US Pharm. 2020;45(7/8):8-11.
Psoriasis, once thought of as a dermatologic disorder, is now recognized as a chronic, systemic immune-mediated inflammatory condition that speeds up the growth cycle in skin cells.1,2 It is the most prevalent autoimmune disease in the United States, affecting more than 8 million Americans.3 While it can affect anyone at any age, there appears to be a bimodal age distribution, with those aged 18 to 39 years and 50 to 69 years most affected.
Psoriasis is typically characterized by erythematous patches, as well as silvery, scaly patches typically found in areas of high movement, such as elbows and knees. It can also affect the scalp, lower back, face, nails, palms and soles, and intertriginous areas.2,4 Disease burden can be seen in its negative physical, psychiatric, and social tolls. Far from being a cosmetic problem, psoriasis can greatly affect a patient’s quality of life; psoriatic patients have higher rates of depression, anxiety, and suicidal ideation.5,6 In a national survey, 88% of patients reported that psoriasis affected their overall emotional well-being, and 82% reported that it affected their enjoyment of life.7
Psoriasis also has a high economic burden. It is estimated that the U.S. spends approximately $63 billion in direct medical costs and up to $35.4 billion in indirect costs.8 Psoriasis has been linked to other physical disorders, such as cardiovascular disease, metabolic disorders, and Crohn’s disease. Additionally, life expectancy is shortened by years in patients with severe psoriasis, mainly due to their increased cardiovascular risk.9
There is currently no cure for psoriasis. Most patients will have to undergo lifelong treatment to minimize and control symptoms. Adherence to treatment is critical for successfully managing disease and reducing severity, but less than half of psoriasis patients are adherent.10,11 Multiple barriers exist that pharmacists can help to overcome. Many patients doubt the efficacy of the treatments or have concerns about adverse effects. Many forget to take their medication or only use the medication when needed. Additionally, many patients have inadequate knowledge of the disease state itself, may not have received proper training on the use of various medications, or have decreased motivation and poor social support.10,12 As one of the most frequently encountered healthcare professionals, pharmacists can play a pivotal role in the management of psoriasis.
Pathophysiology and Risk Factors
Psoriasis is a chronic, complex, multifactorial, inflammatory disease. Although not quite fully understood, the pathogenesis of psoriasis involves disturbances in the innate and adaptive cutaneous immune response. An increased activation of the innate immune system results in a sustained inflammatory state, which ultimately contributes to the overproduction of epidermal cells and dysfunctional differentiation. Normally, epidermal cell turnover occurs every 21 to 28 days, but in psoriasis this occurs about every 3 to 4 days. The hyperkeratosis that results causes the characteristic features associated with psoriasis.4,13,14
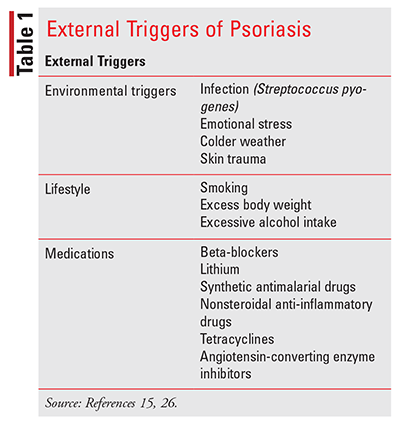
The exact cause for the development of psoriasis is unknown, but genetics and environmental factors both play a role. Multiple alleles and loci have been identified and are associated with an increased risk for psoriasis susceptibility. Approximately one-third of all psoriasis patients have a first-degree relative who is also affected. Studies have shown that if both parents have psoriasis, their children will have a 50% chance of developing this condition; this decreases to 16% if only one parent is afflicted. In studies evaluating the development of psoriasis in twins, it has been shown that environmental factors are also influential; it is thought that a genetic predisposition and the presence of external factors are both required (TABLE 1).4,13,15
Clinical Presentation
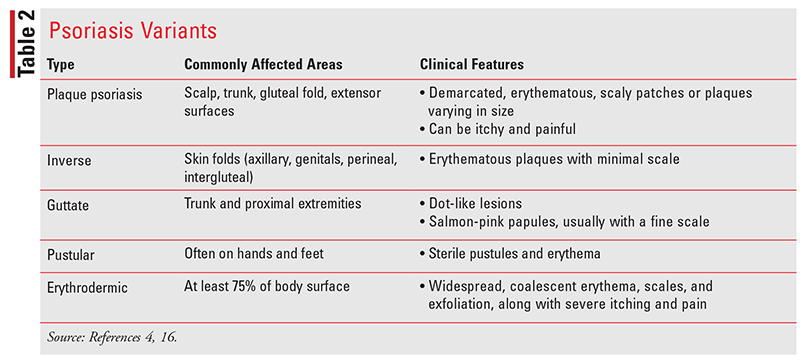
