US Pharm. 2012;37(4):HS8-HS10.
Crohn’s disease (CD) is a chronic, idiopathic, inflammatory disease that can affect any part of the digestive or gastrointestinal (GI) tract, from mouth to anus.1 With an increasing frequency in youths of varying ages, CD has become a significant chronic disease that affects children and adolescents. Due to some of the symptoms and complications of this disease, such as rectal bleeding, weight loss, and abdominal pain, children may experience anemia, growth failure, malnutrition, a delay in puberty, and bone demineralization, in addition to psychological issues.1-3 Consequently, the management of CD in children and adolescents involves great effort from a multidisciplinary team, ranging from a pediatrician, pediatric specialist, and surgeon to a pharmacist, nutritionist, and psychiatric support team.4
Epidemiology and Etiology
CD affects approximately 500,000 individuals in the United States.1 Although it may appear at any age, most cases are diagnosed between the ages of 20 and 30 years.5,6 Approximately 20% to 30% of cases are being diagnosed in children and adolescents younger than the age of 18 years.5 Rangasamy et al report that a greater proportion of colonic and distal CD has been diagnosed in older patients,3 whereas younger patients have predominantly ileal disease.7 The disease is also more common in Caucasians than in African Americans and rare in Asians and Hispanics, with a higher rate in males than in females.3
Although the exact etiology is unknown, causes are linked to genetic, immunologic, environmental, and infectious components.1,2 Researchers have linked mutations within the NOD2/CARD15 gene (found on chromosome 16), which limits the ability to recognize bacteria as harmful, occurring in CD patients twice as frequently as in the general population.3,8,9 Additional regions that have been linked to inflammatory bowel disease (IBD) with susceptibility to CD include the IBD-3 gene on chromosome 6, which contains the human leukocyte antigen (HLA) complex; IBD-5 on chromosome 5q; mutations in the IL23R gene; HLA-DRB1*0103; and a single nucleotide polymorphism in the ATG16L1 gene, which is involved in autophagocytosis, a constituent of the immune response targeted toward pathogen-derived proteins.3,9-11
Other implications in the pathogenesis of CD include infectious agents such as Mycobacterium paratuberculosis and Pseudomonas and Listeria species, and perinatal influences including prematurity, socioeconomic family status at birth, and higher maternal age.12-15 Several studies, such as Hugot et al,16 have investigated birth order and CD risk and report that among families with multiple cases in offspring, affected cases are closer in birth order than may be expected by chance. First-born rather than second-born twins have been reported to be at higher risk, but no association between birth order and CD risk was found in other studies.17-19 Stress and a diet high in fatty foods have also been associated with an increased risk.6,20
Pathophysiology, Clinical Features, and Diagnosis
CD and ulcerative colitis (UC) are the major types of IBD. UC attacks the large intestine, whereas CD can occur anywhere in the digestive tract. In both conditions, symptoms can become exacerbated or flare up and at other moments stay in remission.6
There are implications that CD involves a dysfunctional immune system with chronic inflammation and tissue injury, characterized by a helper lymphocyte type 1 (Th-1) cellular immune response pattern that leads to the production of cytokines, such as interleukin (IL)-12, tumor necrosis factor (TNF)-alpha, and interferon gamma (IFN)-gamma.3,21 Knutson et al state that an imbalance in the local mucosal production of pro-inflammatory cytokines over anti-inflammatory cytokines is theorized to cause the well-demarcated, discontinuous, transmural, ulcerative lesions characteristic of the disease.1
Disease location can involve the terminal ileum only, colon only, or, in some cases, both ileum and colon.22 The most common presenting symptoms of CD among children and adolescents include abdominal pain, weight loss, diarrhea, rectal bleeding, growth failure, and extra-intestinal complications, such as arthritis, arthralgia, uveitis, erythema nodosum, and kidney stones.3,5,6 TABLE 1 lists clinical features of CD.1,3,22,23 Nutrient deficiencies, such as of zinc and vitamins A, D, and B12, have been associated with the disease, with predisposition to vitamin D deficiency leading to osteopenia.5

