US Pharm. 2014;39(4):75-79.
ABSTRACT: Hepatitis C is a common cause of end-stage liver disease in the United States. Historically, standard treatment for hepatitis C virus (HCV) genotype 1 was peginterferon alfa plus ribavirin. Treatment remained unchanged until 2011, when the direct-acting antivirals (DAAs) boceprevir and telaprevir were approved by the FDA. Standard treatment of HCV genotype 1 now consists of peginterferon alfa, ribavirin, and a DAA. The addition of a DAA to standard treatment helped shorten the duration of therapy, but the initially approved agents were not without adverse effects (AEs). In late 2013, two additional DAAs—simeprevir and sofosbuvir—were approved by the FDA. Both of these agents feature improved dosing-frequency and AE profiles.
One of the most common causes of hepatitis is hepatitis C virus (HCV) infection. In the United States, 3.2 million people have chronic HCV infection, which is the most common blood-borne infection.1 The prevalence of hepatitis C is 3.25% in persons born between 1945 and 1965, and 50% to 75% of these individuals are unaware that they have hepatitis C.2 This population constitutes three-fourths of all chronic HCV infections among U.S. adults.2 In 2011, there were 1,229 reported cases of acute HCV infection—a 44% increase from 2010.3 In the U.S., chronic HCV infection is the most common reason for liver transplantation. Five percent to 20% of HCV-infected individuals develop cirrhosis over a period of 20 to 30 years, and 1% to 5% die of cirrhosis or liver cancer.1
HCV is classified into six different genotypes (numbered 1-6), with each genotype divided into subtypes. HCV genotype 1, which is the most common cause of hepatitis C infection in the U.S., is the most difficult form to treat.4
Clinical Presentation
Hepatitis C is classified into two phases: acute infection (<6 months) and chronic infection (>6 months). About 70% of acute hepatitis cases evolve into chronic hepatitis.5 It takes 2 to 26 weeks after HCV exposure for acute hepatitis to develop.6 Although most people infected with HCV are asymptomatic, approximately 20% to 30% of newly infected individuals experience fatigue, abdominal pain, poor appetite, or jaundice.1 Since most patients are asymptomatic, they do not seek treatment, and the infection becomes chronic. Chronic HCV infection can result in severe liver damage, and patients may experience symptoms associated with liver failure (e.g., jaundice, dark urine, pale stools, chronic fatigue).
Diagnosis
Although most people with acute HCV infection are asymptomatic and therefore do not undergo testing, there are specific populations that should be routinely tested. The CDC recommends routine testing of individuals at high risk for HCV infection, including IV drug users, patients who received a blood transfusion or organ transplant before July 1992, those undergoing long-term hemodialysis, those with HIV, and children born to mothers with HCV infection. In August 2012, the CDC updated its routine-testing recommendations to include persons born between 1945 and 1965.7
There are a number of tests that can either definitively diagnose or help diagnose HCV infection. The testing sequence recommended by the CDC begins with a rapid or laboratory assay (i.e., enzyme-linked immunosorbent assay, OraQuick HCV Rapid Antibody Test) that detects HCV antibodies.8 These tests, however, fail to distinguish between active infection and past infection. If either test yields a positive result, then HCV RNA (viral load) testing should be performed.8 The HCV RNA test uses polymerase chain reaction or branched DNA assays to detect HCV RNA in the serum. The aforementioned tests may be used to detect the presence of active HCV infection, determine the HCV genotype, and assist in predicting response to interferon therapy. A liver biopsy may be performed to confirm HCV infection and determine disease severity. Liver enzymes are a marker of hepatic injury, but are not a definitive indicator of HCV infection. Treatment may be considered in patients meeting the criteria outlined in these tests.
