly when handling food, and using a thermometer to ensure that adequate food temperatures (TABLE 3) are reached during cooking.21,22 Steps to reduce cross-contamination should also be implemented, including using a separate cutting board and utensils for raw and fresh foods and frequently disinfecting kitchen surfaces. To prevent the spread of bacteria harbored by kitchen towels and sponges, paper towels should be used to clean up cooking spills, and kitchen towels should be laundered frequently. To significantly reduce bacteria, kitchen sponges may be placed in the dishwasher for a heated cycle or microwaved while wet for 1 minute.23 Some evidence suggests that reusable shopping bags also may harbor bacteria, so separate bags should be used for fresh produce and meat. Also, washing the bags thoroughly either by hand or in the washing machine may help reduce the spread of bacteria to foods.24 Using caution to prevent the spread of bacteria is essential to the reduction of foodborne illness.
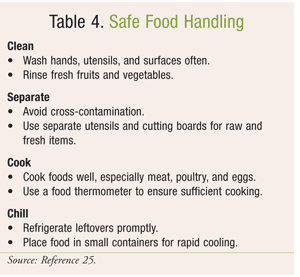
A four-step approach to improving food safety, as recommended by the Partnership for Food Safety Education (PFSE), is described in TABLE 4.25 For fresh produce, the PFSE recommends two additional steps. First, be sure that produce is not damaged or bruised and is adequately refrigerated, if precut. Additionally, throw away produce that has been compromised by bruises or improper storage or that may have been in contact with raw meat, poultry, or seafood. When it comes to the safety of fresh produce, the PFSE recommends: “If in doubt, throw it out.”26
Conclusion: Pharmacists’ Role
Pharmacists can help identify individuals who may be at high risk for foodborne illness, educate patients about how to prevent foodborne illness, make recommendations for self-care, and report incidences of foodborne illness to the local health department and the CDC. Elderly patients, those with small children, and those who are immunocompromised would benefit from education about how to prevent foodborne illness. Pregnant patients should be advised to avoid consuming foods that may be contaminated with Listeria (e.g., deli meats, undercooked meats and hot dogs, unpasteurized milk and soft cheeses, and unwashed fresh produce), particularly because of the risk of harm to the fetus. The CDC and other government agencies maintain Web sites that provide a wealth of valuable food safety information for consumers. Some examples include the PFSE (http://fightbac.org), FoodSafety.gov (http://foodsafety.gov), and Food Safety for Moms-to-Be (www.fda.gov/Food/ResourcesForYou/HealthEducators/ucm081785.htm).
To report a suspected or confirmed foodborne illness, pharmacists can visit www.cdc.gov/outbreaknet/reportillness.html or call 1-800-CDC-INFO (1-800-232-4636). Illness data are used to determine where and why outbreaks occur and may be used to inform the public of the suspected contaminated source. Not all illnesses are associated with large outbreaks; trends can occur on a smaller scale, associated with individual restaurants or foods. The tracking of foodborne illness is essential to our understanding of how these illnesses occur and how future outbreaks can be prevented.
REFERENCES
1. CDC. Vital signs: incidence and trends of infection with pathogens
transmitted commonly through food—Foodborne Diseases Active
Surveillance Network, 10 U.S. sites, 1996-2010. MMWR Morb Mortal Wkly Rep. 2011;60:749-755.
2. Nyachuba DG. Foodborne illness: is it on the rise? Nutr Rev. 2010;68:257-269.
3. CDC. Outbreak Response Team: multistate foodborne outbreaks. www.cdc.gov/outbreaknet/outbreaks.html. Accessed April 19, 2012.
4. CDC. Diagnosis and management of foodborne illnesses: a primer for physicians and other health care professionals. MMWR Recomm Rep. 2004;53:1-33.
5. Barton Behravesh C, Jones TF, Vugia DJ, et al. Deaths associated
with bacterial pathogens transmitted commonly through food: Foodborne
Diseases Active Surveillance Network (FoodNet), 1996-2005. J Infect Dis. 2011;204:263-267.
6. CDC. Surveillance for foodborne disease outbreaks—United States, 2008. MMWR Morb Mortal Wkly Rep. 2011;60:1197-1202.
7. Garcia Rodríguez LA, Ruigómez A, Panés J. Use of acid-suppressing drugs and the risk of bacterial gastroenteritis. Clin Gastroenterol Hepatol. 2007;5:1418-1423.