Oral and perianal lesions are also common. In a study conducted by Markowitz et al, it was reported that 29% of children and adolescents with CD had significant perianal pathology, ranging from small skin tags or anal fissures to more severe abscesses and fistulae.24 In a prospective study by Harty et al, 48 of 49 children with suspected IBD and a final diagnosis of CD were examined by a dentist.25 Oral manifestations of the disease were detected in 20 children (42%) and included mucogingivitis, mucosal tags, deep ulceration, cobblestoning, lip swelling, and pyostomatitis vegetans. Further studies conducted by Kanof et al showed that approximately 50% of children with untreated CD had short stature or evidence of diminished height velocity, accompanied by delayed sexual maturation.26
Management: Pharmacologic Therapy
There are several therapeutic agents used in managing CD, but selecting an appropriate drug therapy depends on the location of the disease, severity, and identification of complications. In providing therapeutic interventions, consider utilizing the Pediatric Crohn’s Disease Activity Index (PCDAI), which summarizes a patient’s disease activity based upon components of the physical examination, laboratory values, and symptoms, such as abdominal pain, the number of stools per day, and the general well-being of the patient.6,4,27 The main goal of treatment is minimizing the severity of flares, inducing and maintaining remission, and preventing complications.6,28 Grossman et al state that drug, biological, and nutritional therapies are the fundamentals of treatment, but drug therapy, especially dose adjustment and schedule, must be tailored for each individual child.6 However, there are few formulations available, and data on optimal dosing specifically for children and adolescents are lacking.4,6
5-Aminosalicylic Acid (5-ASA) Derivatives: 5-ASAs are typically used as maintenance therapy to treat mild-to-moderate symptoms, but they tend to have anti-inflammatory properties, inhibiting the synthesis of prostaglandins and leukotrienes.4,6,8 Currently available options include mesalamine, balsalazide, sulfasalazine, and olsalazine. Although 5-ASAs have proven efficacy in the treatment of mild-to-moderate UC, their role in children and adolescents with CD has not been established.4 Enema and suppository forms are available for children with disease of the lower colon and rectum,6 and sulfasalazine and olsalazine can be compounded into a suspension.4 Side effects of this class include diarrhea, headache, abdominal pain, and dizziness.
Antibiotics: Ciprofloxacin and metronidazole are helpful in some children with mild-to-moderate disease, especially those with disease of the lower colon, rectum, and/or anus.6 Although not FDA approved for the treatment of CD, ciprofloxacin and metronidazole may change the intestinal flora and have a potential effect on the immune system.3 Some side effects of metronidazole include metallic taste, peripheral neuropathy, headache, nausea, and bacterial infections.29 Primary side effects of ciprofloxacin include nausea, diarrhea, abnormal liver function tests, rash, and vomiting.30
Corticosteroids: These agents are primarily used for active moderate-to-severe cases of CD. In children, these therapeutic agents, such as prednisone, budesonide, methylprednisolone, and hydrocortisone (rectal enema), can be typically given over a short period to control a severe flare, whereas long-term use is observed in children and adolescents with “steroid-dependence.”6 However, these drugs have significant short-term and long-term side effects.8 The dose of budesonide in adults for the treatment of active CD is 9 mg/day and 6 mg orally once daily up to 3 months for maintenance of remission. In a retrospective study, Levine et al reported that 62 children used oral budesonide for the treatment of mild-to-moderate CD in doses of 0.45 mg/kg/day (maximum dose of 9 mg/day) with a 48% remission response.31
Immunosuppressants: Immunosuppressants are usually not the first choice of treatment, but are preferred to steroids in children and teens with moderate or severe disease.6 These medications are used to treat steroid-dependent disease or steroid-refractory disease and to maintain remission and reduce symptoms.3 Bousvaros et al state that approximately 70% to 80% of corticosteroid-dependent patients treated with the immunosuppressants azathioprine or 6-mercaptopurine (6-MP) will enter remission.4 A maximal effect may be achieved within 2 to 4 months of taking the medication. The oral dose in adolescents for 6-MP is 1.5 mg/kg/day at a maximum dose of 75 mg/day. However, a study conducted by Grossman et al suggests that children less than 6 years of age may require higher than standard doses to achieve clinical remission.32 Toxicities of these drugs include myelosuppression, infections, pancreatitis, and elevated aminotransferases.33 Methotrexate at a dosage of 25 mg/week IM has been used in adults with CD,34 but there are no data regarding its use in pediatrics.
