US Pharm. 2016;41(1):31-34.
Migraine headache is a common, debilitating condition affecting nearly 1 out of 7 Americans annually.1 This condition affects more women than men, and prevalence is highest during peak productive years, between the ages of 25 and 55 years.2 Migraine accounts for the majority of the 5 million headache visits to U.S. emergency departments annually.3 It has a major impact on quality of life; more than 90% of migraine sufferers find it difficult to work or function normally during an attack, accounting for more than 150 million missed worked days, with an annual cost to employers exceeding $14 billion.4,5 In addition, migraine headache is ranked as the sixth highest cause of disability worldwide.6
Pharmacists are in a unique position to help care for patients suffering from migraines. They are often the first healthcare professionals that patients will encounter when seeking relief for their migraine; as many as 57% of patients self-medicate with OTC products.7 It is important for pharmacists to understand when and how to use OTC products for the management of migraines as well as when patients require referral to their healthcare provider.
Pathophysiology
We have come a long way in our understanding of migraine. Descriptions of headaches date back to roughly 3000 BC. At that time, it was thought that migraines were due to malevolent beings inside the head with treatments consisting of incantations and application of substances to the head to drive out these spirits and demons.8 Although we obviously know that this is no longer the case, the exact pathophysiology of migraine is still unclear. In the past century, there have been two theories that have dominated thought. In the 1940s, the vascular theory was introduced by Harold Wolff, MD. Migraine attacks were caused by the dilation of intracranial blood vessels, while the aura associated with migraines resulted from vasoconstriction of blood vessels.9 However, there have been regional blood and imaging studies that do not support this theory in its entirety. The more accepted theory now is that migraines are caused by a neuronal dysfunction characterized by paroxysmal symptoms; migraine attacks are triggered by excessive neocortical cellular excitability.9
It is believed that migraine headaches are dependent upon activation and sensitization of the central trigeminal system.10 Migraine pain begins with the activation of trigeminal nerve fibers surrounding blood vessels.11 This activation triggers the release of vasoactive and proinflammatory neuropeptides, contributing to increased blood flow and plasma extravasation, eventually causing perivascular inflammation.11 It is this inflammation that sensitizes the trigeminal nerve cells to nonspecific stimuli, increasing pain perception. This trigeminal hyperexcitability, known as central sensitization, results in allodynia and the prolongation of a migraine attack.12
The migraine aura is thought to be a result of neuronal excitation and suppression that spreads throughout the gray matter of the brain, also known as cortical spreading depression (CSD). This phenomenon can also activate the trigeminal nociception and trigger headache mechanisms.10 The idea of CSD is generally now accepted as the biological basis of most types of migraines.10 Migraine without aura may be due to the occurrence of CSD in areas of the brain where tissue polarization is not consciously perceived.10
Triggers
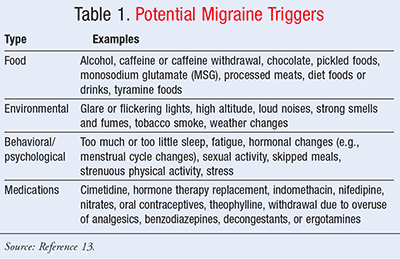
There are several triggers that have been identified that can increase a patient’s risk of experiencing a migraine. Triggers differ for everyone, and it is important for patients to understand what events or stimuli precipitate an attack. Triggers for migraine may be related to foods, environmental stimuli, and behavioral-psychological factors (TABLE 1).13
There appears to be a genetic component to migraines. If one parent suffers from migraines, there is a 40% chance that the child will also suffer. If both parents are afflicted, this chance increases to 90%.5
Clinical Presentation
Migraines are associated with varying symptoms and differ between individuals and attacks.13,14 Untreated migraines can last from 4 to 72 hours. Headache pain is usually described as moderate to severe, throbbing, unilateral, and retro-orbital in location. Patients may also experience nausea, vomiting, malaise, photophobia, phonophobia, irritability, and/or neck pain. In general, migraine headaches can be classified as migraine with aura and migraine without aura. About 25% of patients will experience aura. Auras can occur prior to or during a migraine attack and are most commonly visual, often characterized by flickering lights or loss of vision.13,14
Patient Assessment
A four-question algorithm has been developed to assist pharmacists when assessing a patient seeking treatment for headache15:
1. What percentage of your headaches prohibit you from performing your daily tasks and/or are accompanied by vomiting?
2. How many days per month are you completely headache free?
3. What are the symptoms of your attacks?
4. What OTC products have you tried in the past, and how have they worked?
If patients indicate that more than half of their headaches are disabling or that more than 20% of their migraines are accompanied by vomiting, they are poor candidates for OTC therapy and should be referred to their primary healthcare provider. A patient who spends fewer than 15 days a month head-ache free should also be referred.
