US Pharm. 2014;39(11):HS8-HS15.
ABSTRACT: Many nonpsychiatric medications can cause neuropsychiatric effects, which range from anxiety to psychosis. Drug-induced psychosis was first diagnosed in the 19th century. Since then, many medications have been associated with this phenomenon. The most commonly implicated nonpsychiatric agents include antiparkinsonian agents, cardiac medications, and corticosteroids. Pharmacists must be familiar with the neuropsychiatric adverse effects of many common prescription and nonprescription medications so that they can educate patients and caregivers about this potential adverse effect and develop strategies to minimize risk.
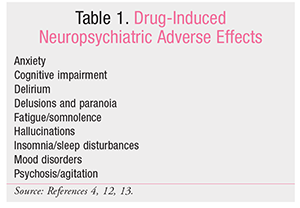
Adverse drug events (ADEs) affect millions of people each year. ADEs have been identified as the most common cause of postdischarge complications and account for more than 3.5 million physician office visits, approximately 1 million emergency department visits, and almost 125,000 hospital admissions annually.1-3 Neuropsychiatric effects constitute up to 30% of ADEs and are associated with considerable morbidity and mortality.4,5 Many nonpsychiatric medications have the potential to cause neuropsychiatric events ranging from anxiety to psychosis (TABLE 1). This article will review some of the common nonpsychiatric agents associated with medication-induced psychosis and discuss strategies for minimizing a patient’s risk.
Background
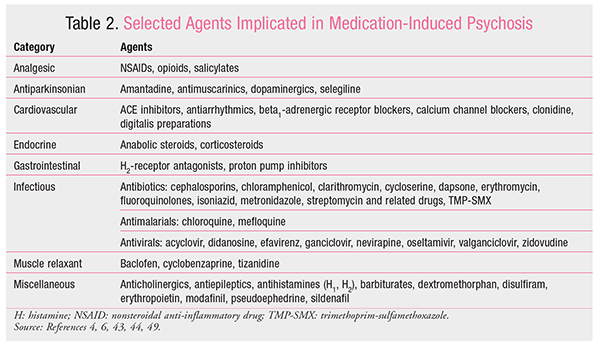
The term psychosis was first used in the 19th century to describe an abnormal state of mind.6 Today, psychosis represents a disturbance in the perception of reality. Psychosis is marked by the presence of one or more of the following symptoms: hallucinations, delusions, disorganized thoughts, and unusual, strange, and/or regressed behavior. The phenomenon now known as medication-induced psychosis was first identified in 1845 by the French psychiatrist Jacques-Joseph Moreau, who described the effects of smoking hashish in his patients as “…acute psychotic reactions, generally lasting but a few hours, but occasionally as long as a week; the reaction seemed dose-related and its main feature included paranoid ideation, illusions, hallucinations, delusions, depersonalization, confusion, restlessness and excitement.”7 Since then, many agents have been associated with medication-induced psychosis (TABLE 2).
The prevalence of medication-induced psychosis is unknown, but it is estimated that in 7% to 25% of individuals presenting with a first episode of psychosis, the condition may be substance- or medication-induced.8 The Diagnostic and Statistical Manual of Mental Health Disorders, Fifth Edition, lists a number of criteria for the diagnosis of substance- or medication-induced psychotic disorder: hallucinations and/or delusions are present; symptoms developed during or soon after substance intoxication or withdrawal, or after exposure to a medication; the involved medication is capable of producing these symptoms; the disturbance is not better explained by a psychotic disorder that is not substance- or medication-induced; the disturbance does not occur exclusively during the course of a delirium; and the disturbance causes significant distress or impairment in social, occupational, or other important areas of functioning.8 The most commonly implicated nonpsychiatric medications associated with medication-induced psychosis are antiparkinsonian agents, cardiac medications, and corticosteroids.5,6
Antiparkinsonian Agents
It is rare for psychotic symptoms to occur in untreated Parkinson’s disease (PD) patients (<10%); these symptoms usually develop as a complication of drug therapy.9 Antiparkinsonian agents are associated with the highest risk of medication-induced psychosis, with symptoms developing in up to 60% of patients.10,11 Owing to their catecholaminergic or anticholinergic properties, all antiparkinsonian medications have the potential to induce psychosis.12 Symptoms range from abnormal dreams to frank psychosis. Visual hallucinations with or without delirium are most frequently reported; auditory hallucinations, which are less common, are usually accompanied by visual hallucinations.13-17 Delusions—fixed beliefs that are unswayed by clear or reasonable contradictory evidence and are held with great conviction—are less common than hallucinations.8,18,19 In PD, delusions are often paranoid in nature, usually follow hallucinations, and affect up to 14% of patients.20 Sleep disturbances and abnormal dream phenomena may precede the development of psychosis in PD patients.4,17
Cardiac Agents
Digoxin has the potential to cause delirium, depression, and psychosis, most likely due to electrolyte imbalances and cerebral hypoxia.4,21 These effects are dose-dependent but may be seen at therapeutic levels, especially in elderly patients or in cases when digoxin is used in combination with diuretics that cause potassium loss.4,21 The risk of developing psychotic symptoms increases when the plasma digoxin concentration exceeds 1.5 ng/mL.4 Psychotic symptoms may be the first and only sign of digoxin toxicity, especially when the serum concentration is in the normal range.