The presentation of psoriasis differs based on the psoriasis variant (TABLE 2). Although one variant will typically predominate, patients frequently present with overlapping features of different variants. Plaque psoriasis is the most common variant, affecting up to 80% of all patients. The other less-common variants include guttate psoriasis, pustular psoriasis, inverse psoriasis, and the very rare, but potentially life-threatening, variant erythrodermic psoriasis.4,16
Psoriasis is also classified based on severity: mild/limited disease, moderate disease, or severe disease, based on affected body surface area (BSA). Those with mild or limited disease usually have up to 3% BSA involvement, while severe disease affects more than 10% of BSA. Most patients are considered to have mild-to-moderate disease. Although BSA is a major determinant, severity also takes into account how psoriasis affects a person’s quality of life. Lesions in areas such as face, hands, feet, or genitalia may signify more severe disease, despite being low in surface area, due to their greater impact on patients’ lives.16,17
Treatment
It is important to establish appropriate expectations and treatment goals. Patients need to understand that this is a chronic condition that will require lifelong therapy; there is currently no cure, but treatments can lead to remission periods and reduce the severity of the disease. When speaking about treatment targets, a panel of experts with the National Psoriasis Foundation stated that an acceptable response for plaque psoriasis after 3 months of treatment is either achieving 3% or less BSA involvement or 75% or greater BSA improvement compared with baseline, with a goal of BSA involvement of 1% or less.
As healthcare professionals, we may only look at the physical markers, but subjective concerns of patients should also be evaluated. Factors such as pain or itching may persist after lesions are treated, and the treatment itself may worsen psychosocial distress, such as a patient’s embarrassment at having hands covered in ointment. Because of this, it is important to set realistic expectations with a patient and determine what nonphysical symptoms are relevant to them, helping to individualize treatment.18
When initiating treatment, a stepwise therapeutic approach is usually followed to attain efficacy while minimizing side effects. Mild-to-moderate psoriasis can typically be managed with topical treatments alone, while moderate-to-severe or unresponsive psoriasis may require systemic therapy or phototherapy in combination with topical remedies.
Topical treatments are available in a variety of classes, including corticosteroids, vitamin D analogues, retinoids, calcineurin inhibitors, keratolytic agents, coal tar, anthralin, ultraviolet phototherapy, or a combination of these agents. Systemic treatments include traditional immunosuppressive agents such as methotrexate and cyclosporine, as well as the newer biologic agents such as etanercept, adalimumab, and secukinumab. Studies have demonstrated the effectiveness of both topical and systemic agents in the management of psoriasis. However, even with demonstrated efficacy in studies, clinical practice continues to show that treatments often fail to adequately improve patients’ psoriasis, potentially due to lack of adherence. Patients on topical therapy tend to be least adherent, with almost 25% of patients considered nonadherent; many patients, when trying a new topical medication, fail to apply an appropriate amount, resulting in an underdose of the medication. Although patients tend to be more adherent to systemic therapies, adherence is still a concern due to tolerability and long-term side effects. Because of this, emphasizing adherence and proper use of therapies is pivotal to successful treatment.11,16,19-22
The Pharmacist’s Role
Most psoriasis patients have mild-to-moderate disease that can be managed with topical medications. Emollients and moisturizers should be used as adjunctive therapy on a daily basis; pharmacists should be speaking with psoriasis patients to ensure this practice. These products help relieve the itching and redness associated with psoriasis by limiting water evaporation and serving as a protective barrier to the outermost skin layer. The use of emollients and moisturizers also help enhance the delivery of topical corticosteroids. Although creams and ointments are preferred due to their occlusive properties, the choice of formulation will ultimately be the one that best suits the patient and will be easy to incorporate into their daily skin-care routine.23,24
