US Pharm. 2015;40(3):HS2-HS6.
ABSTRACT: The rate of death from overdoses of prescription opioids in the United States more than quadrupled between 1999 and 2010. It is imperative to recognize the signs and symptoms of opioid overdose as soon as they start and to administer an antidote. Opioid overdose rescue kits containing naloxone have served as a valuable stepping-stone in helping to save lives from overdoses. Pharmacists can play a key role in the prevention and management of adverse effects and the overdoses associated with opioids. They can also help with education on the use of overdose rescue kits.
Pain is one of the most common symptoms patients experience. Data presented in the recently released Institute of Medicine report, Relieving Pain in America, suggests that more than 100 million persons in the United States live with chronic pain and that the estimated economic burden of just chronic pain alone exceeds $500 billion annually.1 These realities open up an avenue for the pharmacist, who is part of the multidisciplinary healthcare team, to play a major role in pain management.
Opioids are a key component in the management of moderate-to-severe pain. They are generally labeled as high-risk medications because of their capacity to cause significant harm or toxicity to patients if used inappropriately. Many incidents of opioid toxicity are the result of preventable causes.2
In 2010 alone, prescription opioids were involved in 16,651 overdose deaths, whereas heroin was implicated in 3,036. Some 82% of the deaths due to prescription opioids and 92% of those due to heroin were classified as unintentional, with the remainder being predominantly attributed to suicide or “undetermined intent.”2 The classic signs of opioid intoxication include depressed mental status, decreased respiratory rate, decreased tidal volume, decreased bowel sounds, and miotic (constricted) pupils.3
Prevention
Physicians need clear, evidence-based best practices that serve as clinical guidelines for prescribing opioids for the management of chronic (noncancer) pain in the emergency room and in the outpatient setting. Patients also need to be carefully screened to identify those at increased risk of opioid overdose. However, overdose potential must be seen as a separate but parallel phenomenon that can exist in the absence of abuse, diversion, and addiction. A rescue response is often necessary because overdoses will still occur despite prevention efforts. Review of medical examiner data reveals that well over half of the people who accidentally died from drug overdoses were dead prior to the arrival of emergency medical services. This important information clearly shows that there is the need for community-based tools and education.4
Many states with higher-than-average prescription drug mortality rates have already begun designing, implementing, and evaluating opioid prevention strategies, and federal agencies are beginning to respond. There is a National Prescription Drug Abuse Prevention Strategy and a U.S. Department of Justice National Prescription Drug Threat Assessment Program.5 These are measures that have been put in place to prevent patients, especially opioid addicts, from gaining access to multiple prescriptions through doctor and pharmacy shopping.
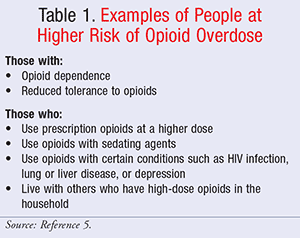
The World Health Organization (WHO) recommends that certain high-risk individuals (see TABLE 1) be given naloxone kits due to the rise in deaths from opioid overdoses; over 16,000 people in the U.S. died of opioid overdose in 2010.5 However, giving naloxone kits to patients is not the only way to prevent opioid overdoses. The WHO recommends several other measures for prevention as well: monitoring opioid prescribing practices; curbing inappropriate opioid prescribing and OTC sales; and increasing the rate of treatment of persons with opioid dependence, including those dependent on prescription opioids.5
Opioid Overdose Rescue Kits
Opioid overdose–related deaths can be prevented when naloxone is administered in a timely manner. As a narcotic antagonist, naloxone displaces opiates from receptor sites in the brain and reverses respiratory depression that usually is the cause of overdose deaths. During the period of time when an overdose can become fatal, respiratory depression can be reversed by giving the affected individual naloxone. Naloxone has no psychoactive effects and does not present any potential for abuse.6
Naloxone rescue kits help reverse the drug overdose. It is typically supplied as a kit consisting of ultraviolet (UV) light-protective bags containing two syringes with needles and two naloxone vials. Injectable naloxone is relatively inexpensive, at a cost of about $6 per dose and $15 per kit.7 Use of an opioid overdose rescue kit requires training and education by an expert on how to administer naloxone using a syringe.