Beta1-adrenergic receptor blockers are known to cause central nervous system (CNS) effects, including bizarre or vivid dreams, sleep disturbances, delirium, psychosis, and visual hallucinations.22 Psychosis and delirium have been reported for metoprolol and propranolol.4,23,24 These effects are not dose-dependent and appear to be partly due to the medications’ lipophilic properties: Hydrophilic agents such as atenolol are excreted unchanged by the kidneys, whereas lipophilic agents such as propranolol and metoprolol are metabolized by the liver and are believed to cross the blood-brain barrier.22,23 Other factors affecting beta-blockers’ penetration of the blood-brain barrier and their ability to cause CNS effects include specific structural details of the molecules, drug-induced increases in plasma catecholamine levels, and decreased melatonin levels.25
Neuropsychiatric effects of ACE inhibitors are limited; however, visual hallucinations associated with use of these agents have been reported, primarily in elderly patients.26,27 Implicated agents include quinapril, enalapril, captopril, lisinopril, ramipril, and perindopril.12,26,27 Hallucination onset occurred 2 hours to 6 years after initiation of an ACE inhibitor and resolved within 1 to 30 days after discontinuation.27 Advancing age and underlying CNS disorders may be risk factors for ACE inhibitor–induced psychosis.27
Other cardiac agents that may induce psychosis include diuretics, calcium channel blockers, and several antiarrhythmic agents.4,27
Corticosteroids
Since the 1950s, corticosteroids have been utilized for the treatment of a variety of immunologic disorders. The reported incidence of corticosteroid-associated psychiatric reactions ranges from 1.8% to 57%; psychosis related to corticosteroid treatment has an incidence of 3% to 13.9%.28-30 The substantial variability in reported incidences reflects the unpredictability of these reactions, differences in dosing, varying treatment durations, and a host of identified risk factors.28,30 Emotional lability and irritability, sometimes accompanied by auditory hallucinations and paranoia, are common symptoms experienced by patients receiving corticosteroids.30 These effects are dose-related, with psychotic reactions more likely to occur in patients receiving dosages of prednisone exceeding 40 mg/day, but even low levels of systemic exposure from inhaled corticosteroids can potentially induce psychiatric adverse effects.4,28,31 The mechanism by which corticosteroids induce psychiatric symptoms such as psychosis and mania remains to be elucidated.
Other Medications
Antimicrobials: Antibiotics are frequently used and are generally well tolerated, but some antibiotics have been associated with neuropsychiatric adverse effects that are usually less recognized.32 Fluoroquinolones, particularly ciprofloxacin, have been reported to cause mania, delirium, and hallucinations in 0.9% to 11% of patients.33,34
A few case reports have linked amoxicillin to the development of acute psychosis. Symptoms developed within 2 hours to 10 days after therapy initiation and resolved completely upon cessation.35 Clarithromycin, a macrolide antibiotic, has been associated with bad dreams, confusion, disorientation, and hallucinations in 3% of patients.36 Trimethoprim-sulfamethoxazole (TMP-SMX) has been associated with the development of psychosis.32 In one review, 11.9% of HIV-infected patients receiving TMP-SMX for Pneumocystis jirovecii pneumonia developed acute psychosis.37 In other reports, initiation of TMP-SMX led to altered mental status involving vivid visual and auditory hallucinations, with improvement of symptoms upon discontinuation.38 Paranoid-hallucinatory psychosis has been reported with chloramphenicol, streptomycin, cephalosporins, and some antituberculous drugs, such as cycloserine.4,39
Antiretrovirals: The prevalence of new-onset psychosis in HIV-infected patients ranges from 0.5% to 15%.40 Antiretroviral therapy (ART), which is a mainstay of HIV treatment, may be a contributing factor.12,40 ART initiation may be associated with onset of psychotic symptoms within 1 month of initiation; resolution of symptoms frequently occurs following discontinuation of the offending agent.40 The most commonly cited agents are efavirenz, zidovudine, abacavir, nevirapine, and combivir.40
Nonprescription Medications: Many nonprescription medications can cause psychotic symptoms. Sympathomimetics in most cold products and nasal sprays have been associated with psychotic symptoms, even at usual dosages.41,42 Nonsteroidal anti-inflammatory drugs have been found to cause a variety of psychiatric adverse events, including psychosis.43 Histamine2 (H2)-receptor antagonists and proton pump inhibitors, although considered relatively safe, have been associated with serious neuropsychiatric events (including mental confusion and agitation, insomnia, and hallucination), especially in elderly patients, severely ill patients, and those with impaired hepatic or renal function.4,44
Clinical Presentation
Medication-induced psychosis may present in a similar manner as idiopathic psychosis.45 The essential features of medication-induced psychosis are prominent delusions and/or hallucinations that are found to be due to the physiological effects of a medication.8 The hallucinations are usually tactile, visual, and/or gustatory.6 The patient may also present with paranoia, anxiety, agitation, grandiosity, and disorganized speech and/or behavior.6