Many patients have indicated barriers to their treatment regimens; using the medication only when needed and fear of adverse effects are some of the most common barriers cited. Pharmacists are ideally positioned to speak with patients regarding their concerns and use of these medications. Identification of patients who may not be adhering to their prescribed regimen can be identified through prescription refills. Pharmacists should routinely speak with their patients to ascertain if patients are dissatisfied with their care; recommendations can be made to help simplify their regimen or make their current regimen more effective. Pharmacist involvement in the care of psoriasis patients has been shown to enhance patients’ knowledge of their disease state, leading to significant improvements in quality of life. Patients may be able to more effectively self-manage their condition with the help and support of pharmacists.10,25
Conclusion
Psoriasis is a chronic, immune-mediated inflammatory disease without any cure. It can have a detrimental effect on patients, greatly impacting their quality of life. This condition requires lifelong treatments to manage symptoms; therefore, effective self-management is extremely important. Poor adherence, lack of understanding, and unrealistic expectations can lead to treatment failure. Pharmacists can make the largest impact by empowering patients through knowledge and support. Pharmacists can help patients learn more about psoriasis and individualize treatment goals. To improve adherence, especially with topical treatments, pharmacists can assist their patients by helping them understand the importance of their treatments and discussing the proper administration of their medication to ensure continued and correct use. Most importantly, pharmacists are there to help relieve any concerns patients may have regarding their psoriasis and their treatments and provide additional support to patients suffering from psoriasis.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
REFERENCES
1. Korman NJ. Management of psoriasis as a systemic disease: what is the evidence? Br J Dermatol. 2020;182(4):840-848.
2. CDC. Psoriasis. www.cdc.gov/psoriasis/index.htm. Accessed June 7, 2020.
3. National Psoriasis Foundation. Statistics. www.psoriasis.org/content/statistics. Accessed June 7, 2020.
4. Armstrong AW, Read C. Pathophysiology, clinical presentation, and treatment of psoriasis: a review. JAMA. 2020;323(19):1945-1960.
5. Kimball AB, Jacobson C, Weiss S, et al. The psychosocial burden of psoriasis. Am J Clin Dermatol. 2005;6(6):383-392.
6. Bhosle MJ, Kulkarni A, Feldman SR, Balkrishnan R. Quality of life in patients with psoriasis. Health Qual Life Outcomes. 2006;4:35.
7. Armstrong AW, Schupp C, Wu J, Bebo B. Quality of life and work productivity impairment among psoriasis patients: findings from the National Psoriasis Foundation survey data 2003–2011. PLoS One. 2012;7(12):e52935.
8. Brezinski EA, Dhillon JS, Armstrong AW. Economic burden of psoriasis in the United States: a systematic review. JAMA Dermatol. 2015;151(6):651-658.
9. Boehncke W-H, Boehncke S, Schön MP. Managing comorbid disease in patients with psoriasis. BMJ. 2010;340:b5666.
10. Feldman SR. Disease burden and treatment adherence in psoriasis patients. Cutis. 2013;92(5):258-263.
11. Thorneloe RJ, Bundy C, Griffiths CEM, et al. Adherence to medication in patients with psoriasis: a systematic literature review. Br J Dermatol. 2013;168(1):20-31.
12. Feldman SR, Horn EJ, Balkrishnan R, et al. Psoriasis: improving adherence to topical therapy. J Am Acad Dermatol. 2008;59(6):1009-1016.
13. Menter A. Psoriasis and psoriatic arthritis overview. Am J Manag Care. 2016;22(8 Suppl):s216-s224.
14. Rendon A, Schäkel K. Psoriasis pathogenesis and treatment. Int J Mol Sci. 2019;20(6):1475.
15. Gupta R, Debbaneh MG, Liao W. Genetic epidemiology of psoriasis. Curr Dermatol Rep. 2014;3(1):61-78.
16. Menter A, Gottlieb A, Feldman SR, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis. J Am Acad Dermatol. 2008;58(5):826-850.
