US Pharm. 2021;46(8):HS10-HS16.
ABSTRACT: Poisoning is a significant public-health issue for children and adolescents. Most poisoning cases occurring in this patient population are unintentional, and most exposures occur in the home. Because pharmacists are drug experts, the community relies on them to be knowledgeable about ingredients found not only in drugs but also in OTC supplements and household products. For this reason, pharmacists may receive incoming calls or cases concerning pediatric ingestion of possibly harmful products. Pharmacists should accordingly be aware of the many aspects of poison control and its public-health implications and understand how to refer and possibly manage these cases with the help of the appropriate resources.
Poisoning is a significant public-health issue for children and adolescents, and most cases of exposure occurring in this patient population are unintentional. Each year in the United States, approximately 1 million poison exposures in children younger than age 6 years are reported to the American Association of Poison Control Centers (AAPCC). In addition, approximately 132,000 to 135,000 exposures in children aged 6 to 12 years and 171,000 to 177,000 exposures in adolescents aged 13 to 19 years are reported. The National Poison Data System (NPDS) is a near–real-time surveillance system that improves situational awareness of chemical and poison exposures based on data from U.S. poison centers. The CDC uses this information to enhance public-health surveillance of poison and chemical exposures and associated illness, identify early markers of chemical events, and improve situational awareness during outbreaks.1
Most poisoning exposures occur in the home, and patterns of poisonings varies by age and sex. In preadolescents, poisoning occurs slightly more often in boys than in girls, but this trend reverses in adolescents, with approximately 60% of all poisonings in those aged 13 to 19 years occurring in girls. The majority of poisonings involving young children are classified as unintentional (e.g., exploratory ingestions, therapeutic errors). However, in adolescents, more than one-half of poisoning exposures (62% in 2019) are intentional. According to NPDS coding data from poison-control centers across the U.S., poisoning exposure usually causes minor symptoms in young children.2
Notably, the importance of safety labeling is illustrated by the fact that ingestion of OTC cough and cold preparations by young children declined after the labels of these products were revised to warn against use in children younger than age 4 years. Child self-ingestion of pharmaceutical agents increased between 2004 and 2010 with the rising availability of prescription medications, but the rate decreased between 2010 and 2013. Based on national surveillance conducted between 2007 and 2011, it is estimated that nearly 9,500 U.S. children younger than age 6 years are hospitalized each year for unsupervised ingestion of prescription medications.2,3
Opioids and benzodiazepines were found to be the most commonly ingested medications.2,3 Among children who presented to the emergency department with unsupervised medication exposure between 2010 and 2013, opioids and benzodiazepines were the most commonly ingested prescription solids; acetaminophen, cough and cold remedies, ibuprofen, and diphenhydramine were the most commonly ingested liquid OTC medications.2,3 According to the NPDS, self-exposure to electronic cigarettes in children also appears to be on the rise. Substances most frequently involved in fatalities in children aged 5 years and older in 2019 included fumes, gases, and vapors (primarily carbon monoxide); batteries; hydrocarbons; and analgesics.4
One study formulated a hazard factor to objectively assess the pediatric poisoning hazard of various products based on the potential acute toxicity of individual ingredients and the frequency and extent of injuries following actual exposures.5 By considering frequency and extent of injury after actual exposures, the hazard factor denotes more than the acute toxicity of individual ingredients and is influenced by variables such as packaging, accessibility, availability (as a reflection of marketing), formulations, and closure types. The hazard factor was derived by analyzing >3.8 million exposures in children younger than age 6 years that were reported to the AAPCC from 1985–1989 (TABLE 1), and significant hazards were limited to a few products.5

Pharmacist Involvement