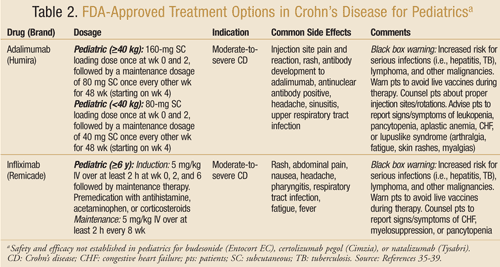
Biological Therapies: There are several FDA-approved biologics used to treat active CD and fistulae. Infliximab by infusion and adalimumab, both FDA approved, are indicated for children and adolescents with moderate-to-severe active disease who are refractory to conventional therapy (TABLE 2).35,36 Adalimumab is administered by injection every other week.8 Natalizumab, a recombinant monoclonal antibody, has been FDA approved in adults for moderate-to-severe disease, but efficacy and safety have not been established in pediatrics.37 Certolizumab pegol, an anti-TNF-alpha antibody, is also FDA approved for adult patients with CD. The recommended maintenance dosage is 400 mg subcutaneously once every 4 weeks. Common adverse effects include arthralgia, urinary tract infection, and upper respiratory tract infection.38
Management: Nonpharmacologic Therapy
Nutritional therapy and psychological support are also vital in the management of CD. Children who receive suitable medical treatment and adequate nutrition often experience dramatic reversal of symptoms and increased growth. It is recommended that parents consult a nutritionist for meeting the child’s nutritional needs. A well-balanced diet is ideal but should be tailored based upon the child’s symptoms, nutritional deficiencies, and disease pattern. Additionally, the involvement of support groups for the entire family is important in coping with the disease.
Surgery is reserved primarily for patients unresponsive to medications or those suffering with complications requiring surgical intervention.4,6,8 Grossman et al state that “surgery usually is considered when medical therapy has failed.”6 In such cases, growth failure, obstruction, abscess, fistula, hemorrhage, and perforation are all indications for surgery. According to Bousvaros et al, surgery may usually involve resection of the diseased bowel segment, stricturoplasty (widening a strictured segment of the intestine that involves incision and closure in opposing directions), and primary end-to-end anastomosis.4 Full colonic resection and end-ileostomy may be unavoidable in patients with extensive CD. Ultimately, the goal of surgery is to resect the least amount of the bowel and provide rapid improvement in an ill patient and catch-up growth and puberty in a child or adolescent.4
Conclusion
Although there is no cure for CD, most children with the illness are able to lead productive lives.8 It is important for patients to have an understanding of the disease, its symptoms and complications, the appropriate use of medications, self-monitoring, and the support from a multidisciplinary team, including pharmacists, physicians, family, and other health care providers.
REFERENCES
1. Knutson D, Greenberg G, Cronau H. Management of Crohn’s disease—a practical approach. Am Fam Physician. 2003;68:707-714, 717-718.
2. Lichtenstein G, Hanauer S, Sandborn W; the Practice
Parameters Committee of the American College of Gastroenterology.
Management of Crohn’s disease in adults. Am J Gastroenterol. 2009;104:465-483.
3. Rangasamy P, Chen Y, Coash M, et al. Crohn disease. Medscape. http://emedicine.medscape.com/article/172940-overview. Accessed September 3, 2011.
4. Bousvaros A, Leichtner A. Overview of the management of Crohn’s disease in children and adolescents. UpToDate [online database]. www.uptodate.com. Accessed August 30, 2011.
5. Bousvaros A, Burpee T, Leichtner A. Clinical manifestations of Crohn’s disease in children and adolescents. UpToDate [online database]. www.uptodate.com. Accessed September 23, 2011.
6. Grossman AB, Mamula P. Crohn’s disease in children and teens. WebMD. www.emedicinehealth.com/crohn_disease_in_children_and_teens/article_em.htm. Accessed November 20, 2011.
7. Kornbluth A, Sachar DB, Salomon P. Crohn’s disease. In: Feldman M, Scharschmidt BF, Sleisenger MH, eds. Sleisenger & Fordtran’s Gastrointestinal and Liver Disease: Pathophysiology, Diagnosis, and Management. Vol 2. 6th ed. Philadelphia, PA: WB Saunders Co; 1998:1708-1734.
8. About Crohn’s disease. Crohn’s and Colitis Foundation of America. www.ccfa.org. Accessed October 7, 2011.
9. Ahmad T, Armuzzi A, Neville M, et al. The contribution
of human leucocyte antigen complex genes to disease phenotype in
ulcerative colitis. Tissue Antigens. 2003;62:527-535.
10. James L, Lyons P, McKinney E, et al. Gene expression
profiling of CD8+ T cells predicts prognosis in patients with Crohn
disease and ulcerative colitis. J Clin Invest. 2011;121:4170-4179.
11. Thoreson R, Cullen JJ. Pathophysiology of inflammatory bowel disease: an overview. Surg Clin North Am. 2007;87:575-585.
12. Pansonby A, Catto-Smith A, Pezic A, et al. Association
between early-life factors and risk of child-onset Crohn’s disease
among Victorian children born 1983–1998: a birth cohort study. Inflamm Bowel Dis. 2009;15:858-866.
13. Sonntag B, Stolze B, Heinecke A, et al. Preterm birth
but not mode of delivery is associated with an increased risk of
developing inflammatory bowel disease later in life. Inflamm Bowel Dis. 2007;13:1385-1390.