There are no definitive tests to determine whether a patient is experiencing medication-induced psychosis. A thorough history is needed to help establish a temporal relationship. It is important to determine the onset of psychotic symptoms; medication-induced psychosis is usually related to an increase in dosage or changes to medication regimens, with symptoms appearing within days of drug initiation, dosage change, or discontinuation.6 Abrupt onset or the appearance of symptoms in patients older than 35 years with no known psychiatric history should suggest medication-induced psychosis.6,8 In certain cases, such as with corticosteroids, symptom onset can occur as long as 3 months later.6,28 Symptom duration also can help determine the etiology of a patient’s symptomatology; if symptoms persist for more than 4 weeks after discontinuation of the suspected medication, other causes of psychosis must be evaluated.39
Risk Factors and Prevention
Certain factors increase a patient’s risk of medication-induced psychosis, including age (young children, the elderly), altered hepatic or renal function, female gender, polypharmacy, and previous psychiatric history.6,8,13,28 It is important to obtain a thorough medical history to determine past and current psychotic illness. In addition, a complete medication history including all prescription and nonprescription drugs, herbal products, and supplements is essential. Illicit drug use and alcohol consumption must be addressed as well. Polypharmacy, especially in the elderly, may be associated with an increased risk of medication-induced psychosis; this population is more likely to be treated for parkinsonism, cardiovascular disease, and other conditions that have the potential to induce psychosis.39 In initiating drug therapy, it is always best to use the lowest dosage possible, taking into consideration the patient’s weight and age. Awareness of potential drug interactions also is important for preventing medication-induced psychosis.
Management
Medication-induced psychosis is typically self-limiting, usually resolving within a day (in some cases, several days) after discontinuation of the offending agent.8,28 Treatment involves discontinuing the suspected agent or, when discontinuation is not possible, lowering the dosage to below psychotomimetic levels and/or using antipsychotic medications to treat symptoms.6
In PD-treated patients, the drug with the greatest psychosis-inducing potential and the least antiparkinsonian activity should be eliminated first.13 PD medications should be eliminated in the following order: 1) adjunctive drugs such as anticholinergics, amantadine, and selegiline; 2) dopamine agonists; and 3) levodopa-carbidopa.13 If an antipsychotic medication is utilized to treat chronic and bothersome psychosis in a PD patient, the potential effect of worsened motor symptoms caused by dopamine blockade must be weighed against the potential benefit. Typical antipsychotics and most atypical antipsychotics are not recommended for this reason.46 Clozapine and quetiapine have been shown to be the most efficacious agents with the least likelihood of worsening motor symptoms.46,47 However, their side-effect profiles have prompted investigations into finding alternative agents that are effective in reducing hallucinations in PD patients. The most promising medications are the cholinesterase inhibitors rivastigmine and donepezil.46,47
Keeping the patient safe is an important aspect of treating acute illness. Ideally, the patient should be in an environment where he or she can be observed and contained, if necessary, to avoid self-harm or harm to others.6 Medical management is usually unnecessary if the offending agent is discontinued. Short-term treatment with antipsychotics or benzodiazepines during a period of psychosis may be warranted for patients in danger of harming themselves or others.6
A medication retrial may be appropriate in certain situations, such as when the patient’s psychosis developed as a result of a high dosage or when the agent was used in combination with other psychotomimetics.6 If a retrial is attempted, the medication should be initiated at a lower dosage, with careful monitoring of the patient for early signs of psychosis.6
Conclusion
Medication-induced psychosis has been associated with many nonpsychiatric medications. It is important to be aware of the psychotropic ADEs of many common nonprescription and prescription medications. Educating patients and caregivers about potential ADEs of psychotomimetic drugs and inquiring about ADEs at each patient encounter will aid in the early detection and prevention of medication-induced psychosis.28 Patients should be instructed to consult their pharmacist or other healthcare provider prior to using any nonprescription medication and to avoid excessive consumption of caffeinated products (≥10 mg/kg/day) when taking psychotomimetic agents.7,48 Preventive strategies directed at avoidance of high-risk medications, appropriate dosing regimens based on age and weight, reduction of polypharmacy, and close follow-up can improve patient outcomes.