Because pharmacists are drug experts, the community relies on them to be knowledgeable of ingredients found not only in drugs but also in OTC supplements and household products. For this reason, pharmacists may receive incoming calls or cases involving ingestion of possibly harmful products. Pharmacists can foster public awareness by explaining to parents and other caregivers that most pediatric poisoning cases can be managed safely at home by consultation with a specialist from a poison-control center, many of which hire healthcare professionals, including licensed pharmacists, certified and specialized in poison information. Poison-control centers are found across the U.S.; some states have more than one, and some centers take calls from more than one state. Pharmacists can use and provide patients a national toll-free number (1-800-222-1222) that connects to the regional poison-control center serving the calling area.6
Poison-control centers have two relatively distinct educational activities: primary and secondary prevention. The goal of primary prevention is to avoid the occurrence of a poisoning exposure. Examples include advising caregivers to lock up medicines and household cleaners to keep them out of the reach of young children; requiring employees who could be exposed to hazardous chemicals to wear safety equipment such as gloves, goggles, and personal protective equipment; and recommending storage techniques to older adults in order to avoid medication mishaps. Secondary prevention aims to reduce the effect of a poisoning exposure through improved access to poison-control services. Examples include raising awareness of the poison-control center’s telephone number and ensuring that activated charcoal is used as an antidote only when specifically advised by a physician or by poison-control center staff, as it is not indicated in all circumstances.6
It is generally not recommended for caregivers to keep antidotes at home, as this practice may interfere with the administration of other antidotes and treatments for counteracting the hazardous activity of the ingested toxin and diminishing its metabolites. Therefore, it is always best to recommend that the caregiver or patient contact the poison-control center, which is available for toxicology consultation 24 hours per day, 7 days per week, and has specialized information on how to best manage the ingested poison either under supervision at home or at a healthcare facility. In toxicologic emergencies, the antidote must be determined by the poison-control center and weighed against the potential adverse effects and toxicity of the antidote. In the case of severe poisoning, the antidote is strictly an adjunct to supportive treatment, and its use should not distract the healthcare provider from attending adequately to the airway, breathing, circulation, and decontamination. Appropriate administration of an antidote may limit morbidity and mortality; on the other hand, if it is unavailable or used inappropriately, the patient may experience adverse effects from the poison or from the antidote, respectively.4,6
Risk Factors Associated With Potential Toxins
Age and sex are factors to consider in evaluating a child’s or adolescent’s risk for poisoning, and this can be a point of conversation with parents and other caregivers in the pharmacy. When educating caregivers, pharmacists should keep in mind that the developmental and environmental factors that contribute to the risk of a pediatric poisoning event can be effective demonstrators of the need for prevention. First, for infants and toddlers, normal developmental milestones, including exploration of their environment, put this age group at risk for a poisoning event. As babies learn to crawl and walk, they begin to investigate their surroundings, including opening cabinets and examining what they find inside.7
Second, developmental factors and pressures that evolve as the child ages contribute to the increased risk of poisoning among adolescents. The goal of independence and the tendency to believe that they are indestructible may cause adolescents to take undue risks, such as experimenting with illicit drugs, other substances of abuse, or potentially dangerous trends that spread on a larger scale through social media (e.g., TikTok). Peer pressure and the desire to conform also contribute to this problem. In addition, adolescents (more commonly girls than boys) may take an overdose of medication as a suicide attempt or as a bid for attention.8
Third, the home and similar environments may harbor numerous potentially toxic substances, particularly in the kitchen (e.g., dishwasher-detergent packets/pods), bathroom, laundry room (e.g., laundry-detergent pods), and garage. Items used frequently, such as cleaning products, may be stored in low cabinets for easy access. Some products are so familiar and commonly used that caregivers may not realize their toxicity (e.g., drain clearers and toilet-bowl cleaners can be highly toxic if ingested).6,7 Another problem may arise when frequently used products or medications are stored properly but during or after use may be accidentally left within the child’s reach.