OTC Treatments
Acetaminophen: Although not FDA approved for migraine treatment, acetaminophen has been shown to be effective for the treatment of mild-to-moderate migraines.16 Acetaminophen 1,000 mg was found to be highly effective in relieving pain, functional disability, photophobia, and phonophobia in patients with nonincapacitating migraine.17 Patients should be advised not to exceed more than 4,000 mg in 24 hours due to risk of hepatotoxicity; however, this dose may be too much for certain patients, such as those who drink more than three alcoholic beverages per day and those on warfarin.18 Patients should also be alerted to the fact that various products contain acetaminophen and should not be used in combination.18
Aspirin: Aspirin is an agent that has anti-inflammatory properties and may be beneficial in migraine treatment. High-dose aspirin (900-1,000 mg) has been established as an effective treatment option for acute migraine.16,19 Aspirin should be used with caution in patients with a history of peptic ulcer disease and those taking warfarin. When used in high doses, the development of tinnitus may be indicative of aspirin overdose.20
Ibuprofen: Nonsteroidal anti-inflammatory drugs (NSAIDs) in general are a good starting point for acute migraines that are mild to moderate in severity, although they may be effective in patients with more severe migraines if they have experienced adequate relief in the past.16 Several clinical studies have demonstrated the efficacy of ibuprofen in the management of migraine, with doses ranging from 200 to 1,200 mg.21-24 Both the 200- and 400-mg doses have been proven to provide clinical benefit 2 hours post administration. Various measures of pain relief and symptom improvement scores were utilized within these studies. Studies demonstrated a trend in improvement with increasing ibuprofen doses, but statistical significance was not achieved.
Ibuprofen is available in a variety of dosage forms and numerous brand names, one of which is FDA approved for the management of migraines, Advil Migraine (solubilized ibuprofen 200 mg capsules). Formulations that provide more rapid dissolution of the dosage form are associated with a faster onset of symptom relief.16 The short half-life of ibuprofen may require that multiple doses be used to prevent recurrence of symptoms.16 These products carry a risk of gastro-intestinal (GI) bleeding. Patients who are 60 years of age or older, have a history of stomach ulcers, are on anticoagulants, or drink more than three alcoholic beverages a day have an increased risk.
Combination Products: The first OTC product to gain FDA approval for the treatment of migraine was the combination of acetaminophen, aspirin, and caffeine (AAC), which is available as Excedrin Migraine (acetaminophen 250 mg, aspirin 250 mg, and caffeine 65 mg). The combination of these agents has been shown to be more effective than any one of the components alone in comparable doses.25 In a landmark study comparing AAC (n = 602) to placebo (n = 618), 59% of the AAC-treated patients experienced adequate pain relief in 2 hours compared with 33% with placebo.26,27 A further analysis of 172 of these patients who had severe or incapacitating disability showed that 40% of the AAC users had mild or no pain at 2 hours versus 20% for placebo.27
The effectiveness of a combination AAC product was compared with ibuprofen and placebo in the treatment of migraine in over 1,500 patients who had similar demographic profiles, migraine histories, and baseline symptom profiles.28 Patients were randomized to receive 2 tablet doses of each of the treatment regimens. Both active treatment regimens provided better relief in relieving pain and associated symptoms than placebo. However, the combination of AAC provided more rapid and superior pain relief compared with ibuprofen.
If patients use a combination product for their migraines, it is important to educate them about the caffeine content. There is as much caffeine in this product as there is in a cup of coffee; they should limit their caffeine intake while taking this product.
Conclusion
When confronted with a patient seeking advice for migraine pain, it is important for the pharmacist to adequately assess the patient to determine whether he or she is a candidate for self-treatment or in need of a referral. Both Advil Migraine and Excedrin Migraine received FDA approval for the treatment of migraines and are viable options. Other options, including acetaminophen and aspirin, do not have FDA approval for migraine but are considered effective for the management of mild-to-moderate migraines. Patients should take the product at the earliest signs of a migraine and to treat a minimum of three attacks. An agent is considered a therapeutic failure when the patient does not have relief in at least two of the three treated attacks. At this point, an alternate OTC agent should be tried or the patient should be referred to his or her healthcare provider.