Naloxone Monograph: The product monograph information for naloxone hydrochloride and the drug rescue kits (Naloxone [Narcan] Life-Saving Drug Overdose Kit; Evzio) is provided in TABLE 2.8

Evzio: Evzio is a take-home naloxone auto-injector that patients, family members, and other caregivers can keep close by in case an opioid overdose occurs.8,9 The naloxone automated injector (FIGURE 1) has been approved by the FDA since April 2014 and does not require special training to use because it has voice instructions that are activated when the cap is removed from the device.10 The device can rapidly deliver a single dose of naloxone through clothing when placed on the outer thigh muscle.11 The per-dose cost of naloxone via the auto-injector has not yet been determined.6

Overdose Education and Naloxone Distribution (OEND) Programs
Project Lazarus: Project Lazarus is a secular, public health nonprofit organization established in 2008 in response to extremely high drug-overdose death rates in Wilkes County, North Carolina (four times higher than the state average).12 The educational component of Project Lazarus is conducted in the privacy of a physician’s office. At the end of a video and after completing the enrollment forms, patients receive the naloxone kit free of charge from their healthcare provider, along with any prescriptions for pain management that they may require. The Project Lazarus Naloxone Rescue Kit contains13:
• Two needle-free syringes of naloxone rescue medication
• Two nasal adaptors
• A refrigerator magnet
• A DVD of the instructional video
• Guides on how to talk to your family about overdose.
The Massachusetts OEND Program: The objective of this study was to evaluate the impact of state-supported OEND programs on rates of opioid-related death from overdose and acute care utilization in Massachusetts.3 OEND programs have primarily been implemented among substance users who are at risk for overdose themselves and likely to witness another person overdosing, and thus are in a position to help.14 In 2006-2007, two community public health agencies began providing OEND. The Massachusetts Department of Public Health expanded the program to four more organizations in 2007 and two more in 2009. These agencies, which provided HIV education and prevention services to substance users, provided OEND to potential overdose bystanders through trained nonmedical public health workers under a standing order from the OEND medical director. OEND trainers completed a 4-hour course, knowledge test, and two training sessions of potential bystanders supervised by a master trainer. Key elements included minimizing the risk of overdose by reducing polysubstance misuse (e.g., concomitant alcohol, benzodiazepine, or cocaine), accounting for reduced tolerance after abstinence, and not using alone; recognizing overdose by assessing for unresponsiveness and decreased respirations; and responding to an overdose by seeking help, providing rescue breathing, administering nasal naloxone, and staying with the person until medical personnel arrives or the person recovers.14
Of 327 rescue attempts using naloxone reported by 212 individuals, 87% (286/327) were reported by users.14 Most rescue attempts occurred in private settings. The rescuer and the person who overdosed were usually friends. Naloxone was successful in 98% (150/153) of the rescue attempts. For the three rescue attempts where naloxone was not successful, the persons who overdosed received care from the emergency medical system and survived. Compared with no implementation, both low and high implementation of OEND was associated with lower rates of opioid-related deaths from overdose, when adjusted for demographics, utilization of addiction treatment, and doctor shopping (Schedule II opioid prescriptions from >4 prescribers and filled prescriptions at >4 pharmacies in a 12-month period).3
This study provides observational evidence that OEND is an effective public health intervention to address increasing mortality in the opioid overdose epidemic by training potential bystanders to prevent, recognize, and respond to overdoses. Program implementation seemed to have a dose-related impact, where the higher the cumulative rate of OEND use, the greater the reduction in death rates.3
Opioid Overdose Rescue by Trained Verses Untrained Individuals: Another retrospective cohort study compared overdose rescues by trained and untrained participants and change in opioid use among substance-using participants in OEND programs from 2006 to 2010.15 OEND programs have primarily been implemented among substance users who are at risk for overdose. This study showed that education is needed along with naloxone distribution because naloxone kits can provide a false sense of security. Of the 373 substance-using OEND program participants who reported an overdose rescue, 34% of the trained and 24% of the untrained participants reported more than one overdose rescue with a mean of 2.9 and 2.6 rescues among those with more than one in each group, respectively. In this study, however, there was no substantive difference in overdose rescue management by those trained by the OEND program directly compared to those trained via social networks on the Internet.15
Prospective studies are warranted to determine how social network training and dissemination should be formally incorporated into program design. Randomized, controlled trials or prospective cohort studies of OEND with systematic and thorough follow-up are the needed next steps in addressing the structure, content, and optimal amount of training to accompany naloxone rescue kits and the effect of OEND on participant drug use.14
Role of the Pharmacist
Prescription Drug Monitoring Programs (PDMPs) have emerged as an important strategy for addressing the misuse and abuse of prescription opioids, thus preventing opioid overdoses and deaths.6 This is a key area where pharmacists can play a role. They can check their state’s PDMP database to determine whether a patient is filling the prescriptions provided and/or obtaining prescriptions for the same or a similar drug from multiple pharmacies.6 This can put a restriction on easy access to prescription opioids and hence prevent possible overdose.