Treatment
Until recently, HCV genotype 1 infection was thought to be incurable; however, medications have since been discovered that can treat and possibly cure this disease.9 Previously, treatment of HCV genotype 1 consisted solely of pegylated interferon (PEG-IFN) and ribavirin (TABLE 1). Since 2011, four direct-acting antivirals (DAAs) have been FDA-approved for chronic infection caused by HCV genotype 1: boceprevir (Victrelis), telaprevir (Incivek), simeprevir (Olysio), and sofosbuvir (Sovaldi) (TABLE 2). These drugs greatly improve treatment response in patients with genotype 1. Boceprevir, telaprevir, and simeprevir act by inhibiting HCV NS3/4A protease. This protease is responsible for proteolytic cleavage of the HCV-encoded polyprotein into mature forms; without it, the virus is unable to replicate.10-12 Sofosbuvir is an HCV nucleotide analogue NS5B polymerase inhibitor that prevents HCV from replicating.13
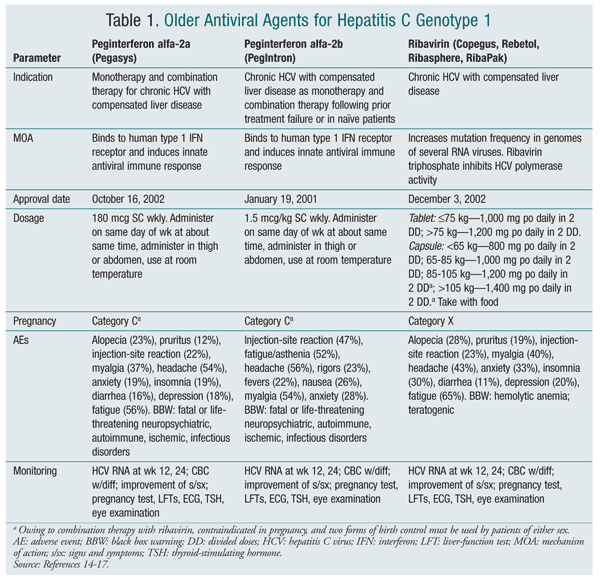
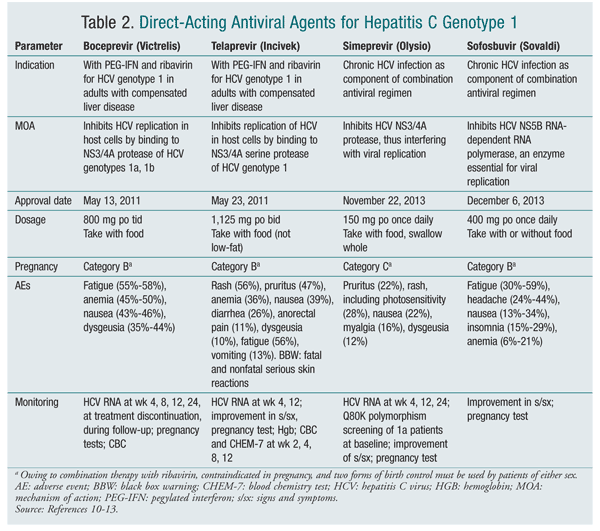
PEG-IFN and weight-based ribavirin are indicated to treat HCV infections caused by all genotypes.14,15 Addition of one of the new DAAs is determined by the genotype. Boceprevir, telaprevir, and simeprevir are indicated to treat only hepatitis C infection caused by HCV genotype 1.10-12 Sofosbuvir is indicated for treatment of genotypes 1 through 4.13
PEG-IFN: PEG-IFN is available in two forms: Pegasys (peginterferon alfa-2a) and PegIntron (peginterferon alfa-2b). These agents are synthetic versions of human proteins that enhance immune response. Pegasys and PegIntron are dosed once weekly and injected SC. The major difference between the two is that Pegasys is a fixed dose (180 mcg), whereas PegIntron is weight-based (1.5 mcg/kg).14,15 Each agent carries a black box warning stating that the drug may cause or aggravate fatal or life-threatening neuropsychiatric, autoimmune, ischemic, and infectious disorders.14,15 Headache, injection-site reactions, fatigue, nausea, vomiting, diarrhea, and insomnia also may occur.14,15
Ribavirin: Ribavirin, an antiviral agent whose mechanism of action is unknown, is given together with PEG-IFN to treat HCV infection. It is dosed at 800 mg to 1,200 mg per day, depending upon body weight. Ribavirin is contraindicated during pregnancy, as well as in male partners of pregnant women.16,17 Ribavirin is known to cause teratogenic effects in animals. Its primary toxicity is hemolytic anemia, which can worsen cardiac disease and cause myocardial infarction.16,17 Ribavirin is also associated with headache, fatigue, muscle pain, nausea, chills, fever, and insomnia.16,17
New Antivirals: Boceprevir, telaprevir, simeprevir, and sofosbuvir are used in conjunction with peginterferon alfa and ribavirin to enhance suppression of HCV genotype 1 viral replication and ultimately cure the host of the virus.10-13 Boceprevir is dosed at 800 mg every 7 to 9 hours and initiated after completion of 4-week treatment with peginterferon alfa and ribavirin.10 Boceprevir can cause fatigue, nausea, vomiting, diarrhea, anemia, taste disturbances, and headache.10