It is very important to educate patients on the importance of limiting the use of OTC analgesics to no more than 2 days per week.29 Overuse of analgesics, including nonprescription products, can lead to medication overuse headache. If the headache worsens in severity or is not relieved with OTC agents, further evaluation is warranted.
PATIENT INFORMATION
What Can I Take for My Migraine?

Types
There are two major types of migraine headaches—migraine with aura and migraine without aura. The aura may start 20 minutes to 1 hour before the actual onset of symptoms. It can include seeing flashing lights/dots, tingling in the arm, or difficulty speaking.
Triggers
Many things can trigger a migraine, such as hormonal changes, certain foods or smells, hunger, and tension relief after stressful events. Keeping a headache diary can help you identify your triggers. Some food triggers may include chocolate, hard cheeses, red wine, or food and drinks that contain caffeine, gluten, nitrates, monosodium glutamate (MSG), or artificial sweeteners. Other common headache triggers include stress, skipping meals or not eating enough, too little or too much caffeine, over- or undersleeping, and drinking alcohol.
Treatment
Patients with a migraine often try to avoid lights, sounds, and smells due to increased sensitivity. Some people feel better if they lie down in a cool, dark, quiet room. Apply ice to decrease pain—use an ice pack or put crushed ice in a plastic bag. Cover the ice pack with a towel, and place it on your head where it hurts for 15 to 20 minutes every hour.
Some people need to take medications to help relieve their symptoms. This can include OTC and prescription drugs.
OTC Pain Medications: Aspirin used alone or in combination with acetaminophen plus caffeine may help your headache pain. Anti-inflammatory drugs such as ibuprofen or naproxen can also be used. You may need to try several different products to see which ones work best for you. Your doctor will want you to use the least amount of medication to treat your migraines. Aspirin, ibuprofen, or naproxen should be taken with food to reduce the chance of stomach upset. Alcohol should be avoided while taking these medications. Read the label on the package to ensure you do not take too much medication in a 24-hour period.
Prescription Drugs: Your doctor may prescribe a triptan (e.g., sumatriptan [Imitrex]) for your migraines. Triptans work on the cause of the migraine. They usually help the other symptoms that come with the headache, too. Triptans can be very effective but are not right for everyone. If you have heart disease or severe high blood pressure, these medications should be avoided.
Prevention
To help prevent migraines in the future, you can refer to your diary. In it, write down every time you have a headache and what you ate and did before it started. That way you can find out if there is anything you should avoid eating or doing. Also note what medications you took for the migraine and whether or not they helped. You should bring your diary with you to the doctor’s office.
Remember, if you have questions, Consult Your Pharmacist.
REFERENCES
1. Burch RC, Loder S, Loder E, Smitherman TA. The prevalence and burden of migraine and severe headache in the United States: updated statistics from government health surveillance studies. Headache J Head Face Pain. 2015;55(1):21-34.
2. Lipton RB, Stewart WF, Scher AI. Epidemiology and economic impact of migraine. Curr Med Res Opin. 2001;17(suppl 1):s4-s12.
3. Minen MT, Tanev K, Friedman BW. Evaluation and treatment of migraine in the emergency department: a review. Headache. 2014;54(7):1131-1145.
4. Goldberg LD. The cost of migraine and its treatment. Am J Manag Care. 2005;11(suppl 2):S62-S67.
5. Migraine Research Foundation. Migraine fact sheet. www.migraineresearchfoundation.org/fact-sheet.html. Accessed November 30, 2015.
6. Steiner TJ, Birbeck GL, Jensen RH, et al. Headache disorders are third cause of disability worldwide. J Headache Pain. 2015;16:58.
7. Lipton RB, Diamond S, Reed M, et al. Migraine diagnosis and treatment: results from the American Migraine Study II. Headache. 2001;41(7):638-645.
8. Villalón CM, Centurión D, Valdivia LF, et al. Migraine: pathophysiology, pharmacology, treatment and future trends. Curr Vasc Pharmacol. 2003;1(1):71-84.
9. Reddy DS. The pathophysiological and pharmacological basis of current drug treatment of migraine headache. Expert Rev Clin Pharmacol. 2013;6(3):271-288.