Pharmacists can also help in education on the use of opioid overdose rescue kits, especially in the community setting. Pharmacists can be involved in educating the community to identify an individual who is experiencing opioid overdose and call 911 to get immediate medical attention, and providing information on resources and educational pamphlets that may be useful to local organizations. Some of these resources can be found on the websites of the Substance Abuse and Mental Health Services Administration (www.samhsa.gov) and the CDC (www.cdc.gov).16
In conclusion, opioid overdose rescue kits have shown to be successful, and a step in the right direction toward helping to minimize opioid overdose treatment delays. Pharmacists can play a vital role in bridging the gap with patients.
ACKNOWLEDGMENT: The author would like to thank Afua Gyapong, PharmD Candidate, for her assistance on this article.
REFERENCES
1. Volkow ND, Frieden TR, Hyde PS, Cha SS. Medication-assisted therapies—tackling the opioid-overdose epidemic. N Engl J Med. 2014;370(22):2063-2066.
2. Baumann TJ, Herndon CM, Strickland JM. Chapter 44. Pain management. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 9th edition. New York, NY: McGraw-Hill; 2014. http://accesspharmacy.mhmedical.com/content.aspx?bookid=689&Sectionid=45310494. Accessed December 17, 2014.
3. Walley AY, Xuan Z, Hackman HH, et al. Opioid overdose rates and implementation of overdose education and nasal naloxone distribution in Massachusetts: interrupted time series analysis. BMJ. 2013; 346:f174.
4. Dasgupta N, Sanford C, Albert S, Brason FW II. Opioid drug overdoses: a prescription for harm and potential for prevention. Am J Lifestyle Med. 2010;4(1):32-37.
5. World Health Organization (WHO). Community Management of Opioid Overdose. Geneva, Switzerland: WHO; 2014. http://apps.who.int/iris/bitstream/10665/137462/1/ 9789241548816_eng.pdf?ua=1&ua=1. Accessed February 9, 2015.
6. Bagnola AJ, Escano AK. Identifying potential causes of opioid toxicity necessitating a rapid response team visit. J Pharm Technol. 2013;29:118-122.
7. Samhsa opioid overdose toolkit. Substance Abuse and Mental Health Services Administration. Updated 2014. http://store.samhsa.gov/product/Opioid-Overdose-Prevention-Toolkit-Updated-2014/SMA14-4742. Accessed December 17, 2014.
8. Naloxone hydrochloride. Micromedex Solutions. www.micromedexsolutions.com. Accessed December 17, 2014.
9. EVZIO: the first and only naloxone auto-injector. Indication. What is Evzio? http://evzio.com/patient/?gclid=CjwKEAiAk8qkBRDOqYediILQ5BMSJAB40A5ULFSizc8OknKtIbEwAg34W8YnNI8srTfq_ij1JZ2UohoCruzw_wcB. Accessed December 17, 2014.
10. Evzio (naloxone hydrochloride injection) package insert. Richmond, VA: Kaleo, Inc; April 2014. http://evzio.com/pdfs/Evzio%20PI.PDF. Accessed February 5, 2015.
11. Finklea K, Sacco L, Bagalman E. Prescription Drug Monitoring Programs. Congressional Research Service. March 24, 2014. www.fas.org/sgp/crs/misc/R42593.pdf. Accessed February 12, 2015.
12. About Project Lazarus. Project Lazarus. www.projectlazarus.org/about-project-lazarus. Accessed December 17, 2014.
13. How do I get an overdose reversal kit? Project Lazarus. http://projectlazarus.org/patients-families/how-do-i-get-overdose-reversal-kit. Accessed February 5, 2015.
14. Doe-Simkins M, Quinn E, Xuan Z, et al. Overdose rescues by trained and untrained participants and change in opioid use among substance-using participants in overdose education and naloxone distribution programs: a retrospective cohort study. BMC Public Health 2014;14:297.
15. Acute opioid intoxication in adults. Clinical features of overdose. UptoDate. www.uptodate.com/contents/acute-opioid-intoxication-in-adults. Accessed December 18, 2014.16. Ready-to-use guidance and prescription+patient instructions. Naloxone rescue kit compounding & storage information. Prescribe to Prevent. http://prescribetoprevent.org/pharmacists. Accessed December 18, 2014.
To comment on this article, contact rdavidson@uspharmacist.com.