17. Psoriasis speaks (AbbVie). Psoriasis severity and location. www.psoriasis.com/about-psoriasis/psoriasis-severity. Accessed June 10, 2020.
18. Armstrong AW, Siegel MP, Bagel J, et al. From the medical board of the National Psoriasis Foundation: treatment targets for plaque psoriasis. J Am Acad Dermatol. 2017;76(2):290-298.
19. Mason AR, Mason J, Cork M, et al. Topical treatments for chronic plaque psoriasis. Cochrane Database Syst Rev. 2013;(3):CD005028.
20. Storm A, Benfeldt E, Andersen SE, Serup J. A prospective study of patient adherence to topical treatments: 95% of patients underdose. J Am Acad Dermatol. 2008;59(6):975-980.
21. Kim IH, West CE, Kwatra SG, et al. Comparative efficacy of biologics in psoriasis: a review. Am J Clin Dermatol. 2012;13(6):365-374.
22. Chan SA, Hussain F, Lawson LG, Ormerod AD. Factors affecting adherence to treatment of psoriasis: comparing biologic therapy to other modalities. J Dermatolog Treat. 2013;24(1):64-69.
23. Van Onselen J. An overview of psoriasis and the role of emollient therapy. Br J Community Nurs. 2013;18(4):174-179.
24. Fluhr JW, Cavallotti C, Berardesca E. Emollients, moisturizers, and keratolytic agents in psoriasis. Clin Dermatol. 2008;26(4):380-386.
25. Tucker R, Stewart D. The role of community pharmacists in supporting self-management in patients with psoriasis. Int J Pharm Pract. 2017;25(2):140-146.
26. Kim GK, Del Rosso JQ. Drug-provoked psoriasis: is it drug induced or drug aggravated? J Clin Aesthet Dermatol. 2010;3(1):32-38.To comment on this article, contact rdavidson@uspharmacist.com.

What causes psoriasis?
The exact cause of psoriasis is unknown. It seems to run in families, meaning a person is more likely to have it if a parent is affected. Psoriasis can be triggered by a number of things, such as injury, illness, or irritation. Psoriasis cannot be caught from someone who has it.
When should I see a healthcare provider?
Psoriasis can vary in severity and type. If the affected area is covering a large surface or is in a sensitive region, it may be time to schedule an appointment with a primary care provider or a dermatologist. Some types of psoriasis, such as erythrodermic and pustular, can be harmful and even cause death if left untreated. Signs would include widespread (at least 75% of the skin) rash or scales with itching and pain. For these, it is best to visit an emergency room. Other cases can benefit from additional therapy, so if OTC treatments are not enough, it might be time to schedule a doctor’s appointment.
What can I take for psoriasis?
The mainstay of psoriasis care is topical lotions, creams, and ointments that may include steroids. These medications help control the itching sensation while helping the skin to heal. For more severe psoriasis, you may need a higher strength steroid requiring a prescription. When cases are severe or not responding to topical treatments, there are other medications that can be used to get the condition back under control. People with the worst cases of psoriasis may have to use medications that need to be injected. Other options include coal tar, salicylic acid, and epsom salt baths, which are available OTC but come with their own drawbacks and are not thought to be as effective. Speak with a pharmacist or other healthcare professional before using them.
How are topical treatments used?
It is important to speak with a pharmacist whenever starting a new treatment because each can have differences in the amount to apply, how often, and expected results. Adherence to a regimen is the most important thing for success; it may take weeks to see the maximum effect, so don’t be discouraged if there’s no immediate improvement. Additionally, it is important to make sure you are applying enough of the medication to treat the area. Some providers will recommend covering the area to keep the medication where it is applied, but this can differ based on what the medication is and the application site, so make sure to clarify this with providers and pharmacists.
Where can I get more information about psoriasis?
For more information, visit the National Psoriasis Foundation website: www.psoriasis.org and TalkPsoriasis: http://talkpsoriasis.org.