Child self-exposure accounted for 95% of visits to a healthcare facility for evaluation of exposure to a potentially toxic dose of a pharmaceutical agent reported to the AAPCC between 2001 and 2008. Look-alikes also pose a problem for small children. Some medications may be mistaken for candy; similarly, some cleaning products may look like or be stored in containers resembling those for food or juice. The availability of medications, drugs, or other substances of abuse at school or at home may put vulnerable children and adolescents at further risk. This has been a particular problem during the COVID-19 pandemic given the accessibility and increased use of hand sanitizers, many of which were recalled because they contained toxic levels of methanol. Even in small amounts, ingestion of methanol (a toxic alcohol) can result in serious health outcomes, such as metabolic acidosis and vision loss. This scenario underscores the importance of always referring caregivers to the poison-control center, as these entities are best equipped with the expertise in toxicology to accurately evaluate and manage potential ingestions.9,10
Prevention
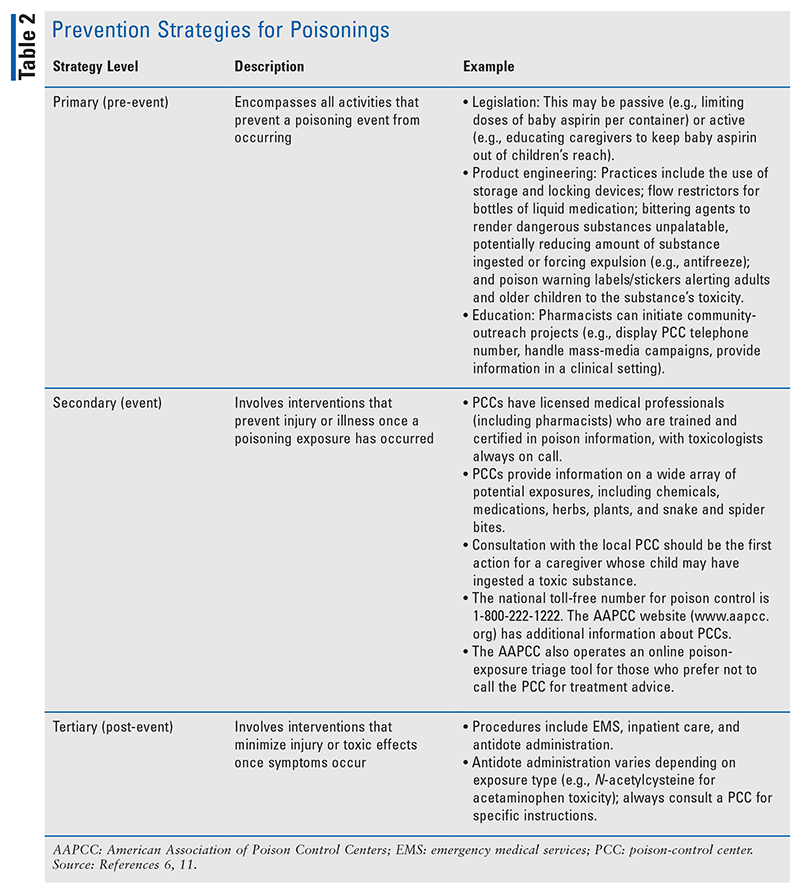
Prevention strategies for poisonings, as for other types of injury, may be classified into primary (pre-event), secondary (event), and tertiary (post-event) levels (TABLE 2).6,11
Education and Resources
Dosing errors and incorrect use of devices designed to deliver liquid medications may result in unintentional pediatric poisonings. In 2015, the American Academy of Pediatrics (AAP) Committee on Drugs issued a policy statement on the dosing of orally administered liquid medications for children. The AAP policy statement, which can be reviewed by pharmacists, recommends the following12:
• Metric dosing should be used exclusively for liquid medications, which should be dosed to the nearest 0.1 mL, 0.5 mL, or 1 mL, as appropriate.
• The concentration of a liquid medication should be included on the prescription so that the appropriate dose can be calculated.
• Pharmacists can review mL-based doses with families at the time of prescription.
• Pharmacies may provide a mL-based dosing device with an appropriate volume (in order to avoid a twofold dosing error).
Another educational effort involves minimizing issues around polypharmacy and multiple medications taken for different therapeutic indications. Pharmacists encounter many patient populations, particularly elderly patients, that require multiple medication refills. The pharmacist can take a few extra moments to discuss with these patients important steps they can take to keep children away from their medication by emphasizing some of these key points6,13-16:
• Keep harmful products locked up and out of the child’s sight and reach.
• Baby-proof drawers and cabinets where potentially toxic products are kept.
• Instruct the child that the medicine is not candy even though it may appear similar.
• Always replace the safety cap immediately after product use.
• Never leave containers of alcohol or electronic cigarettes/nicotine refill cartridges within the child’s reach; a small amount of liquid nicotine spilled on the skin or swallowed can be fatal to a child.
• Keep products and medicines in their original containers; never put nonfood products in food or drink containers.
• Take special care to keep colorfully packaged products (e.g., laundry-detergent pods) away from the child, who may think that they are candy.
• Read all product labels carefully and thoroughly before use.
• Teach the child not to drink or eat anything unless it is provided by a trusted adult (preferably packed or given by a parent).
• Avoid administering medicine or taking your own medicine in front of the child, as children tend to imitate their parents and grandparents.
• Check your home often for old medicines and dispose of them appropriately through a take-back drug program (the FDA provides guidance on drug disposal for collection sites).