10. Pietrobon D, Moskowitz MA. Pathophysiology of migraine. Annu Rev Physiol. 2013;75(1):365-391.
11. Schürks M, Diener HC. Migraine, allodynia, and implications for treatment. Eur J Neurol. 2008;15(12):1279-1285.
12. Dodick D, Silberstein S. Central sensitization theory of migraine: clinical implications. Headache J Head Face Pain. 2006;46(suppl 4):S182-S191.
13. Ross LA, Ross BS. Chapter 35. Headache. In: Chisholm MA, Wells BG, Schwinghammer TL, et al, eds. Pharmacotherapy: Principles and Practice. 3rd ed. New York, NY: The McGraw-Hill Companies; 2013:621-632.
14. Minor DS, Wofford MR. Chapter 45. Headache disorders. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach, 9e. New York, NY: The McGraw-Hill Companies; 2014. http://mhmedical.com/content.aspx?aid=57493135. Accessed November 30, 2015.
15. Wenzel RG, Sarvis CA, Krause ML. Over-the-counter drugs for acute migraine attacks: literature review and recommendations. Pharmacotherapy. 2003;23(4):494-505.
16. Becker WJ. Acute migraine treatment in adults. Headache J Head Face Pain. 2015;55(6):778-793.
17. Lipton RB, Baggish JS, Stewart WF, et al. Efficacy and safety of acetaminophen in the treatment of migraine: results of a randomized, double-blind, placebo-controlled, population-based study. Arch Intern Med. 2000;160(22):3486-3492.
18. Tylenol. McNeil-PPC, Inc. www.tylenol.com/products/headache-muscle. Accessed November 30, 2015.
19. Ingledue VF, Mounsey A. PURLs: treating migraine: the case for aspirin. J Fam Pract. 2014;63(2):94-96.
20. Bayer safety coated aspirin. Comprehensive prescribing information. Morristown, NJ: Bayer Corporation. www.fda.gov/ohrms/dockets/ac/03/briefing/4012B1_03_Appd%201-Professional%20Labeling.pdf. Accessed November 30, 2015.
21. Nebe J, Heier M, Diener HC. Low-dose ibuprofen in self-medication of mild to moderate headache: a comparison with acetylsalicylic acid and placebo. Cephalalgia Int J Headache. 1995;15(6):531-535.
22. Kloster R, Nestvold K, Vilming ST. A double-blind study of ibuprofen versus placebo in the treatment of acute migraine attacks. Cephalalgia Int J Headache. 1992;12(3):169-171; discussion 128.
23. Codispoti JR, Prior MJ, Fu M, et al. Efficacy of nonprescription doses of ibuprofen for treating migraine headache. a randomized controlled trial. Headache. 2001;41(7):665-679.
24. Sandrini G, Franchini S, Lanfranchi S, et al. Effectiveness of ibuprofen-arginine in the treatment of acute migraine attacks. Int J Clin Pharmacol Res. 1998;18(3):145-150.
25. Diener HC, Pfaffenrath V, Pageler L, et al. The fixed combination of acetylsalicylic acid, paracetamol and caffeine is more effective than single substances and dual combination for the treatment of headache: a multicentre, randomized, double-blind, single-dose, placebo-controlled parallel group study. Cephalalgia Int J Headache. 2005;25(10):776-787.
26. Lipton RB, Stewart WF, Ryan RE, et al. Efficacy and safety of acetaminophen, aspirin, and caffeine in alleviating migraine headache pain: three double-blind, randomized, placebo-controlled trials. Arch Neurol. 1998;55(2):210-217.
27. Goldstein J, Hoffman HD, Armellino JJ, et al. Treatment of severe, disabling migraine attacks in an over-the-counter population of migraine sufferers: results from three randomized, placebo-controlled studies of the combination of acetaminophen, aspirin, and caffeine. Cephalalgia Int J Headache. 1999;19(7):684-691.
28. Goldstein J, Silberstein SD, Saper JR, et al. Acetaminophen, aspirin, and caffeine in combination versus ibuprofen for acute migraine: results from a multicenter, double-blind, randomized, parallel-group, single-dose, placebo-controlled study. Headache. 2006;46(3):444-453.
29. Matchar DB, Young WB, Rosenberg JH, et al. Evidence-Based Guidelines for Migraine Headache in the Primary Care Setting: Pharmacological Management of Acute Attacks. Minneapolis, MN: American Academy of Neurology; 2012. http://tools.aan.com/professionals/practice/pdfs/gl0087.pdf. Accessed November 30, 2015.
To comment on this article, contact rdavidson@uspharmacist.com.