Telaprevir, which is dosed at 1,125 mg twice daily (10-14 hours apart) with meals (not low-fat), is given in combination with peginterferon alfa and ribavirin (triple therapy) for 12 weeks.11 After the initial triple therapy, the patient continues treatment with peginterferon alfa and ribavirin. Fatal and nonfatal serious skin reactions, including Stevens-Johnson syndrome, drug reaction with eosinophilia and systemic symptoms, and toxic epidermal necrolysis have been reported in patients receiving telaprevir combination therapy.11 Adverse effects (AEs) of telaprevir include anemia, rash, nausea, vomiting, diarrhea, fatigue, taste changes, and anal or rectal itching.11
Simeprevir, like telaprevir, is given in combination with peginterferon alfa and ribavirin for 12 weeks, after which treatment consists of peginterferon alfa and ribavirin alone. Simeprevir is dosed at 150 mg daily.12 The efficacy of simeprevir combination therapy is substantially reduced in patients infected with HCV genotype 1a with an NS3 Q80K polymorphism. Therefore, Q80K polymorphism screening is strongly recommended for patients with HCV genotype 1a infection, and alternative therapy should be considered if a polymorphism is found.12 Commonly reported AEs of simeprevir were rash, nausea, muscle pain, and pruritus.12
For the treatment of HCV genotype 1 infection, sofosbuvir is dosed at 400 mg once daily and given in combination with peginterferon alfa and ribavirin for 12 weeks. AEs of sofosbuvir include fatigue, headache, nausea, insomnia, and anemia.13
Duration of Therapy: Treatment duration is based on many factors, such as whether the patient is treatment-naïve, the extent of liver damage, and the patient’s response to treatment. Treatment response is defined by the amount of, lack of, or reduction of HCV RNA in the infected individual. Rapid virologic response is an undetectable HCV RNA test at treatment week 4.4 Early virologic response is a ≥2 log decrease in HCV RNA from baseline.4 End-of-treatment response is an undetectable HCV RNA test at the end of treatment week 24 or 48.4 Sustained virologic response (SVR) is an undetectable HCV RNA test at 24 weeks after treatment completion.4 See TABLE 3 for more detailed definitions.

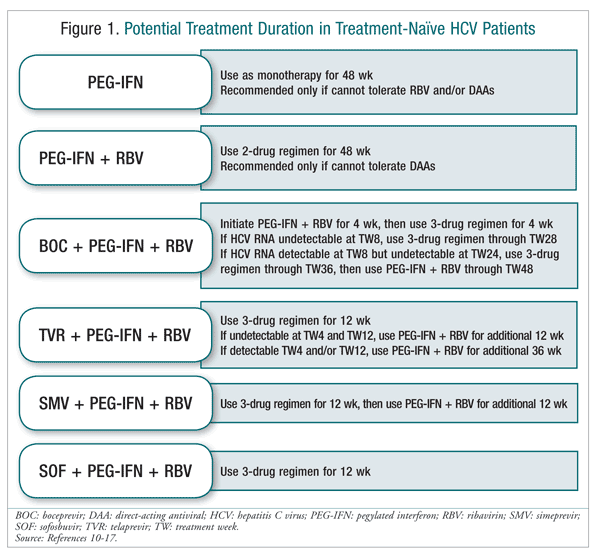
On January 29, 2014, new HCV guidelines were released. The recommended therapy for a patient monoinfected with HCV genotype 1 is sofosbuvir plus peginterferon alfa and ribavirin.18 See FIGURE 1 for alternative treatment and duration options for patients who are monoinfected with HCV genotype 1 and treatment-naïve, without cirrhosis of the liver.