• Avoid use of and dispose of old-fashioned treatments (e.g., oil of wintergreen, which can contain a concentrated amount of aspirin in a small amount and be life-threatening to a child if ingested).
• Remember that there is more danger of poisoning when a child is away from home, especially at a grandparent’s home.
Additional resources related to poisoning prevention are available for pharmacists to apply in their practice. These include6,14-16:
• AAPCC (www.aapcc.org)
• CDC, “Tips to Prevent Poisonings” (www.cdc.gov/homeandrecreationalsafety/poisoning/preventiontips.htm)
• Nemours KidsHealth, “Household Safety: Preventing Poisoning” (https://kidshealth.org/en/parents/safety-poisoning.html)
• SafeKids Worldwide, “Poison Prevention Tips” (www.safekids.org/tip/poison-prevention-tips)
Conclusion
Pharmacists are in a key position in the community to serve a critical role in both direct patient care and public health with regard to poison prevention. Pharmacists with less specialized knowledge and training in toxicology-related events and poison prevention can become better equipped by familiarizing themselves with poison-control centers’ resources and scope of services. It is important for pharmacists to understand the benefits of using poison-control centers and other sources of preventive care in clinical situations and be knowledgeable about available resources so that they can educate their patients on how to prevent poison occurrences and refer them as necessary to help them better manage exposures.
REFERENCES
1. Wolkin AF, Martin CA, Law RK, et al. Using poison center data for national public health surveillance for chemical and poison exposure and associated illness. Ann Emerg Med. 2012;59(1):56-61.
2. Gummin DD, Mowry JB, Spyker DA, et al. 2018 annual report of the American Association of Poison Control Centers’ National Poison Data System (NPDS): 36th annual report. Clin Toxicol (Phila). 2019;57(12):1220-1413.
3. Lovegrove MC, Weidle NJ, Budnitz DS. Trends in emergency department visits for unsupervised pediatric medication exposures, 2004-2013. Pediatrics. 2015;136(4):e821-e829.
4. Gummin DD, Mowry JB, Beuhler MC, et al. 2019 annual report of the American Association of Poison Control Centers’ National Poison Data System (NPDS): 37th annual report. Clin Toxicol (Phila). 2020;58(12):1360-1541.
5. Litovitz T, Manoguerra A. Comparison of pediatric poisoning hazards: an analysis of 3.8 million exposure incidents. A report from the American Association of Poison Control Centers. Pediatrics. 1992;89(6 Pt 1):999-1006.
6. National Capital Poison Center. Poison control. www.poison.org. Accessed May 7, 2021.
7. Wynn PM, Zou K, Young B, et al. Prevention of childhood poisoning in the home: overview of systematic reviews and a systematic review of primary studies. Int J Inj Contr Saf Promot. 2016;23(1):3-28.
8. Spiller HA, Ackerman JP, Spiller NE, Casavant MJ. Sex- and age-specific increases in suicide attempts by self-poisoning in the United States among youth and young adults from 2000 to 2018. J Pediatr. 2019;210:201-208.
9. Bond GR, Woodward RW, Ho M. The growing impact of pediatric pharmaceutical poisoning. J Pediatr. 2012;160(2):265-270.e1.
10. Yip L, Bixler D, Brooks DE, et al. Serious adverse health events, including death, associated with ingesting alcohol-based hand sanitizers containing methanol—Arizona and New Mexico, May-June 2020. MMWR Morb Mortal Wkly Rep. 2020;69(32):1070-1073.
11. Pandve HT. Quaternary prevention: need of the hour. J Family Med Prim Care. 2014;3(4):309-310.
12. Committee on Drugs. Metric units and the preferred dosing of orally administered liquid medications. Pediatrics. 2015;135(4):784-787.
13. HealthyChildren.org. Poison prevention & treatment tips. www.healthychildren.org/English/safety-prevention/all-around/Pages/Poison-Prevention.aspx. Accessed May 31, 2021.
14. CDC. Poisoning prevention. www.cdc.gov/safechild/poisoning/index.html. Accessed May 17, 2021.
15. KidsHealth. Household safety: preventing poisoning. https://kidshealth.org/en/parents/safety-poisoning.html. Accessed May 12, 2021.
16. Safe Kids Worldwide. Poison prevention tips. www.safekids.org/tip/poison-prevention-tips. Accessed May 10, 2021.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.