REFERENCES
1. Forster AJ, Murff HJ, Peterson JF, et al. The incidence and severity of adverse events affecting patients after discharge from the hospital. Ann Intern Med. 2003;138:161-167.
2. Bourgeois FT, Shannon MW, Valim C, Mandl KD. Adverse drug events in the outpatient setting: an 11-year national analysis. Pharmacoepidemiol Drug Saf. 2010;19:901-910.
3. Budnitz DS, Pollock DA, Weidenbach KN, et al. National surveillance of emergency department visits for outpatient adverse drug events. JAMA. 2006;296:1858-1866.
4. Ashton CH. Psychiatric effects of drugs for other disorders. Medicine. 2004;32:50-52.
5. Desai AK. Psychotropic side effects of commonly prescribed medications in the elderly. Primary Psychiatry. 2004;11:27-34.
6. Goren JL. Psychosis. In: Tisdale JE, Miller DA, eds. Drug-Induced Diseases: Prevention, Detection, and Management. 2nd ed. Bethesda, MD: American Society of Health-System Pharmacists; 2010:344-356.
7. D’Souza DC. Hazy—the association between cannabis & psychosis. Pharmacy Weekly. 2011;6.
8. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). Washington, DC: American Psychiatric Publishing; 2013.
9. Ecker D, Unrath A, Kassubek J, Sabolek M. Dopamine agonists and their risk to induce psychotic episodes in Parkinson’s disease: a case-control study. BMC Neurology. 2009;9:23.
10. Fénelon G, Alves G. Epidemiology of psychosis in Parkinson’s disease. J Neurol Sci. 2010;289:12-17.
11. Forsaa EB, Larsen JP, Wentzel-Larsen T, et al. A 12-year population-based study of psychosis in Parkinson disease. Arch Neurol. 2010;67:996-1001.
12. Turjanski N, Lloyd GG. Psychiatric side-effects of medications: recent developments. Adv Psychiatr Treat. 2005;11:58-70.
13. Kuzuhara S. Drug-induced psychotic symptoms in Parkinson’s disease. Problems, management, and dilemma. J Neurol. 2001;248(suppl 3):III28-III31.
14. Fénelon G, Mahieux F, Huon R, Ziégler M. Hallucinations in Parkinson’s disease: prevalence, phenomenology and risk factors. Brain. 2000;123:733-745.
15. Factor SA, Molho ES, Podskalny GD, Brown D. Parkinson’s disease: drug-induced psychiatric states. Adv Neurol. 1995;65:115-138.
16. Holroyd S, Currie L, Wooten GF. Prospective study of hallucinations and delusions in Parkinson’s disease. J Neurol Neurosurg Psychiatry. 2001;70:734-738.
17. Onofrj M, Thomas A, Bonanni L. New approaches to understanding hallucinations in Parkinson’s disease: phenomenology and possible origins. Expert Rev Neurother. 2007;7:1731-1750.
18. Molho ES, Factor SA. Parkinson’s disease: the treatment of drug-induced hallucinations and psychosis. Curr Neurol Neurosci Rep. 2001;1:320-328.
19. Fernandez HH, Trieschmann ME, Friedman JH. Treatment of psychosis in Parkinson’s disease: safety considerations. Drug Saf. 2003;26:643-659.
20. Friedman JH. Parkinson’s disease psychosis 2010: a review article. Parkinsonism Relat Disord. 2010;16:553-560.
21. Eisendrath SJ, Sweeney MA. Toxic neuropsychiatric effects of digoxin at therapeutic serum concentrations. Am J Psychiatry. 1987;144:506-507.
22. Conant J, Engler R, Janowsky D, et al. Central nervous system side effects of beta-adrenergic blocking agents with high and low lipid solubility. J Cardiovasc Pharmacol. 1989;13:656-661.