14. Blanchard JF, Bernstein CN, Wajda A, et al. Small-area
variations and sociodemographic correlates for the incidence of Crohn’s
disease and ulcerative colitis. Am J Epidemiol. 2001;154:328-335.
15. Montgomery SM, Wakefield AJ, Ekbom A. Sex-specific risks for pediatric onset among patients with Crohn’s disease. Clin Gastroenterol Hepatol. 2003;1:303-309.
16. Hugot JP, Cezard JP, Colombel JF, et al. Clustering of Crohn’s disease within affected sibships. Eur J Hum Genet. 2003;11:179-184.
17. Spehlmann ME, Begun AZ, Burghardt J, et al.
Epidemiology of inflammatory bowel disease in a German twin cohort:
results of a nationwide study. Inflamm Bowel Dis. 2008;14:968-976.
18. Thompson NP, Montgomery SM, Wadsworth ME, et al. Early
determinants of inflammatory bowel disease: use of two national
longitudinal birth cohorts. Eur J
Gastroenterol Hepatol.
2000;12:25-30.
19. Rigas A, Rigas B, Glassman M, et al. Breast-feeding
and maternal smoking in the etiology of Crohn’s disease and ulcerative
colitis in childhood. Ann Epidemiol. 1993;3:387-392.
20. D’Souza S, Levy E, Mack D, et al. Dietary patterns and risk for Crohn’s disease in children. Inflamm Bowel Dis. 2008;14:367-373.
21. Wall GC, Heyneman C, Pfanner TP. Medical options for
treating Crohn’s disease in adults: focus on antitumor necrosis
factor-alpha chimeric monoclonal antibody. Pharmacotherapy. 1999;19:1138-1152.
22. Silverberg MS, Satsangi J, Ahmad T, et al. Toward an
integrated clinical, molecular and serological classification of
inflammatory bowel disease: report of a working party of the 2005
Montreal World Congress of Gastroenterology. Can J Gastroenterol. 2005;19(suppl A):5-36.
23. Hanauer SB, Sandborn W. Management of Crohn’s disease in adults. Am J Gastroenterol. 2001;96:635-643.
24. Markowitz J, Grancher K, Rosa J, et al. Highly destructive perianal disease in children with Crohn’s disease. J Pediatr Gastroenterol Nutr. 1995;21:149-153.
25. Harty S, Fleming P, Rowland M, et al. A prospective study of the oral manifestations of Crohn’s disease. Clin Gastroenterol Hepatol. 2005;3:886-891.
26. Kanof ME, Lake AM, Bayless TM. Decreased height
velocity in children and adolescents before the diagnosis of Crohn’s
disease. Gastroenterology. 1988;95:1523-1527.
27. Hyams J, Markowitz J, Otley A, et al. Evaluation of
the pediatric Crohn disease activity index: a prospective multicenter
experience. J Pediatr Gastroenterol Nutr. 2005;41:416-421.
28. Akobeng AK. Crohn’s disease: current treatment options. Arch Dis Child. 2008;93:787-792.
29. Flagyl (metronidazole) package insert. New York, NY: GD Searle, LLC; April 2010.
30. Cipro (ciprofloxacin) package insert. Kenilworth, NJ: Schering-Plough; October 2008.
31. Levine A, Broide E, Stein M, et al. Evaluation of oral
budesonide for treatment of mild and moderate exacerbations of Crohn’s
disease in children. J Pediatr. 2002;140:75-80.
32. Grossman AB, Noble AJ, Mamula P, Baldassano RN.
Increased dosing requirements for 6-mercaptopurine and azathioprine in
inflammatory bowel disease patients six years and younger. Inflamm Bowel Dis. 2008;14:750-755.
33. Kirschner BS. Safety of azathioprine and 6-mercaptopurine in pediatric patients with inflammatory bowel disease. Gastroenterology. 1998;115:813-821.
34. Feagan BG, Rochon J, Fedorak RN, et al: Methotrexate for the treatment of Crohn’s disease. N Engl J Med. 1995;332:292-297.
35. Humira (adalimumab) product information. North Chicago, IL: Abbott Laboratories; 2008.
36. Remicade (infliximab) package insert. Horsham, PA: Janssen Biotech, Inc; 2011.
37. Tysabri (natalizumab) product information. Cambridge, MA: Biogen Idec, Inc; 2008.
38. Cimzia (certolizumab pegol) product information. Smyrna, GA: UCB Inc; 2009.
39. Entocort EC (budesonide) product information. San Diego, CA: Prometheus Laboratories, Inc; 2011.
To comment on this article, contact rdavidson@uspharmacist.com.