8. Francis GA, Gallone A, Nychas GJ, et al. Factors affecting quality and safety of fresh-cut produce. Crit Rev Food Sci Nutr. 2012;52:595-610.
9. Pui CF, Wong WC, Chai LC, et al. Salmonella: a foodborne pathogen. Int Food Res J. 2011;18:465-473.
10. CDC. Multistate outbreak of listeriosis associated with Jensen Farms cantaloupe—United States, August-September 2011. MMWR Morb Mortal Wkly Rep. 2011;60:1357-1358.
11. Scallan E, Hoekstra RM, Angulo FJ, et al. Foodborne illness acquired in the United States—major pathogens. Emerg Infect Dis. 2011;17:7-15.
12. CDC. Ongoing multistate outbreak of Escherichia coli serotype O157:H7 infections associated with consumption of fresh spinach—United States, September 2006. MMWR Morb Mortal Wkly Rep. 2006;55:1045-1046.
13. Feng P. Pathogenic Escherichia coli group. In: Lampel KA, Al-Khaldi S, Cahill SM, eds. Bad Bug Book: Foodborne Pathogenic Microorganisms and Natural Toxins Handbook.
2nd ed. Silver Spring, MD: FDA; 2012.
www.fda.gov/downloads/Food/FoodSafety/FoodborneIllness/FoodborneIllnessFoodbornePathogensNaturalToxins/BadBugBook/UCM297627.pdf.
Accessed April 9, 2012.
14. Hammack T. Salmonella species. In: Lampel KA, Al-Khaldi S, Cahill SM, eds. Bad Bug Book: Foodborne Pathogenic Microorganisms and Natural Toxins Handbook.
2nd ed. Silver Spring, MD: FDA; 2012.
www.fda.gov/downloads/Food/FoodSafety/FoodborneIllness/FoodborneIllnessFoodbornePathogensNaturalToxins/BadBugBook/UCM297627.pdf.
Accessed April 9, 2012.
15. DuPont HL. Bacterial diarrhea. N Engl J Med. 2009;361:1560-1569.
16. Thielman NM, Guerrant RL. Acute infectious diarrhea. N Engl J Med. 2004;350:38-47.
17. Pennington H. Escherichia coli O157. Lancet. 2010;376(9750):1428-1435.
18. Gandhi M, Chikindas ML. Listeria: a foodborne pathogen that knows how to survive. Int J Food Microbiol. 2007;113:1-15.
19. Cheng Y. Listeria monocytogenes. In: Lampel KA, Al-Khaldi S, Cahill SM, eds. Bad Bug Book: Foodborne Pathogenic Microorganisms and Natural Toxins Handbook.
2nd ed. Silver Spring, MD: FDA; 2012.
www.fda.gov/downloads/Food/FoodSafety/FoodborneIllness/FoodborneIllnessFoodbornePathogensNaturalToxins/BadBugBook/UCM297627.pdf.
Accessed April 9, 2012.
20. Choice of antibacterial drugs. Treat Guidel Med Lett. 2007;5:33-50.
21. Partnership for Food Safety Education. Cook: heat it up chart.
www.fightbac.org/safe-food-handling/cook/127-cook-heat-it-up-chart.
Accessed May 13, 2012.
22. Hillers VN, Medeiros L, Kendall P, et al. Consumer food-handling
behaviors associated with prevention of 13 foodborne illnesses. J Food Prot. 2003;66:1893-1899.
23. Sharma M, Eastridge J, Mudd C. Effective household disinfection methods of kitchen sponges. Food Control. 2009;20:310-313.
24. Gerba CP, Williams D, Sinclair RG. Assessment of the potential
for cross contamination of food products by reusable shopping bags.
http://uanews.org/pdfs/GerbaWilliamsSinclair_BagContamination.pdf.
Accessed May 14, 2012.
25. Partnership for Food Safety Education. Safe food handling. www.fightbac.org/safe-food-handling. Accessed April 19, 2012.
26. Partnership for Food Safety Education. Safe handling of fresh
fruits and vegetables. October 14, 2004.
www.fightbac.org/storage/documents/flyers/producebrochure-bw.pdf.
Accessed April 19, 2012.
To comment on this article, contact rdavidson@uspharmacist.com.