23. Sirois FJ. Visual hallucinations and metoprolol. Psychosomatics. 2006;47:537-538.
24. Steinhart J, Pugh CR. Two patients with schizophrenic-like psychosis after treatment with beta-adrenergic blockers. Br Med J. 1979 Mar 24;1:790.
25. Goldner JA. Metoprolol-induced visual hallucinations: a case series. J Med Case Rep. 2012;6:65-67.
26. Huffman JC, Stern TA. Neuropsychiatric consequences of cardiovascular medications. Dialogues Clin Neurosci. 2007;9:29-45.
27. Doane J, Stults B. Visual hallucinations related to angiotensin-converting enzyme inhibitor use: case reports and review. J Clin Hypertens (Greenwich). 2013;15:230-233.
28. Warrington TP, Bostwick M. Psychiatric adverse effects of corticosteroids. Mayo Clin Proc. 2006;81:1361-1367.
29. Wolkowitz OM, Rubinow D, Doran AR, et al. Prednisone effects on neurochemistry and behavior. Preliminary findings. Arch Gen Psychiatry. 1990;47:963-968.
30. Ciriaco M, Ventrice P, Russo G, et al. Corticosteroid-related central nervous system side effects. J Pharmacol Pharmacother. 2013;4(suppl 1):S94-S98.
31. Türktas I, Gücüyener K, Ozden A. Medication-induced psychotic reaction. J Am Acad Child Adolesc Psychiatry. 1997;36:1017-1018.
32. Grill MF, Maganti RK. Neurotoxic effects associated with antibiotic use: management considerations. Br J Clin Pharmacol. 2011;72:381-393.
33. Testa A, Giannuzzi R, Sollazzo F, et al. Psychiatric emergencies (part II): psychiatric disorders coexisting with organic diseases. Eur Rev Med Pharmacol Sci. 2013;17(suppl 1):65-85.
34. Moorthy N, Raghavendra N, Venkatarathnamma PN. Levofloxacin-induced acute psychosis. Indian J Psychiatry. 2008;50:57-58.
35. Shah M, Subhani M, Rizvon K, Mustacchia P. Transient psychotic episode induced by Helicobacter pylori triple therapy treatment. Case Rep Gastroenterol. 2012;6:381-386.
36. Elahi F, Bhamjee M. A case of clarithromycin psychosis. Psychiatr Bull. 2004;28:98-99.
37. Lee KY, Huang CH, Tang HJ, et al. Acute psychosis related to use of trimethoprim/sulfamethoxazole in the treatment of HIV-infected patients with Pneumocystis jirovecii pneumonia: a multicentre, retrospective study. J Antimicrob Chemother. 2012;67:2749-2754.
38. Stuhec M. Trimethoprim-sulfamethoxazole–related hallucinations. Gen Hosp Psychiatry. 2014;36:203.e7-e8.
39. Bangar S. P03-58—Treatment of cycloserine induced psychosis—a case series [abstract]. Eur Psychiatry. 2011;26(suppl 1):1227.
40. Benton T, Blume J, Dubé B. Treatment considerations for psychiatric syndromes associated with HIV infection. HIV Ther. 2010;4:231-245.
41. Flaherty JH. Psychotherapeutic agents in older adults. Common prescribed and over-the-counter medications: causes of confusion. Clin Geriatr Med. 1998;14:101-127.
42. Brown TM, Stoudemire A. Psychiatric Side Effects of Prescription and Over-the-Counter Medications: Recognition and Management. Washington, DC: American Psychiatric Press; 1998.
43. Browning CH. Nonsteroidal anti-inflammatory drugs and severe psychiatric side effects. Int J Psychiatry Med. 1996;26:25-34.
44. Picotte-Prillmayer D, DiMaggio JR, Baile WF. H2 blocker delirium. Psychosomatics. 1995;36:74-77.
45. Sciolla A. Iatrogenic psychoses. Semin Clin Neuropsychiatry. 1998;3:61-69.
46. Connolly BS, Fox SH. Drug treatments for the neuropsychiatric complications of Parkinson’s disease. Expert Rev Neurother. 2012;12:1439-1449.
47. Zahodne LB, Fernandez HH. Pathophysiology and treatment of psychosis in Parkinson’s disease: a review. Drugs Aging. 2008;25:665-682.
48. Hedges DW, Woon FL, Hoopes SP. Caffeine-induced psychosis. CNS Spectr. 2009;14:127-129.
49. Drugs that may cause psychiatric symptoms. Med Lett Drugs Ther. 2008;50:100-103.
To comment on this article, contact rdavidson@uspharmacist.com.ß