Conclusion
The treatment of HCV genotype 1 is ever-evolving. Improvements in treatment have led to better outcomes in this population. With new treatment options, patients monoinfected with HCV genotype 1 can possibly clear the virus from their systems and ultimately be cured. Although this article focused only on the treatment of patients monoinfected with HCV genotype 1, other medications are being developed to improve outcomes in patients infected with other genotypes. At this writing, other DAAs are awaiting FDA approval.
REFERENCES
1. CDC. Hepatitis C information for health professionals. www.cdc.gov/hepatitis/HCV/HCVfaq.htm. Accessed March 14, 2014.
2. Smith BD, Patel N, Beckett GA, Ward JW. Hepatitis C virus antibody
prevalence, correlates and predictors among persons born from 1945
through 1965, United States, 1999-2008. Hepatology. 2011;54(suppl):554A-555A.
3. CDC. Surveillance for viral hepatitis—United States, 2011.
www.cdc.gov/hepatitis/Statistics/2011Surveillance/Commentary.htm#hepC.
Accessed March 14, 2014.
4. Ghany MG, Strader DB, Thomas DL, Seeff LB. Diagnosis, management, and treatment of hepatitis C: an update. Hepatology. 2009;49:1335-1374.
5. Dhawan VK. Hepatitis C clinical presentation. Medscape. http://emedicine.medscape.com/article/177792-clinical. Accessed March 14, 2014.
6. Marcellin P. Hepatitis C: the clinical spectrum of the disease. J Hepatol. 1999;31(suppl 1):9-16.
7. CDC. Testing recommendations for chronic hepatitis C virus
infection. www.cdc.gov/hepatitis/hcv/guidelinesc.htm. Accessed March 14,
2014.
8. CDC. Testing for HCV infection: an update of guidance for clinicians and laboratorians. MMWR Morb Mortal Wkly Rep. 2013;62:362-365.
9. Cheinquer H. Treatment of chronic hepatitis C virus infection in the near future. Ann Hepatol. 2013;12:854-859.
10. Victrelis (boceprevir) product information. Whitehouse Station, NJ: Merck Sharp & Dohme Corp; February 2014.
11. Incivek (telaprevir) product information. Cambridge, MA: Vertex Pharmaceuticals Inc; October 2013.
12. Olysio (simeprevir) product information. Titusville, NJ: Janssen Therapeutics; November 2013.
13. Sovaldi (sofosbuvir) product information. Foster City, CA: Gilead Sciences, Inc; December 2013.
14. Pegasys (peginterferon alfa-2a) product information. South San Francisco, CA: Genentech USA, Inc; July 2013.
15. PegIntron (peginterferon alfa-2b) product information. Whitehouse Station, NJ: Schering Corp; December 2013.
16. Copegus (ribavirin) product information. South San Francisco, CA: Genentech USA, Inc; February 2013.
17. Rebetol (ribavirin) product information. Whitehouse Station, NJ: Merck Sharp & Dohme; November 2013.
18. American Association for the Study of Liver Diseases (AASLD) and
Infectious Diseases Society of America. Recommendations for testing,
managing, and treating hepatitis C.
www.hcvguidelines.org/full-report/initial-treatment-box-summary-recommendations-patients-who-are-initiating-therapy-hcv.
Accessed March 14, 2014.
To comment on this article, contact rdavidson@uspharmacist.com.





